In the traditional landscape of healthcare, the physical assessment is a tactile, almost rhythmic ritual. Among the “big four” techniques—inspection, palpation, percussion, and auscultation—percussion has long been considered one of the most difficult skills for a nurse to master. It involves tapping on a surface to determine the density of the underlying tissue, translating sound into a map of the human body. However, as we move deeper into the decade of digital transformation, the question “what is percussion in nursing” is no longer answered solely by manual dexterity. Today, it is being redefined by high-fidelity simulations, artificial intelligence, and haptic technology.
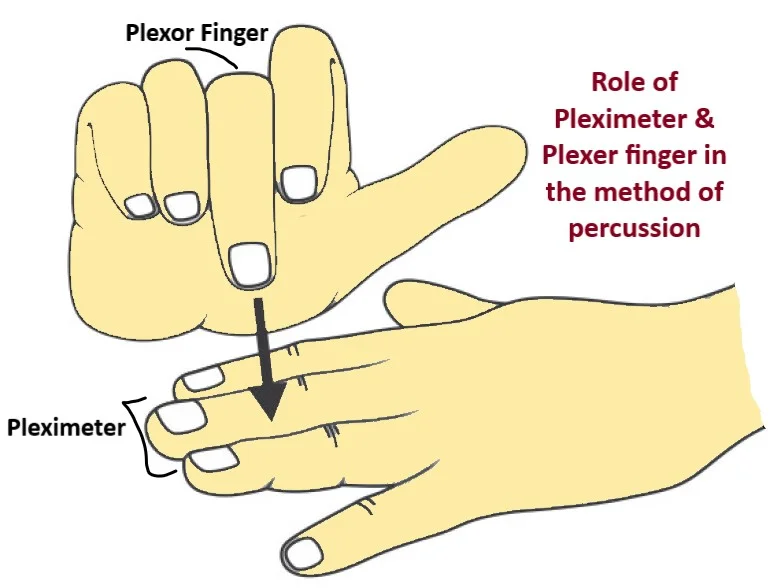
The integration of technology into clinical assessment is not merely a convenience; it is a response to the need for greater diagnostic precision and the rise of telehealth. By digitizing the nuances of percussion, the nursing field is bridging the gap between centuries-old physical techniques and the cutting edge of data science.
Bridging Tradition and Innovation: The Tech-Driven Core of Percussion
To understand how technology is reshaping this field, we must first look at the mechanical foundation of the skill. In a manual setting, a nurse uses their fingers to strike the body, listening for sounds like resonance (hollow), dullness (solid), or tympany (drum-like). In the modern tech-centric environment, these acoustic properties are being converted into digital data points.
From Manual Skill to Digital Data Point
The traditional method of percussion relies heavily on the subjective hearing of the practitioner. Technology is changing this by introducing acoustic sensors that can capture the frequency and amplitude of the sounds produced during a percussion exam. By converting these sounds into visual waveforms, software allows nurses to see what they are hearing. This “visual percussion” reduces the margin of error, particularly in loud clinical environments where subtle changes in sound might be missed by the human ear.
The Role of Haptic Feedback Devices
One of the greatest challenges in nursing education has been the inability to “feel” what a veteran nurse feels. New haptic feedback devices are solving this. These gadgets simulate the resistance and vibration of different tissue types—such as a fluid-filled lung versus a healthy, air-filled one. For a nursing student, this means using a digital stylus or a glove that provides tactile resistance, allowing them to practice the “tap” of percussion in a controlled, tech-enabled environment before ever touching a patient.
EdTech and the Virtualization of Physical Assessment
The most significant tech shift regarding percussion in nursing is occurring within the realm of Education Technology (EdTech). As nursing schools grapple with limited clinical placements, Virtual Reality (VR) and Augmented Reality (AR) have stepped in to provide a digital sandbox for clinical skills.
VR Simulations: Mastering Resonance Without a Patient
In a VR environment, a nurse can “perform” percussion on a 3D patient model. Using motion-tracked controllers, the software detects the force and location of the nurse’s strike. If the nurse taps over a virtual liver, the software generates a precise “dull” sound; if they move to the lungs, it shifts to “resonance.” This immediate, software-driven feedback loop accelerates the learning curve. Furthermore, these programs can simulate rare pathologies—such as a tension pneumothorax—that a student might not encounter in years of traditional clinical rotations.
High-Fidelity Manikins and IoT Integration
Modern simulation labs utilize high-fidelity manikins that are essentially large-scale Internet of Things (IoT) devices. These manikins are programmed via a central interface to alter their internal acoustic properties. A clinical instructor can, with a click of a button, change a manikin’s “chest” from resonant to dull to simulate pleural effusion. This allows for a standardized testing environment where technology ensures that every student is evaluated on their ability to recognize specific, digitally-replicated sounds.
Smart Diagnostics: Enhancing Percussion with AI and Sensors
As we look toward the future of bedside care, the fusion of percussion and Artificial Intelligence (AI) is creating a new category of “Smart Diagnostics.” These tools don’t replace the nurse; they augment the nurse’s natural senses with machine-learning capabilities.
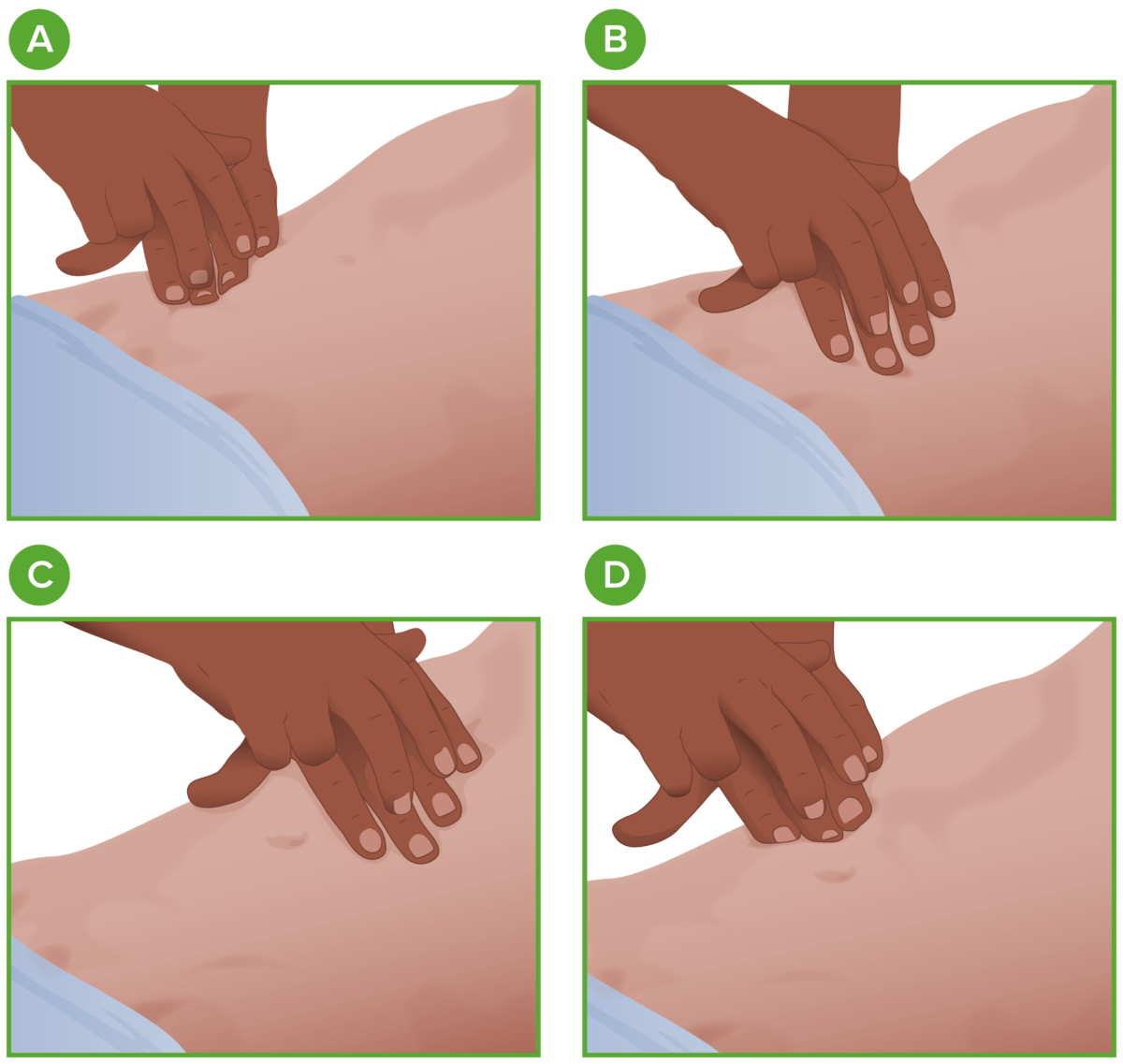
AI-Driven Analysis of Sound Frequencies
AI algorithms are now capable of analyzing sound files recorded during a percussion exam. While a human ear might struggle to distinguish between “flatness” and “dullness” in a complex case, an AI tool can compare the sound frequency against a database of thousands of clinical recordings. This software can provide a “probability score,” suggesting, for example, a 92% likelihood that the percussed area indicates localized fluid. This level of decision support is a game-changer for early intervention.
The Advent of Digital Percussors
Much like the digital stethoscope changed auscultation, the development of digital percussors is on the horizon. These handheld gadgets use ultrasonic or mechanical pulses to “strike” the tissue and sensors to record the return vibratory wave. This eliminates the physical strain on the nurse’s hands—a common issue leading to repetitive strain injuries—while providing a standardized output that can be directly uploaded to the patient’s Electronic Health Record (EHR).
Telehealth and Remote Monitoring: Percussion in the Cloud
One of the most ambitious frontiers for nursing tech is the application of physical assessment in remote settings. As healthcare shifts toward the home, the “what” and “how” of percussion are adapting to the cloud.
Wearable Tech and Continuous Thoracic Monitoring
The logic of percussion—detecting changes in density—is being baked into wearable technology. Smart vests equipped with bio-impedance sensors can monitor changes in lung density (fluid buildup) in heart failure patients. While this isn’t “tapping” in the literal sense, it is the technological evolution of percussion’s core objective: monitoring tissue density changes over time. These devices send alerts to a nurse’s dashboard, allowing for “proactive percussion” without the nurse needing to be in the room.
Bridging the Gap in Rural Nursing through Digital Assessment
In rural or underserved areas, specialized nursing knowledge is often a distance away. Tele-nursing platforms now include peripheral attachments that allow a local nurse or even a trained caregiver to perform a physical assessment while a specialist views the data in real-time. By using a digital sensor to perform percussion, the acoustic data is streamed via high-speed internet to a remote diagnostician, ensuring that the “sound” of the patient’s health is not lost across the miles.
Cybersecurity and Data Ethics in Digital Nursing Assessment
As percussion moves from a physical act to a digital one, it enters the complex world of digital security. When a nurse uses a tech tool to perform an assessment, that data becomes a part of the patient’s digital footprint, necessitating rigorous security protocols.
Protecting Patient Auditory Data
If a nurse uses an AI-powered app to record and analyze percussion sounds, that audio file is protected health information (PHI). Software developers in the nursing space are now prioritizing end-to-end encryption for auditory data. The challenge lies in ensuring that these files are high-quality enough for analysis but compressed enough for storage, all while remaining encrypted against potential breaches.
Standardizing Digital Health Records for Physical Findings
A major hurdle in nursing tech is interoperability. For the “digital percussion” data to be useful, it must be standardized so that it can be read by different EHR systems. Tech innovators are working on creating a universal nomenclature for digital physical assessment findings. Instead of a nurse typing “dullness noted in the left lower lobe,” the system might auto-populate a data field with a specific frequency range and an attached audio-visual clip, creating a more objective and permanent record of the patient’s physical state.

The Future: Will Technology Replace the “Human Touch”?
The evolution of “what is percussion in nursing” through a technological lens often raises the question of whether the human element will be lost. The consensus among nursing tech leaders is that these tools are meant to enhance, not replace. By automating the more subjective aspects of percussion and providing high-tech training tools, technology allows nurses to spend less time guessing and more time acting on accurate data.
The future of nursing percussion lies in a “cyborg” approach—the nurse’s clinical intuition and empathy combined with the precision of AI and the reach of digital sensors. As we continue to develop software that can hear what we cannot and VR that allows us to practice a thousand times before a single patient interaction, the art of nursing moves into a more scientific, data-driven, and safer era. Percussion, once a simple tap, is becoming a sophisticated symphony of digital insights.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.