The exploration into the specific steroids utilized for occipital nerve blocks, while primarily a clinical question, unveils a multifaceted financial landscape that impacts patients, healthcare providers, and the broader economic ecosystem. Understanding the fiscal implications associated with such medical interventions is paramount for informed financial planning, strategic investment, and efficient healthcare resource allocation. From the cost of pharmaceuticals to insurance complexities and the business models of pain management clinics, the financial threads woven into chronic pain treatment are numerous and significant.
The Economic Landscape of Chronic Pain Management
Chronic pain, including conditions like occipital neuralgia, represents a staggering economic burden globally. Beyond the individual suffering, the costs associated with diagnosis, treatment, and lost productivity due to chronic pain run into hundreds of billions of dollars annually. Occipital nerve blocks are a common interventional treatment for various forms of occipital neuralgia and headaches, involving the injection of a local anesthetic, often combined with a corticosteroid, near the occipital nerves. While the immediate clinical goal is pain relief, the choice of steroid, the frequency of treatment, and the overall management strategy inherently carry substantial financial ramifications.
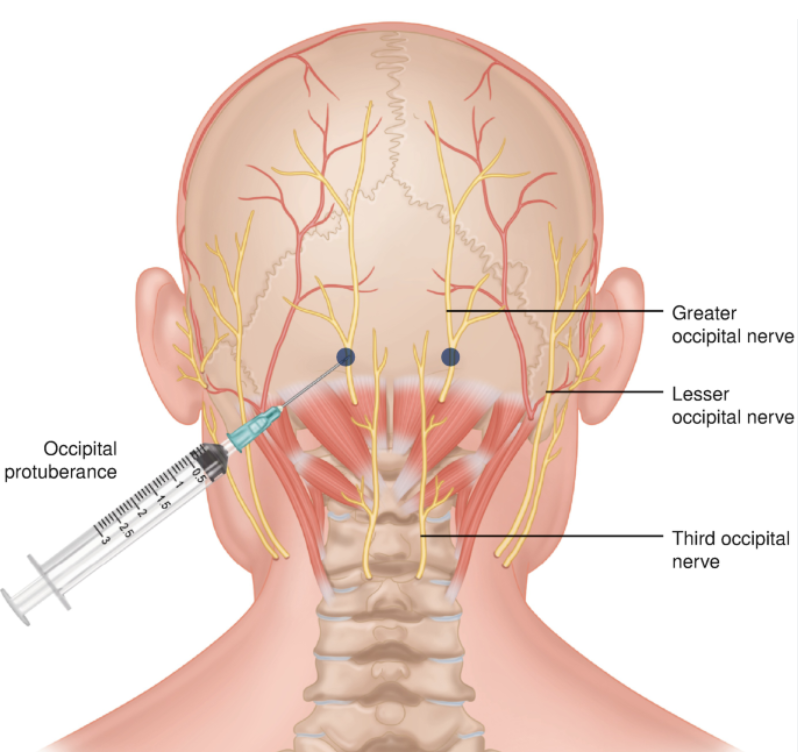
The pain management sector is a robust and growing segment of the healthcare economy. As populations age and understanding of chronic pain mechanisms evolves, demand for effective, minimally invasive treatments continues to climb. This creates a dynamic financial environment ripe for analysis, influencing investment decisions in pharmaceutical development, medical device innovation, and specialized healthcare facilities. The economic considerations extend far beyond the immediate cost of a single injection, encompassing long-term patient financial stability, healthcare system sustainability, and investor returns.
Cost-Benefit Analysis of Steroid Choices in Nerve Blocks
The selection of a specific steroid for an occipital nerve block is a clinical decision based on efficacy, side effect profile, and physician preference. However, each choice carries a distinct financial profile that influences the total cost of care.
Pharmaceutical Pricing and Accessibility
Common corticosteroids used in occipital nerve blocks include Dexamethasone, Triamcinolone, and Methylprednisolone. These drugs vary in their potency, duration of action, and, crucially, their market price.
- Dexamethasone: Often favored for its lower particulate matter, which some clinicians prefer for nerve blocks due to concerns about neurovascular compromise. It is generally a less expensive corticosteroid, readily available in generic formulations. Its cost-effectiveness can be appealing to both providers and patients, especially in systems with constrained budgets or high patient out-of-pocket expenses.
- Triamcinolone: A common choice, available in various concentrations. While effective, it is a particulate steroid, which can sometimes raise concerns among practitioners depending on the anatomical location of the injection. Its pricing is moderate, with generic options widely available, making it a frequently utilized option balancing cost and effectiveness.
- Methylprednisolone: Another widely used particulate steroid, often associated with a higher cost profile compared to Dexamethasone, particularly certain formulations. The decision to use Methylprednisolone may be driven by specific clinical considerations, but these must be weighed against its higher per-dose cost, which can impact both clinic profitability and patient charges.
The difference in acquisition cost for a clinic, even if seemingly small per dose, can accumulate significantly over hundreds or thousands of procedures annually. These differences directly influence the billing practices, markups, and ultimately, the final price presented to the patient or insurer. The availability of generic versus brand-name formulations also plays a critical role, with generics invariably offering a more economical option, thereby reducing the overall financial burden on the system.
Insurance Reimbursement Complexities
The financial impact of steroid choice extends significantly into insurance reimbursement. Healthcare payers scrutinize procedure codes (CPT codes) and associated drug costs when adjudicating claims.
- CPT Coding and Drug Billing: Occipital nerve blocks are typically billed under specific CPT codes that cover the procedure itself. However, the cost of the drug (the steroid) may be billed separately using specific HCPCS codes, or it may be bundled into the overall procedure fee. If billed separately, the specific steroid chosen can directly affect the reimbursement amount. Insurers often have preferred drug formularies, and non-formulary drugs, or those deemed more expensive without superior efficacy, may lead to lower reimbursement or require prior authorization, adding administrative cost and potential delays.
- Formularies and Prior Authorization: Many insurance plans classify drugs into tiers or list them on formularies. A steroid that is not on a preferred tier or formulary might incur higher patient out-of-pocket costs or require a prior authorization process. This administrative hurdle adds cost to the healthcare system (for both the provider and the insurer) and can delay necessary treatment, indirectly increasing overall care costs if pain escalates.
- Patient Out-of-Pocket Expenses: For patients, the choice of steroid can affect deductibles, co-pays, and co-insurance. A more expensive steroid, or one less favorably reimbursed by their insurance, can translate into a higher financial responsibility. Patients with chronic conditions often undergo multiple blocks over time, making cumulative drug costs a substantial financial consideration for their personal budgets. Transparent communication regarding these costs is crucial for patients to make informed decisions about their treatment plans.
Investment Opportunities in Pain Management Therapeutics
The financial ecosystem surrounding pain management treatments offers significant opportunities for investors, particularly within the pharmaceutical and biotechnology sectors, as well as in healthcare service providers.
Pharmaceutical Sector Spotlight
Companies that research, develop, and manufacture the steroids and local anesthetics used in nerve blocks represent a stable investment avenue. The consistent demand for pain relief ensures a steady market for these essential drugs.
- Established Pharmaceutical Giants: Larger pharmaceutical companies with diversified portfolios often include corticosteroids in their product lines. Investments here can offer stability and returns tied to broad healthcare trends.
- Biotech Innovators: While the steroids themselves are largely generic, continuous innovation in drug delivery systems or novel adjuvant therapies to extend the efficacy or reduce side effects of nerve blocks presents opportunities. Companies exploring sustained-release steroid formulations or non-opioid alternatives for pain management are particularly attractive.
- Market Trends: The global pain management drug market is projected for significant growth. Investors track patent expirations for existing drugs, the pipeline of new treatments, and regulatory changes that could impact market access and profitability.
Ancillary Services and Technology
Beyond the drugs themselves, the broader infrastructure supporting pain management procedures also presents investment potential.
- Pain Management Clinics and Ambulatory Surgical Centers (ASCs): These facilities are direct beneficiaries of the demand for interventional pain procedures. Investment in private equity-backed clinics or public clinic chains offers exposure to the operational and service delivery aspects of pain management. Their profitability is directly linked to efficient procedure scheduling, advantageous insurance contracts, and cost-effective procurement of supplies, including steroids.
- Diagnostic Tools and Imaging Technology: Accurate diagnosis of occipital neuralgia often relies on advanced imaging. Companies developing or supplying MRI, CT, or ultrasound equipment utilized for precise nerve block guidance (reducing complications and enhancing efficacy) are integral to the ecosystem.
- Telehealth and Digital Health Solutions: The rise of telehealth has significant implications for chronic pain management, enabling remote consultations, monitoring, and follow-up care. Investment in digital platforms that streamline patient care, improve adherence, and offer remote pain coaching can enhance patient outcomes and create new revenue streams.
Financial Planning for Chronic Pain Sufferers
For individuals living with chronic pain, managing the financial impact of ongoing treatment, including procedures like occipital nerve blocks, is a critical aspect of their overall well-being.
Navigating Healthcare Costs
Proactive financial planning can significantly mitigate the burden of healthcare expenses.
- Understanding Insurance Benefits: Patients must thoroughly understand their insurance policy’s specifics, including deductibles, co-pays, out-of-pocket maximums, and formulary restrictions. Knowing which providers and facilities are in-network can prevent unexpected charges.
- Negotiating and Advocating: Patients should not hesitate to negotiate medical bills, especially for out-of-network services or unexpected charges. Seeking clarification on billing codes and drug costs can identify discrepancies. Patient advocacy groups can also provide valuable resources and support.
- Seeking Financial Assistance: Many hospitals and pharmaceutical companies offer patient assistance programs, discounts, or payment plans for those facing significant financial hardship. Exploring these options can considerably reduce the out-of-pocket costs for necessary treatments. Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs) offer tax advantages for saving for medical expenses.
Impact on Earning Potential and Productivity
Chronic pain doesn’t just incur direct medical costs; it also impacts a person’s ability to work, earn income, and participate fully in the economy.
- Lost Wages and Productivity: Recurrent pain can lead to absenteeism, reduced work performance, and, in severe cases, disability. This translates directly to lost wages and a significant blow to personal finance. For employers, this means reduced productivity and increased costs.
- Career Limitations: Chronic pain can force individuals to change careers or reduce work hours, potentially limiting their earning potential and long-term financial security. Vocational rehabilitation and support programs can play a crucial role in helping individuals navigate these challenges.
- Societal Economic Cost: On a broader scale, the economic cost of lost productivity due due to chronic pain, including conditions requiring occipital nerve blocks, is immense, impacting national GDP and healthcare expenditures.
In conclusion, while the question “what steroid is used for occipital nerve block” is clinical in nature, its implications extend deeply into the financial health of patients, providers, and investors. The choice of steroid influences drug costs, insurance reimbursement, clinic profitability, and the overall economic burden of chronic pain. A comprehensive understanding of these financial dynamics is essential for navigating the complex landscape of modern healthcare.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.