Amyotrophic Lateral Sclerosis (ALS), often referred to as Lou Gehrig’s disease, is a devastating neurodegenerative condition that progressively paralyzes individuals by attacking motor neurons. These specialized nerve cells are responsible for transmitting signals from the brain to the muscles, enabling voluntary movement. As ALS progresses, these neurons die, leading to muscle weakness, atrophy, and eventually, the inability to perform basic functions like walking, speaking, swallowing, and breathing. While the exact cause of ALS remains largely unknown, research is continuously advancing, offering hope for better understanding, management, and ultimately, a cure. This article will delve into the complexities of ALS, exploring its symptoms, diagnosis, current treatment approaches, and the ongoing scientific efforts to combat this relentless disease.
Understanding the Neurological Impact of ALS
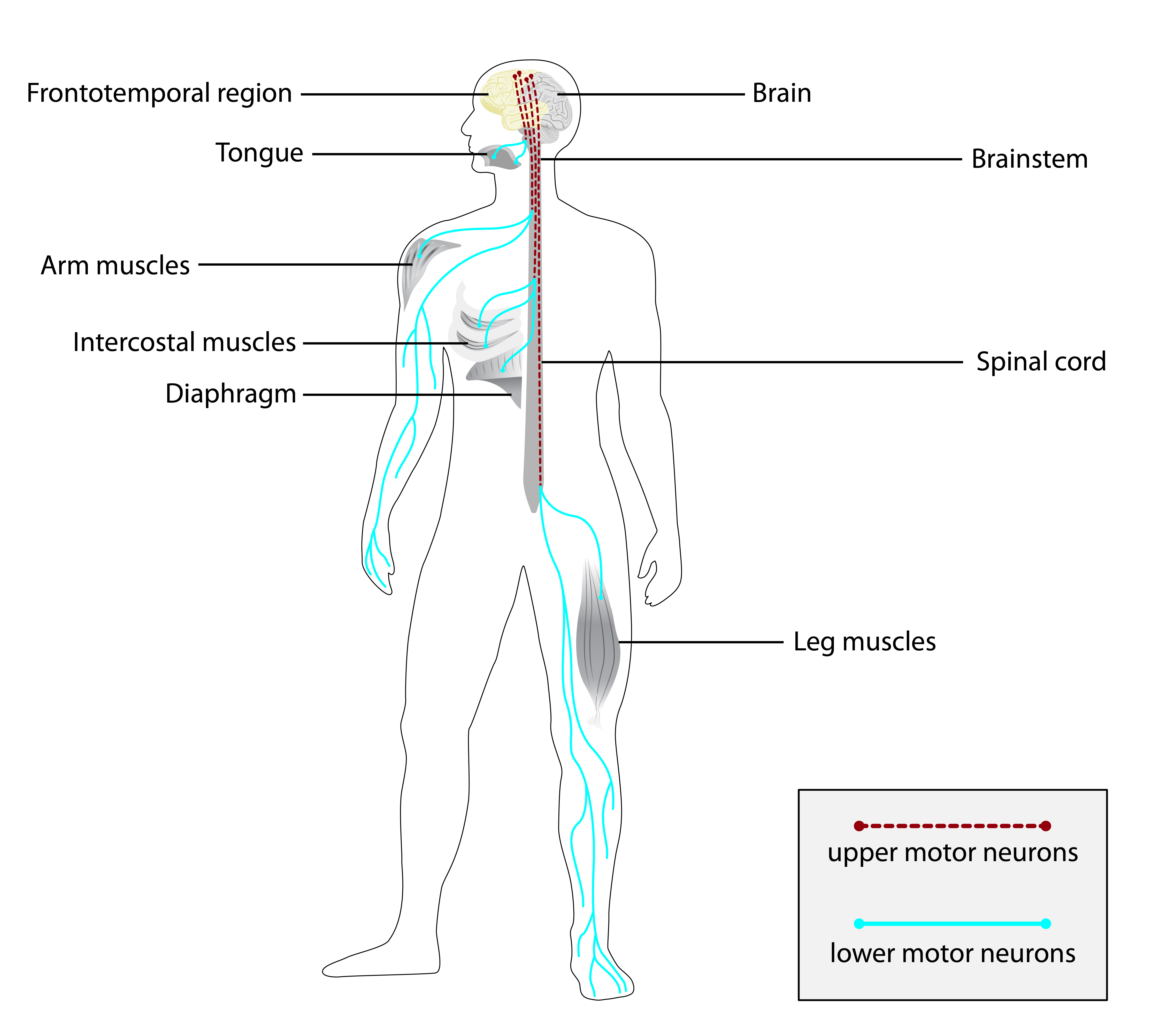
At its core, ALS is a disease of the motor neurons. These neurons are organized into two primary systems: the upper motor neurons, originating in the brain and controlling voluntary movements, and the lower motor neurons, extending from the spinal cord to the muscles. In ALS, both upper and lower motor neurons are affected, leading to a cascade of symptoms. The degeneration of these neurons disrupts the communication pathway between the brain and muscles, resulting in a progressive loss of motor control. This neural breakdown is insidious, often beginning with subtle signs that can be easily overlooked, only to escalate into significant functional impairment. The progressive nature of ALS means that as more motor neurons are lost, the affected muscles weaken, become spastic, and eventually waste away.
The Degeneration of Motor Neurons
The primary pathological hallmark of ALS is the degeneration of motor neurons in the cerebral cortex, brainstem, and spinal cord. While the exact trigger for this neuronal death is still a subject of intense research, several theories are being explored. Oxidative stress, excitotoxicity (overstimulation of neurons by certain neurotransmitters), protein aggregation, and mitochondrial dysfunction are among the leading candidates. These cellular processes can lead to the accumulation of abnormal proteins within the neurons, disrupting their normal function and ultimately leading to their demise. The progressive loss of these critical cells is what underlies the characteristic muscle weakness and atrophy seen in ALS patients.
Upper vs. Lower Motor Neuron Involvement
The distinction between upper and lower motor neuron involvement is crucial in understanding the diverse manifestations of ALS. Damage to upper motor neurons can lead to spasticity, hyperreflexia (exaggerated reflexes), and a positive Babinski sign (an abnormal reflex in the foot). Conversely, damage to lower motor neurons results in flaccid paralysis, muscle atrophy (wasting), fasciculations (involuntary muscle twitches), and hyporeflexia (diminished reflexes). In ALS, patients often exhibit a combination of both upper and lower motor neuron signs, a characteristic feature known as a “mixed” presentation. This dual impact explains the wide spectrum of symptoms experienced by individuals with the disease, affecting various muscle groups and bodily functions.
Symptoms and Diagnosis of ALS
The onset of ALS symptoms can vary significantly from person to person, making early diagnosis a challenge. Symptoms typically begin subtly, often affecting one limb or a specific muscle group before spreading. As the disease progresses, these symptoms become more pronounced and widespread, impacting the individual’s ability to perform everyday tasks. The diagnostic process for ALS is complex, relying on a combination of neurological examination, medical history, and exclusion of other neurological conditions. There is no single definitive test for ALS; instead, diagnosis is made through a process of elimination and by identifying characteristic patterns of neurological deficits.
Early Signs and Progression
Initial symptoms of ALS can be very diverse. Common early signs include:
- Muscle Weakness: Often noticeable in the hands and feet, leading to difficulty with fine motor skills, such as buttoning clothes or writing, or with walking and maintaining balance.
- Muscle Twitching and Spasms (Fasciculations): Small, involuntary muscle contractions that can be seen under the skin, often described as a “rippling” sensation.
- Slurred Speech (Dysarthria): Difficulty articulating words due to weakness in the muscles of the tongue, lips, and throat.
- Difficulty Swallowing (Dysphagia): Trouble with chewing and swallowing food, which can lead to choking or aspiration.
- Fatigue: Profound tiredness that is not relieved by rest.
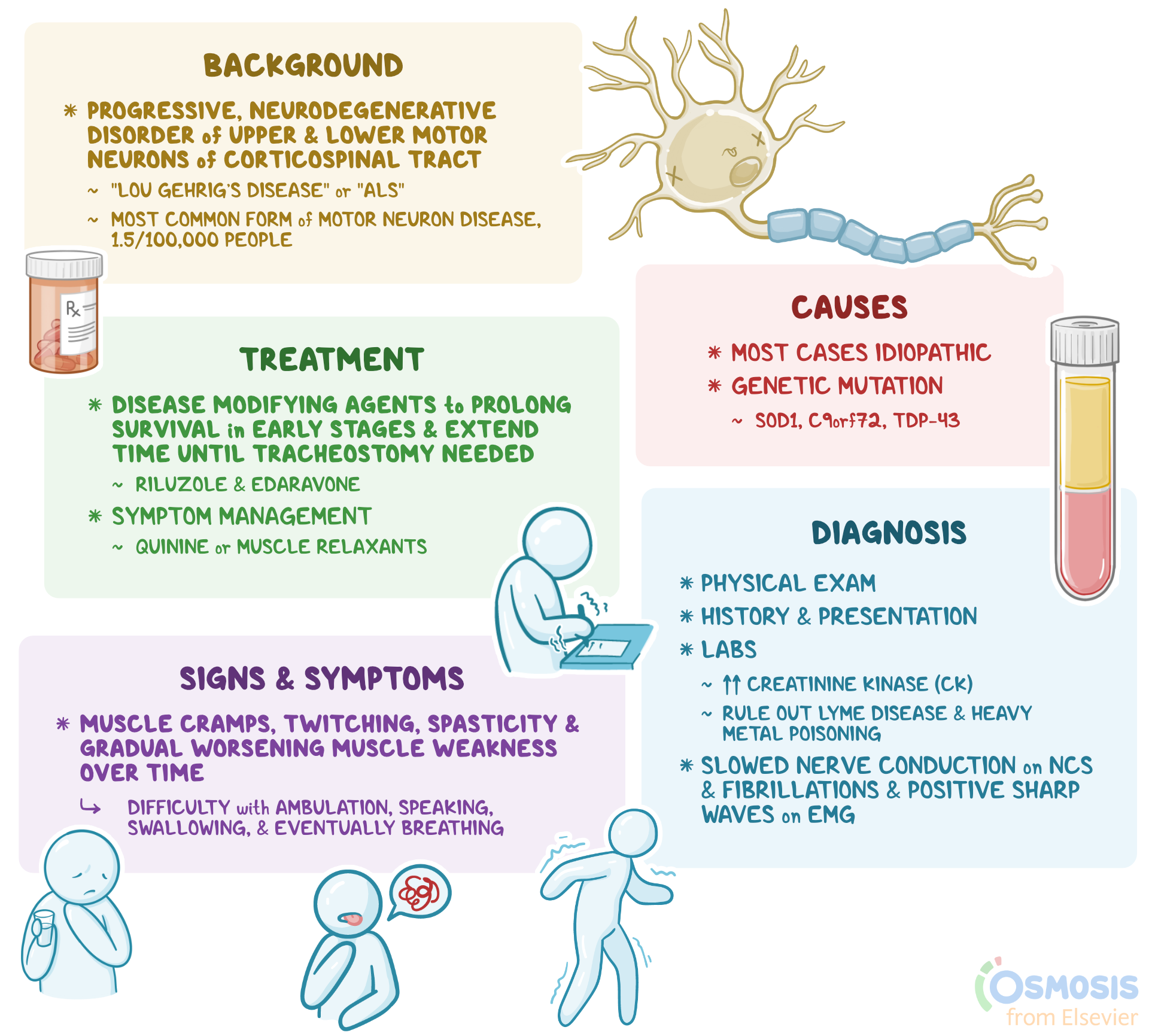
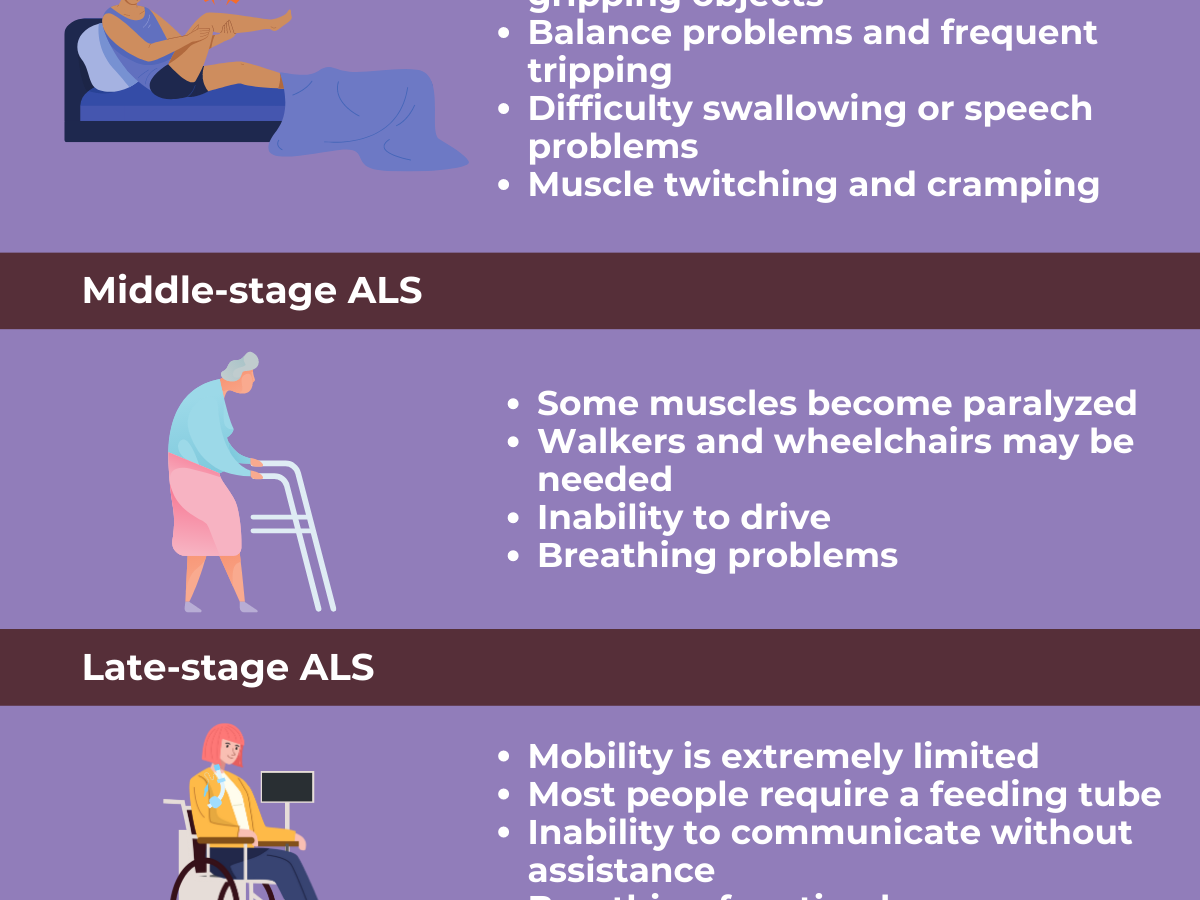
As ALS progresses, these symptoms worsen, and new ones emerge. The disease typically affects all voluntary muscles, but involuntary functions like heart rate, blood pressure, and digestion are usually spared. Crucially, ALS does not affect a person’s intellect or consciousness, meaning individuals remain aware and mentally engaged even as their physical abilities decline.
Diagnostic Pathways and Challenges
Diagnosing ALS is a meticulous process that requires the expertise of neurologists, particularly those specializing in neuromuscular disorders. The diagnostic pathway typically involves:
- Detailed Medical History and Neurological Examination: The physician will inquire about the patient’s symptoms, their progression, and family history, followed by a thorough examination assessing muscle strength, reflexes, coordination, and sensory function.
- Electromyography (EMG) and Nerve Conduction Studies (NCS): These tests evaluate the electrical activity of muscles and the speed at which nerve impulses travel. EMG can detect signs of nerve damage and muscle dysfunction characteristic of ALS.
- Magnetic Resonance Imaging (MRI): While MRI cannot definitively diagnose ALS, it is crucial for ruling out other conditions that can mimic ALS symptoms, such as spinal cord compression, tumors, or multiple sclerosis.
- Blood Tests: These are used to exclude other conditions, such as vitamin deficiencies or autoimmune diseases, that could be causing similar symptoms.
- Lumbar Puncture (Spinal Tap): In some cases, this procedure may be performed to analyze cerebrospinal fluid, again to rule out other neurological disorders.
The absence of a single, definitive diagnostic marker for ALS is a significant challenge. Diagnosis is often made after a period of observation and testing, which can be a stressful and uncertain time for patients and their families.
Current Treatments and Future Directions in ALS Research
While there is currently no cure for ALS, significant advancements have been made in managing the disease and improving the quality of life for individuals living with it. Treatment strategies focus on alleviating symptoms, slowing disease progression, and providing supportive care. The landscape of ALS research is dynamic, with a constant influx of new studies exploring potential therapeutic targets and innovative treatment approaches.
Symptomatic Management and Supportive Care
The cornerstone of ALS management lies in a multidisciplinary approach that addresses the diverse needs of patients. This includes:
- Medications: Riluzole, an oral medication, is the only FDA-approved drug shown to modestly extend survival in ALS patients by potentially reducing damage to motor neurons. Edaravone, another FDA-approved drug administered intravenously, has also shown some benefit in slowing functional decline in certain ALS patient populations.
- Respiratory Support: As ALS progresses, breathing muscles weaken, often necessitating non-invasive ventilation (NIV) or, in advanced stages, a tracheostomy with mechanical ventilation.
- Nutritional Support: Dysphagia can lead to malnutrition. A feeding tube (gastrostomy tube) is often recommended to ensure adequate nutrition and hydration.
- Speech and Physical Therapy: These therapies are vital for maintaining as much function as possible. Speech therapists help with communication strategies and swallowing techniques, while physical therapists assist with mobility, exercise, and assistive devices.
- Occupational Therapy: Occupational therapists help patients adapt their environment and learn new strategies to perform daily activities.
- Psychological Support: The emotional toll of ALS is immense. Counseling and support groups are crucial for patients and their families to cope with the challenges of the disease.
Promising Avenues in Research
The scientific community is actively pursuing a variety of promising research avenues to unravel the mysteries of ALS and develop effective treatments:
- Genetics: Identifying genetic mutations linked to ALS, such as those in the C9orf72 gene, has opened doors for gene-targeting therapies. Research is exploring gene silencing and gene replacement strategies.
- Stem Cell Therapy: Investigating the potential of stem cells to replace damaged motor neurons or provide neurotrophic support is a significant area of research.
- Drug Development: A vast array of novel drug candidates are undergoing preclinical and clinical trials, targeting mechanisms like protein misfolding, inflammation, and excitotoxicity.
- Biomarker Discovery: Researchers are working to identify reliable biomarkers that can aid in early diagnosis, track disease progression, and predict treatment response.
- Understanding Disease Mechanisms: Continued exploration into the cellular and molecular pathways that lead to motor neuron degeneration is fundamental to developing targeted therapies.
The collaborative efforts of researchers worldwide, coupled with increased patient participation in clinical trials, offer a beacon of hope for a future where ALS can be effectively treated, managed, and potentially even prevented. While the journey is challenging, the dedication to understanding and conquering ALS continues to drive innovation and bring us closer to finding answers.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.