In the rapidly evolving landscape of personal technology, the boundary between medical-grade diagnostics and consumer electronics has blurred. We have entered the era of the “Quantified Self,” where tech enthusiasts, software engineers, and biohackers use sophisticated data points to optimize human performance. One of the most significant metrics currently dominating the health-tech sector is blood glucose monitoring. While traditionally reserved for clinical management of diabetes, understanding what constitutes “normal sugar levels” has become a foundational pillar for non-diabetics seeking to leverage technology for peak productivity, longevity, and metabolic efficiency.
This shift is driven by the realization that “normal” is a spectrum, and where an individual falls on that spectrum can be the difference between a mid-afternoon energy slump and sustained cognitive focus. By viewing glucose levels through the lens of data analytics and wearable hardware, we can transform a static biological marker into a dynamic tool for lifestyle optimization.
The Hardware Revolution: From Finger Pricks to Continuous Glucose Monitors (CGMs)
The technological journey of glucose monitoring has transitioned from invasive, episodic testing to seamless, real-time data streams. For a non-diabetic, the interest in sugar levels is rarely about immediate survival; it is about the “user experience” of their own biology.
From Medical Devices to Consumer Wearables
For decades, blood glucose monitoring required manual lancing and test strips—a reactive approach that provided only a snapshot in time. However, the rise of Continuous Glucose Monitors (CGMs), such as those developed by Dexcom and Abbott, has revolutionized the field. These devices use a small filament inserted under the skin to measure glucose levels in the interstitial fluid every few minutes.
Originally designed for Type 1 and Type 2 diabetics, these sensors are now being integrated into high-end consumer tech ecosystems. Startups are bridging the gap between medical hardware and sleek mobile applications, allowing non-diabetics to track their metabolic response to specific stimuli—like a high-stress meeting or a specific software development sprint—in real-time.
The Engineering of Subcutaneous Sensors
The technology behind these sensors involves complex enzyme-based electrochemical reactions. A glucose oxidase enzyme on the sensor reacts with glucose, producing an electrical signal that is processed by a tiny transmitter. This transmitter then sends the data via Bluetooth to a smartphone or smartwatch. For the tech-focused user, this is more than a medical reading; it is a live telemetry feed of their internal combustion engine. Understanding the “normal” range is the first step in calibrating this sophisticated piece of biological hardware.
Analyzing the Data: What Defines “Normal” in a Tech-Driven Context?
To optimize any system, one must first establish a baseline. In the world of metabolic tech, “normal” sugar levels for a non-diabetic are generally categorized by two states: fasting levels and post-prandial (after eating) levels. However, health-tech platforms are now arguing that the standard clinical “normal” might be too broad for those seeking optimal performance.
Decoding the Benchmarks: Fasting and Post-Prandial Data
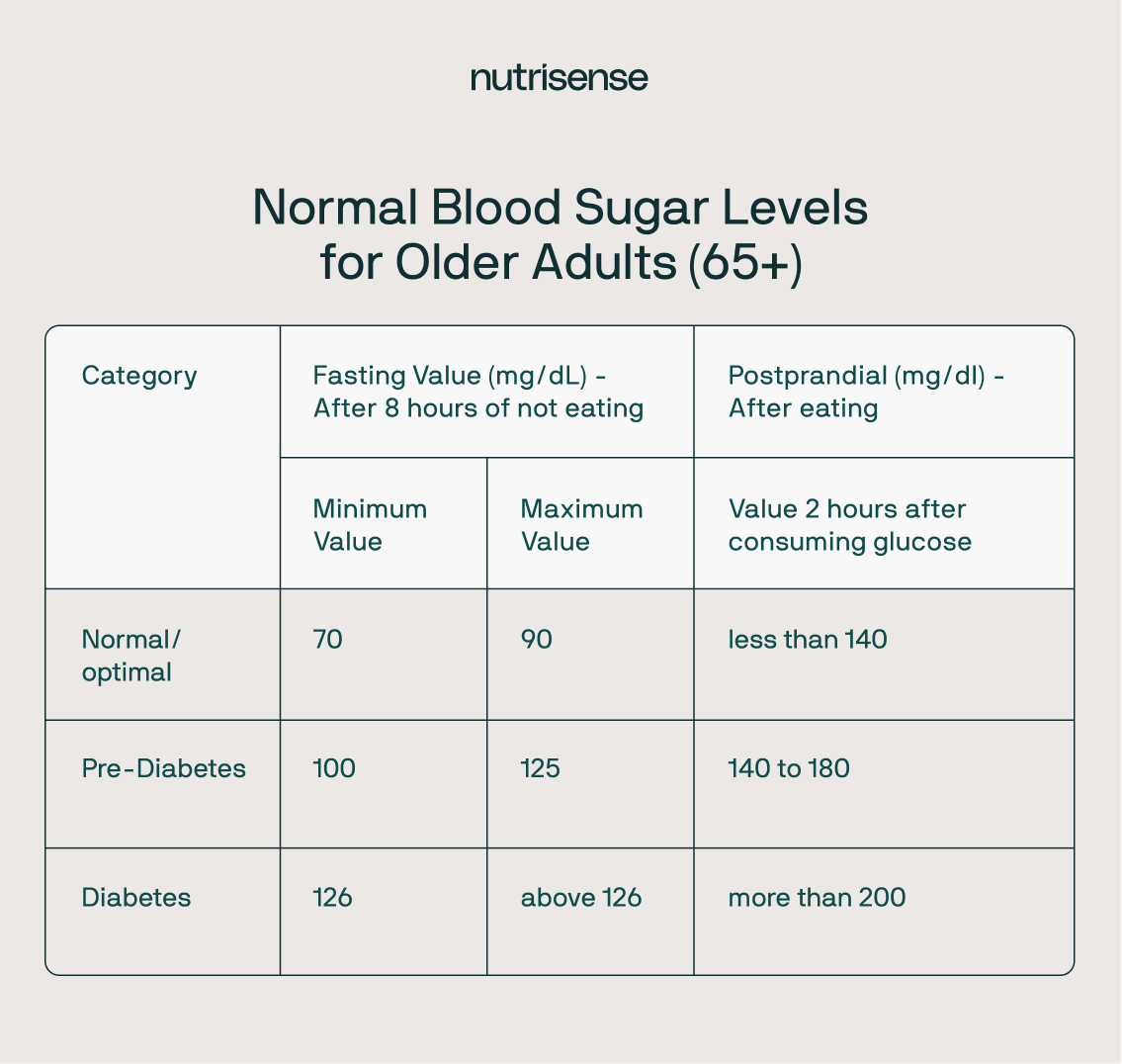
In a clinical setting, a fasting blood sugar level between 70 and 99 mg/dL (3.9 to 5.5 mmol/L) is considered normal for a non-diabetic. After a meal, levels should typically stay below 140 mg/dL (7.8 mmol/L) when measured two hours later.
From a technology and performance standpoint, many biohackers aim for a “tighter” range. They use apps to ensure their levels stay between 70 and 110 mg/dL throughout the day, minimizing the “glucose spikes” that trigger insulin surges. By maintaining this narrow band, users aim to avoid the neuro-inflammatory effects of high sugar and the “brain fog” associated with the subsequent crash. The goal is a flat, stable line on the graph—the ultimate visual representation of metabolic stability.
AI-Driven Insights vs. Static Clinical Ranges
The true power of modern health tech lies in its ability to provide context. A “normal” reading of 130 mg/dL means something very different if you just finished a high-intensity interval training (HIIT) session versus if you have been sitting at a desk for six hours.
New AI-driven platforms analyze glucose data alongside sleep cycles from an Oura ring, heart rate variability (HRV) from an Apple Watch, and caloric intake from logging apps. These algorithms provide a “Metabolic Score,” which interprets sugar levels through the lens of individual variability. This is the shift from “General Health” to “Personalized Precision Tech,” where “normal” is defined by your unique recovery needs and energy expenditures.

Digital Security and the Ethics of Biological Data
As we integrate our biological markers into the cloud, the conversation naturally shifts toward digital security and data privacy. Tracking sugar levels generates a massive amount of highly personal biometric data, creating both opportunities for discovery and risks for exploitation.
Privacy, Encryption, and Interoperability
Biometric data is among the most sensitive information a person can generate. When non-diabetics use third-party apps to interpret their CGM data, they are often uploading their metabolic “source code” to a company’s servers. Ensuring that this data is protected via end-to-end encryption and stored in HIPAA-compliant (or equivalent) environments is paramount.
Furthermore, the tech industry is pushing for greater interoperability. The goal is to create a seamless “Health Stack” where glucose data can be securely shared between different software tools—such as an AI nutritionist or a fitness coaching platform—without compromising the user’s digital identity or security.
The Future of Biometric Cloud Storage
As more non-diabetics adopt these tools, we are seeing the emergence of “decentralized health data.” Some blockchain-based startups are exploring ways for individuals to own their biological data, granting temporary access to researchers or clinicians in exchange for tokens or services. This ensures that the record of your “normal sugar levels” remains your property, shielded from insurance companies or data brokers who might use that information to adjust premiums or target advertising based on your metabolic vulnerabilities.
The Future of Preventative Tech: Machine Learning and Predictive Analytics
The ultimate goal of tracking sugar levels for non-diabetics is not just to see what is happening now, but to predict what will happen in the future. We are moving from descriptive analytics (what happened?) to predictive and prescriptive analytics (what will happen, and what should I do?).
Machine Learning and Metabolic Pattern Recognition
Modern health-tech platforms use machine learning to recognize patterns that the human eye might miss. For example, an app might notice that every time a user has poor sleep (tracked via wearable), their sugar levels are 15% higher the next morning after a standard breakfast.
By identifying these correlations, the software can provide preemptive nudges. If the sensor detects a sharp rise in glucose, the user’s smartwatch might suggest a ten-minute walk to increase insulin sensitivity and “blunt” the spike before it affects their cognitive performance. This is the pinnacle of “Human-in-the-Loop” systems, where technology acts as an external pre-frontal cortex, helping the user make better decisions for their biological hardware.
Shifting the Healthcare Paradigm: From Illness to Optimization
The widespread adoption of glucose-tracking tech by non-diabetics represents a fundamental shift in the healthcare industry. For decades, the model has been “Break-Fix”—wait until a metric falls outside the normal range (diabetes) and then intervene.
The tech-centric approach is “Prevent-Optimize.” By monitoring sugar levels while they are still “normal,” users can identify the earliest signs of metabolic dysfunction—such as rising fasting levels or delayed recovery after meals—years before they would trigger a clinical diagnosis. This proactive stance, fueled by real-time data and sophisticated software, is turning the human body into a transparent, tunable system.

Conclusion: The New Standard of Digital Wellness
Understanding “normal sugar levels for non-diabetics” is no longer just a medical query; it is a data-driven pursuit of excellence. In the niche of health technology, glucose is viewed as a primary fuel source whose regulation is key to unlocking the next level of human potential.
As sensors become smaller, cheaper, and more accurate, and as AI continues to refine our understanding of metabolic data, the “Quantified Self” will become the “Optimized Self.” By treating our biology with the same rigor we treat our software and hardware systems, we can ensure that our “normal” is not just the absence of disease, but the presence of peak performance. Through the lens of technology, the blood sugar graph is more than just a line; it is a roadmap to a more resilient and efficient human experience.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.