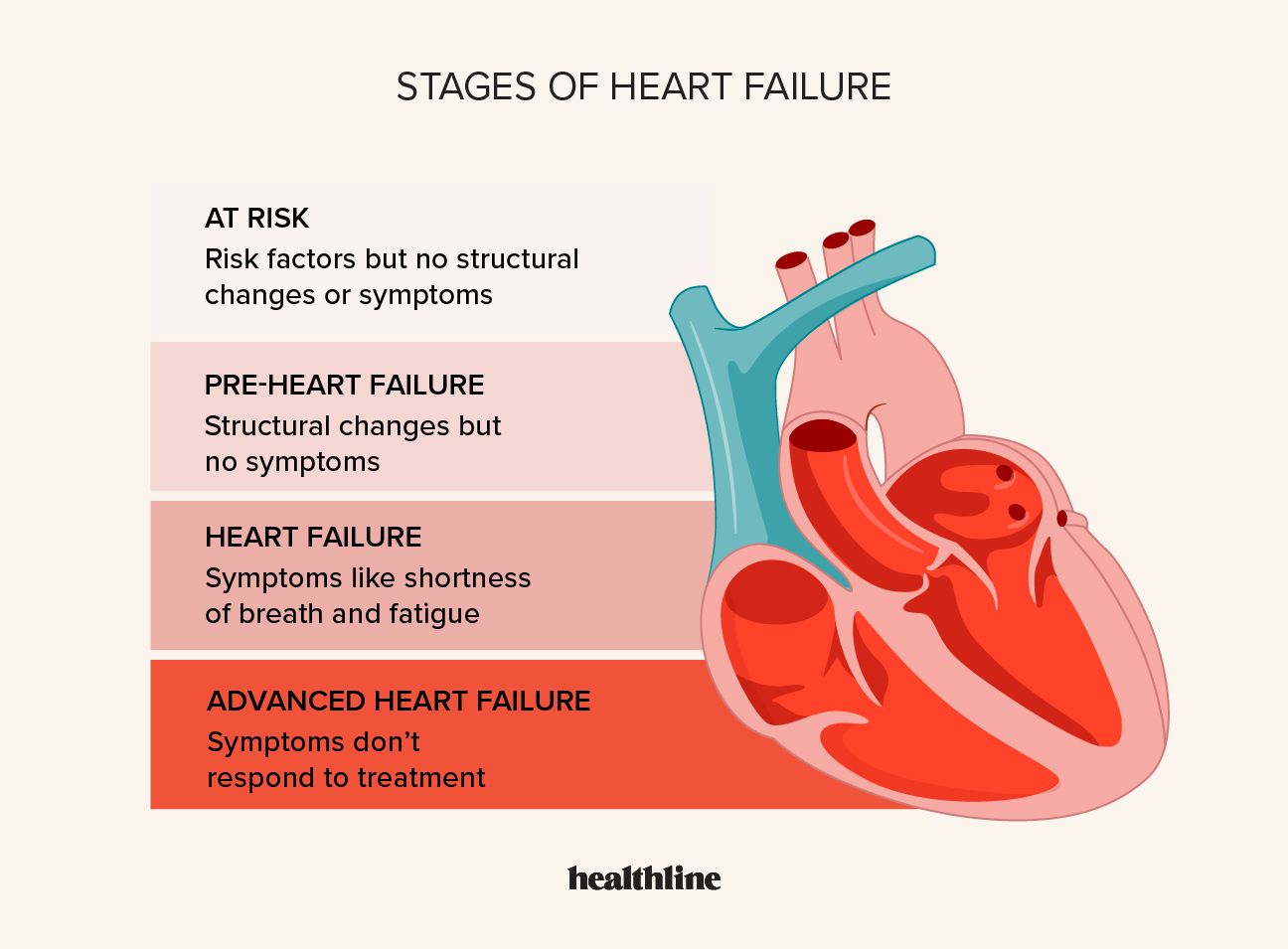
Congestive Heart Failure (CHF) is often misunderstood as a sudden cessation of the heart’s function. In reality, it is a chronic, progressive condition in which the heart muscle is unable to pump blood effectively enough to meet the body’s needs for blood and oxygen. As the pump weakens, blood often backs up, and fluid can build up in the lungs and the extremities, leading to the “congestion” that gives the condition its name.
While CHF was once managed primarily through lifestyle changes and rudimentary pharmaceuticals, the 21st century has ushered in a revolution in cardiac care. Today, the treatment of heart failure is inextricably linked to the “Tech” niche. From artificial intelligence (AI) diagnostics to sophisticated wearable sensors and implantable bio-electronic devices, technology is redefining what it means to live with—and treat—congestive heart failure.
Understanding CHF in the Era of Precision Medicine
To understand how technology treats CHF, one must first understand the mechanical and digital mapping of the disease. CHF occurs when the heart’s ventricles cannot pump enough blood volume to the body (systolic failure) or cannot relax sufficiently to fill with blood (diastolic failure).
The Physiological Mechanics of CHF
Traditionally, doctors relied on physical exams and stethoscopes to detect the “gallop” rhythm of a failing heart. However, tech-driven diagnostics now allow for a granular view of cardiac mechanics. High-resolution imaging and fluid dynamics software help clinicians visualize how blood moves through the chambers, identifying specific areas of muscular weakness that were previously invisible.
Digital Diagnostics: AI and Predictive Imaging
The frontline of CHF treatment today is AI-enhanced echocardiography. Modern software packages can now take standard ultrasound images of the heart and apply deep-learning algorithms to calculate the “ejection fraction”—the percentage of blood leaving the heart each time it contracts—with higher precision than a human technician. Furthermore, AI tools are being used to analyze Electrocardiograms (ECGs) to find subtle patterns that predict heart failure years before the first symptom appears, allowing for preventative tech-interventions.
The Rise of Remote Patient Monitoring (RPM)
One of the greatest challenges in treating CHF is the “revolving door” of hospitalizations. Patients often stabilize in the hospital, go home, and return weeks later in crisis because fluid buildup wasn’t detected early enough. Remote Patient Monitoring (RPM) technology has transformed this cycle by turning the patient’s home into a continuous data stream.
Continuous Monitoring Wearables
Beyond the consumer-grade Apple Watch or Fitbit, medical-grade wearables are now a cornerstone of CHF treatment. These devices monitor heart rate variability (HRV), respiratory rate, and oxygen saturation (SpO2) around the clock. By utilizing Internet of Things (IoT) connectivity, these devices upload data to a cloud-based platform where clinicians can monitor trends. If a patient’s heart rate begins to climb or their activity level drops, the software triggers an alert, allowing doctors to adjust medication dosages remotely.
Smart Scales and Bioimpedance Sensors
Weight gain is a primary indicator of fluid retention in CHF patients. New “Smart Scales” equipped with bioelectrical impedance analysis (BIA) can distinguish between fat mass and extracellular water. This technology allows the care team to see if a patient is “getting wet”—retaining fluid—long before the patient feels short of breath. This proactive data allows for the early administration of diuretics, preventing an emergency room visit and keeping the patient stable.
Advanced Interventional Technologies and Implantables
When lifestyle and medication aren’t enough, the treatment of CHF moves into the realm of high-tech hardware. The heart is, at its core, an electrical organ, and modern technology provides the tools to “reprogram” a failing heart.
CRT and Smart Pacemakers
Cardiac Resynchronization Therapy (CRT) is a sophisticated tech solution for patients whose heart chambers are no longer beating in sync. A CRT device, often called a biventricular pacemaker, sends timed electrical impulses to both lower chambers of the heart. Modern “Smart Pacemakers” are now equipped with Bluetooth connectivity, allowing them to send diagnostic reports directly to a smartphone app. These devices don’t just regulate rhythm; they collect data on thoracic impedance, which helps doctors monitor the progression of heart failure in real-time.
Left Ventricular Assist Devices (LVADs) as High-Tech Bridges
For patients with end-stage heart failure, the Left Ventricular Assist Device (LVAD) represents the pinnacle of medical engineering. An LVAD is a mechanical pump that is surgically implanted to help the left ventricle pump blood to the rest of the body. Unlike older versions, modern LVADs use magnetic levitation (MagLev) technology to suspend the pump’s rotor, reducing friction and minimizing damage to blood cells. These devices are connected to an external controller and power source, effectively making the patient a part of a complex, life-sustaining electronic system.
Data-Driven Pharmacotherapy and the Virtual Care Loop
Treating CHF is not just about hardware; it is about the software and data structures that manage the patient’s journey. Digital health platforms are now integrating pharmacological data with physiological data to create a “Virtual Care Loop.”
Algorithmic Dosage Optimization
The “Big Four” medications for CHF (Beta-blockers, ACE inhibitors/ARNIs, MRAs, and SGLT2 inhibitors) require precise titration—adjusting the dose to find the “sweet spot” of efficacy without side effects. New software tools use patient data from wearables and lab results to suggest optimal dosing schedules to physicians. This “decision support software” ensures that patients reach their target doses faster, which has been shown to significantly improve long-term survival rates.
Telehealth and the Virtual Heart Failure Clinic
The integration of telehealth platforms has solved the geographical barriers to specialist care. Through high-definition video conferencing and integrated digital stethoscopes, heart failure specialists can perform comprehensive evaluations remotely. These virtual clinics use centralized dashboards to prioritize patients based on risk scores generated by AI, ensuring that the most unstable patients receive attention first. This triage technology is essential in managing large populations of CHF patients with limited medical staff.
The Future of Cardiac Tech: Nanotech and Gene Editing
As we look toward the future, the treatment of congestive heart failure is moving toward the molecular level, blending biotechnology with traditional computing.
CRISPR and Regenerative Medicine
While still in the clinical trial phases, gene-editing technologies like CRISPR are being explored to treat the genetic causes of certain types of heart failure. Software-driven genomic mapping allows scientists to identify the exact “glitch” in a patient’s DNA that leads to a weakened heart. By correcting these sequences, we move from managing symptoms with tech to potentially curing the underlying condition.
The Challenge of Cybersecurity in Connected Cardiac Devices
As CHF treatment becomes more reliant on connected devices, the niche of digital security becomes vital. A “hacked” pacemaker or a compromised LVAD controller is a life-threatening prospect. Consequently, the next frontier of CHF treatment involves the implementation of robust encryption and blockchain-based data integrity protocols to ensure that the patient’s life-sustaining tech remains secure from external interference.

Conclusion
Congestive Heart Failure is a complex, multifaceted condition, but the lens of technology provides a roadmap for a more manageable future. Through the integration of AI diagnostics, remote monitoring wearables, and advanced mechanical implants, the “treatment” of CHF has evolved into a sophisticated technological ecosystem. As we continue to refine these tools, the goal remains clear: to use the power of tech to turn a once-terminal diagnosis into a manageable chronic condition, giving patients not just more years of life, but better quality within those years.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.