In the modern medical landscape, the intersection of biology and technology has birthed diagnostic tools that are more precise, faster, and more accessible than ever before. Among the most significant advancements in clinical laboratory science is the development and refinement of the Enzyme-Linked Immunosorbent Assay, commonly known as ELISA. While traditional methods of blood typing—such as the simple ABO/Rh slide agglutination—remain foundational, the integration of ELISA technology has revolutionized how we screen blood for complex antibodies, pathogens, and metabolic markers.
Understanding the technological nuances of blood analysis is essential for grasping the future of personalized medicine. This article explores the mechanics of ELISA, its role in modern blood diagnostics, and the technological infrastructure that supports high-throughput medical testing.
Understanding the Technology: What is ELISA?
To understand how blood components are analyzed at a granular level, one must first look at the technology behind ELISA. At its core, ELISA is a biochemical technique used primarily in immunology to detect the presence of an antibody or an antigen in a sample. It is a cornerstone of biotechnology, bridging the gap between raw biological samples and digital data.
The Mechanics of Enzyme-Linked Immunosorbent Assay
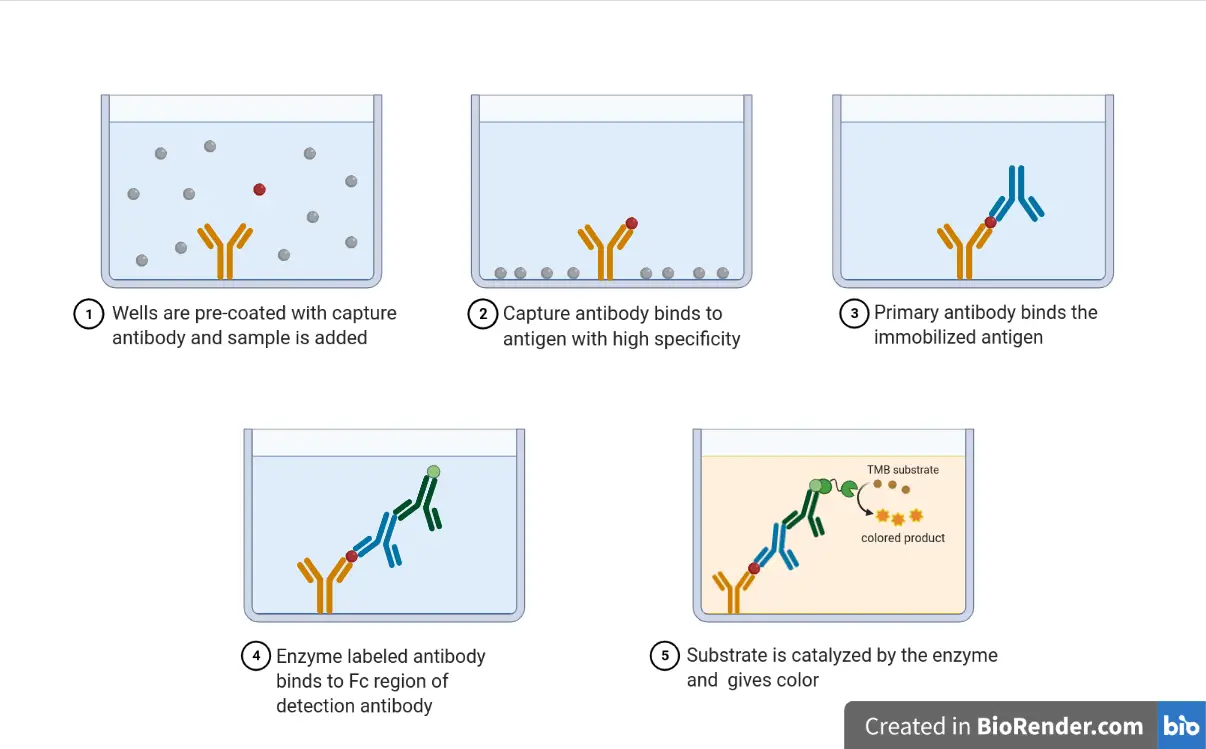
The “magic” of ELISA lies in its specificity. The process utilizes a “solid phase” (usually a polystyrene multi-well plate) where specific antibodies or antigens are immobilized. When a patient’s blood sample is introduced, the target molecule binds to the immobilized agent. A subsequent “reporting” enzyme is added, which triggers a color change—a signal that can be measured using sophisticated optical sensors.
This technological approach allows for quantification. Unlike manual tests that simply provide a “positive” or “negative” result, ELISA can determine the exact concentration of a substance in the bloodstream. This precision is vital for monitoring therapeutic drug levels, hormonal imbalances, and viral loads.
Different Types of ELISA Architectures
The technology is not monolithic; it has evolved into several specialized configurations:
- Direct ELISA: The simplest form, where an antigen is adsorbed to a plastic plate and a labeled antibody binds to it.
- Indirect ELISA: Uses a secondary antibody for detection, increasing the sensitivity of the test.
- Sandwich ELISA: The most powerful format for blood analysis, where the analyte is “sandwiched” between two layers of antibodies, ensuring extremely high specificity.
- Competitive ELISA: Often used when the target molecule is small, providing a unique way to measure concentration through interference.
Applying ELISA to Blood Identification and Immunoassays
When a patient asks, “What test do you do to check blood type?” the answer usually involves agglutination. However, when we move into the realm of complex blood screening—such as cross-matching for organ transplants or detecting rare blood group antibodies—ELISA-based technology becomes indispensable.
The Role of Antigens and Antibodies in Digital Detection
Blood typing is essentially an exercise in identifying surface antigens on red blood cells. While traditional methods rely on the visual clumping of cells, ELISA technology digitizes this process. By using enzyme-linked reactions, labs can detect subtle variations in blood group sub-types that a manual slide test might miss. This is particularly critical in “weak D” testing or when identifying rare phenotypes that could cause a transfusion reaction.
Comparing ELISA with Traditional Agglutination Methods
The shift from manual agglutination to automated ELISA-based platforms represents a significant technological leap. Traditional methods are prone to human error—misreading a faint clump or timing the reaction incorrectly. ELISA, however, is conducted within automated plate readers. These machines use spectrophotometry to measure light absorbance at specific wavelengths, converting a chemical reaction into a precise numerical value. This transition from qualitative (visual) to quantitative (digital) analysis is the hallmark of modern laboratory technology.
The Technological Infrastructure of Modern Blood Labs
The efficiency of a modern diagnostic center does not rely solely on the chemical assay itself, but on the integrated technology stack that supports it. From robotics to cloud-based data management, the ecosystem of a blood lab is a marvel of engineering.
Automated Platforms and Robotic Integration
High-volume laboratories utilize Liquid Handling Systems (LHS) to perform ELISA and other blood tests. These robotic arms can pipette microliter volumes of blood and reagents into 96-well or 384-well plates with a precision that far exceeds human capabilities.
Automation reduces the risk of cross-contamination and ensures that every sample is treated under identical environmental conditions (temperature, incubation time, and humidity). This consistency is what allows global healthcare systems to maintain standardized results, ensuring that a blood type recorded in one country is recognized and verified by another.
Software and Data Management in Serology
Behind every ELISA reader is a powerful suite of software. Laboratory Information Systems (LIS) track a sample from the moment the needle hits the patient’s arm to the moment the result is uploaded to an Electronic Health Record (EHR).
In the context of blood typing and screening, these software platforms use complex algorithms to interpret the “optical density” (OD) provided by the ELISA reader. If an OD value falls within a certain range, the software automatically flags the sample for retesting or confirms a specific antibody presence. This digital gatekeeping minimizes the “gray areas” in medical diagnostics, providing clinicians with actionable data.
Future Trends in Diagnostic Biotechnology
As we look toward the future of blood testing technology, the focus is shifting from large-scale centralized laboratories to decentralized, immediate testing. The goal is to make the power of ELISA and complex blood typing available at the point of care.
Point-of-Care Testing (POCT) and Microfluidics
One of the most exciting trends in tech is “Lab-on-a-Chip.” This technology seeks to shrink the entire ELISA process onto a small disposable cartridge. Using microfluidics, tiny amounts of blood are moved through microscopic channels where they react with pre-loaded reagents.
For blood typing, this could mean that a first responder in a remote area could determine a patient’s precise blood profile in minutes using a handheld device. This tech-driven accessibility has the potential to save thousands of lives in emergency trauma situations where every second counts.
AI and Machine Learning in Blood Analysis
Artificial Intelligence is now being integrated into diagnostic hardware to assist in pattern recognition. While ELISA provides highly accurate data, the interpretation of results in patients with multiple comorbidities or rare autoimmune disorders can be complex.
Machine learning models are being trained on millions of previous ELISA results to identify “signatures” of rare blood conditions. By analyzing data points that might seem insignificant to a human technician, AI can predict potential complications in blood transfusions or identify early markers of blood-borne diseases long before symptoms appear. This proactive approach marks the transition from reactive diagnostics to predictive health technology.

Conclusion: The Digital Future of Serology
The question of “what test do you do to check blood type” may have a simple clinical answer, but the technological reality is a sophisticated blend of biochemistry, robotics, and digital analysis. While ELISA is often the unsung hero of the lab, its ability to provide sensitive, quantifiable, and automated results has made it a pillar of modern biotechnology.
As we continue to refine these tools—miniaturizing the hardware through microfluidics and enhancing the software through AI—the accuracy of blood analysis will only increase. We are moving toward a world where blood typing and screening are not just clerical checkboxes in a medical file, but are data-rich insights that empower both doctors and patients to make more informed decisions about their health. The synergy between biological assays like ELISA and cutting-edge technology ensures that the future of medicine is faster, safer, and infinitely more precise.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.