The delicate balance of blood glucose, often referred to as blood sugar, is a cornerstone of our physiological well-being. While the perils of elevated blood sugar (hyperglycemia) are widely discussed in the context of diabetes and metabolic health, the phenomenon of blood sugar dropping too low, or hypoglycemia, is equally critical and can pose immediate, and sometimes severe, health risks. Understanding the triggers for hypoglycemia is not just an academic exercise; it’s an essential component of proactive health management, particularly for individuals with diabetes, but also for those who may experience reactive hypoglycemia. This article delves into the multifaceted causes of blood sugar drops, exploring the intricate interplay of diet, lifestyle, medication, and underlying physiological responses that can lead to this state.
The Carbohydrate Conundrum: Fueling the Drop
Our bodies primarily utilize carbohydrates for immediate energy, breaking them down into glucose which then enters the bloodstream. The rate at which this occurs, and the subsequent insulin response, plays a pivotal role in preventing blood sugar fluctuations. However, certain dietary choices can inadvertently set the stage for a hypoglycemic event.
The Impact of Fast-Digesting Carbohydrates
The glycemic index (GI) is a valuable tool for understanding how quickly different carbohydrate-containing foods raise blood sugar levels. Foods with a high GI, such as white bread, sugary cereals, fruit juices, and candy, are rapidly digested and absorbed, leading to a swift spike in blood glucose. In response, the pancreas releases a proportional amount of insulin to help cells absorb this glucose. The challenge arises when this insulin response is particularly robust or when the carbohydrate intake is followed by a period of reduced physical activity. The excess insulin can effectively “over-lower” blood sugar, leading to a dip below normal levels. This can feel like a sudden crash, accompanied by symptoms of shakiness, dizziness, and fatigue, often occurring a couple of hours after consuming these high-GI foods.
Insufficient Carbohydrate Intake and Skipping Meals
Conversely, not consuming enough carbohydrates, or skipping meals altogether, can also lead to a drop in blood sugar. When the body hasn’t received a sufficient supply of glucose from food, it has to rely on stored glucose (glycogen) in the liver and muscles. If these stores are depleted, or if the body needs more energy than is readily available, blood sugar levels can fall. This is particularly relevant for individuals managing diabetes who may be on medication that lowers blood sugar, as a missed meal can exacerbate the effect of their treatment. For those without diabetes, a prolonged period without food can still lead to mild hypoglycemia, especially if they engage in physical activity during this time. The body interprets the lack of external fuel as a signal to conserve energy, but this conservation can sometimes overshoot, leading to a drop in glucose.
The Role of Alcohol Consumption
Alcohol consumption, especially on an empty stomach or in excessive amounts, can significantly contribute to blood sugar drops. While alcohol itself does not contain carbohydrates, its metabolism by the liver interferes with the liver’s ability to release stored glucose. Normally, when blood sugar levels start to fall, the liver releases glucose into the bloodstream to bring them back up. However, when the liver is busy processing alcohol, this crucial glucose-releasing function is impaired. This can lead to a delayed and prolonged drop in blood sugar, which can be particularly dangerous because the symptoms of hypoglycemia can be mistaken for intoxication, potentially delaying necessary intervention. The risk is amplified for individuals with diabetes who are taking insulin or certain oral diabetes medications, as alcohol can interact with these treatments to cause severe hypoglycemia.
The Influence of Physical Activity: Burning More Than Expected
Exercise is a cornerstone of a healthy lifestyle, playing a vital role in managing weight, improving cardiovascular health, and regulating blood sugar. However, the relationship between physical activity and blood sugar is nuanced, and certain aspects of exercise can precipitate a drop in glucose levels.
Increased Glucose Uptake by Muscles
During physical activity, muscles require more energy, and therefore more glucose, to function. This increased demand leads to greater glucose uptake from the bloodstream by muscle cells, independent of insulin in some cases. For individuals with diabetes who are using insulin or taking medications that enhance insulin sensitivity, this heightened glucose uptake can lead to a significant drop in blood sugar. The risk is particularly high if exercise is undertaken without adequate pre-exercise carbohydrate intake or if medication dosages are not adjusted accordingly. Even for individuals without diabetes, prolonged or intense exercise can deplete glycogen stores, potentially leading to hypoglycemia if not replenished.
The Timing and Intensity of Exercise
The timing of exercise relative to meals and medication is a critical factor. Exercising several hours after a meal, especially if that meal was rich in carbohydrates, can lead to a blood sugar drop as the body continues to process the digested food and the muscles are actively utilizing glucose. Similarly, engaging in intense exercise without sufficient fuel can rapidly deplete glucose reserves. The body’s adaptive responses to exercise can also contribute. For instance, after a bout of exercise, the body may become more sensitive to insulin for up to 24 hours, increasing the risk of delayed hypoglycemia. Understanding these temporal relationships and adjusting food and medication intake accordingly is paramount for preventing exercise-induced hypoglycemia.
The Effect of Delayed-Onset Muscle Soreness (DOMS)

While not a direct cause, delayed-onset muscle soreness (DOMS), the stiffness and pain experienced 24-72 hours after unaccustomed or strenuous exercise, can indirectly influence blood sugar control. During the repair process of damaged muscle tissue, the body may experience altered glucose metabolism. Some research suggests that muscle damage can lead to increased glucose uptake by the damaged muscle cells as they work to repair themselves. This increased utilization, even after the exercise itself has ceased, can contribute to lower blood sugar levels. Therefore, individuals prone to hypoglycemia should be aware that periods of DOMS might require closer monitoring of their blood sugar and potentially adjustments to their dietary intake.
Medications and Medical Conditions: The Unseen Triggers
Beyond diet and exercise, certain medications and underlying medical conditions can significantly impact blood sugar regulation, making individuals more susceptible to hypoglycemic episodes.
Insulin Therapy and Oral Diabetes Medications
For individuals managing type 1 and type 2 diabetes, insulin therapy and certain oral diabetes medications are designed to lower blood glucose levels. However, an improper dosage, incorrect timing, or unexpected changes in diet or activity can lead to an overdose of these medications, resulting in hypoglycemia. Insulin, a hormone that facilitates glucose uptake into cells, can cause blood sugar to drop too rapidly if too much is administered. Similarly, oral medications such as sulfonylureas and meglitinides stimulate the pancreas to release more insulin, and their effects can be exacerbated by insufficient food intake or increased physical activity. Glucagon-like peptide-1 (GLP-1) receptor agonists and DPP-4 inhibitors, while generally having a lower risk of hypoglycemia, can still contribute to it when combined with other glucose-lowering agents or under specific circumstances. Careful monitoring, patient education, and individualized treatment plans are crucial to mitigate this risk.
Other Medical Conditions
Certain medical conditions can predispose individuals to hypoglycemia. For example, pancreatic tumors known as insulinomas can overproduce insulin, leading to dangerously low blood sugar levels. Adrenal insufficiency, a condition where the adrenal glands do not produce enough essential hormones, can also affect glucose regulation, as these hormones play a role in maintaining blood sugar. Severe liver disease can impair the liver’s ability to store and release glucose, contributing to hypoglycemia. Kidney disease can also impact the clearance of certain diabetes medications, potentially leading to prolonged or excessive glucose-lowering effects. Rarer conditions, such as hormonal deficiencies, can also disrupt the delicate balance of blood sugar.
Bariatric Surgery and Postprandial Hypoglycemia
Bariatric surgery, procedures designed for weight loss, can significantly alter digestion and nutrient absorption, sometimes leading to a condition called dumping syndrome or, more specifically, postprandial hypoglycemia. In this scenario, food, particularly carbohydrates, moves too quickly from the stomach into the small intestine. This rapid transit causes a swift release of insulin to handle the sudden influx of glucose, often leading to an overshoot and a subsequent drop in blood sugar a few hours after eating. Symptoms can include dizziness, sweating, nausea, and confusion. Management often involves dietary modifications, such as eating smaller, more frequent meals and avoiding high-sugar foods.
Recognizing and Responding to Hypoglycemia
Understanding the causes of blood sugar drops is only the first step; recognizing the symptoms and knowing how to respond are crucial for preventing serious complications.
Common Symptoms of Low Blood Sugar
The symptoms of hypoglycemia can vary from person to person and can range from mild to severe. Early warning signs often include shakiness or trembling, sweating, rapid heartbeat, anxiety, and hunger. As blood sugar continues to drop, more significant symptoms can emerge, such as dizziness, confusion, irritability, blurred vision, headache, and difficulty concentrating. In severe cases, if left untreated, hypoglycemia can lead to seizures, loss of consciousness, and even coma. It’s important to note that individuals with long-standing diabetes may develop hypoglycemia unawareness, where they no longer experience the early warning signs, making regular blood glucose monitoring even more vital.
Immediate Management of Hypoglycemia
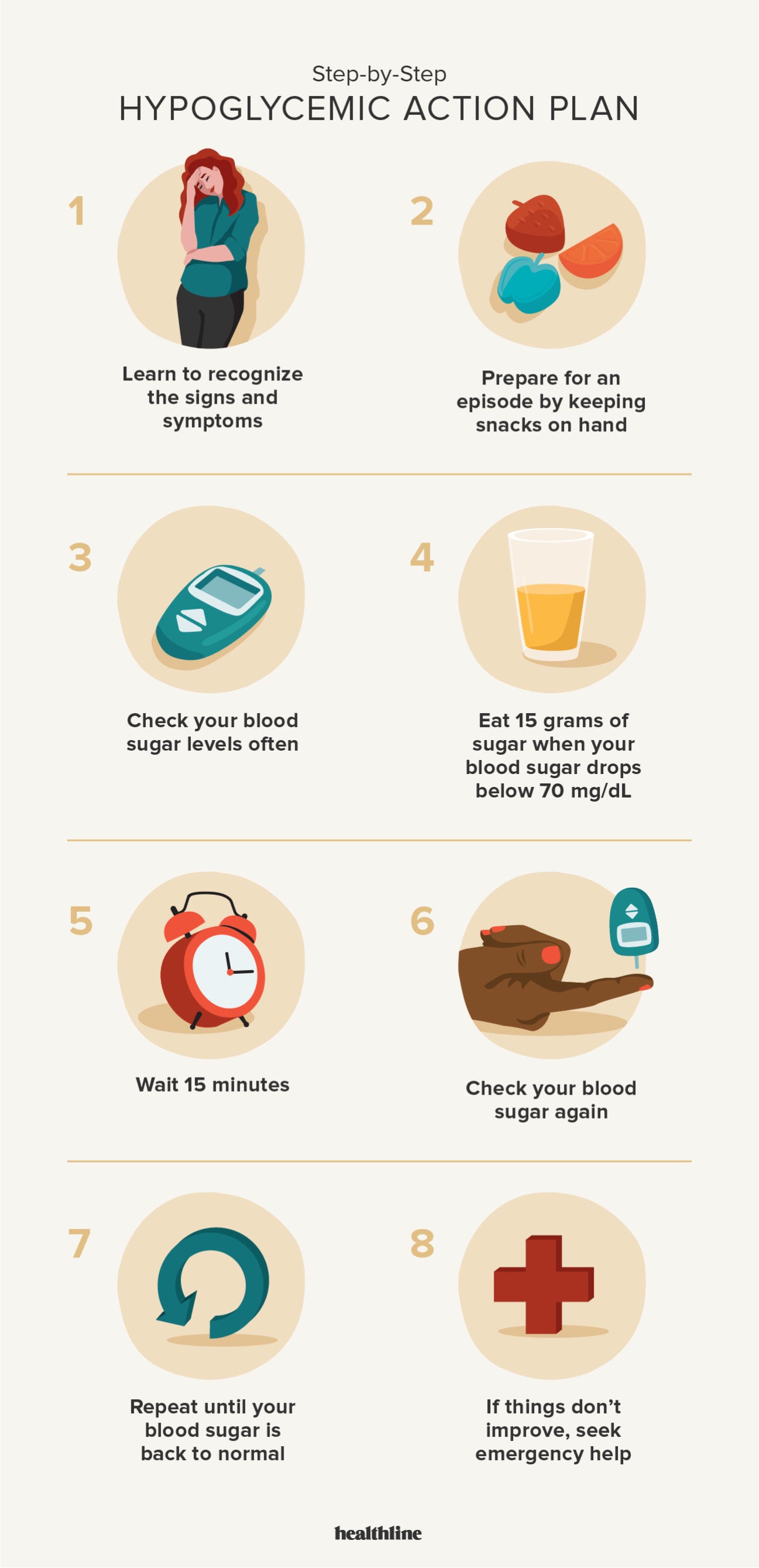
The primary goal in managing hypoglycemia is to quickly raise blood sugar levels. The “15-15 rule” is a widely recommended approach: consume 15 grams of fast-acting carbohydrates, such as glucose tablets, fruit juice, regular soda (not diet), or hard candy. Wait 15 minutes and recheck blood sugar. If it’s still low, repeat the process. Once blood sugar levels return to normal, it’s advisable to eat a more substantial snack or meal containing carbohydrates and protein to help stabilize glucose levels and prevent another drop. For individuals with a prescription for glucagon, an emergency hormone that raises blood sugar, it should be administered if the person is unable to consume anything by mouth or is unconscious, followed by immediate medical attention.

Long-Term Strategies for Prevention
Preventing recurrent episodes of hypoglycemia involves a multi-pronged approach. For individuals with diabetes, this means consistent blood glucose monitoring, adherence to medication schedules, balanced meal planning with consistent carbohydrate intake, and careful consideration of exercise. Educating oneself and one’s support network about the signs and management of hypoglycemia is also essential. For those experiencing reactive hypoglycemia, identifying trigger foods and adjusting dietary patterns to include more fiber and protein, and limiting high-GI carbohydrates, can be effective. Regular medical check-ups are vital to address any underlying conditions that may be contributing to blood sugar fluctuations and to ensure that treatment plans are optimized for individual needs. By understanding the intricate mechanisms that can lead to blood sugar drops and implementing appropriate preventative measures, individuals can significantly improve their health and well-being.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.