The intersection of behavioral health and cutting-edge technology has ushered in a transformative era for psychiatric care. Historically, understanding “what is bipolar depression disorder” required months of subjective patient journaling and retrospective clinical interviews. Today, the integration of Artificial Intelligence (AI), wearable biosensors, and digital phenotyping is redefining the diagnosis and management of this complex condition. By shifting from reactive treatment to predictive analytics, technology is providing a high-definition lens through which we can observe the cyclical nature of bipolar disorder.
The Digital Architecture of Bipolar Depression
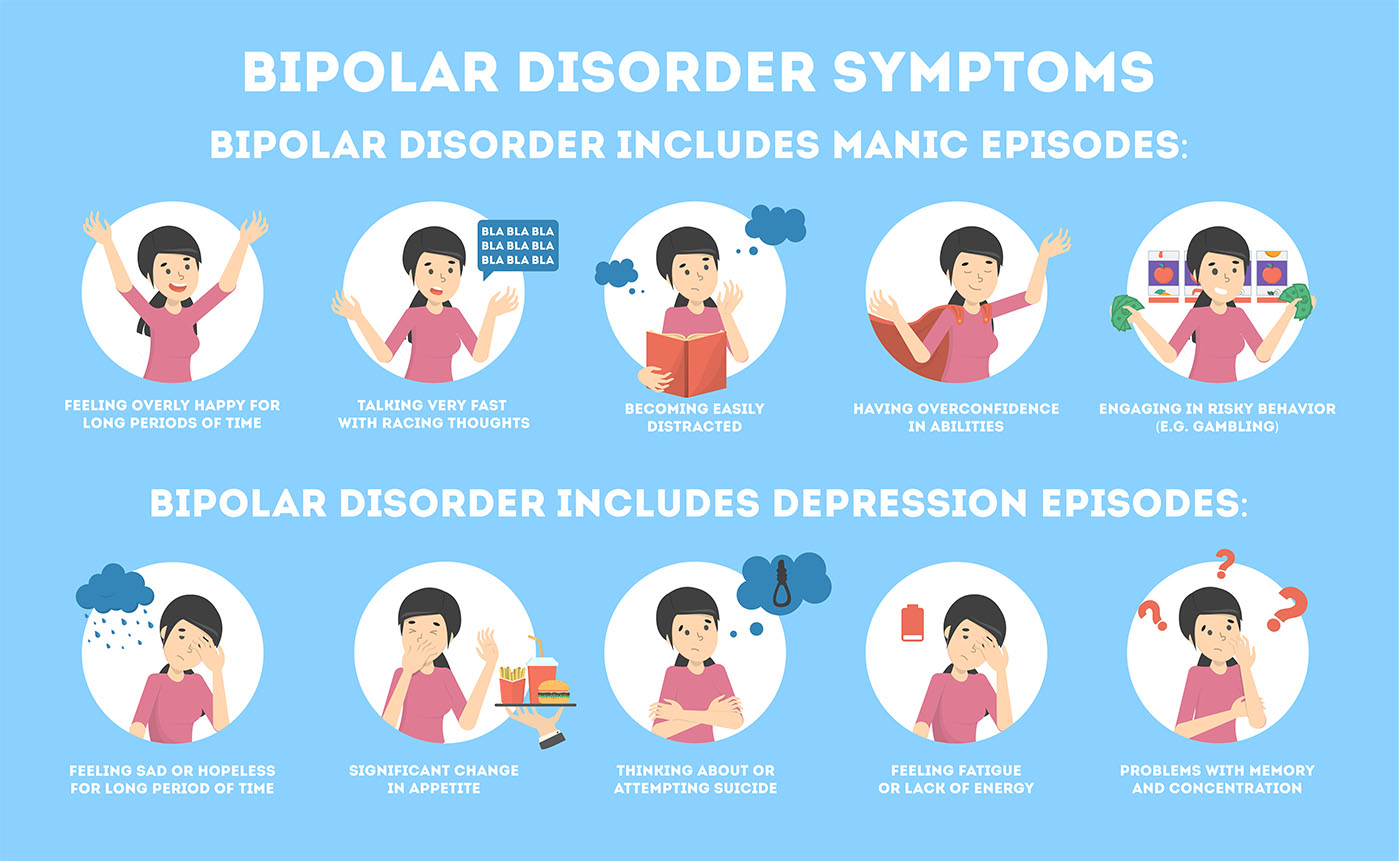
To understand bipolar depression from a technical perspective, one must view it as a systemic dysregulation of biological rhythms. Bipolar disorder is a chronic mental health condition characterized by significant fluctuations in mood, energy, and activity levels. Unlike unipolar depression, bipolar depression occurs as part of a cycle that includes manic or hypomanic “highs.”

Defining the Data Points of Mood Cycles
From a tech-centric viewpoint, bipolar depression represents a “low-state” data phase. In this state, the “user”—or patient—experiences a sharp decline in cognitive processing speed, physical mobility, and social interaction. Technology tools now allow us to quantify these shifts. Through digital phenotyping, researchers use smartphone sensor data to track passive biomarkers such as GPS movement, typing speed, and frequency of communication. These metrics provide an objective baseline, allowing software to detect the onset of a depressive episode long before the patient becomes consciously aware of the shift.
The Role of Machine Learning in Differential Diagnosis
One of the greatest challenges in clinical psychiatry is distinguishing bipolar depression from major depressive disorder (MDD). Misdiagnosis is common because patients often seek help during the “low” phase while failing to report previous “high” phases. Tech-driven diagnostic tools are bridging this gap. By utilizing machine learning algorithms trained on thousands of hours of speech patterns and facial recognition data, software can identify subtle markers of “pressured speech” or “psychomotor agitation” that characterize the manic side of the spectrum, thereby clarifying the bipolar diagnosis with greater precision than traditional questionnaires.
Wearables and the Quantification of Biological Rhythms
The hardware revolution, led by sophisticated gadgets like the Apple Watch, Oura Ring, and specialized medical-grade wearables, has provided a 24/7 stream of biometric data. For an individual managing bipolar depression, these devices function as an external nervous system, monitoring the physiological triggers that precede a mood shift.
Sleep Tracking as a Predictive Metric
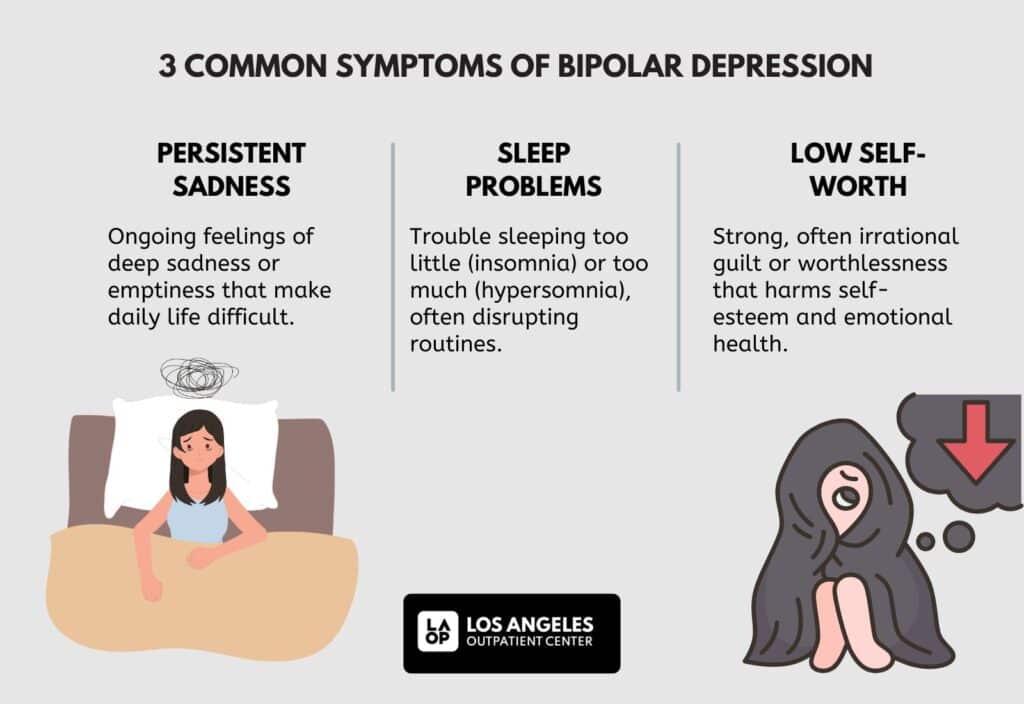
Sleep disturbance is a primary diagnostic criterion for bipolar disorder. A sudden decrease in the need for sleep often signals an impending manic episode, while hypersomnia (excessive sleeping) is a hallmark of the depressive phase. Modern sleep-tracking apps utilize accelerometers and optical heart rate sensors to map sleep architecture. By analyzing REM cycles and deep sleep duration, these tools can alert both the user and their healthcare provider to deviations from their “euthymic” (stable) baseline. This real-time feedback loop allows for immediate pharmacological or behavioral adjustments.
Heart Rate Variability (HRV) and Autonomic Balance
Heart Rate Variability (HRV) has emerged as a critical digital biomarker in the tech-health space. HRV measures the variation in time between each heartbeat and serves as a proxy for the autonomic nervous system’s resilience. Low HRV is frequently associated with the “shutdown” response seen in bipolar depression. By monitoring HRV via photoplethysmography (PPG) sensors, wearable gadgets can provide a “readiness score.” This data empowers users to understand their physiological capacity for stress on any given day, preventing the over-stimulation that often triggers a subsequent crash into depression.
AI and Predictive Analytics: Moving Toward Proactive Care
The most significant tech trend in mental health is the move toward predictive modeling. If bipolar depression is a cycle, then the goal of modern software is to flatten the curve. AI tools are now capable of analyzing vast datasets to identify “prodromal” symptoms—early warning signs that occur before a full-blown episode.
Natural Language Processing (NLP) in Mood Monitoring
Our digital footprint—the way we text, post on social media, and search the web—contains a wealth of information about our mental state. Natural Language Processing (NLP) algorithms can scan text for sentiment analysis, word frequency, and syntax changes. For instance, a shift toward using more first-person singular pronouns (“I,” “me”) and words associated with stagnation can be a digital signature for depression. Conversely, rapid-fire messaging and fragmented sentence structures may indicate hypomania. These AI tools act as a “check engine light” for the human brain, providing objective feedback to the user.
Algorithmic Intervention and Digital Therapeutics (DTx)
Digital Therapeutics (DTx) are a new category of software-driven treatments designed to prevent, manage, or treat medical disorders. For bipolar depression, DTx platforms utilize Cognitive Behavioral Therapy (CBT) modules delivered via smartphone. These are not simple “meditation apps”; they are evidence-based, regulated software systems. When an algorithm detects a dip in activity or a disruption in sleep, the DTx platform can automatically prompt the user with a specific behavioral activation exercise or a “mood-charting” task to mitigate the severity of the coming depressive episode.
Telemedicine and the Virtualization of Specialized Care
The digital transformation of the clinical landscape has dismantled many of the barriers to treating bipolar depression. Telemedicine is no longer just a video call; it is an integrated ecosystem of digital tools that connect the patient to a global network of specialists.
The Rise of Remote Patient Monitoring (RPM)
Remote Patient Monitoring (RPM) software allows psychiatrists to view a dashboard of a patient’s biometric data in real-time. Instead of waiting for a monthly appointment to hear how a patient has been feeling, a clinician can see a graphical representation of the patient’s activity levels, sleep quality, and medication adherence over the past 30 days. This “data-driven psychiatry” allows for more nuanced medication management. If the software shows a trending decrease in physical activity, the physician can intervene via a virtual visit before the patient reaches a state of clinical crisis.
Virtual Reality (VR) in Therapeutic Environments
Virtual Reality is emerging as a powerful tool in treating the cognitive symptoms of bipolar depression. During a depressive phase, individuals often struggle with executive function and “brain fog.” VR tutorials and cognitive training games are being developed to help stimulate neural plasticity. Furthermore, VR can be used for “exposure therapy” in a controlled environment, helping patients practice social interactions that they might otherwise avoid during a depressive withdrawal.
Security, Ethics, and the Future of Mental Health Tech
As we integrate apps and gadgets into the treatment of bipolar depression, the conversation inevitably turns to digital security and data privacy. The sensitivity of mental health data requires a higher standard of protection than typical consumer data.
Encrypting the Mind: Data Security in HealthTech
For technology to be a viable tool in managing bipolar disorder, users must trust that their most private thoughts and biological signals are secure. This has led to the adoption of end-to-end encryption in mental health apps and the implementation of HIPAA-compliant cloud storage solutions. The trend toward “edge computing”—where data is processed locally on the device rather than in the cloud—is also gaining traction as a way to enhance privacy.
The Ethical Integration of AI
The future of tech in the mental health space hinges on the ethical application of AI. While predictive algorithms can save lives by identifying suicidal ideation or severe depressive shifts, they must be used as a supplement to, not a replacement for, human intuition. The “black box” nature of some AI models poses a challenge in clinical settings where transparency is vital. The next generation of mental health tech will focus on “Explainable AI” (XAI), ensuring that both patients and providers understand the “why” behind an algorithm’s recommendation.
In conclusion, answering “what is bipolar depression disorder” in the 21st century requires an acknowledgment of our digital reality. It is no longer just a clinical diagnosis found in the DSM-5; it is a complex, fluctuating biological state that can be mapped, monitored, and managed through an ecosystem of software and hardware. As AI continues to evolve and wearables become more unobtrusive, the goal of “stability” for those living with bipolar disorder becomes more attainable than ever before. Through the lens of technology, we are not just observing the cycles of the mind—we are learning to master them.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.