The escalating rates of obesity among adults in the United States represent a complex public health challenge with profound implications across various sectors, including healthcare, economics, and individual well-being. Understanding the precise percentage of adults affected is crucial for developing targeted interventions, allocating resources effectively, and fostering a national dialogue around health and lifestyle. This article delves into the current statistics, explores the contributing factors, and examines the multifaceted impact of obesity on the U.S. adult population, with a particular focus on its financial ramifications and the role of financial literacy in addressing this crisis.
The Shifting Landscape of Adult Obesity in the U.S.
The prevalence of obesity in the United States has been a growing concern for decades, with recent data painting a stark picture of its widespread impact. This section will explore the most up-to-date statistics and trends, highlighting the demographic variations and the evolution of obesity rates over time.
Current Prevalence and Trends
According to the most recent data from leading health organizations such as the Centers for Disease Control and Prevention (CDC) and the National Center for Health Statistics (NCHS), the percentage of adults in the U.S. classified as obese has continued to rise, albeit with some fluctuations. Obesity is generally defined as having a Body Mass Index (BMI) of 30 or higher. Recent estimates suggest that approximately 40% of U.S. adults fall into this category. This figure represents a significant portion of the adult population and underscores the chronic nature of this health issue.
Beyond the overall percentage, it’s important to acknowledge trends. While rates have stabilized somewhat in recent years compared to the rapid increases seen in the late 20th and early 21st centuries, they remain persistently high. This stabilization may be attributed to increased awareness and a growing number of public health initiatives, but the sheer number of individuals affected continues to present a substantial burden.
Demographic Disparities
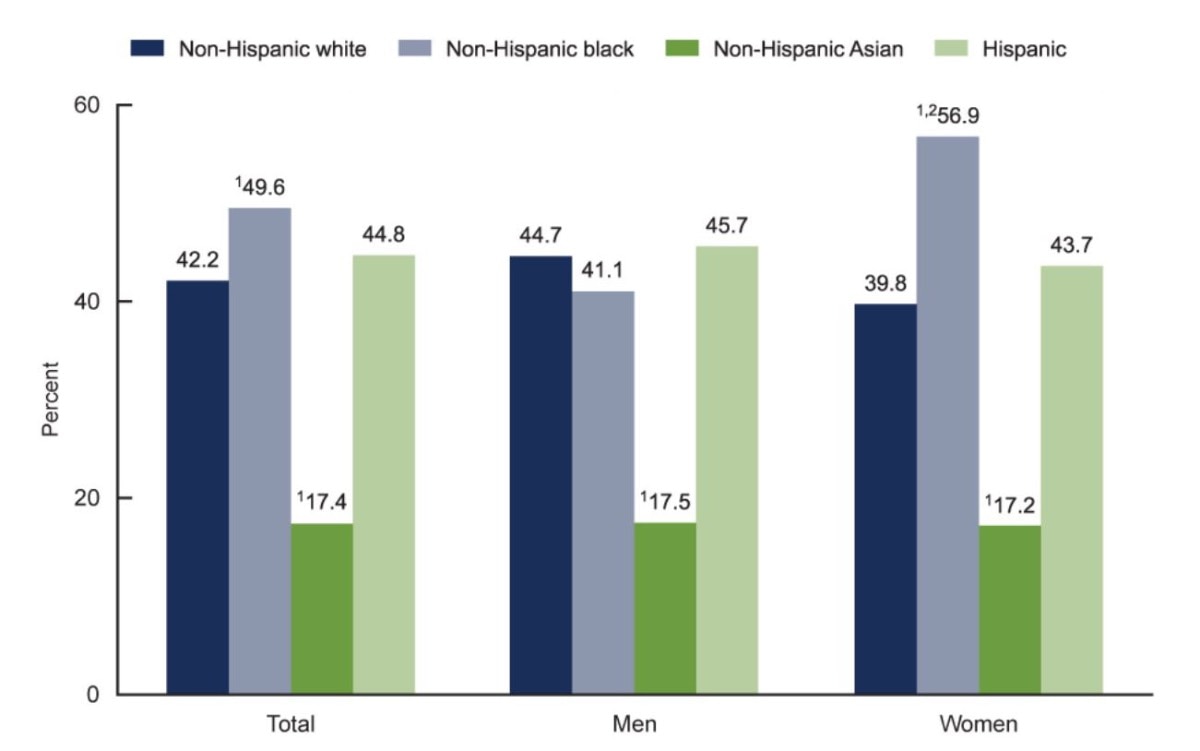
Obesity is not uniformly distributed across the U.S. adult population. Significant disparities exist across racial, ethnic, socioeconomic, and geographic lines. For instance, certain racial and ethnic minority groups, particularly Black and Hispanic adults, tend to have higher rates of obesity compared to their White and Asian counterparts. These disparities are often linked to a complex interplay of factors including genetics, access to healthy food options (food deserts), availability of safe spaces for physical activity, cultural dietary practices, and systemic socioeconomic disadvantages that can influence health behaviors and outcomes.
Geographically, obesity rates can vary by state and even by urban versus rural areas. Rural populations, for example, may face challenges related to limited access to healthcare services, fewer opportunities for physical recreation, and a higher prevalence of food environments that favor less healthy options. Understanding these disparities is critical for tailoring public health strategies to be culturally relevant and accessible to all segments of the population.
The Financial Burden of Adult Obesity
The personal and societal costs associated with obesity extend far beyond individual health, creating a substantial financial strain on individuals, families, and the broader economy. This section will explore the direct and indirect financial implications of widespread obesity.
Increased Healthcare Expenditures
One of the most significant financial consequences of adult obesity is the dramatic increase in healthcare expenditures. Obese individuals are at a higher risk of developing a multitude of chronic diseases, including type 2 diabetes, heart disease, stroke, certain types of cancer, osteoarthritis, and sleep apnea. The management and treatment of these conditions necessitate frequent doctor visits, hospitalizations, prescription medications, and specialized medical procedures.
Studies have consistently shown that individuals with obesity incur significantly higher annual healthcare costs compared to those with a healthy weight. These costs are borne by individuals through insurance premiums and out-of-pocket expenses, as well as by employers and government programs that provide health insurance coverage. The U.S. healthcare system is already burdened by escalating costs, and the prevalence of obesity exacerbates this challenge, diverting valuable resources that could be used for other critical health initiatives or societal needs. The direct medical costs associated with obesity have been estimated to be in the tens of billions, if not hundreds of billions, of dollars annually.
Lost Productivity and Economic Impact
Beyond direct medical costs, obesity has a profound impact on economic productivity. Individuals struggling with obesity-related health issues may experience more frequent sick days, reduced physical capacity for their jobs, and a diminished ability to perform tasks efficiently. This can lead to lower overall productivity in the workforce, impacting businesses and the national economy.
Moreover, obesity can affect career advancement and earning potential. Some studies suggest a correlation between higher BMI and lower wages, potentially due to factors like employer discrimination (though often subconscious or subtle), reduced job opportunities, or limitations in physical roles. The cumulative effect of reduced individual earning potential and decreased workforce productivity represents a substantial economic drain. Industries that rely on physical labor or require sustained energy levels can be particularly affected. The estimated economic cost due to lost productivity and disability associated with obesity further adds to the multi-billion dollar annual burden.
The Cost of Prevention and Management Programs
While the cost of treating obesity-related conditions is substantial, significant financial resources are also dedicated to prevention and management programs. These include public health campaigns, educational initiatives, subsidies for healthy food, and funding for research into effective weight management strategies. While these investments are crucial for long-term health and economic well-being, they represent an ongoing financial commitment.
Furthermore, the market for weight-loss products, diet plans, and fitness services is enormous, reflecting both the desire of individuals to manage their weight and the economic opportunities arising from this public health issue. While these industries can provide valuable support, they also highlight the significant financial investment the nation makes in addressing obesity, both proactively and reactively.
Addressing the Obesity Epidemic: A Financial Literacy Perspective
While tackling obesity requires a multi-pronged approach involving healthcare, public policy, and individual behavior change, understanding the financial implications of poor health choices can serve as a powerful motivator for individuals to prioritize their well-being. This section will explore how financial literacy can play a crucial role in empowering individuals to make healthier, more financially sound decisions.
The Interplay Between Financial Health and Physical Health
There is a well-documented, bidirectional relationship between financial well-being and physical health. Individuals facing financial insecurity often experience chronic stress, which can contribute to unhealthy eating habits and a lack of motivation for physical activity. Limited financial resources can also restrict access to nutritious food, safe environments for exercise, and quality healthcare. Conversely, poor health due to obesity can lead to increased medical expenses, reduced earning potential, and greater financial strain, creating a vicious cycle.
Financial literacy equips individuals with the knowledge and skills to manage their money effectively, build savings, and make informed decisions about spending. When individuals understand the long-term financial consequences of health-related conditions, including the direct costs of medical care and the indirect costs of lost income, they may be more motivated to adopt healthier lifestyles. This understanding can empower them to prioritize preventative health measures, which are often more cost-effective in the long run than treating chronic diseases.
Budgeting for Health: Making Healthy Choices Affordable
A key component of financial literacy is budgeting. By effectively budgeting, individuals can identify areas where they can allocate funds towards healthier choices. This might involve planning meals to reduce reliance on expensive convenience foods, setting aside money for gym memberships or fitness classes, or investing in healthier groceries. Many individuals mistakenly believe that healthy eating is inherently more expensive than unhealthy eating. While some specialized health foods can be costly, a diet rich in whole grains, fruits, vegetables, and lean proteins can be surprisingly affordable when planned effectively.
Learning to cook at home, planning weekly menus, buying in-season produce, and utilizing coupons can significantly reduce food expenses while improving nutritional intake. Financial literacy programs can incorporate modules on how to budget for healthy meals and snacks, demystifying the process and making it accessible to individuals from all socioeconomic backgrounds.
Understanding Health Insurance and Its Value
Navigating the complexities of health insurance can be daunting, but understanding its value is crucial for financial well-being, especially when dealing with health conditions like obesity. Financial literacy can empower individuals to make informed decisions about their health insurance plans, understanding deductibles, co-pays, and covered services. This knowledge can help them utilize their insurance effectively for preventative care, screenings, and necessary medical treatments, thereby mitigating the financial impact of health issues.
Furthermore, understanding the link between lifestyle choices and insurance premiums can be a powerful motivator. Insurers are increasingly recognizing the impact of lifestyle factors on health outcomes, and while direct premium adjustments based solely on weight are complex and often regulated, promoting healthier lifestyles can lead to overall lower healthcare costs for individuals and society, potentially influencing future insurance market dynamics. Financial literacy education should include a component on how to leverage health insurance for proactive health management and disease prevention.
The Broader Societal and Economic Implications
The prevalence of adult obesity in the U.S. extends beyond individual health and immediate financial concerns, impacting societal structures and the broader economic landscape in profound ways. This section will examine these wider ramifications.
Strain on Social Programs and Infrastructure
High rates of obesity and related chronic diseases place a significant strain on public health systems and social safety nets. Government programs like Medicare and Medicaid bear a substantial portion of the healthcare costs associated with obesity. As the obese population grows, so does the demand on these programs, potentially impacting their long-term sustainability and requiring increased taxpayer contributions.
Beyond direct healthcare costs, obesity can also influence demand for other social services. For instance, individuals with severe obesity-related mobility issues may require greater access to disability services and specialized transportation. The cumulative effect is a significant financial burden that impacts the allocation of public resources and the overall economic health of the nation.
Impact on Workforce Development and Future Economic Growth
A healthier workforce is a more productive workforce. The long-term trend of rising obesity rates poses a risk to future economic growth. A population with a higher prevalence of chronic health conditions may lead to a less physically capable and mentally resilient workforce. This can hinder innovation, reduce output, and make the nation less competitive in the global economy.
Investing in public health initiatives that promote healthy lifestyles and prevent obesity is not just a health imperative but also an economic strategy. By fostering a culture of well-being, the U.S. can aim to reduce the future burden of chronic disease, improve workforce productivity, and ensure sustained economic prosperity for generations to come. This requires a commitment to comprehensive strategies that address the multifaceted drivers of obesity, from early childhood education to accessible healthcare and supportive community environments.

The Role of Policy and Investment in Combating Obesity
Effectively addressing the obesity epidemic requires a concerted effort involving policy changes and strategic investments. Government policies can play a crucial role in shaping environments that promote healthier choices. This can include initiatives like promoting access to nutritious food in underserved communities, implementing taxes on unhealthy food products, subsidizing healthier alternatives, investing in safe and accessible recreational spaces, and regulating the marketing of unhealthy foods to children.
Furthermore, increased investment in research to understand the complex causes of obesity and develop more effective prevention and treatment strategies is vital. Public-private partnerships can leverage resources and expertise to create innovative solutions. Ultimately, combating the obesity epidemic is a long-term endeavor that requires sustained commitment and a willingness to invest in the health and economic future of the nation. The financial implications are significant, but the costs of inaction are far greater.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.
