The Tuberculosis (TB) skin test, often referred to colloquially as the “TB shot,” remains a cornerstone in the global effort to detect latent and active tuberculosis infections. While the name “shot” might evoke images of an injection, the Mantoux tuberculin skin test (TST) involves a much more localized and precise intradermal administration of a small amount of tuberculin purified protein derivative (PPD). The subsequent interpretation of the skin reaction is a crucial diagnostic step, and understanding what a positive result looks like is vital for healthcare professionals and for individuals undergoing the screening. This article delves into the visual characteristics of a positive TB skin test, the factors influencing its interpretation, and the technological underpinnings that enable this critical diagnostic tool.
The Science Behind the Skin Test: An Immunological Response
The TB skin test is not a direct detection of the Mycobacterium tuberculosis bacterium itself. Instead, it leverages the body’s immune system’s memory to a previous exposure to TB antigens. When a small amount of PPD is injected into the skin, it acts as a trigger for individuals who have been sensitized to TB.
Cellular Immunity and Delayed-Type Hypersensitivity
The mechanism behind the TST relies on cellular immunity, specifically a delayed-type hypersensitivity (DTH) reaction. In individuals previously exposed to Mycobacterium tuberculosis, their immune system has developed T lymphocytes that are specific to antigens present in the PPD. Upon re-exposure via the skin test, these sensitized T lymphocytes are activated.
This activation leads to the release of cytokines, such as interferon-gamma (IFN-γ). These cytokines then recruit other immune cells, primarily macrophages, to the injection site. This influx of immune cells causes inflammation, which manifests as a visible and palpable swelling, or induration, at the injection site. The induration is the key indicator of a positive reaction. It’s a localized inflammatory response, demonstrating that the immune system recognizes the TB antigens.
The Tuberculin Purified Protein Derivative (PPD)
The PPD used in the TB skin test is a complex mixture of proteins derived from the cultivation of Mycobacterium tuberculosis. The purification process is a critical technological step, ensuring that the PPD is standardized and contains specific antigens that are likely to elicit a response from sensitized individuals without causing a significant reaction in those who have not been exposed. The consistent quality and composition of PPD are essential for the reliability of the diagnostic test. Advances in biochemical engineering and manufacturing processes have been instrumental in developing and producing highly specific and stable PPD antigens.
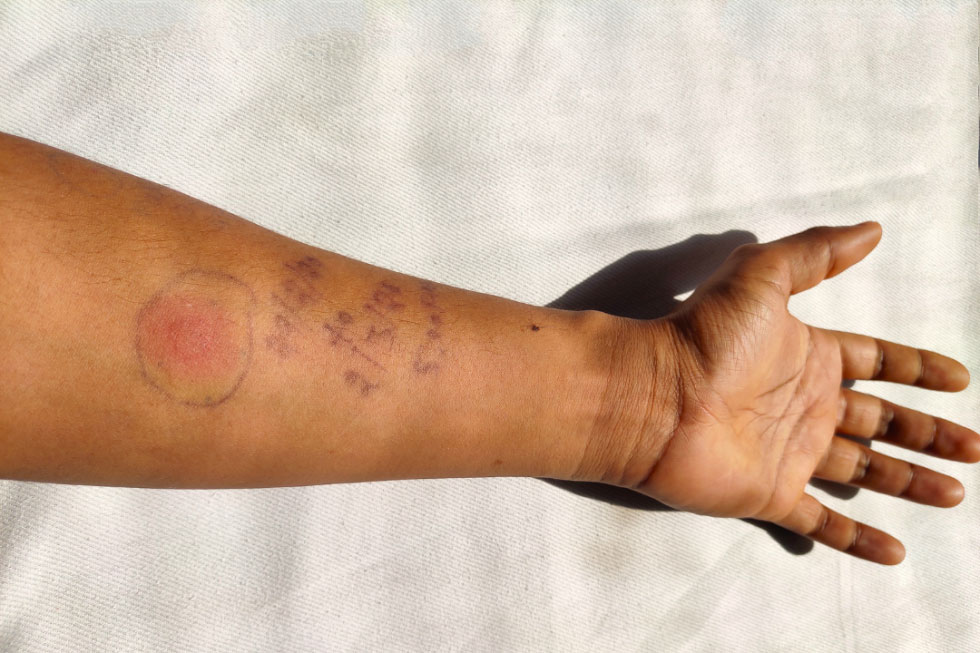
Visualizing a Positive Reaction: The Induration
The hallmark of a positive TB skin test is the presence of induration – a raised, hardened area of swelling. It is crucial to distinguish this induration from a simple redness or erythema, which can occur even in negative reactions due to the needle prick and minor skin irritation.
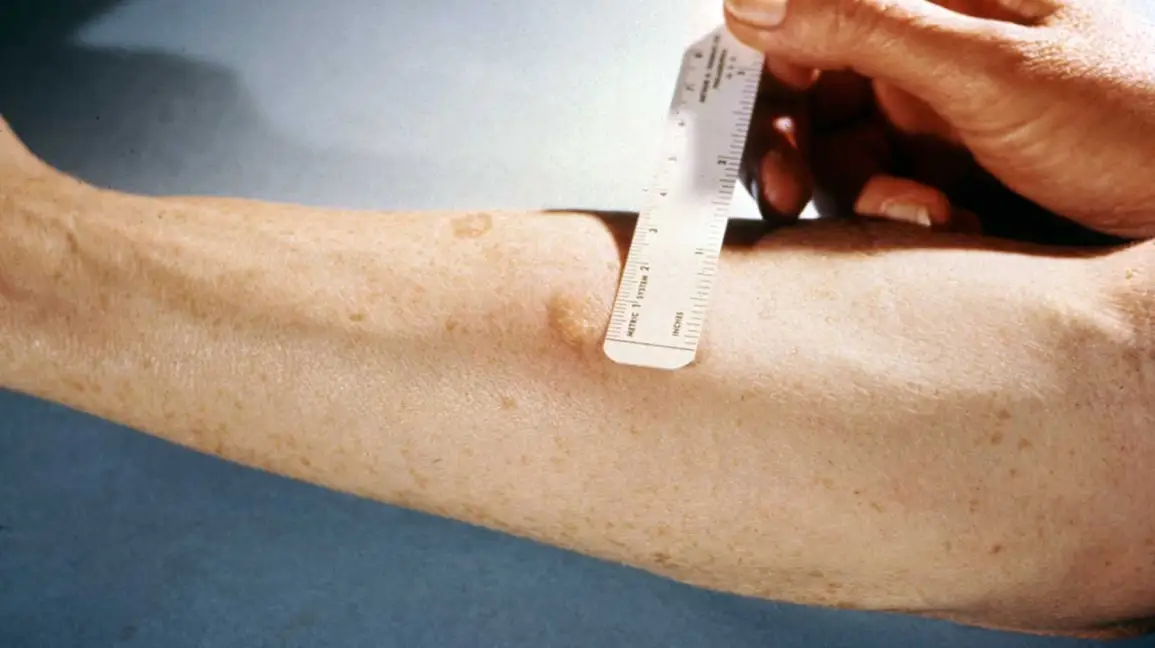
Measuring the Induration
A trained healthcare professional will measure the diameter of the induration in millimeters (mm) using a ruler. The measurement is taken across the diameter of the raised, hardened area, irrespective of any redness. The induration is palpated by running a finger gently over the skin to feel the extent of the hardened tissue.
- What constitutes “positive” depends on the risk factors of the individual being tested. For most individuals, an induration of 15 mm or greater is considered a positive reaction. However, for individuals with certain risk factors for TB exposure or progression, such as close contacts of infectious TB cases, individuals with HIV, or those with organ transplants, a lower threshold is used. For these higher-risk groups, an induration of 10 mm or greater may be considered positive. In very high-risk populations, such as immunocompromised individuals or those with a history of prior TB disease or vaccination, an induration of 5 mm or greater can be indicative of a positive test.
Differentiating from Erythema
It’s vital to reiterate that the redness (erythema) surrounding the induration is not the primary indicator of a positive test. A person can have significant redness but no palpable induration, and this would be considered a negative test. Conversely, a firm, raised area of induration with or without some surrounding redness is what signifies a positive result. The consistency and texture of the raised area are key distinguishing features. The induration should feel firm and well-defined, indicating the localized inflammatory response.

Factors Influencing Test Results and Interpretation
While the visual appearance of the induration is central to interpreting a TB skin test, several other factors can influence the test results and their meaning. Understanding these variables is crucial for accurate diagnosis and to avoid misinterpretations.
False Positives and False Negatives
False positive reactions can occur due to several reasons. One common cause is infection with non-tuberculous mycobacteria (NTM). These bacteria are found in the environment and can cause a similar immunological response to TB, leading to a positive skin test in individuals who do not have TB infection. BCG vaccination, a vaccine against TB given in some countries, can also sometimes lead to a positive PPD test, although the induration size is typically smaller compared to a true TB infection and the interpretation often takes vaccination history into account. Improper administration of the test, such as injecting the PPD too deeply or into the subcutaneous tissue instead of the dermis, can also lead to inaccurate results.
False negative reactions, where the test is negative despite the presence of TB infection, are also a concern. This can happen in individuals who are severely immunocompromised, such as those with advanced HIV infection or undergoing certain immunosuppressive therapies. Their immune systems may be too weak to mount a detectable inflammatory response. Other factors contributing to false negatives include very recent TB infection (where the immune system hasn’t yet sensitized), overwhelming TB disease, or errors in test administration or interpretation.
The Role of Technology in Improving Accuracy
The development and refinement of TB testing technologies have been ongoing. While the PPD skin test remains widely used due to its cost-effectiveness and accessibility, newer diagnostic tools are also emerging. Interferon-gamma release assays (IGRAs), such as the QuantiFERON-TB Gold Plus and the T-SPOT.TB test, are blood tests that measure the immune response to TB antigens directly. These tests have shown higher specificity than the skin test in certain populations, particularly in individuals who have received the BCG vaccine, as they are less likely to be affected by BCG-induced immunity.
The technology behind IGRAs involves sophisticated laboratory techniques for detecting and quantifying specific cytokines like IFN-γ. These assays offer an alternative approach to TB screening that can complement or, in some cases, replace the traditional skin test, especially in situations where serial testing is required or when distinguishing between latent TB infection and BCG vaccination is important.
Next Steps After a Positive TB Shot
A positive TB skin test is not a definitive diagnosis of active TB disease. Instead, it indicates that the individual has been infected with Mycobacterium tuberculosis at some point in their life. The next crucial step is to determine if the infection is latent (meaning the bacteria are present but not causing active disease) or if it has progressed to active TB disease, which is contagious.
Differentiating Latent TB Infection (LTBI) from Active TB Disease
Following a positive TST, further evaluation is necessary. This typically involves a chest X-ray to look for any signs of active disease in the lungs. If the chest X-ray is abnormal, sputum samples may be collected for microscopy and culture to detect the presence of live bacteria. Clinical symptoms such as persistent cough, fever, night sweats, and unexplained weight loss are also carefully assessed.
-
Latent TB Infection (LTBI): In cases of LTBI, the individual has TB bacteria in their body, but they are dormant and not causing illness. They are not contagious. Treatment for LTBI, often with a course of antibiotics, is highly effective in preventing the progression to active TB disease.
-
Active TB Disease: If active TB disease is diagnosed, treatment with a specific regimen of multiple antibiotics is initiated. This treatment is essential to cure the disease and prevent its spread to others. It is crucial for individuals with active TB to follow their treatment regimen meticulously to ensure successful recovery and prevent the development of drug-resistant TB.
The Importance of Follow-Up and Public Health
The accurate interpretation of a TB skin test and appropriate follow-up are critical public health measures. Early detection and treatment of both latent and active TB are essential for controlling the spread of the disease. Technological advancements in diagnostic tools, coupled with continued vigilance in screening and follow-up, play a vital role in the global strategy to eliminate TB. The seemingly simple visual interpretation of a skin reaction belies a complex interplay of immunology and sophisticated diagnostic technology that forms a crucial line of defense against this persistent infectious disease.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.