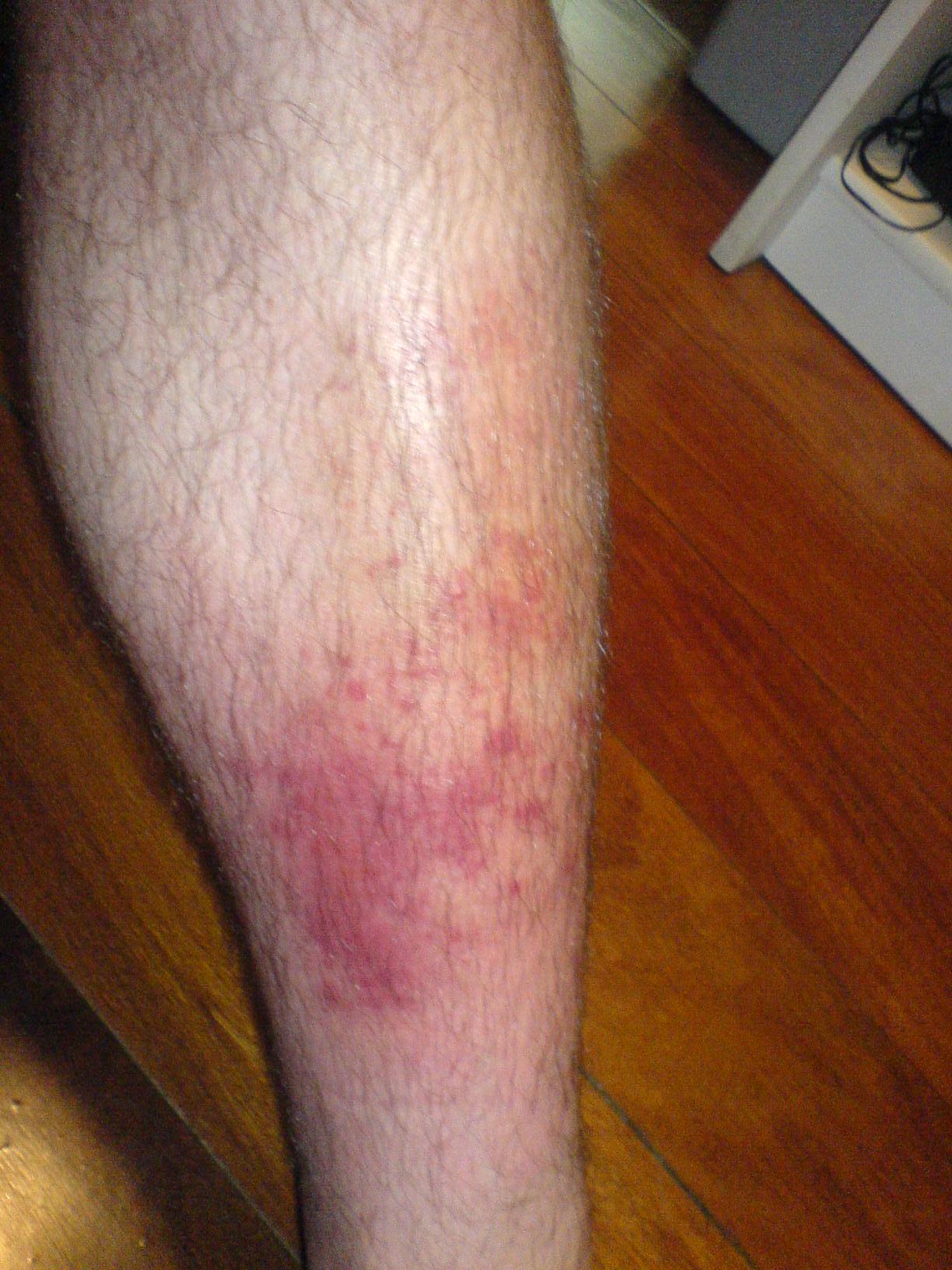
A “cellulite infection” is, more accurately, known as cellulitis – a common yet serious bacterial infection of the skin and underlying tissues. It typically appears as a red, swollen, tender area that feels hot to the touch and can spread rapidly. While the term “cellulite” refers to a benign cosmetic condition involving dimpled skin, combining it with “infection” immediately signals a grave health concern. When left untreated, or when complications arise, cellulitis can escalate from a localized problem to a life-threatening systemic illness. Beyond the immediate physical discomfort and health risks, however, lies a significant and often underestimated financial burden. Understanding what cellulitis is, from the perspective of its economic impact, is crucial for both personal finance and holistic well-being. This article delves into the various financial costs associated with cellulitis, from direct medical expenses to indirect economic repercussions, and discusses strategies for managing these challenges effectively.
The Hidden Financial Burden of Cellulitis
The onset of a health crisis like cellulitis triggers a cascade of financial consequences, often catching individuals unprepared. These costs are multifaceted, extending far beyond a simple prescription fee, and can severely strain personal and household budgets. Recognizing these potential expenditures is the first step toward mitigating their impact.
Direct Medical Costs: From Diagnosis to Recovery
The most apparent financial strain comes from the direct costs of medical intervention. Cellulitis, by its nature, demands prompt and often intensive treatment, leading to a series of charges that can quickly accumulate.
Initially, a diagnosis requires a visit to a healthcare professional. This could be a primary care physician, an urgent care clinic, or, if symptoms are severe and rapid, an emergency room. Each of these entry points carries a different price tag. A standard doctor’s visit might incur a co-pay or a deductible payment, while an emergency room visit, particularly without adequate insurance, can run into hundreds or even thousands of dollars before any treatment is rendered. The diagnostic process itself, though often clinical, might involve blood tests to rule out other conditions or identify the specific bacterial strain, adding further laboratory fees.
Once diagnosed, the primary treatment for cellulitis involves antibiotics. Oral antibiotics are typically prescribed for milder cases, with prescription costs varying widely depending on the drug, dosage, duration, and insurance coverage. A course could range from tens to hundreds of dollars. However, if the infection is widespread, severe, or not responding to oral medication, intravenous (IV) antibiotics become necessary. This often necessitates hospitalization, transforming a relatively manageable cost into a substantial financial outlay. Hospital stays for cellulitis can range from a few days to over a week, accruing daily charges for room and board, nursing care, IV medication administration, monitoring, and potentially specialist consultations (e.g., infectious disease specialists or dermatologists). The aggregate cost of a hospital admission for cellulitis can easily reach thousands to tens of thousands of dollars, making it a leading cause of unplanned medical debt for many individuals.
Furthermore, some severe cases of cellulitis, especially those leading to abscess formation or tissue necrosis, might require surgical intervention. This could involve draining pus from an abscess, debridement (removal of dead tissue), or in rare, extreme cases, amputation. Surgical procedures come with their own set of costs: surgeon’s fees, anesthesiologist’s fees, operating room charges, and extended post-operative care, adding another layer of significant expense. Even after the acute phase, follow-up appointments with the treating physician or specialists are crucial to ensure complete resolution and monitor for recurrence, each visit contributing to the overall direct medical cost.
Indirect Financial Costs: The Price of Lost Productivity
Beyond the explicit medical bills, cellulitis imposes a substantial burden through indirect financial costs, primarily stemming from lost productivity and personal disruption. These costs are often overlooked but can have a profound impact on an individual’s or family’s financial stability.
When battling an infection like cellulitis, an individual is often too unwell to perform their work duties. This translates directly into lost wages for hourly workers or a reduction in income for self-employed individuals and small business owners. Depending on the severity and duration of the illness, days or even weeks of missed work can significantly deplete savings or lead to immediate income shortfalls. For those with paid sick leave, the impact might be softened in the short term, but prolonged illness can exhaust these benefits, forcing reliance on unpaid leave or short-term disability, which typically provides only a fraction of regular income.
The disruption extends beyond the affected individual. If the patient is a primary caregiver for children, elderly relatives, or dependents with special needs, their illness can necessitate hiring temporary care services. The costs of childcare, home health aides, or other support services can quickly accumulate, adding to the financial strain. For family members who take time off work to care for the infected individual, their lost wages become another indirect cost.
Moreover, the long-term impact on career progression should not be underestimated. Frequent or prolonged absences due to recurring cellulitis or complications can lead to reduced performance reviews, missed promotion opportunities, or even job insecurity. While these are harder to quantify in immediate financial terms, their cumulative effect on lifetime earning potential can be substantial. For small business owners, an illness can mean lost contracts, operational disruption, and damage to business reputation, all of which have direct financial consequences.
Navigating Healthcare Costs: Insurance, Out-of-Pocket, and Aid
Managing the financial fallout of cellulitis requires a proactive approach to understanding healthcare systems and available resources. A well-informed strategy can significantly alleviate the economic pressure.
Understanding Your Insurance Coverage
Health insurance is the primary buffer against exorbitant medical costs. However, simply having insurance is not enough; understanding its nuances is critical. Individuals must familiarize themselves with their policy’s specifics, including deductibles, co-pays, and out-of-pocket maximums. The deductible is the amount you must pay out of pocket before your insurance starts to cover costs. Co-pays are fixed amounts paid for specific services, like doctor visits. The out-of-pocket maximum is the most you’ll have to pay in a plan year for covered services before your health insurance pays 100% of the cost. A severe case of cellulitis, especially with hospitalization, can easily push individuals towards their out-of-pocket maximum, making it vital to know this limit.
It’s also crucial to distinguish between in-network and out-of-network providers. Using out-of-network services often results in higher costs or lower insurance coverage, as the insurer may pay a smaller percentage or not cover them at all. Before receiving care, if possible, verify that the doctors, facilities, and even specific specialists (like anesthesiologists in a hospital setting) are within your insurance network. For planned follow-ups, ensuring pre-authorization for certain treatments or tests can prevent denied claims and unexpected bills. Regularly reviewing your Explanation of Benefits (EOB) statements from your insurer allows you to track charges and identify any discrepancies or potential overbilling.
Strategies for Managing Out-of-Pocket Expenses
Even with robust insurance, out-of-pocket expenses for cellulitis can be substantial. Employing various strategies can help manage these costs effectively.
One key strategy is negotiation. Hospitals and providers often have charity care policies or financial assistance programs, especially for those with lower incomes or significant medical debt. It’s always worth inquiring about discounted rates for uninsured patients or payment plans that can spread the cost over several months or years without interest. Reviewing itemized bills for errors is also crucial; medical billing can be complex and mistakes happen.
Utilizing healthcare savings accounts (HSAs) or flexible spending accounts (FSAs) can provide a tax-advantaged way to save for medical expenses. Contributions to these accounts are pre-tax, reducing your taxable income, and funds can be used for eligible medical expenses, including deductibles, co-pays, and prescriptions. For those facing extreme financial hardship, exploring state-specific programs, Medicaid, or non-profit organizations that offer assistance for medical bills can provide a vital safety net.
Prevention as a Financial Strategy: Avoiding Costly Complications
The old adage “an ounce of prevention is worth a pound of cure” holds significant financial weight when it comes to conditions like cellulitis. Proactive health management is not just about physical well-being; it’s a powerful financial strategy to avoid potentially crippling costs.
Proactive Health Management
Minimizing the risk of developing cellulitis, or catching it early, can save individuals thousands of dollars in medical bills and lost income. One of the most effective preventive measures is early symptom recognition. Cellulitis often starts subtly, but rapid progression is common. Being aware of the early signs—a small area of redness, swelling, tenderness, or warmth—allows for prompt medical consultation. Timely treatment with oral antibiotics in the initial stages can prevent the infection from escalating, averting the need for hospitalization and more aggressive, costly interventions.
Good hygiene and meticulous wound care are paramount. Cellulitis typically occurs when bacteria enter the skin through a break, such as a cut, scrape, insect bite, surgical incision, or athlete’s foot. Regularly cleaning and protecting wounds, no matter how small, with antiseptic and sterile dressings can significantly reduce the risk of bacterial entry. Keeping skin moisturized can also prevent cracking, another potential entry point for bacteria.
Managing underlying health conditions is another critical aspect of prevention. Individuals with chronic conditions like diabetes, lymphedema (swelling due to fluid buildup), or peripheral artery disease are at a higher risk for cellulitis. Poorly controlled diabetes can impair the immune system and delay wound healing, making infections more likely. Lymphedema creates an environment where fluid accumulation makes tissues more susceptible to infection. Diligently managing these conditions through medication adherence, regular medical check-ups, and lifestyle adjustments directly contributes to preventing cellulitis and, consequently, its associated financial burdens.
The Cost-Benefit of Early Intervention
The financial disparity between early intervention and delayed treatment for cellulitis is staggering. A simple, timely course of oral antibiotics, costing perhaps a few hundred dollars, stands in stark contrast to the expenses associated with advanced infection. Left untreated, cellulitis can rapidly spread, leading to severe complications that are not only life-threatening but also incredibly expensive to manage.
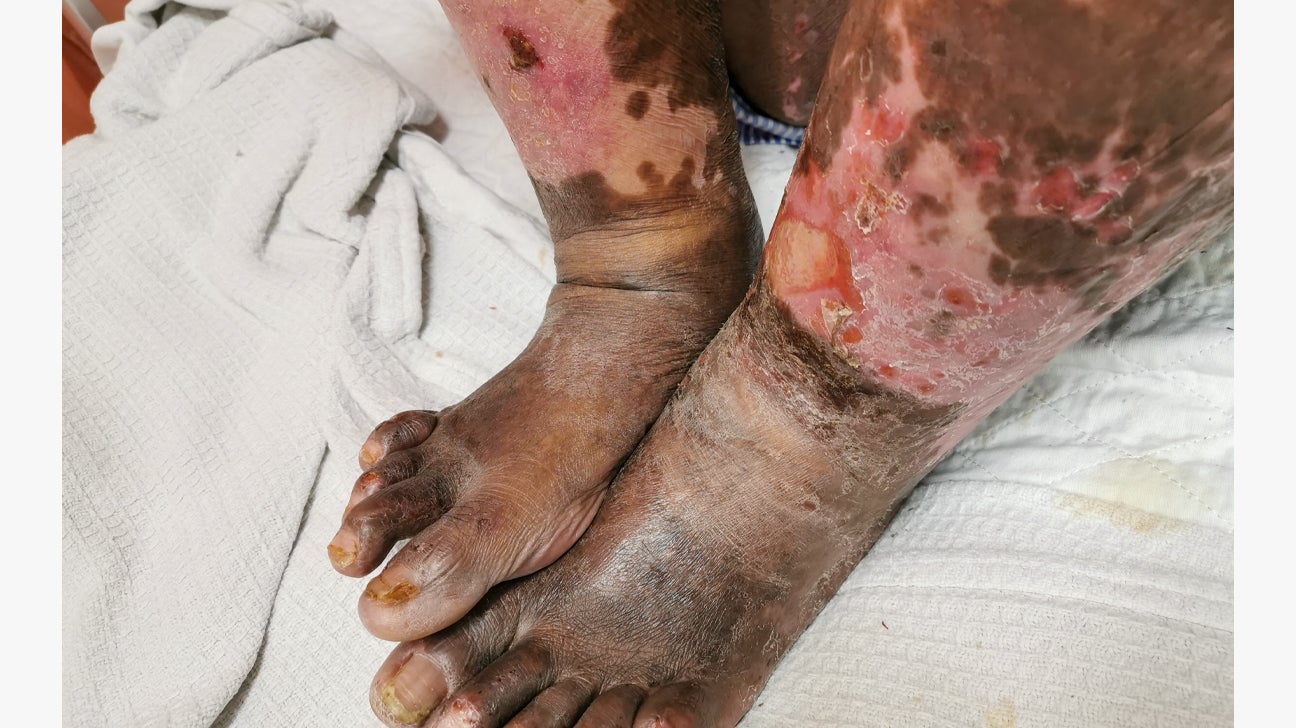
Complications such as abscess formation requiring surgical drainage, osteomyelitis (bone infection), sepsis (a life-threatening response to infection), or even necrotizing fasciitis (a flesh-eating bacterial infection) necessitate prolonged hospital stays, intensive care, complex surgical procedures, and extended rehabilitation. The costs for such severe conditions can skyrocket into tens or hundreds of thousands of dollars, placing an insurmountable financial strain on most individuals. In extreme cases, severe, untreated infections can lead to amputation, incurring not only the immediate surgical and hospitalization costs but also long-term expenses for prosthetics, physical therapy, and potential inability to return to previous employment, creating a lifelong financial impact.
Therefore, the investment in early medical attention—a doctor’s visit and a course of antibiotics—is a highly cost-effective financial decision. It protects against future, exponentially higher medical bills, preserves income by minimizing time off work, and safeguards overall financial stability.
Financial Preparedness for Unexpected Health Events
While preventing cellulitis is ideal, unexpected health crises can still occur. Being financially prepared is a cornerstone of robust personal finance, especially when facing unpredictable medical events.
Building an Emergency Fund
One of the most fundamental principles of personal finance is establishing and maintaining an emergency fund. This fund, typically comprising three to six months’ worth of essential living expenses, acts as a crucial buffer against unforeseen financial shocks, including medical emergencies like cellulitis. When faced with hospital bills, prescription costs, or lost income due to illness, an adequately stocked emergency fund prevents individuals from falling into debt, liquidating investments prematurely, or compromising other financial goals.
For those prone to health issues or with high-deductible insurance plans, it might even be prudent to aim for a larger emergency fund, specifically earmarking a portion for medical out-of-pocket expenses. Regularly contributing to this fund, even small amounts, can build significant resilience over time. Reviewing the fund’s adequacy annually, especially after any major life changes or shifts in health insurance coverage, ensures it remains a robust safety net.
Reviewing and Optimizing Your Health Insurance
Health insurance is a complex product that requires regular scrutiny. Annual policy reviews are essential, ideally during the open enrollment period. This allows individuals to compare their current plan against alternatives offered by their employer or on the marketplace. Consider factors such as changes in deductibles, co-pays, out-of-pocket maximums, and network providers. If you or a family member have developed a chronic condition or increased risk factors (like frequent skin breaks), a plan with a lower deductible or more comprehensive coverage for specialists might be a more financially sound choice, despite potentially higher monthly premiums.
Understanding changes in benefits, especially for prescription drug coverage, is also critical. A shift in formulary could mean a commonly used antibiotic suddenly moves to a higher co-pay tier or is no longer covered. Proactively engaging with your insurance provider to understand your benefits and how they apply to potential medical scenarios can empower you to make informed decisions that optimize your coverage and minimize future financial surprises.
In conclusion, while the core of “what is cellulite infection” lies in its medical definition, its financial ramifications are equally profound and deserve careful consideration. From direct costs of diagnosis and treatment to indirect losses from missed work and the long-term impact on financial stability, cellulitis represents a significant economic challenge. By understanding these costs, proactively managing health, diligently utilizing insurance, and building a strong financial safety net, individuals can better navigate the financial landscape of unexpected health events, ultimately safeguarding both their health and their wealth.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.