The Body Mass Index (BMI) has long been a cornerstone of health assessments, a seemingly simple ratio of weight to height intended to categorize individuals into weight groups. For decades, health professionals and individuals alike have relied on BMI as a quick and accessible metric to gauge potential health risks associated with weight. However, the question of what constitutes an “ideal” BMI is far more nuanced than a single number might suggest. This article will delve into the complexities surrounding BMI, exploring its origins, its limitations, and how technological advancements are shaping a more personalized and accurate approach to understanding our body composition and its implications for our health.
The Historical Foundation and Widespread Adoption of BMI
The concept of BMI, while now a global health standard, has a surprisingly complex and non-medical origin story. Understanding its genesis is crucial to appreciating its widespread adoption and, subsequently, its limitations.
From Quetelet’s Index to a Health Metric
The foundation of BMI can be traced back to the mid-19th century and the work of Adolphe Quetelet, a Belgian mathematician and astronomer. Quetelet was interested in studying human physical characteristics and developed a statistical index that related weight to height squared. His goal was not to diagnose individual health but rather to understand population averages and variations in physique.
In the early 20th century, this Quetelet index began to be adopted by the insurance industry. Companies recognized that individuals at the extremes of weight—both underweight and overweight—tended to have higher mortality rates. BMI offered a convenient way to stratify risk among their policyholders. This practical application in the insurance sector paved the way for its broader use.
The WHO’s Endorsement and Global Influence
The World Health Organization (WHO) officially adopted the BMI as a standard for classifying weight categories in the late 20th century. This endorsement was pivotal. It provided a universally recognized framework for public health initiatives, epidemiological studies, and clinical assessments worldwide. The simplicity of the calculation—weight in kilograms divided by height in meters squared—made it easily accessible for large-scale data collection and comparison.
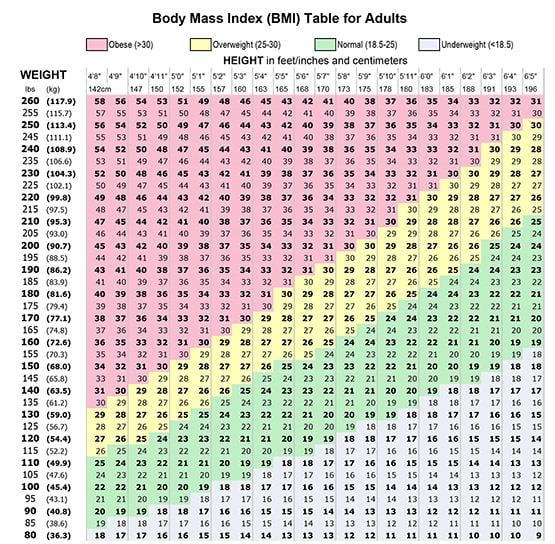
The established BMI ranges became widely publicized:
- Underweight: BMI < 18.5
- Normal or Healthy Weight: 18.5 to 24.9
- Overweight: 25.0 to 29.9
- Obese: BMI ≥ 30.0
These categories offered a seemingly clear-cut way for individuals to understand their weight status and, by extension, their potential health risks. This ubiquitous presence in health campaigns, doctor’s offices, and public discourse has solidified BMI’s status as the go-to metric for assessing weight-related health.
The Evolving Understanding: Beyond the Simple Ratio
While BMI has served a valuable purpose in broad population studies and as an initial screening tool, its limitations have become increasingly apparent as our understanding of human physiology and body composition has advanced. The “ideal” BMI is not a universal constant but rather a spectrum influenced by a multitude of individual factors.
The Muscle vs. Fat Dilemma
One of the most significant criticisms of BMI is its inability to differentiate between lean body mass (muscle) and fat mass. Muscle is denser than fat, meaning an individual with a high muscle mass, such as an athlete or someone engaged in regular strength training, could have a BMI that falls into the “overweight” or even “obese” category, despite having a low percentage of body fat and being perfectly healthy. Conversely, a sedentary individual with a “normal” BMI might have a high percentage of body fat and low muscle mass, putting them at increased risk for certain health conditions.
This distinction is critical because it’s the amount and distribution of body fat, rather than just total body weight, that is most closely linked to many health risks. Visceral fat, the fat that surrounds internal organs, is particularly metabolically active and associated with increased risks of heart disease, type 2 diabetes, and other metabolic disorders. BMI, by itself, cannot reveal this crucial information.
Age, Sex, and Ethnicity as Modifying Factors
The ideal BMI range is not static and can vary based on demographic factors.
-
Age: As people age, their body composition naturally changes. Muscle mass tends to decrease, and fat mass may increase, even if total weight remains stable. Therefore, what might be considered a healthy BMI for a younger adult might be less indicative for an older adult. Furthermore, some research suggests that a slightly higher BMI might even be protective in older populations, offering a buffer against illness and injury.
-
Sex: Men and women tend to have different body compositions. On average, women have a higher percentage of body fat than men, which is biologically necessary for reproduction. This can mean that a BMI that is considered healthy for a woman might be slightly lower for a man.
-
Ethnicity: Emerging research indicates that the relationship between BMI, body fat percentage, and health outcomes can differ across various ethnic groups. For instance, some studies suggest that individuals of South Asian descent may be at higher risk for cardiovascular disease at a lower BMI compared to individuals of European descent. Similarly, individuals of African descent may have greater bone density and muscle mass, potentially leading to higher BMIs without increased health risks. These differences highlight the need for a more nuanced, culturally sensitive approach to health assessment.
The Importance of Body Composition and Distribution
Beyond the overall BMI number, understanding what makes up that number is paramount. Advanced body composition analysis tools provide a more detailed picture than BMI alone. These tools can measure:
- Body Fat Percentage: The proportion of your total weight that is fat.
- Lean Body Mass: The weight of everything in your body that isn’t fat, including muscle, bone, water, and organs.
- Visceral Fat Level: The amount of fat surrounding your internal organs.
- Muscle Distribution: Where your muscle mass is located.
By considering these factors, individuals and healthcare providers can gain a more accurate assessment of health risks. For example, someone with a BMI of 26 but a healthy body fat percentage and no excess visceral fat might be at lower risk than someone with a BMI of 24 who carries a significant amount of visceral fat.
Technological Advancements Shaping the Future of Health Assessment
The limitations of BMI have spurred innovation in health technology, leading to the development of more sophisticated tools that offer a personalized and dynamic approach to understanding individual health. These advancements are moving us beyond generalized metrics towards data-driven insights.
From Scales to Smart Devices: The Rise of Body Composition Analysis
The most significant technological leap has been in the accessibility and accuracy of body composition analysis.

-
Bioelectrical Impedance Analysis (BIA) Scales: These increasingly common smart scales use low-level electrical currents to estimate body fat, muscle mass, and water content. While accuracy can vary, modern BIA scales, especially those from reputable brands, provide a much richer dataset than a simple weight reading. They allow individuals to track trends in their body composition over time, offering valuable insights into the effectiveness of diet and exercise.
-
Dual-energy X-ray Absorptiometry (DXA) Scans: Considered a gold standard for body composition analysis, DXA scans are more accurate than BIA and can also measure bone mineral density. While historically only available in clinical settings, the cost and accessibility of DXA are slowly improving, making it a more viable option for individuals seeking precise measurements.
-
Near-Infrared Interactance (NIR) Devices: Emerging technologies are also exploring the use of near-infrared light to assess body composition. These non-invasive methods are being developed for potential use in clinical settings and even portable devices.
These technologies empower individuals to move beyond the single BMI number and engage with a more comprehensive understanding of their physical well-being.
Wearable Technology and Personalized Health Insights
Wearable devices, such as smartwatches and fitness trackers, have become ubiquitous. Beyond step counting and heart rate monitoring, many of these devices are integrating more advanced health sensors.
-
Activity and Calorie Tracking: By monitoring activity levels, heart rate, and sleep patterns, wearables provide data that can inform personalized calorie expenditure estimates and activity recommendations. This data, when correlated with diet logs, offers a holistic view of energy balance.
-
Heart Health Monitoring: Advanced wearables can track heart rate variability, detect irregular heart rhythms (like atrial fibrillation), and even provide electrocardiogram (ECG) readings. This provides early warning signs for cardiovascular issues, which are often linked to weight.
-
Integration with Health Apps: The true power of wearables lies in their integration with sophisticated health and wellness applications. These apps can aggregate data from multiple sources, including BIA scales, fitness trackers, and even genetic testing services, to provide personalized recommendations for diet, exercise, and lifestyle modifications. They can help individuals set realistic health goals based on their unique physiology and track their progress in a meaningful way.
AI and Machine Learning in Health Risk Prediction
Artificial intelligence (AI) and machine learning (ML) are poised to revolutionize how we interpret health data, including BMI.
-
Predictive Analytics: AI algorithms can analyze vast datasets that include BMI, body composition, genetic predispositions, lifestyle factors, and medical history to predict an individual’s risk for developing specific chronic diseases. This allows for proactive interventions tailored to an individual’s unique risk profile.
-
Personalized Nutrition and Exercise Plans: ML models can learn from an individual’s responses to different diets and exercise regimens to generate highly personalized and adaptive plans that optimize outcomes and adherence. Instead of a generic “eat less, move more” approach, AI can suggest specific macronutrient ratios, exercise types, and intensities that are most effective for that individual.
-
Bias Correction and Refinement: As AI systems are trained on diverse datasets, they have the potential to identify and mitigate biases inherent in traditional metrics like BMI. This could lead to more equitable and accurate health assessments for all populations.
Redefining “Ideal”: A Personalized and Holistic Approach
The pursuit of an “ideal” BMI is gradually giving way to a more sophisticated understanding of health and well-being. Technology is instrumental in this shift, moving us from a one-size-fits-all approach to highly personalized, data-driven strategies.
Beyond the Number: Focusing on Health Behaviors and Outcomes
The emphasis is shifting from achieving a specific number on the scale to cultivating healthy habits and achieving positive health outcomes. This means:
-
Prioritizing Sustainable Lifestyle Changes: Instead of crash diets or extreme exercise routines, the focus is on building consistent, sustainable habits that can be maintained long-term. This includes balanced nutrition, regular physical activity, adequate sleep, and stress management.
-
Monitoring Health Markers Beyond BMI: While BMI can be an initial indicator, it’s crucial to monitor a broader range of health markers. This includes blood pressure, cholesterol levels, blood glucose, waist circumference, and body fat percentage. These metrics provide a more comprehensive picture of cardiovascular and metabolic health.
-
Understanding Individual Variability: Recognizing that there is no single “ideal” BMI for everyone is paramount. What is optimal for one person might be suboptimal for another, depending on genetics, lifestyle, and individual health goals.
The Role of Healthcare Professionals in the New Landscape
Healthcare professionals are increasingly leveraging technology to provide more personalized care.
-
Utilizing Advanced Diagnostic Tools: Doctors and dietitians are incorporating BIA, DXA, and other body composition analyses into their assessments. This allows them to move beyond basic BMI calculations and offer more targeted advice.
-
Leveraging Health Data Platforms: The integration of wearable data and health app information allows clinicians to have a more complete picture of their patients’ daily lives, enabling more informed conversations and interventions.
-
Emphasizing Education and Empowerment: A key role for healthcare providers is to educate patients about the limitations of BMI and the benefits of understanding their unique physiology. Empowering individuals with knowledge fosters greater self-advocacy and engagement in their health journeys.
Setting Realistic and Achievable Health Goals
The concept of an “ideal BMI” can be a source of anxiety and unrealistic expectations. A more constructive approach involves setting personalized health goals that are:
- Measurable: Based on tangible improvements in body composition, health markers, or physical performance.
- Achievable: Realistic and attainable within a reasonable timeframe.
- Relevant: Aligned with individual values and long-term health objectives.
- Time-bound: With defined milestones and target dates.
For example, instead of aiming for a BMI of 22, an individual might set a goal to reduce their body fat percentage by 5% over six months, improve their cardiovascular endurance by being able to run a 5K, or maintain consistent healthy eating habits for 80% of the week.
In conclusion, the question of “what’s the ideal BMI” is evolving. While BMI remains a useful starting point, the future of health assessment lies in leveraging technology to gain a deeper, more personalized understanding of our bodies. By embracing advanced diagnostics, wearable technology, and AI-driven insights, we can move beyond generalized metrics to cultivate truly holistic and sustainable well-being, where the “ideal” is not a number, but a state of thriving health tailored to each unique individual.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.