The question of “What percentage of the US population is obese?” is far more than a simple public health statistic. It is a powerful indicator of societal well-being that carries profound economic implications. Beyond the individual health consequences, the pervasive issue of obesity in the United States translates into staggering financial burdens, impacting healthcare systems, productivity, and overall economic growth. Understanding the scale of this problem is the first step toward grasping its multifaceted economic ramifications.
The Shifting Landscape: Defining and Quantifying Obesity in the US
Before delving into the economic fallout, it’s crucial to establish a clear understanding of what constitutes obesity and how its prevalence is measured. This foundational knowledge helps frame the scale of the challenge and its subsequent financial weight.
Defining Obesity: Beyond a Number
The most widely accepted definition of obesity is based on the Body Mass Index (BMI). BMI is a measure that uses a person’s weight and height to estimate body fat. A BMI of 30 or higher is generally classified as obese. It’s important to acknowledge that BMI is a screening tool and doesn’t directly measure body fat, nor does it account for muscle mass or other individual physiological differences. However, at a population level, it remains the most practical and consistent metric for tracking trends.
Tracking the Tide: Prevalence Rates and Trends
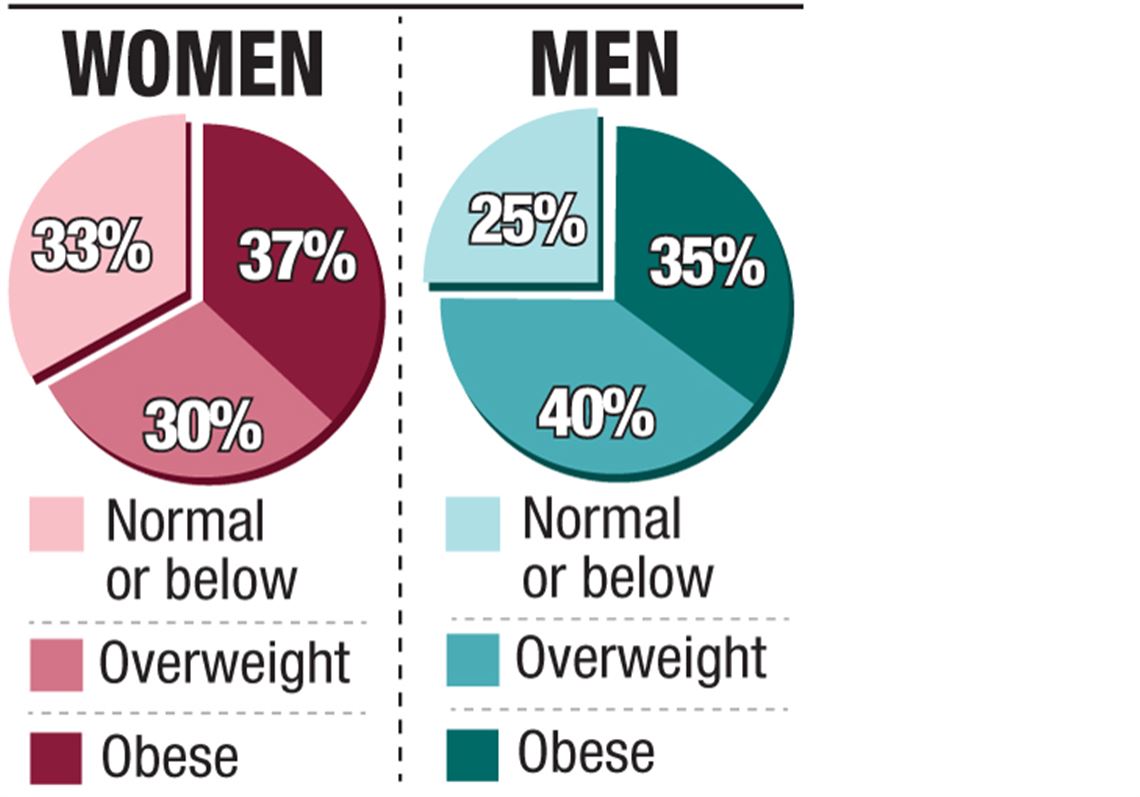
Over the past few decades, the United States has witnessed a dramatic increase in obesity rates. Data from the Centers for Disease Control and Prevention (CDC) consistently paints a concerning picture. While specific percentages fluctuate slightly based on the survey year and methodology, general trends are undeniable. Recent figures indicate that approximately 40% of US adults are classified as obese. This represents a significant portion of the adult population, translating into tens of millions of individuals.
Furthermore, the problem is not confined to adults. Childhood and adolescent obesity rates have also escalated alarmingly, setting the stage for long-term health and economic challenges. The persistence of these high rates signifies a deeply entrenched societal issue with compounding financial consequences.
The Economic Ripple Effect: Obesity’s Financial Footprint
The sheer number of individuals classified as obese in the US translates into a substantial and multifaceted economic burden. This burden is felt across various sectors, from direct healthcare expenditures to indirect costs associated with reduced productivity and workforce participation.
Healthcare Costs: The Direct Financial Drain
The most immediate and tangible economic impact of obesity stems from increased healthcare utilization and costs. Individuals with obesity are at a significantly higher risk for a myriad of chronic health conditions, including but not limited to:
- Type 2 Diabetes: A chronic condition that requires ongoing management, including medication, regular monitoring, and potential complications like kidney disease, nerve damage, and blindness.
- Heart Disease and Stroke: Obesity is a major risk factor for hypertension, high cholesterol, and atherosclerosis, all of which contribute to cardiovascular events.
- Certain Types of Cancer: Studies have linked obesity to an increased risk of developing several types of cancer, including breast, colon, and endometrial cancers.
- Osteoarthritis: Excess body weight places increased stress on joints, leading to pain, mobility issues, and the need for medical interventions such as physical therapy and joint replacement surgery.
- Sleep Apnea: A sleep disorder that can lead to daytime fatigue, impaired cognitive function, and increased risk of cardiovascular problems.
These conditions necessitate more frequent doctor’s visits, hospitalizations, diagnostic tests, prescription medications, and surgical procedures. The cumulative cost of treating these obesity-related comorbidities is astronomical. Estimates consistently place the annual healthcare spending directly attributable to obesity in the United States in the hundreds of billions of dollars. This massive expenditure strains not only individual household budgets but also the financial stability of insurance providers and government healthcare programs like Medicare and Medicaid.
Lost Productivity and Workforce Impact: The Hidden Costs

Beyond direct medical expenses, the economic toll of obesity extends to lost productivity and its impact on the workforce. Health issues associated with obesity can lead to:
- Increased Absenteeism: Employees struggling with obesity-related health problems are more likely to take time off from work due to illness, appointments, or recovery from procedures. This lost work time directly affects business output and profitability.
- Presenteeism: Even when employees are at work, they may be less productive due to pain, fatigue, or cognitive impairments stemming from their health conditions. This “presenteeism” is often harder to quantify but represents a significant drain on economic output.
- Reduced Work Capacity: In some cases, obesity can lead to limitations in physical capacity, impacting job performance and potentially limiting an individual’s ability to perform certain tasks or engage in physically demanding roles. This can lead to reduced earning potential and career advancement opportunities.
- Disability and Early Retirement: For individuals whose health conditions become severe, disability benefits and early retirement can become necessary. This removes experienced workers from the labor force and places a financial burden on social security systems.
The collective impact of these productivity losses translates into billions of dollars in lost economic output annually. Businesses face higher costs associated with managing employee health and reduced efficiency, while the broader economy suffers from a less productive workforce.
The Burden on Public Finances: Beyond Direct Healthcare
The financial repercussions of obesity are not limited to private healthcare spending. Public finances bear a significant portion of this burden.
- Government Healthcare Programs: As mentioned, Medicare and Medicaid, which serve a large proportion of the elderly and low-income populations, are heavily impacted by the costs of treating obesity-related diseases. The rising prevalence of these conditions puts immense pressure on the budgets of these vital public programs, potentially leading to increased taxes or reduced services.
- Disability and Social Security: The increase in obesity-related disabilities contributes to higher payouts from Social Security and other disability programs, further straining public resources.
- Public Health Initiatives: While often underfunded, public health campaigns and initiatives aimed at preventing and managing obesity are necessary investments. The cost of these programs, while intended to mitigate future expenses, represents an upfront financial commitment.
The interconnectedness of these financial streams means that the economic impact of obesity is a complex web, with consequences rippling through individual households, corporate balance sheets, and government budgets alike.
Addressing the Economic Challenge: Strategies and Investments
Recognizing the profound economic implications of obesity is a critical motivator for implementing effective solutions. Investing in prevention and treatment is not just a public health imperative; it is a sound economic strategy that can yield significant returns.
Prevention: An Ounce of Prevention is Worth Pounds of Cure
The most economically sensible approach to tackling obesity is through robust prevention strategies. Investing in initiatives that promote healthy lifestyles from an early age can have a lasting impact on both individual well-being and national economic health.
- Promoting Healthy Diets: Education on nutrition, making healthy food options more accessible and affordable, and implementing policies that discourage the consumption of unhealthy, calorie-dense foods (e.g., taxes on sugary drinks) can significantly impact dietary habits.
- Encouraging Physical Activity: Creating safe and accessible environments for physical activity, promoting active transportation, and integrating physical education into school curricula are vital. This includes investing in parks, recreational facilities, and community programs.
- Early Childhood Interventions: Addressing unhealthy weight gain in infants, toddlers, and young children sets a foundation for healthier lifelong habits. This can involve parental education, access to nutritious food programs for families, and early screening for weight-related health issues.
- Workplace Wellness Programs: Businesses can play a crucial role by implementing comprehensive wellness programs that encourage healthy eating, physical activity, and stress management among employees. These programs can lead to reduced healthcare costs and improved productivity for the company.
Treatment and Management: Reducing the Financial Burden
While prevention is paramount, effective treatment and management of obesity and its associated comorbidities are also essential to mitigate the ongoing economic drain.
- Access to Evidence-Based Interventions: Ensuring access to affordable and effective weight management programs, including nutritional counseling, behavioral therapy, and, where appropriate, medical or surgical interventions, is crucial.
- Integrated Healthcare Models: A more integrated approach to healthcare that addresses obesity as a chronic disease and incorporates prevention, screening, and management into routine medical care can lead to better outcomes and more efficient resource allocation.
- Technological Innovations in Health Management: The role of technology in supporting weight management and chronic disease care is growing. This includes health tracking apps, wearable devices that monitor activity and vital signs, telehealth services for remote consultations and support, and AI-powered personalized health plans. While these tools have development and adoption costs, their ability to empower individuals and facilitate continuous monitoring can lead to improved adherence to treatment plans and potentially reduce long-term healthcare expenditures.
The Economic Case for Action: A Long-Term Investment
The data unequivocally points to the substantial economic burden imposed by obesity in the United States. The costs are borne by individuals, businesses, and the government, impacting everything from personal finances to national economic competitiveness. By investing in comprehensive prevention and effective treatment strategies, the US can not only improve the health and well-being of its citizens but also realize significant long-term economic benefits through reduced healthcare spending, increased productivity, and a healthier, more robust workforce. The question is no longer if we can afford to address obesity, but rather, can we afford not to? The financial returns on investing in a healthier nation are undeniable.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.
