The removal of lymph nodes from the neck, medically known as a neck dissection, was once a procedure defined by large incisions, significant recovery times, and high risks of nerve damage. However, in the contemporary era of MedTech, the question of “what happens” during this procedure is increasingly answered by software engineers, robotics experts, and data scientists. As surgical interventions migrate into the digital realm, the removal of lymphatic tissue has become a case study for the integration of artificial intelligence, high-precision robotics, and advanced imaging software.
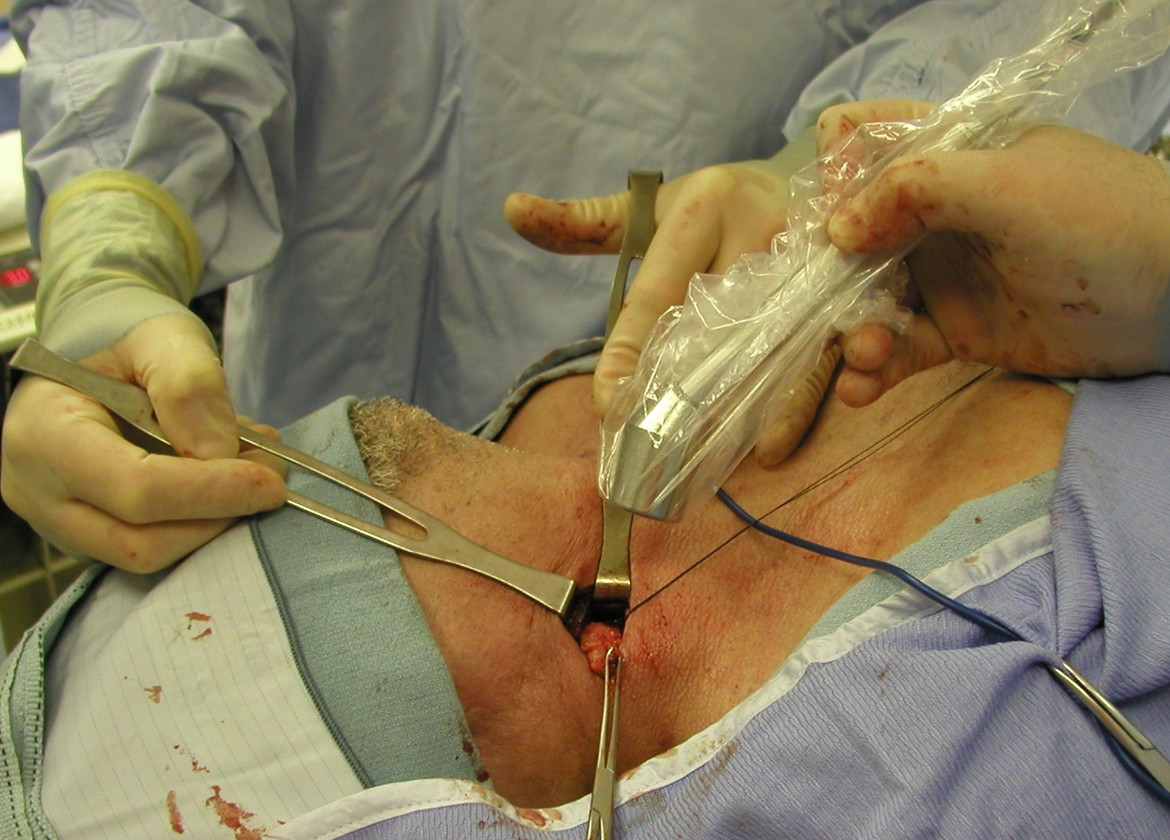
In the tech niche, we view the human body not just as a biological entity, but as a complex network of nodes and pathways. When these nodes are compromised—often by oncological threats—the technological response involves a sophisticated array of hardware and software designed to maximize efficiency and minimize collateral damage.
The Digital Architecture of Lymphatic Mapping
Before a single incision is made, the modern surgical suite utilizes a “digital twin” approach to map the patient’s cervical anatomy. This phase is dominated by advanced imaging software and AI algorithms that determine which nodes require removal and which can be spared.
AI-Driven Sentinel Node Identification
The first thing that happens technologically is the deployment of AI-enhanced imaging. Traditionally, surgeons relied on manual palpation or standard CT scans. Today, machine learning algorithms analyze PET-CT and MRI data to identify the “sentinel” node—the first node to which cancer cells are most likely to spread. Software like IBM’s Watson Health or specialized oncology AI can process thousands of images to highlight metabolic anomalies that the human eye might miss. This predictive modeling allows for a “targeted removal” rather than a “radical removal,” preserving vital tech-mapped structures.
3D Visualization and Pre-Surgical Simulation
Surgeons now use VR (Virtual Reality) and AR (Augmented Reality) platforms to rehearse the procedure. By importing a patient’s specific DICOM (Digital Imaging and Communications in Medicine) files into a 3D rendering engine, the medical team can visualize the proximity of lymph nodes to the jugular vein and the spinal accessory nerve. This software provides a high-fidelity roadmap, ensuring that when the physical removal happens, the path has already been digitally traversed multiple times.
Robotic-Assisted Neck Dissection (RAND): The Hardware Revolution
When the actual removal occurs, the most significant “tech” event is the transition from manual tools to robotic-assisted platforms. Systems like the Da Vinci Surgical System or the Medrobotics Flex Robotic System have redefined the mechanical limits of the human hand.
Precision Engineering and Tremor Filtration
What happens during the removal process is a feat of precision engineering. Robotic arms equipped with “Endowrist” technology offer a degree of motion greater than the human wrist. One of the most critical software features in these gadgets is tremor filtration. The software intercepts the surgeon’s hand movements, filters out microscopic physiological tremors, and translates them into perfectly smooth mechanical motions. This is essential when dissecting lymph nodes nestled against the carotid artery, where a fraction of a millimeter is the difference between success and catastrophe.
Haptic Feedback and Near-Infrared Fluorescence
Modern robotic platforms are increasingly integrating haptic feedback—technology that allows the surgeon to “feel” the resistance of tissues through the robotic console. Additionally, tech like Firefly (near-infrared fluorescence imaging) allows the surgeon to inject a specialized dye that glows under a specific light spectrum. The robotic cameras capture this, and the software overlays a bright green glow on the lymph nodes in real-time, effectively giving the surgeon “X-ray vision” to distinguish between healthy tissue and the nodes slated for removal.
Post-Operative Monitoring: The Role of Wearables and IoT

The technology doesn’t stop once the lymph nodes are removed. The “what happens next” phase is managed by a suite of Internet of Things (IoT) devices and remote patient monitoring (RPM) software designed to track recovery and detect complications like lymphedema or chyle leaks.
Smart Dressings and Bio-Sensors
Emerging from the world of wearable tech are “smart dressings.” These are integrated with flexible bio-sensors that monitor pH levels, temperature, and moisture at the incision site. This data is transmitted via Bluetooth to a mobile app, which uses predictive analytics to alert the medical team of a potential infection before clinical symptoms appear. By treating the recovery site as a data-generating node, tech reduces the need for frequent physical checkups and identifies complications with algorithmic speed.
Remote Patient Monitoring (RPM) and Mobile Health Apps
Following neck lymph node removal, patients often use specialized software to track their range of motion and swelling. Mobile health (mHealth) apps utilize the smartphone’s camera and computer vision technology to measure the circumference of the neck or the angle of head rotation. This data is synced to a cloud-based dashboard, allowing the surgical team to monitor the patient’s progress in real-time. If the software detects a plateau or a decline in mobility, it triggers a “telehealth” prompt, bridging the gap between hospital and home.
Cybersecurity in the Connected Operating Room
As we have seen, the removal of lymph nodes is now a highly digitized process. This introduces a critical tech concern: digital security. When life-saving hardware is connected to a network, it becomes a potential endpoint for cyber threats.
Protecting Surgical Robotics from External Breaches
What happens when a surgical robot is online? It becomes part of the hospital’s IoT ecosystem, which means it must be shielded by robust firewalls and encryption protocols. Cybersecurity firms are now specializing in “MedSec,” ensuring that the software controlling the robotic arms cannot be intercepted or manipulated. During a neck dissection, the integrity of the data stream between the surgeon’s console and the robotic unit is maintained through end-to-end encryption, preventing “man-in-the-middle” attacks that could jeopardize the procedure.
HIPAA-Compliant Data Flow and Cloud Storage
The vast amount of data generated—from the initial 3D mapping to the post-op wearable logs—must be stored and transmitted securely. This involves sophisticated cloud architecture that complies with HIPAA (Health Insurance Portability and Accountability Act) in the US or GDPR in Europe. Tech companies like Microsoft (Azure for Health) and AWS are providing the backend infrastructure to ensure that the “digital footprint” of a patient’s surgery remains private, searchable for medical research, yet impenetrable to unauthorized parties.
The Future: Autonomous Nodes and AI Diagnostics
Looking forward, the tech surrounding lymph node removal is trending toward increased autonomy. We are entering an era where the software might not just assist the surgeon but take an active role in the diagnostic and excision process.
Toward Semi-Autonomous Dissection
The next frontier is semi-autonomous surgery, where the AI identifies the lymph node and the robot performs the “pre-dissection” under the supervision of a human. This relies on “Computer Vision” (CV) and deep learning models trained on millions of previous surgeries. The goal is to standardize the procedure, ensuring that a patient in a rural clinic receives the same technological precision as one in a top-tier tech hub.
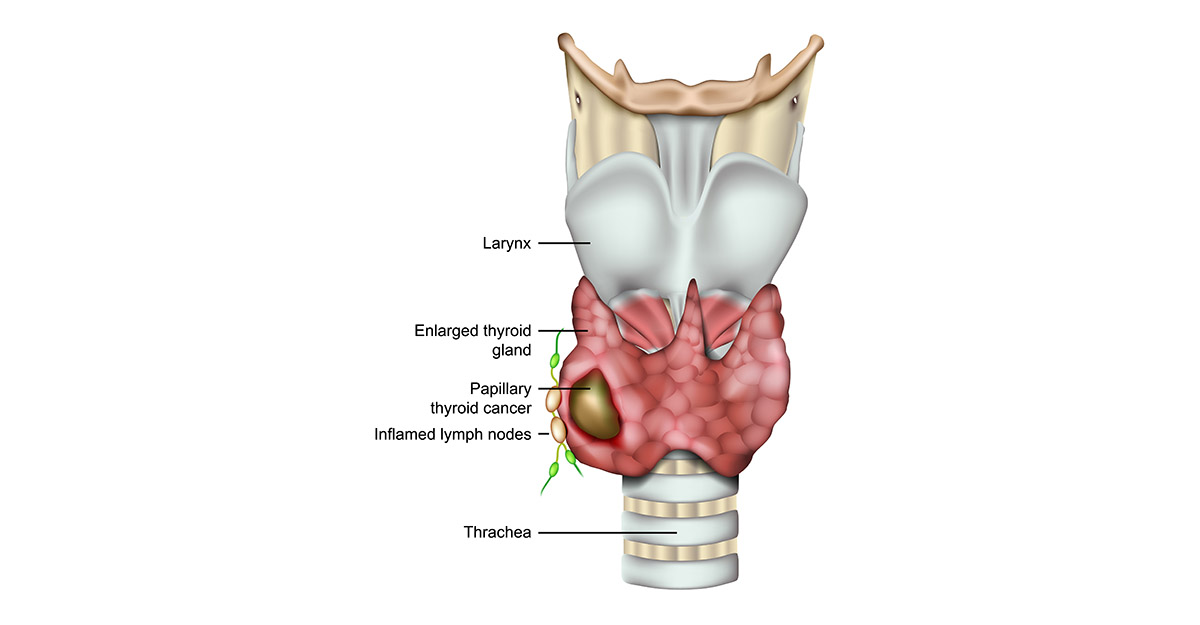
The Bio-Convergence of Tech and Biology
Finally, the “what happens” will eventually involve nanotech. Researchers are developing “nanobots” or smart particles that can be injected into the lymphatic system to flag cancerous nodes from the inside out. This would integrate seamlessly with current robotic platforms, allowing for a level of precision that moves from the millimeter scale to the micron scale.
In conclusion, when lymph nodes are removed from the neck today, it is far more than a biological event. It is a synchronized performance of high-end gadgets, sophisticated software, and secure data networks. From the AI that maps the first node to the wearable tech that monitors the final stages of healing, the procedure is a testament to how technology is rewriting the script of human health and surgical recovery. For the tech-savvy observer, it represents the ultimate integration of hardware, software, and the human “operating system.”
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.