In the contemporary landscape of digital health, the intersection of artificial intelligence (AI) and clinical diagnostics has ushered in a new era of proactive wellness. One of the most significant shifts is occurring in how we approach sensitive health concerns, such as the visual identification of sexually transmitted infections (STIs). For years, the question of “what do vaginal herpes look like” was one relegated to hushed conversations or low-resolution search engine results. Today, that query is the foundation for sophisticated machine learning models, computer vision algorithms, and telehealth infrastructures designed to provide high-accuracy, private, and immediate diagnostic support.
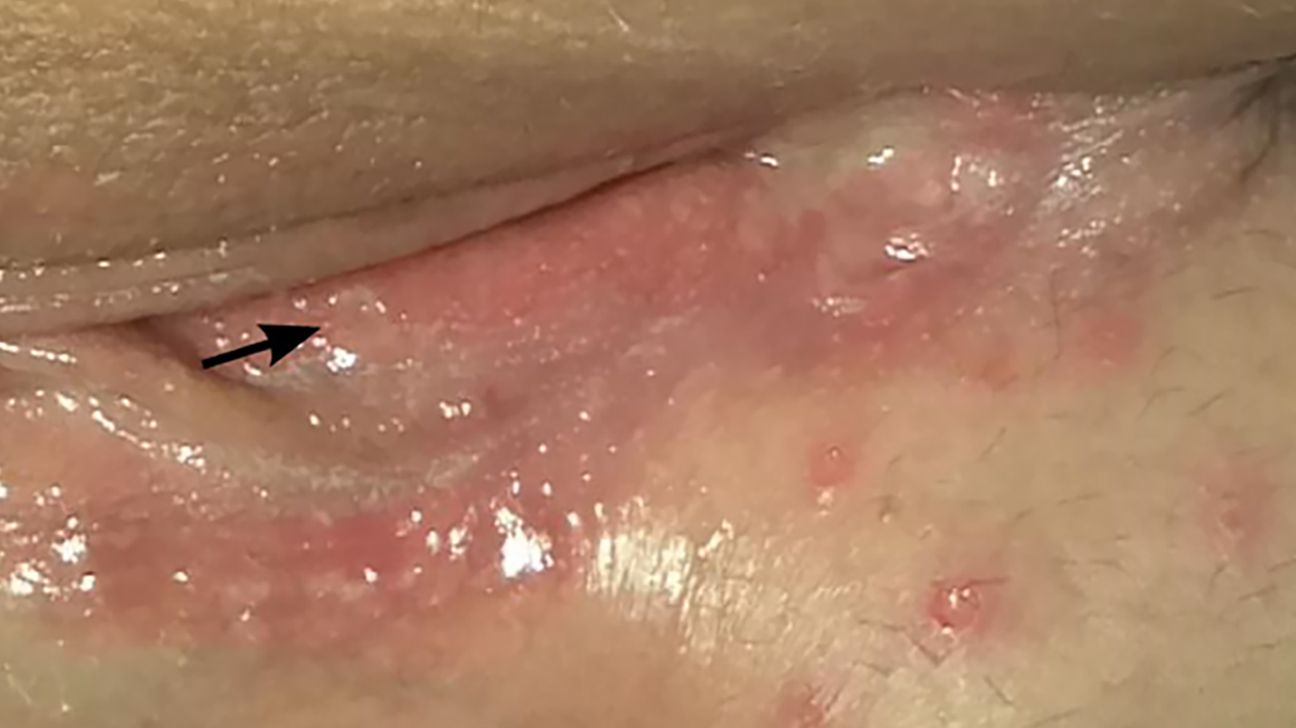
As we delve into the technological architecture of modern sexual health tools, we see a convergence of software engineering, data science, and cybersecurity. This article explores the technical evolution of visual diagnostics, the role of neural networks in clinical recognition, and the security frameworks protecting the most sensitive data in the digital health ecosystem.
The Rise of Visual AI: Training Neural Networks for Clinical Recognition
The cornerstone of modern diagnostic tech is Computer Vision—a field of AI that enables computers to derive meaningful information from digital images or videos. When it comes to identifying dermatological manifestations of STIs like herpes simplex virus (HSV), the technology relies on complex layers of processing.
Convolutional Neural Networks (CNNs) and Image Processing
At the heart of identifying visual pathologies is the Convolutional Neural Network (CNN). Unlike traditional software that follows rigid “if-then” logic, CNNs are designed to mimic the human visual cortex. They process images through multiple layers: the initial layers detect basic edges and textures, while deeper layers identify complex patterns, such as the specific clustering, fluid-filled nature, and erythematous base typical of herpetic lesions.
For a software platform to accurately answer a user’s visual concern, the underlying model must be trained on tens of thousands of annotated images. Developers utilize “supervised learning,” where clinicians label images of various stages of an outbreak—from initial tingling and redness to the formation of vesicles and eventual crusting. This allows the AI to distinguish between herpes and similar-looking conditions, such as contact dermatitis, ingrown hairs, or folliculitis, with increasing precision.
Dataset Diversity and the Challenge of Variance
One of the most significant technical hurdles in developing these AI tools is ensuring dataset diversity. Human physiology varies wildly across different skin tones and anatomical structures. An AI model trained exclusively on one demographic will fail to accurately identify symptoms on another.
Tech companies in the HealthTech space are now prioritizing “inclusive datasets.” This involves sourcing high-resolution imagery across the Fitzpatrick scale (a numerical classification schema for human skin color) to ensure that the software’s “visual” understanding of an infection remains accurate regardless of the patient’s ethnicity. This technical rigor is essential for reducing false negatives and ensuring the tool is a reliable precursor to professional medical consultation.
The Role of Telehealth Infrastructure in Remote Visual Screening
Beyond the AI models themselves, the hardware and software “stack” used to deliver these insights has undergone a revolution. Telemedicine is no longer just a video call; it is an integrated ecosystem of high-definition data transmission and real-time analysis.
High-Definition Asynchronous Communication
The “store-and-forward” (asynchronous) model of telehealth is particularly effective for visual diagnostics. In this workflow, a user uploads high-resolution imagery through a secure portal. The tech stack must support high-bitrate image transfers without heavy compression, as lossy compression algorithms (like those used in standard social media apps) can strip away the micro-details—such as the “umbilicated” center of a vesicle—that are vital for an accurate differential diagnosis.

Engineers focus on optimizing the “Upload-to-Analysis” pipeline. This involves edge computing, where initial image processing occurs closer to the user to reduce latency, and cloud-based processing for the heavy lifting of the AI’s deep learning inference.
Integration with Electronic Health Records (EHR)
A diagnostic tool is only as good as its utility within the broader medical framework. Modern HealthTech apps are designed with API-first architectures that allow for seamless integration with Electronic Health Records (EHR). When a digital tool identifies a high probability of a viral outbreak, the data can be ported directly into a clinician’s workflow via HL7 or FHIR (Fast Healthcare Interoperability Resources) standards. This ensures that the transition from a digital “first look” to a clinical prescription and treatment plan is frictionless and data-driven.
Privacy-First Technology: Securing Sensitive Medical Imagery
When users interact with software to determine “what do vaginal herpes look like” in relation to their own bodies, they are sharing some of the most sensitive data imaginable. Consequently, the “Digital Security” aspect of this niche is perhaps the most critical.
End-to-End Encryption and Zero-Knowledge Proofs
To protect user privacy, leading platforms employ End-to-End Encryption (E2EE) for all image transfers. In an E2EE environment, the image is encrypted on the user’s device and can only be decrypted by the intended recipient (a licensed physician) or a secure, sandboxed AI environment.
Furthermore, some cutting-edge startups are experimenting with Zero-Knowledge Proofs (ZKP). This cryptographic method allows the system to verify that a user has a specific condition (for the purpose of routing them to the right specialist) without actually “seeing” or storing the raw image in a way that is linked to the user’s identity. This “privacy-by-design” approach is essential for building user trust in a digital-first medical world.
Compliance Frameworks: GDPR, HIPAA, and Beyond
Navigating the regulatory tech landscape is a core component of developing health software. Developers must build systems that are compliant with the Health Insurance Portability and Accountability Act (HIPAA) in the US and the General Data Protection Regulation (GDPR) in Europe. This involves implementing rigorous audit logs, multi-factor authentication (MFA), and automated data-wiping protocols. From a technical perspective, this means the software must distinguish between “Protected Health Information” (PHI) and de-identified metadata used for improving the AI’s accuracy.
The Future of Wearables and Real-Time Health Monitoring
As we look toward the next decade, the tech used to identify visual symptoms will likely move from the smartphone screen to wearable devices and integrated biosensors.
Biosensors and Optical Recognition
The next iteration of “visual identification” may not require a camera at all. Research is currently underway into wearable biosensors that can detect the molecular markers of a viral shedding event before a physical lesion even appears. However, for those already experiencing symptoms, augmented reality (AR) glasses or specialized “smart mirrors” could use multi-spectral imaging to highlight areas of inflammation that are invisible to the naked eye.
These devices use infrared and ultraviolet sensors to look “under the skin,” detecting the hyper-vascularization associated with a viral prodrome. This represents a shift from reactive identification (looking at what an outbreak looks like) to predictive monitoring.
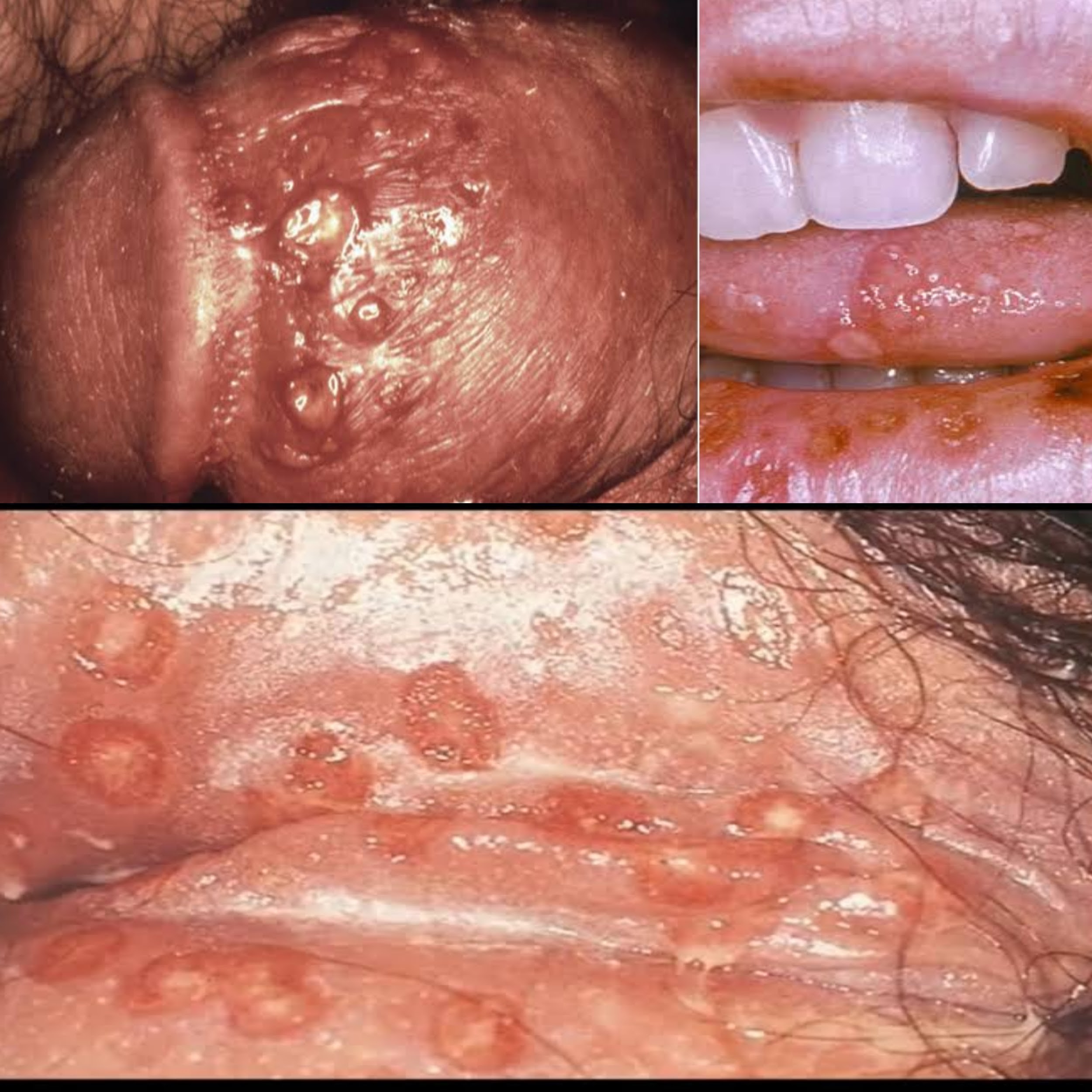
Bridging the Gap Between Consumer Tech and Clinical Tools
The ultimate goal of this technological evolution is the “democratization of diagnostics.” By putting sophisticated computer vision tools into the hands of the consumer, the tech industry is reducing the stigma and the barriers to entry for sexual health care. When a piece of software can accurately, privately, and instantly analyze a symptom, it empowers the user to seek treatment faster, thereby reducing transmission rates and improving long-term health outcomes.
The journey from a simple search query to a sophisticated AI-driven diagnosis is a testament to the power of modern software engineering. As AI models become more refined and security protocols more robust, the digital identification of visual pathologies will become a standard, unremarkable part of our daily health tech stack. The question of “what do symptoms look like” is no longer just a medical one—it is a data science challenge that we are rapidly solving through innovation.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.