For decades, the field of endocrine surgery was governed by a philosophy of “maximal exploration.” Surgeons would perform wide-neck dissections to identify the four tiny parathyroid glands, often relying more on anatomical intuition than precise data. However, as we move further into the digital age, the question of “what is parathyroid surgery” has shifted from a purely biological inquiry to a technological one. Today, parathyroid surgery is a high-tech discipline defined by advanced imaging algorithms, real-time biochemical monitoring, and robotic-assisted precision.
The evolution of this procedure represents a microcosm of the broader shift in modern medicine: the transition from invasive exploration to data-driven intervention. By leveraging hardware and software innovations, surgeons can now locate and resolve hyperparathyroidism with unparalleled accuracy, minimizing recovery times and maximizing surgical success rates.
The Digital Map: Advanced Preoperative Imaging and Localization Tech
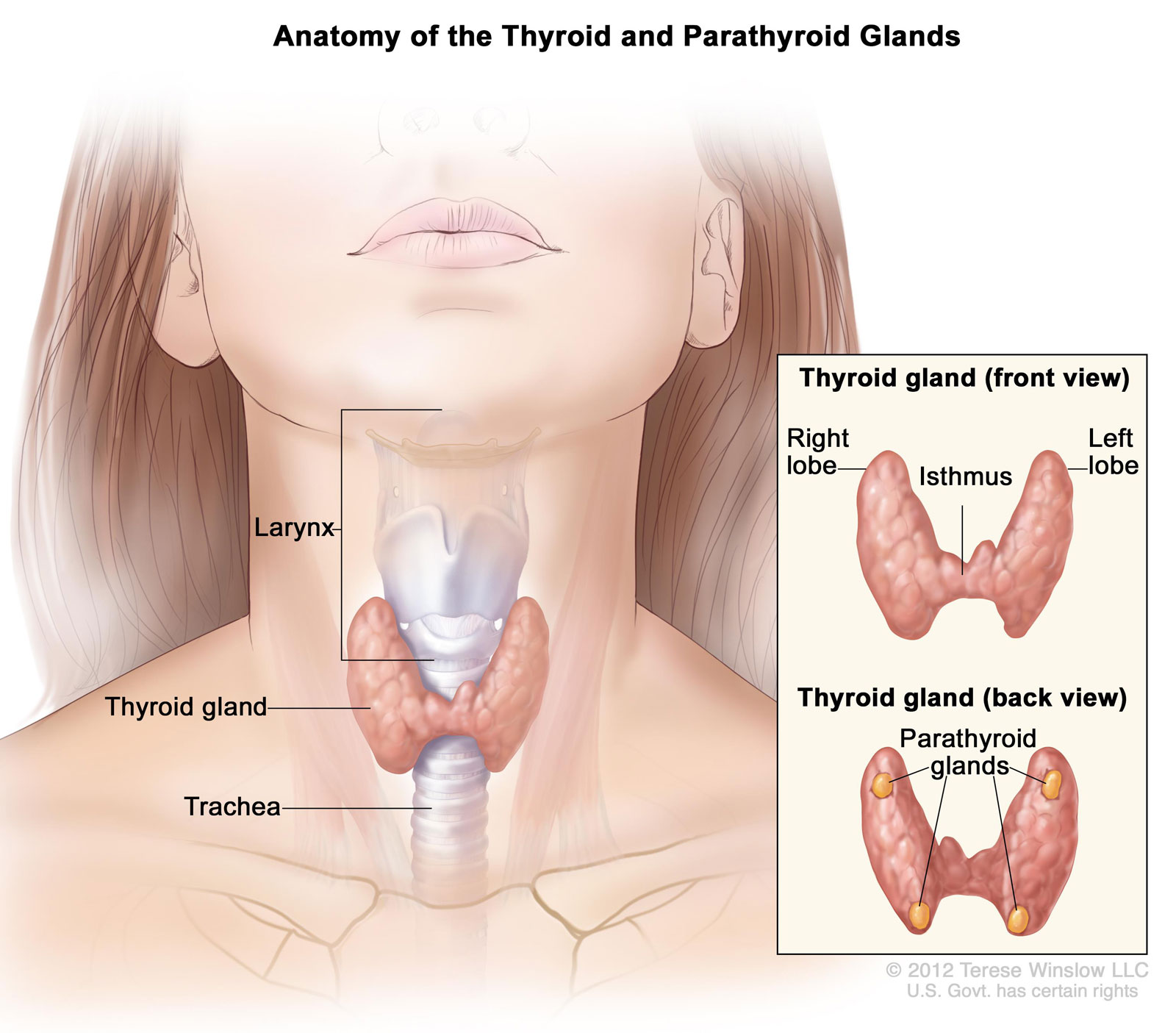
The success of a modern parathyroidectomy—the surgical removal of one or more overactive parathyroid glands—is heavily dependent on the quality of the preoperative “map.” In the past, surgeons had to rely on general anatomical knowledge. Today, specialized imaging technology allows for the pinpoint localization of adenomas (benign tumors) before the first incision is ever made.
Sestamibi and SPECT/CT Integration
The gold standard in parathyroid localization is the Sestamibi scan, but its modern iteration is far more sophisticated than its predecessors. This technology utilizes a radioactive tracer (Technetium-99m) that is absorbed preferentially by overactive parathyroid tissue. When combined with Single-Photon Emission Computed Tomography (SPECT) and traditional CT scans—a process known as SPECT/CT fusion—software algorithms create a three-dimensional anatomical and functional map. This allows surgeons to visualize the exact depth and relationship of the abnormal gland to surrounding structures like the carotid artery and esophagus.
High-Resolution Ultrasound and AI Enhancement
While nuclear medicine provides functional data, high-resolution ultrasound provides morphological detail. Modern ultrasound machines utilize high-frequency transducers that offer clarity down to the millimeter. Emerging software tools are now integrating artificial intelligence to help radiologists differentiate between lymph nodes, thyroid nodules, and parathyroid adenomas. By training neural networks on thousands of previous cases, these AI-enhanced tools reduce the “noise” in imaging, providing the surgical team with a clear technical roadmap.
Intraoperative Monitoring: Real-Time Biochemical Feedback Loops
Perhaps the most significant technological leap in parathyroid surgery is the move toward real-time data analysis during the procedure. In software development, “hot reloading” allows developers to see changes instantly. In the operating room, Intraoperative Parathyroid Hormone (IoPTH) monitoring provides a similar feedback loop.
The Rapid PTH Assay
The parathyroid glands regulate calcium by releasing parathyroid hormone (PTH). Because PTH has an incredibly short half-life (approximately 3 to 5 minutes), it serves as a perfect real-time biomarker. During surgery, specialized point-of-care testing equipment is used to measure PTH levels in the patient’s blood.
The “Miami Criterion,” a widely used clinical algorithm, dictates that a 50% drop in PTH levels within ten minutes of removing a suspected adenoma indicates a successful “cure.” This technological capability allows the surgeon to confirm that no other overactive glands remain, effectively ending the surgery without the need for further exploration. It transforms the surgery from a “best guess” scenario into a data-validated success.
Near-Infrared Autofluorescence (NIRAF)
One of the greatest challenges in neck surgery is the visual similarity between parathyroid glands, fat, and lymph nodes. To solve this, surgeons are increasingly using near-infrared imaging technology. Parathyroid glands possess a unique property of “autofluorescence” when exposed to specific wavelengths of light. Using specialized camera systems, such as the Fluobeam or similar NIRAF devices, surgeons can see the glands “glow” on a digital monitor in real-time. This hardware solution prevents the accidental removal of healthy glands and ensures the preservation of parathyroid function, a critical factor in post-operative patient health.
Surgical Hardware: From Scalpels to Robotic Platforms
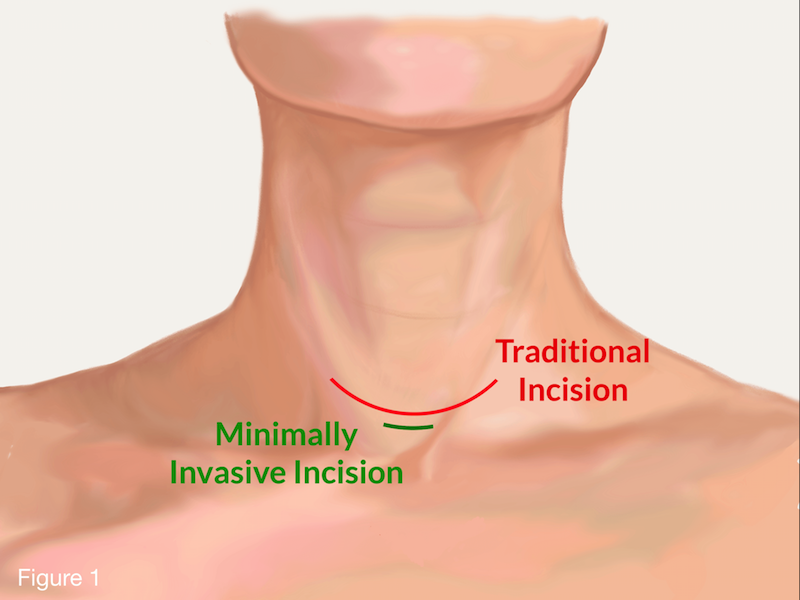
The physical act of performing parathyroid surgery has been revolutionized by advancements in surgical hardware. The goal of “Minimalism” in surgery is achieved through tools that allow for smaller incisions and greater dexterity.
Minimally Invasive Radio-Guided Surgery (MIRP)
Technological convergence is best seen in MIRP. Using a handheld gamma probe—a device that detects radiation—the surgeon can follow the signal from the Sestamibi tracer injected earlier. This “GPS for the neck” allows for an incision as small as 2 centimeters. The probe provides audible and visual feedback, guiding the surgeon directly to the pathology. This reduces the “footprint” of the surgery, leading to faster healing and less tissue trauma.
Robotic-Assisted Endocrine Surgery
For patients concerned with visible scarring, the Da Vinci surgical system and other robotic platforms have introduced the possibility of “scarless” (remote access) parathyroid surgery. Through a robotic-assisted transaxillary (underarm) or retroauricular (behind the ear) approach, the surgeon uses high-definition 3D cameras and wrist-articulated instruments to navigate to the neck.
The technology translates the surgeon’s hand movements into micro-movements, filtering out tremors and providing a level of precision that human hands alone cannot achieve. While more complex to set up, these robotic systems represent the pinnacle of surgical engineering, merging tele-operated robotics with high-stakes medical intervention.
The Future of Endocrine Tech: Big Data and Predictive Analytics
As we look toward the future, the definition of parathyroid surgery is set to expand into the realm of predictive analytics and personalized medicine. The integration of “Big Data” into the surgical workflow is the next frontier.
Machine Learning for Surgical Outcomes
Hospitals are beginning to utilize machine learning models to analyze preoperative data—such as calcium levels, vitamin D status, and imaging results—to predict the likelihood of “multigland disease” versus a single adenoma. This predictive software allows surgical teams to customize their technological approach for each patient. For instance, if a model predicts a high probability of multiple affected glands, the surgeon may opt for a more comprehensive bilateral approach from the start, rather than relying solely on a minimally invasive “targeted” path.
Augmented Reality (AR) in the OR
The next phase of surgical visualization involves Augmented Reality. Imagine a surgeon wearing an AR headset that overlays the 3D SPECT/CT map directly onto the patient’s neck in real-time. This “X-ray vision” would allow the surgeon to see the exact location of the tumor beneath the skin and muscle layers before making an incision. Prototypes for these systems are already in development, promising to further bridge the gap between digital data and physical reality.

Conclusion: The Synergy of Medicine and Technology
What is parathyroid surgery in the 21st century? It is no longer just a manual craft; it is a sophisticated integration of nuclear physics, robotic engineering, and biochemical data analysis. The transition from the “traditional” open exploration to the modern “targeted” approach has been fueled entirely by technological innovation.
By utilizing high-resolution mapping, real-time feedback loops via PTH assays, and precision hardware like gamma probes and robotic arms, the medical community has turned a complex and once-risky procedure into a highly efficient, outpatient-friendly intervention. As AI and AR continue to mature, the precision of parathyroid surgery will only increase, proving that the future of surgery lies not just in the hands of the surgeon, but in the power of the technology they wield. For the patient, this means higher cure rates, smaller scars, and a faster return to health—a perfect example of technology serving humanity.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.