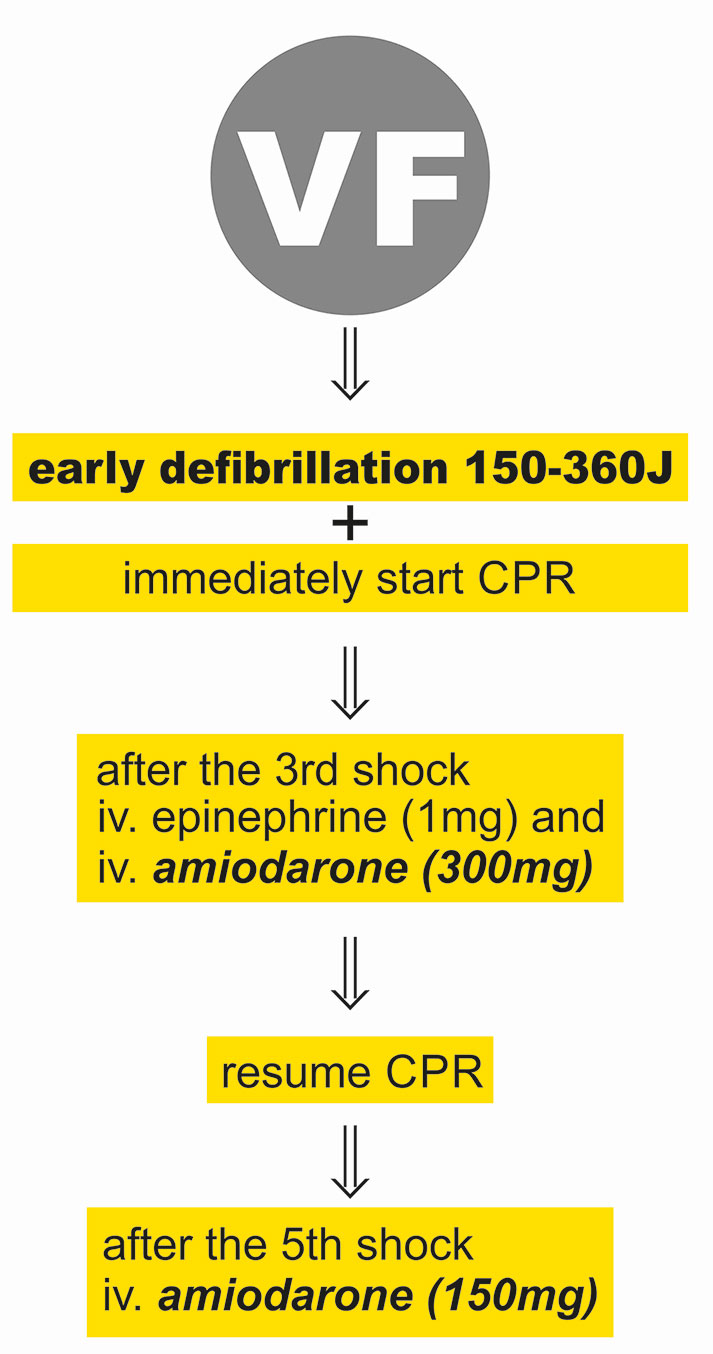
In the realm of emergency medicine, few conditions are as critical or as time-sensitive as ventricular fibrillation (VF). Often described as a “quivering” of the heart’s lower chambers, VF represents a total collapse of the heart’s electrical synchronization, leading to a cessation of effective blood flow. However, while the condition is biological, the solution is profoundly technological. For decades, the first-line treatment for ventricular fibrillation has been high-energy electrical defibrillation.
In the modern landscape, “defibrillation” is no longer just a manual medical procedure; it is a sophisticated intersection of hardware engineering, software algorithms, and digital connectivity. From the evolution of the Automated External Defibrillator (AED) to the integration of Artificial Intelligence (AI) in cardiac monitoring, technology serves as the primary frontline defense against sudden cardiac arrest.
The Evolution of Defibrillation Hardware: From Clinical Tools to Consumer Tech
The concept of shocking a heart back into rhythm has existed for over a century, but the technology that facilitates this has undergone a massive transformation. The shift from bulky, hospital-bound units to portable, intelligent devices has redefined how first-line treatment is delivered.
How Biphasic Waveform Technology Revolutionized Resuscitation
Earlier generations of defibrillators utilized monophasic waveforms, which delivered a high-energy current in one direction. While effective, this required significant voltage, which often caused thermal damage to the heart tissue. The technological breakthrough that changed the industry was the development of the “Biphasic Waveform.”
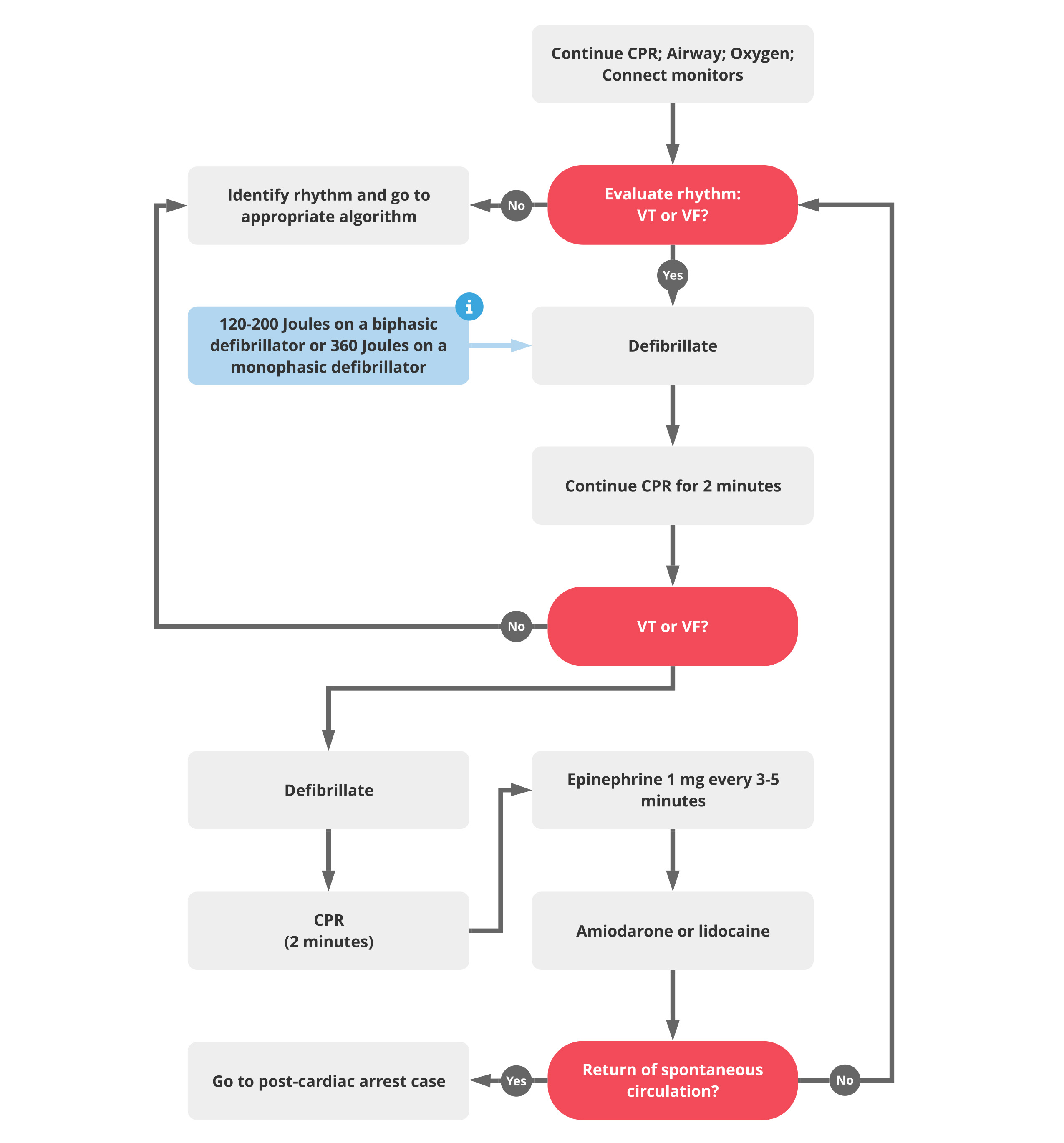
Modern AEDs use biphasic technology to deliver current in two directions. This allows the device to achieve successful defibrillation at lower energy levels (typically 120 to 200 joules compared to the 360 joules required for monophasic devices). This advancement in electrical engineering not only increases the safety of the treatment but also allows for smaller, more efficient capacitors and batteries, making the devices portable enough for public installations.
Smart Algorithms and User Interface Design
The “first-line” nature of the treatment depends on speed. Tech companies specializing in medical devices have focused heavily on the User Experience (UX) of AEDs. Today’s devices are “smart” units; they use advanced digital signal processing (DSP) to analyze the patient’s heart rhythm automatically.
The software within an AED must distinguish between “shockable” rhythms (like VF) and “non-shockable” rhythms (like asystole) with near 100% accuracy. This is achieved through complex pattern-recognition algorithms. Furthermore, the integration of voice prompts and visual cues guide non-technical users through the process, effectively turning a sophisticated piece of medical hardware into a fail-safe consumer gadget.
Wearable and Implantable Tech: The Proactive First Line of Defense
While the public AED is the first line of treatment for a witness to a cardiac event, for high-risk patients, the “first line” is often already inside them or on their skin. The miniaturization of components and the improvement of battery technology have led to the rise of internal and wearable sentinels.
Implantable Cardioverter Defibrillators (ICDs) as Internal Sentinels
The ICD is perhaps the pinnacle of proactive medical technology. These devices are essentially micro-computers implanted under the skin, with leads connecting directly to the heart. The ICD serves a dual purpose: it acts as a continuous monitor and an immediate treatment provider.
The technology within an ICD is designed to sense the onset of ventricular fibrillation within seconds. Once detected, the device’s internal processor determines the appropriate electrical response. It can deliver low-energy pacing to correct minor irregularities or a high-energy shock to terminate VF. The engineering challenge here involves balancing battery longevity—often lasting up to a decade—with the need for high-voltage output capabilities in a device the size of a pocket watch.
The Rise of Wearable Cardioverter Defibrillators (WCDs)
For patients who are at temporary risk or are not candidates for surgery, the Wearable Cardioverter Defibrillator (WCD) offers a non-invasive tech solution. These “smart vests” contain electrodes that monitor the heart 24/7.
If the WCD’s software detects a lethal arrhythmia, it alerts the patient with a series of alarms before delivering a therapeutic shock. This provides a digital safety net, ensuring that the first-line treatment is administered even if the patient is alone. The tech focus here is on “false-positive” reduction; the software must be robust enough to ignore signal “noise” caused by the patient’s movement or muscle contractions.
The Role of AI and Machine Learning in Predicting Arrhythmias
The future of first-line treatment for ventricular fibrillation is shifting from reaction to prediction. Artificial Intelligence (AI) and Machine Learning (ML) are currently being integrated into cardiac monitoring ecosystems to identify the warning signs of VF before the heart actually stops.
Predictive Analytics in Emergency Response
In many smart cities, emergency response systems are being upgraded with AI-driven software. When a 911 call is placed, AI tools can analyze the caller’s voice and the background sounds of the patient’s breathing (agonally gasping) to identify a cardiac arrest with higher accuracy than human dispatchers.
This technological layer ensures that the correct first-line treatment—defibrillation—is prioritized. It can trigger the immediate dispatch of high-tech “first responder” units or even notify nearby civilians who have registered themselves via apps like PulsePoint, which uses GPS technology to bridge the gap between a victim and the nearest AED.
Deep Learning in ECG Interpretation
Interpreting an Electrocardiogram (ECG) is a skill that takes years for medical professionals to master. However, Deep Learning models are now being trained on millions of ECG samples. These AI models can detect subtle patterns in a “normal” heart rhythm that may indicate a high risk of an imminent VF event.
By integrating these AI diagnostics into consumer wearables like the Apple Watch or specialized medical patches, technology is enabling a paradigm shift. The first-line treatment can be initiated earlier—potentially through medication or controlled clinical intervention—before the catastrophic failure of ventricular fibrillation occurs.
Future Tech Frontiers: IoT and Remote Resuscitation
As we look toward the next decade, the first-line treatment for VF will be further optimized through the Internet of Things (IoT) and autonomous systems. The goal is to reduce the “time to shock,” as every minute of delay reduces the chance of survival by 7-10%.
Drone-Delivered Defibrillators
One of the most exciting trends in digital health technology is the use of autonomous drones to deliver AEDs. In rural areas or congested urban centers where ambulances may be delayed, GPS-coordinated drones can fly directly to the coordinates of a 911 caller.
These drones are more than just delivery vehicles; they are part of a connected ecosystem. Upon arrival, the drone’s camera can provide a live feed to a remote physician, who can then supervise the administration of the first-line treatment via the IoT-connected AED. This “tele-resuscitation” ensures that even in the absence of a trained medic, the best technology and expertise are present on the scene.
Cybersecurity and Med-Tech Integrity
As defibrillators and cardiac monitors become more connected, the focus on digital security becomes paramount. An ICD that is connected to the cloud for remote monitoring is, theoretically, an endpoint on a network.
Tech firms are now investing heavily in the cybersecurity of medical devices to prevent unauthorized access or interference with life-saving treatments. Ensuring the integrity of the software that delivers the shock is just as important as the hardware that generates the electricity. Advanced encryption and secure boot protocols are becoming standard features in the next generation of cardiac tech.
Conclusion: The Convergence of Medicine and Silicon
The first-line treatment for ventricular fibrillation remains, at its core, the rapid application of electrical energy to the heart. However, the delivery of that treatment is a feat of modern technology. From the biphasic waveforms that ensure safety to the AI models that predict vulnerability, the tech industry has become the primary architect of cardiac survival.
As we move forward, the line between medical intervention and technological innovation will continue to blur. Whether it is through a drone-delivered AED, a smart wearable, or an AI-enhanced monitoring system, technology is ensuring that the “first line” of defense is faster, smarter, and more accessible than ever before. In the battle against ventricular fibrillation, silicon and software are proving to be the ultimate lifesavers.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.