In the realm of human biology, the liver is often described as the “central processing unit” of the body. Just as a high-performance server manages data, filters traffic, and ensures the stability of an entire network, the liver performs over 500 vital functions, ranging from detoxification to protein synthesis. However, when we ask what organ Hepatitis B affects, the answer is singular and critical: the liver. In the modern era, the battle against this viral infection is no longer fought solely with traditional medicine. It is being waged with high-level technology, data science, and computational biology.
The intersection of technology and hepatology (the study of the liver) has created a new frontier where software and hardware are used to diagnose, monitor, and potentially cure a disease that affects millions worldwide. By treating the liver as a complex biological system that requires advanced “system maintenance,” the tech industry is providing the tools necessary to mitigate the damage caused by Hepatitis B and move toward an era of personalized, tech-driven healthcare.
The Core of the Problem: Why the Liver is the “Mainframe” of the Human Body
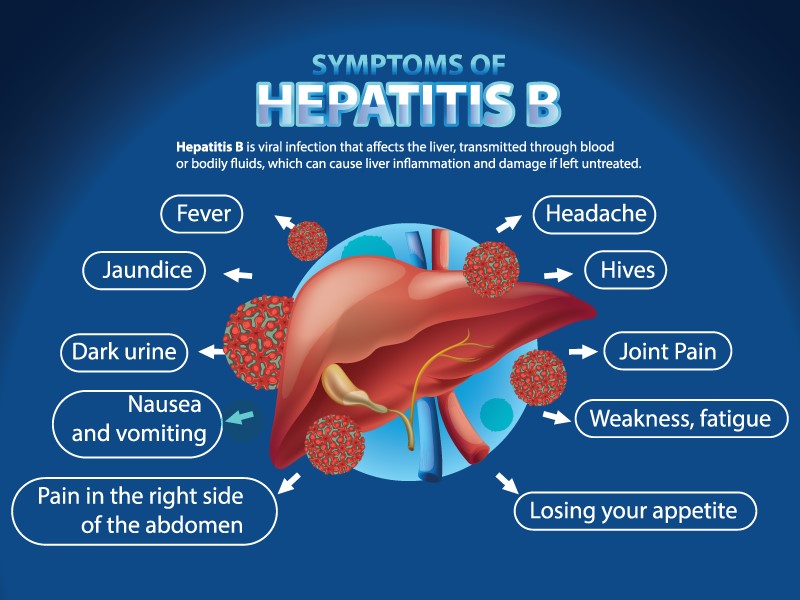
To understand how technology interacts with Hepatitis B, one must first view the liver through a technical lens. The liver is the body’s primary filtration system. It processes nutrients, metabolizes drugs, and neutralizes toxins. When Hepatitis B enters the system, it targets the hepatocytes—the functional cells of the liver—effectively “hacking” the cellular machinery to replicate its own viral DNA.
The Biological Processor: Understanding Systemic Load
The liver manages the body’s metabolic load much like a data center manages bandwidth. When Hepatitis B causes inflammation (hepatitis), it creates “latency” in the system. The liver’s ability to process toxins slows down, leading to a buildup of waste products. Technology-driven diagnostic tools now allow us to measure this metabolic load with unprecedented precision, treating the liver not just as a piece of tissue, but as a dynamic processor whose efficiency can be quantified through digital biomarkers.
Viral Integration: The Software Patch of the Virus
Hepatitis B is particularly insidious because it can integrate its DNA into the host’s genome. In tech terms, this is equivalent to a rootkit—a type of malicious software that embeds itself deep within the operating system, making it nearly impossible to remove with standard anti-virus software. Modern biotechnology is currently developing “patch” technologies, such as CRISPR-Cas9, to identify these viral sequences and “delete” them from the cellular code, a feat that requires massive computational power and sophisticated genetic mapping software.
Computational Diagnostics: Using AI to Visualize Viral Impact
Historically, determining the extent of liver damage from Hepatitis B required invasive procedures like biopsies. Today, the tech sector has introduced non-invasive alternatives that rely on complex algorithms and advanced imaging hardware.
AI-Enhanced Imaging and Computer Vision
Artificial Intelligence (AI) has revolutionized how we “see” the liver. Through Computer Vision and Convolutional Neural Networks (CNNs), software can now analyze ultrasound, CT, and MRI scans with higher accuracy than the human eye. These AI models are trained on millions of images to identify early signs of fibrosis (scarring) or cirrhosis caused by chronic Hepatitis B. By identifying these patterns early, the technology allows for “predictive maintenance” of the organ, preventing total system failure.
Transient Elastography and IoT Sensors
One of the most significant tech breakthroughs in hepatology is transient elastography (often known by the brand name FibroScan). This technology uses low-frequency elastic waves to measure liver stiffness. The data is processed in real-time by proprietary software, providing a “health score” that mirrors how a systems administrator might check the health of a hard drive. Furthermore, integrated IoT (Internet of Things) sensors in high-end medical devices now allow this data to be uploaded directly to the cloud, enabling doctors to monitor liver health remotely and adjust treatment protocols based on live data feeds.
The Data of Disease: Bioinformatics and the Genomic Mapping of Hepatitis B
The fight against Hepatitis B is increasingly a “big data” problem. The virus exists in multiple genotypes, each responding differently to various treatments. Bioinformatics—the application of computer science to biological data—is the key to unlocking personalized treatment plans.
Genomic Sequencing and Cloud Computing
To understand how Hepatitis B affects a specific individual’s liver, researchers utilize Next-Generation Sequencing (NGS). This process generates terabytes of data regarding the viral genome and the patient’s immune response. Processing this information requires massive computational resources, often utilizing cloud-based platforms like AWS or Google Cloud’s Life Sciences tools. By analyzing this data, bioinformaticians can identify specific mutations that might lead to drug resistance, allowing for a more agile and responsive treatment strategy.
Predictive Analytics in Population Health
On a macro level, tech companies are using predictive analytics to track the spread of Hepatitis B and its long-term effects on global health. By aggregating anonymized data from electronic health records (EHRs), machine learning models can predict which populations are at the highest risk for developing liver cancer (hepatocellular carcinoma) as a result of chronic infection. This “data-first” approach allows healthcare systems to allocate resources more efficiently, much like how a Content Delivery Network (CDN) optimizes traffic flow to prevent server crashes.
Future-Proofing Bio-Tech: Nanotechnology and the Elimination of Viral Reservoirs
The ultimate goal of the technology sector in this space is the “functional cure”—a state where the virus is no longer detectable and the liver can regenerate. This requires moving beyond traditional pills and into the realm of nanotechnology and smart drug delivery.
Nanorobotics and Targeted Delivery
One of the biggest challenges in treating the liver is ensuring that medication reaches the hepatocytes without affecting other organs. Engineers are developing “smart” nanoparticles that act as targeted delivery vehicles. These nanoparticles are programmed to recognize the surface proteins of liver cells. Once they “dock” with the target cell, they release their therapeutic payload. This is the biological equivalent of a targeted software update, ensuring that only the affected “files” are modified while the rest of the system remains untouched.
Digital Twins: Modeling the Liver in Virtual Space
The concept of a “Digital Twin”—a virtual model of a physical asset—is commonly used in aerospace and manufacturing. Now, it is being applied to the liver. By creating a digital twin of a patient’s liver, researchers can simulate how the organ will react to different Hepatitis B medications before a single dose is administered. These simulations take into account blood flow, viral load, and genetic predispositions, allowing for a “sandbox” environment where treatments can be tested for safety and efficacy.
Wearables and Telehealth: Managing Chronic Viral Impact Digitally
For those living with chronic Hepatitis B, the “user experience” of healthcare is being transformed by mobile apps and wearable technology. Managing a chronic condition is a long-term project, and tech is providing the management tools to ensure success.
Real-Time Monitoring and Adherence Apps
Patient adherence to antiviral medication is critical to preventing liver damage. New mobile platforms are designed to gamify and track medication schedules, providing “push notifications” for health. Some advanced systems even use ingestible sensors—tiny, biocompatible chips—that send a signal to a smartphone app once the medication has been digested, ensuring 100% data accuracy in treatment logs.
The Rise of Specialized Tele-Hepatology
For patients in remote areas, accessing a liver specialist can be difficult. Telehealth platforms integrated with diagnostic software allow patients to share their “liver data” (from blood tests and scans) with specialists thousands of miles away. This democratization of tech ensures that the organ affected by Hepatitis B receives expert care regardless of geography. High-speed 5G networks and secure, encrypted communication channels ensure that sensitive medical data is transmitted without latency or security breaches.

Conclusion: The Synthesis of Silicon and Biology
When we address the question of what organ Hepatitis B affects, we are talking about the very core of human life support. The liver’s complexity demands more than just biological intervention; it requires the precision, scalability, and analytical power of modern technology.
From the use of AI in early diagnosis to the application of big data in genomic sequencing, the tech industry has become an indispensable ally in the fight against Hepatitis B. As we move forward, the line between “medical technology” and “information technology” will continue to blur. By applying the principles of system architecture, data integrity, and predictive modeling to the human liver, we are not just treating a disease—we are optimizing the most important “hardware” we will ever own. The future of hepatology is digital, and through these innovations, the goal of a world free from the damage of Hepatitis B is becoming a technical reality.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.