Nasal turbinates, those intricate bony structures nestled within our nasal passages, play a crucial role in conditioning the air we breathe. They warm, humidify, and filter inhaled air before it reaches our lungs, acting as sophisticated biological air purifiers and humidifiers. However, when these delicate structures enlarge beyond their normal size – a condition known as hypertrophy of nasal turbinates – they can transform from benevolent guardians into troublesome obstructions, leading to a cascade of uncomfortable and often debilitating symptoms. While traditionally a subject of medical inquiry, the understanding, diagnosis, and management of nasal turbinate hypertrophy are increasingly being shaped by groundbreaking technological advancements. This article delves into the phenomenon of turbinate hypertrophy, with a particular focus on the innovative technological solutions emerging in the field.
The Technological Lens on Nasal Anatomy and Physiology
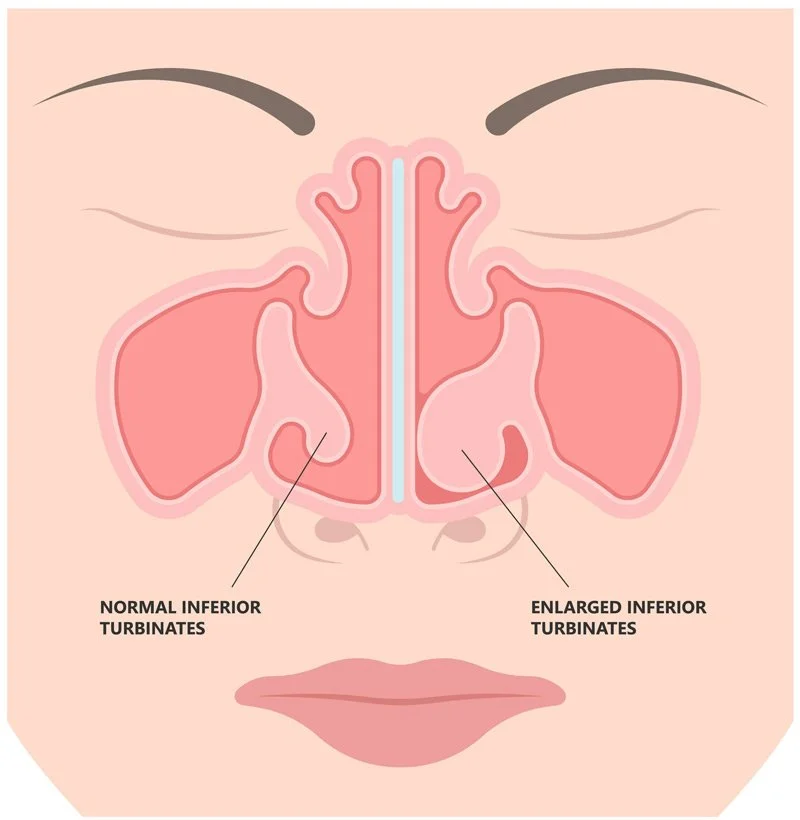
The human nasal cavity is a marvel of biological engineering, and understanding its complex anatomy is the first step in comprehending conditions like turbinate hypertrophy. Technology has played an indispensable role in both visualizing and quantifying the nuances of this delicate ecosystem.
3D Imaging and Computational Fluid Dynamics: Visualizing the Invisible
Historically, our understanding of nasal airflow and turbinate size was limited by two-dimensional imaging and direct observation. However, the advent of advanced imaging technologies has revolutionized our ability to peer into the nasal cavity with unprecedented detail.
High-Resolution CT and MRI Scans: Precision Anatomy Mapping
Computed Tomography (CT) and Magnetic Resonance Imaging (MRI) scans are now standard tools in diagnosing a wide range of medical conditions, including nasal turbinate hypertrophy. These technologies provide cross-sectional images of the nasal passages, allowing clinicians to precisely measure the size and shape of the turbinates. Unlike X-rays, CT and MRI offer detailed anatomical views, revealing the extent of turbinate enlargement and its impact on surrounding structures.
- Quantifying Enlargement: Sophisticated software can analyze these scans to quantify the degree of turbinate hypertrophy. This objective measurement is crucial for determining the severity of the condition and guiding treatment decisions. Parameters such as turbinate volume, cross-sectional area, and degree of mucosal thickening can be precisely determined, offering a more objective assessment than subjective visual inspection alone.
- Identifying Underlying Causes: Advanced imaging can also help identify secondary causes of turbinate hypertrophy, such as chronic rhinosinusitis, allergies, or anatomical variations, which might require different treatment approaches. The ability to visualize mucosal inflammation, polyps, or septal deviations in conjunction with turbinate enlargement provides a comprehensive diagnostic picture.
Computational Fluid Dynamics (CFD): Simulating Airflow Dynamics
While imaging provides static anatomical data, Computational Fluid Dynamics (CFD) offers a dynamic perspective on how air moves through the nasal cavity. CFD is a branch of fluid mechanics that uses numerical analysis and algorithms to solve and analyze problems involving fluid flows.
- Predicting Airflow Obstruction: By integrating CT scan data into CFD models, researchers and clinicians can simulate airflow patterns within an individual’s nasal passages. This allows for the visualization of areas where airflow is restricted due to enlarged turbinates. CFD can pinpoint specific turbinate regions that contribute most significantly to nasal obstruction, providing a more functional assessment of the anatomical findings.
- Optimizing Treatment Strategies: CFD simulations can also be used to predict the potential outcomes of different surgical interventions. For instance, a surgeon could model how a particular turbinate reduction technique might alter airflow dynamics, helping to select the most effective approach for relieving the patient’s symptoms. This technology moves beyond simply treating an enlarged structure to understanding and optimizing the functional consequences of that enlargement.
Digital Olfaction and Breath Analysis: Sensing the Senses
The sense of smell and the quality of breath are intrinsically linked to nasal function. Emerging technologies are beginning to explore how to objectively measure and analyze these sensory aspects, potentially offering new avenues for understanding and managing turbinate hypertrophy.
Electronic Noses (E-Noses): Detecting Olfactory Impairments
The olfactory epithelium, responsible for our sense of smell, is located within the nasal cavity, often in close proximity to the turbinates. Hypertrophy can physically impede the passage of odor molecules to this sensitive tissue, leading to diminished or altered sense of smell (hyposmia or dysosmia).
- Objective Smell Assessment: Electronic noses, equipped with an array of sensors that mimic the human olfactory system, are being developed to provide objective measurements of smell perception. These devices can be trained to recognize specific odor profiles. In the context of turbinate hypertrophy, an e-nose could potentially assess the degree of olfactory impairment by comparing a patient’s response to known odors with that of a healthy individual.
- Monitoring Treatment Efficacy: As turbinate hypertrophy can impact smell, monitoring improvements in olfactory function using e-noses could serve as a valuable indicator of treatment success, complementing symptom questionnaires. This technological approach offers a more quantifiable and less subjective alternative to traditional smell tests.
Breath Analysis Technologies: Beyond Airflow
The composition of exhaled breath can reveal a great deal about respiratory health. While not directly diagnosing turbinate hypertrophy, advanced breath analysis can provide insights into related conditions or the overall health of the respiratory tract, which can be influenced by nasal obstruction.
- Volatile Organic Compounds (VOCs): Sophisticated sensors can detect volatile organic compounds (VOCs) in exhaled breath. Changes in VOC profiles can indicate inflammatory processes, infections, or metabolic alterations. For individuals with chronic nasal issues, including turbinate hypertrophy, these changes might offer clues about underlying inflammation or the body’s response to impaired breathing.
- Biomarker Discovery: The field of breathomics is rapidly evolving, with the potential to discover novel biomarkers associated with various respiratory and systemic diseases. While direct biomarkers for turbinate hypertrophy are still in their infancy, advancements in breath analysis could indirectly contribute to a more holistic understanding of the condition and its impact on overall health.
Technological Innovations in Turbinate Reduction
The core of managing symptomatic turbinate hypertrophy often lies in reducing the size of the enlarged tissues. Technology has driven significant advancements in the precision, minimally invasiveness, and efficacy of these procedures.
Minimally Invasive Surgical Techniques and Devices
Traditional surgical approaches to turbinate reduction could sometimes be overly aggressive, leading to complications like excessive dryness or bleeding. Modern technology has enabled more conservative and targeted interventions.
Radiofrequency Ablation (RFA): Targeted Tissue Reduction
Radiofrequency ablation is a minimally invasive technique that uses radiofrequency energy to heat and shrink turbinate tissue. A probe is inserted into the turbinate, and controlled heat is applied, causing the tissue to shrink over several weeks.
- Precision and Control: RFA devices allow for precise control over the depth and extent of tissue heating, minimizing damage to surrounding healthy tissue and the mucosal lining. This targeted approach helps preserve the turbinate’s essential functions while reducing its obstructive volume.
- Outpatient Procedure: RFA is typically performed in an outpatient setting under local anesthesia, making it a less invasive and more convenient option for patients compared to traditional surgery. Recovery is generally faster, with less pain and discomfort.
Microdebrider-Assisted Turbinoplasty: Precise Sculpting
The microdebrider is a small, powered surgical instrument with a rotating blade used for tissue removal. In turbinoplasty, it’s employed to shave away excess turbinate tissue with high precision.
- Preserving Mucosa: Microdebriders are designed to remove hypertrophied tissue while preserving the crucial mucosal lining, which is vital for humidification and filtration. This helps to mitigate the risk of dryness and crusting.
- Improved Visualization: The procedure is often performed under endoscopic visualization, allowing the surgeon to see the turbinate structures in detail and precisely remove the hypertrophied tissue, ensuring optimal airflow and function.
Laser Turbinate Reduction: Targeted Vaporization
Similar to RFA, laser technology can be used to ablate or vaporize excess turbinate tissue. Different types of lasers can be employed, each with specific wavelengths and penetration depths, allowing for tailored treatment.

- Minimizing Bleeding: Lasers have a cauterizing effect, which can help to reduce bleeding during and after the procedure. This can lead to a cleaner surgical field and potentially faster recovery.
- Versatility: Laser techniques offer versatility in targeting specific areas of turbinate hypertrophy, whether it’s the bony structure or the soft tissue component.
Post-Operative Monitoring and Rehabilitation Technologies
The technological journey doesn’t end with the surgical procedure. Advanced tools are also emerging for monitoring patient recovery and optimizing long-term outcomes.
Smart Nasal Implants and Sensors: Real-Time Monitoring
While still in nascent stages for turbinate hypertrophy, the concept of smart implants and embedded sensors is gaining traction in various medical fields. For nasal procedures, future applications could include:
- Continuous Airflow Monitoring: Miniature sensors could potentially be used to monitor airflow and pressure within the nasal cavity post-operatively, providing objective data on the effectiveness of the intervention and detecting any emerging issues.
- Inflammation and Healing Detection: Biosensors could be integrated to detect inflammatory markers or signs of infection, alerting clinicians to potential complications early on.
Virtual Reality (VR) and Augmented Reality (AR) in Rehabilitation
VR and AR are revolutionizing rehabilitation across many disciplines, and the field of otolaryngology is no exception.
- Patient Education and Visualization: VR can be used to create immersive educational experiences for patients, allowing them to visualize their nasal anatomy, understand the impact of hypertrophy, and see how surgical interventions will address their condition. This can alleviate anxiety and improve compliance.
- Therapeutic Exercises: AR applications could guide patients through targeted nasal hygiene and breathing exercises, crucial for post-operative recovery and maintaining optimal nasal function. This gamified approach can enhance patient engagement and adherence to rehabilitation protocols.
The Future of Turbinate Hypertrophy Management: AI and Personalized Medicine
The convergence of advanced imaging, minimally invasive techniques, and the burgeoning power of Artificial Intelligence (AI) promises a paradigm shift in how we approach nasal turbinate hypertrophy.
AI in Diagnosis and Predictive Analytics
AI algorithms are increasingly being trained on vast datasets of medical images and patient information, enabling them to identify patterns and make predictions that may elude human observation.
Image Analysis and Automated Diagnosis
AI-powered software can analyze CT and MRI scans with remarkable speed and accuracy, flagging potential areas of turbinate hypertrophy and quantifying their severity. This can assist radiologists and otolaryngologists in making faster and more consistent diagnoses.
- Early Detection: AI’s ability to discern subtle abnormalities could potentially lead to earlier detection of turbinate hypertrophy, especially in cases where symptoms are mild or nonspecific.
- Reducing Diagnostic Variability: By providing objective and consistent analysis of imaging data, AI can help reduce inter-observer variability in diagnosis, leading to more standardized patient care.
Predictive Modeling for Treatment Outcomes
AI can analyze patient data, including imaging, clinical history, and genetic factors, to predict the likelihood of success for different treatment modalities.
- Personalized Treatment Plans: This predictive capability will be instrumental in developing personalized treatment plans. AI can help clinicians determine which surgical technique or medical management strategy is most likely to yield the best outcome for an individual patient, minimizing trial-and-error approaches.
- Identifying Risk Factors: AI can also help identify individuals at higher risk for developing severe turbinate hypertrophy or experiencing complications, enabling proactive interventions.
The Rise of Nanotechnology and Regenerative Medicine
Looking further ahead, nanotechnology and regenerative medicine hold exciting potential for future therapeutic interventions.
Targeted Drug Delivery Systems
Nanoparticles can be engineered to deliver anti-inflammatory or other therapeutic agents directly to the hypertrophied turbinate tissue, minimizing systemic side effects and maximizing efficacy. This could offer a less invasive alternative for managing inflammation contributing to hypertrophy.
Tissue Engineering and Regeneration
The ultimate goal in regenerative medicine is to repair or replace damaged tissue. While still a distant prospect for turbinate hypertrophy, future research might explore ways to stimulate the regeneration of healthy turbinate tissue or to engineer functional turbinate equivalents.
Interoperability and Data Integration
The true power of these technological advancements will be realized through seamless integration and interoperability.
Electronic Health Records (EHRs) and Cloud Computing
Integrating imaging data, AI diagnostic tools, treatment outcomes, and patient feedback into comprehensive EHR systems, accessible via secure cloud platforms, will create a holistic view of patient care. This allows for continuous learning and improvement in diagnostic and therapeutic strategies.
- Data-Driven Research: Aggregated and anonymized data from these integrated systems will fuel further research into the causes, progression, and optimal management of turbinate hypertrophy.
- Global Collaboration: Cloud-based platforms facilitate collaboration among researchers and clinicians worldwide, accelerating the pace of discovery and innovation.
Conclusion: A Technologically Enhanced Future for Nasal Health
Hypertrophy of nasal turbinates, once understood primarily through the limited tools of traditional medicine, is now at the forefront of technological innovation. From the precision of 3D imaging and CFD simulations that allow us to visualize and understand airflow dynamics, to the development of minimally invasive surgical techniques that preserve function, technology is profoundly reshaping patient care. Emerging fields like digital olfaction and breath analysis offer new avenues for objective assessment, while AI promises to revolutionize diagnosis and personalize treatment strategies. As we continue to explore and implement these technological frontiers, the future of managing nasal turbinate hypertrophy looks increasingly sophisticated, precise, and patient-centric, aiming not just to alleviate symptoms but to restore optimal nasal health and function.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.