The ubiquitous chest X-ray, a cornerstone of medical imaging for decades, plays a crucial role in the initial screening and diagnosis of various pulmonary conditions. For lung cancer, understanding what it can “look like” on an X-ray is not merely a matter of visual pattern recognition; it is increasingly about the sophisticated technological tools and analytical approaches that enhance the accuracy and efficiency of interpretation. In the realm of technology, the focus shifts from the purely anatomical to the algorithmic, the software-driven, and the AI-assisted. This article delves into how modern technology is revolutionizing the way we identify and analyze potential signs of lung cancer on X-ray images, moving beyond the limitations of the human eye.
The Evolving Landscape of Chest X-ray Interpretation
Historically, interpreting a chest X-ray was a skill honed through years of experience, relying on the radiologist’s ability to discern subtle anomalies. However, the sheer volume of images, coupled with the inherent variability in presentation, presents significant challenges. Technology has emerged not to replace the radiologist, but to augment their capabilities, providing a powerful suite of tools that can identify patterns, flag suspicious areas, and even quantify characteristics that might be missed by traditional methods.
Traditional Visual Cues and Their Technological Enhancements
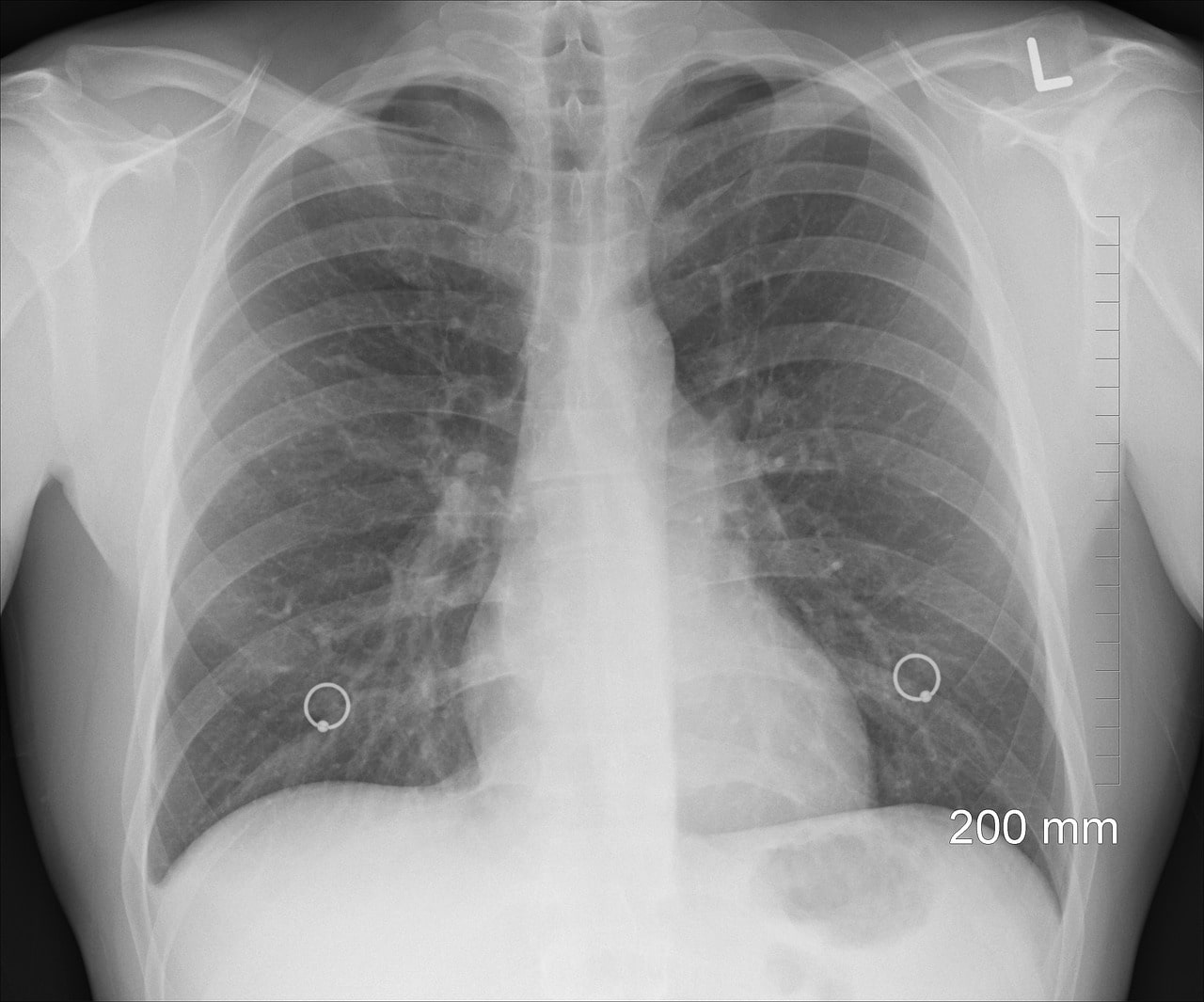
The most basic manifestation of lung cancer on an X-ray is often a nodule or mass. These appear as opaque or dense spots against the translucent background of the lung tissue. However, the size, shape, density, and location of these findings are critical indicators.
Identifying Nodules and Masses with Digital Precision
Modern digital X-ray systems capture images with higher resolution and a broader dynamic range than their film predecessors. This improved image quality is the bedrock for advanced analysis. Software algorithms can now be employed to:
- Automated Nodule Detection (AND): These systems utilize machine learning and deep learning algorithms trained on vast datasets of annotated X-rays. They can scan an entire image and highlight potential nodules, often distinguishing them from benign structures like blood vessels or scarring. This serves as a first-pass screening, reducing the chance of a small or subtle nodule being overlooked. The output from such systems can be presented as bounding boxes around potential nodules, along with a confidence score indicating the likelihood of it being a true finding.
- Nodule Characterization: Beyond simple detection, technology can assist in characterizing nodules. Software can measure precise dimensions (diameter, volume), assess regularity of the border (smooth vs. irregular), and even analyze the internal density and texture. For instance, a spiculated margin, where the nodule has sharp, irregular projections, is often a more concerning feature than a smooth, rounded one. AI models can quantify these features, providing objective data points for the radiologist.
- Comparison with Prior Studies: One of the most powerful tools in detecting malignancy is tracking changes over time. Technology facilitates this by enabling rapid and accurate digital comparison of current X-rays with previous ones. Software can automatically register and overlay images, highlighting any new nodules, growth in existing nodules, or changes in their morphology. This is crucial for differentiating a new cancerous growth from a stable, benign lesion.
Beyond the Nodule: Subtle Indicators and Advanced Imaging Techniques
Lung cancer doesn’t always present as a distinct nodule. It can manifest in more diffuse or subtle ways, making detection even more challenging and reliant on sophisticated technological interpretation.
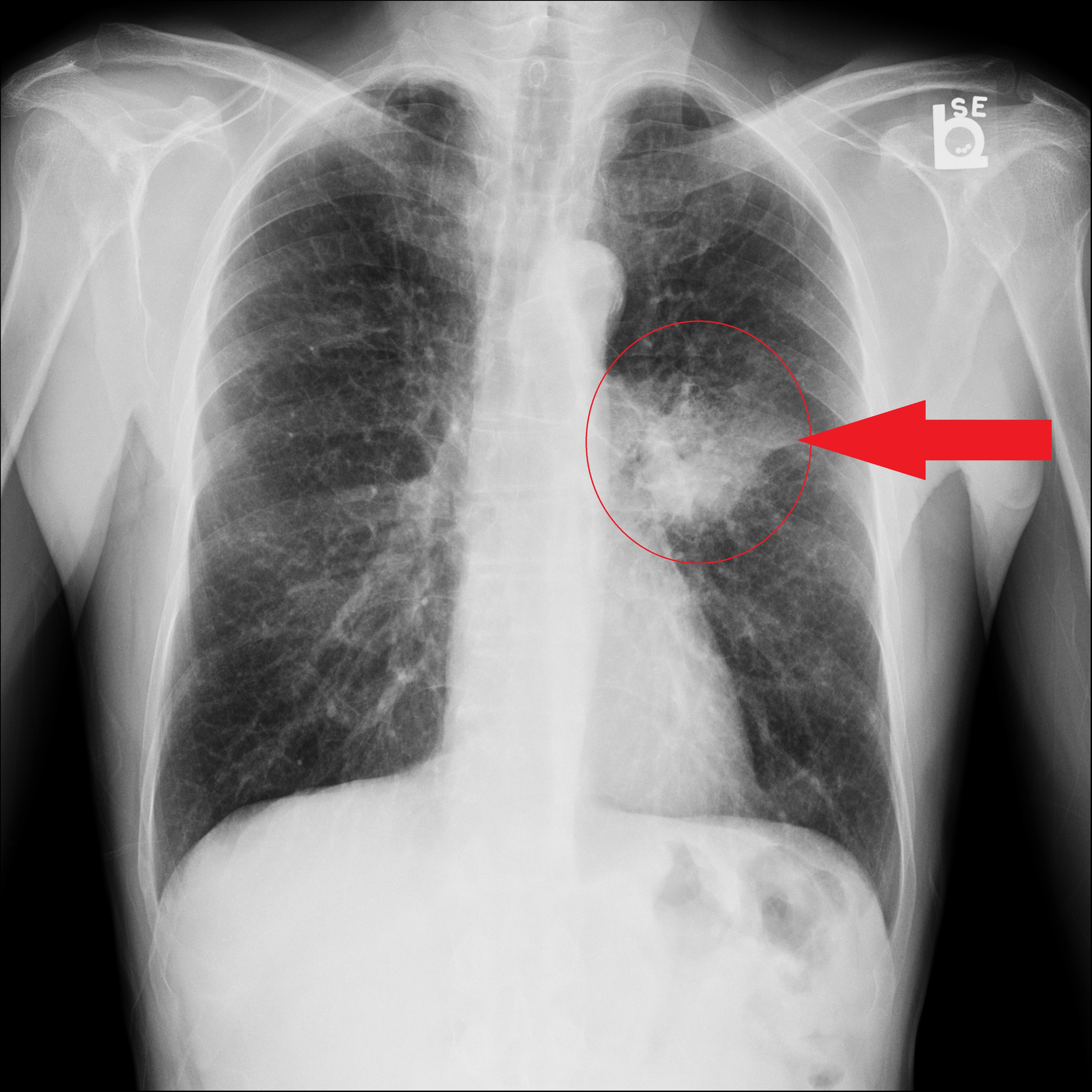
Recognizing Subtle Signs Through Pattern Recognition Algorithms
- Atelectasis and Airway Obstruction: A tumor can block an airway, leading to the collapse of a portion of the lung (atelectasis). On an X-ray, this appears as a loss of lung volume, increased opacity, and displacement of fissures or the diaphragm. AI algorithms can be trained to recognize these complex patterns of collapse and opacity, which might be difficult to attribute solely to a tumor without further context.
- Pleural Effusions and Lymphadenopathy: Cancer can spread to the lining of the lung (pleura), causing fluid accumulation (pleural effusion), or to the lymph nodes in the chest. These can appear as blunting of the costophrenic angles (for effusions) or enlarged lymph nodes, respectively. Advanced imaging analysis software can assist in detecting these subtle fluid collections and quantifying lymph node enlargement with greater precision, comparing measurements against established thresholds for suspicion.
- Advanced Texture and Density Analysis: Machine learning models can go beyond simple pixel intensity to analyze complex textural patterns within lung tissue. These subtle textural differences, imperceptible to the naked eye, can sometimes correlate with early cancerous changes. Techniques like radiomics, which extract a large number of quantitative features from medical images, are being explored to predict malignancy and even treatment response based on these subtle textural characteristics.
The Role of Artificial Intelligence (AI) in Lung Cancer Detection
Artificial intelligence, particularly deep learning, is rapidly transforming how medical images are analyzed. It offers the potential for faster, more accurate, and more consistent interpretations, addressing some of the inherent limitations of human perception.
AI-Powered Diagnostic Support Systems
- Deep Learning Models for Classification: AI models, trained on massive datasets of diagnosed lung cancers and benign findings, can learn to classify lesions with remarkable accuracy. These systems can provide a probability score for malignancy, helping radiologists prioritize cases and make more informed decisions. The development of convolutional neural networks (CNNs) has been particularly instrumental in this area, as they excel at identifying hierarchical features within images, from simple edges to complex shapes.
- Reducing Radiologist Fatigue and Improving Throughput: The sheer volume of medical imaging can lead to fatigue and burnout among radiologists. AI can act as a valuable assistant, pre-screening images and flagging areas of concern. This allows radiologists to focus their expertise on the most complex and ambiguous cases, improving overall efficiency and reducing the likelihood of errors due to prolonged visual inspection.
- Standardization and Reproducibility: Human interpretation, while skilled, can be subjective and vary between individuals. AI-driven analysis offers a higher degree of standardization and reproducibility. Once trained, an algorithm will consistently apply the same criteria to every image, leading to more uniform diagnostic outcomes. This is particularly important in large-scale screening programs.
Future Directions and Technological Advancements
The journey of technology in X-ray interpretation for lung cancer is far from over. Ongoing research and development are pushing the boundaries of what’s possible, promising even more sophisticated tools for early detection and diagnosis.

Towards Proactive and Predictive Diagnostics
- Integration with Other Data Sources: The future likely involves integrating X-ray analysis with other patient data, such as clinical history, genetic information, and other imaging modalities (like CT scans). AI systems can be developed to synthesize this multi-modal data for a more comprehensive risk assessment and diagnosis.
- Quantitative Imaging Biomarkers: The development of quantitative imaging biomarkers, derived from AI analysis of X-rays, could offer objective measures of disease progression, treatment effectiveness, and even the risk of recurrence. This moves beyond qualitative assessment to precise, data-driven insights.
- Real-time Feedback and Training Tools: AI can also be used to provide real-time feedback to less experienced radiologists during image interpretation, acting as a digital mentor. Furthermore, these advanced analytical tools can be integrated into educational platforms to train the next generation of medical imaging specialists.
In conclusion, while the fundamental visual appearance of lung cancer on an X-ray may involve familiar signs like nodules and masses, the technology now available to detect, analyze, and interpret these findings is profoundly advanced. From digital image enhancement and automated detection algorithms to sophisticated AI-powered diagnostic support systems, technology is not just a tool but a transformative force in the ongoing battle against lung cancer, empowering healthcare professionals with the insights needed for earlier, more accurate diagnoses.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.