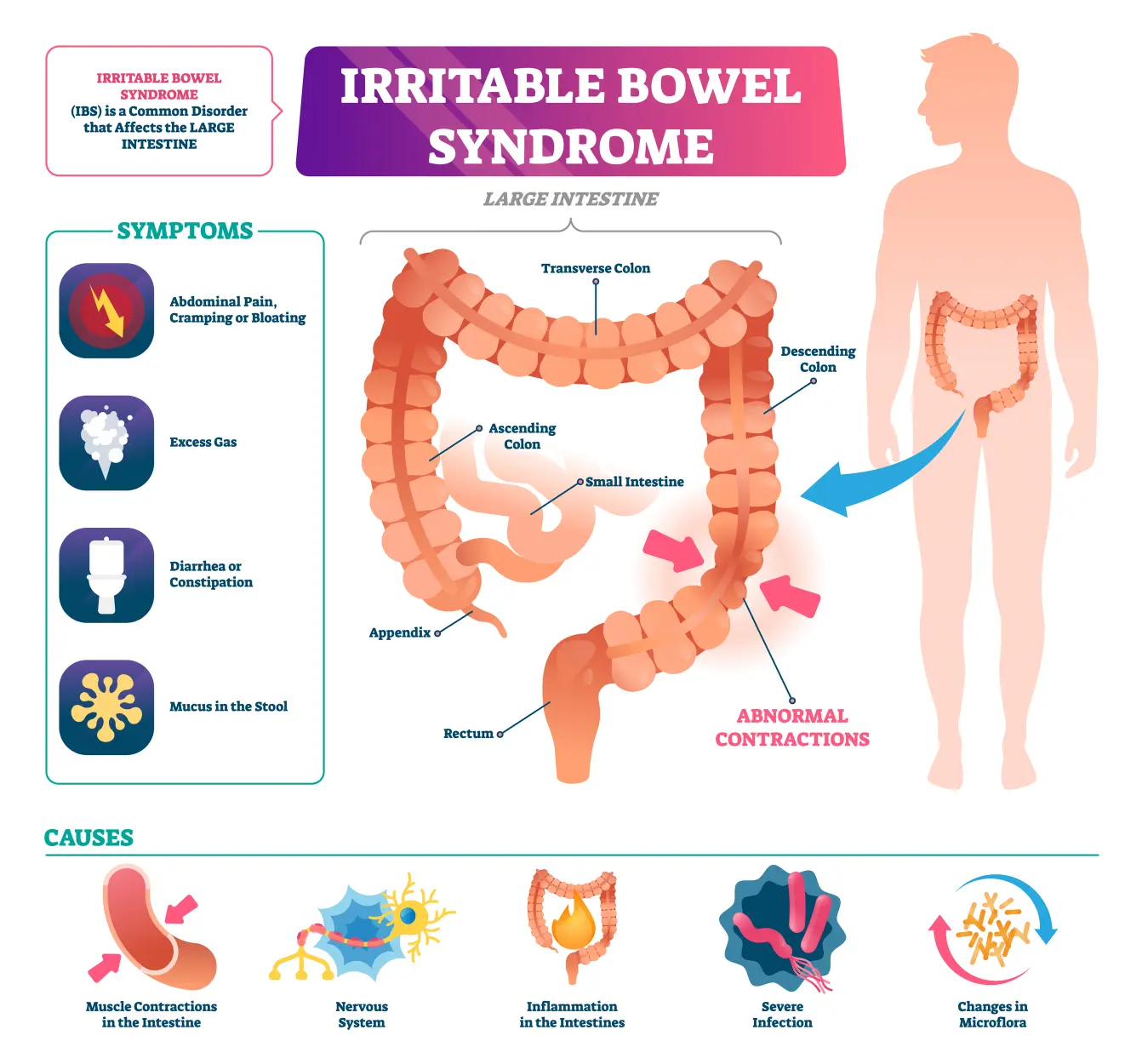
Irritable Bowel Syndrome (IBS) is a common, chronic gastrointestinal disorder that affects the large intestine. While not life-threatening, it can significantly impact an individual’s quality of life, causing discomfort, pain, and a range of disruptive symptoms. Understanding IBS is the first step towards managing it effectively and regaining control over your well-being. This article will delve into what IBS is, its potential causes, common symptoms, and crucially, how technology, strategic approaches, and even financial considerations can play a role in navigating this condition.
Unpacking the Gut: Understanding the Fundamentals of IBS
At its core, IBS is a functional gastrointestinal disorder. This means that while the intestines may appear normal during medical examinations (like endoscopies or colonoscopies), they are not functioning as they should. The communication between the brain and the gut, known as the gut-brain axis, appears to be disrupted in individuals with IBS. This miscommunication can lead to a variety of issues, including:
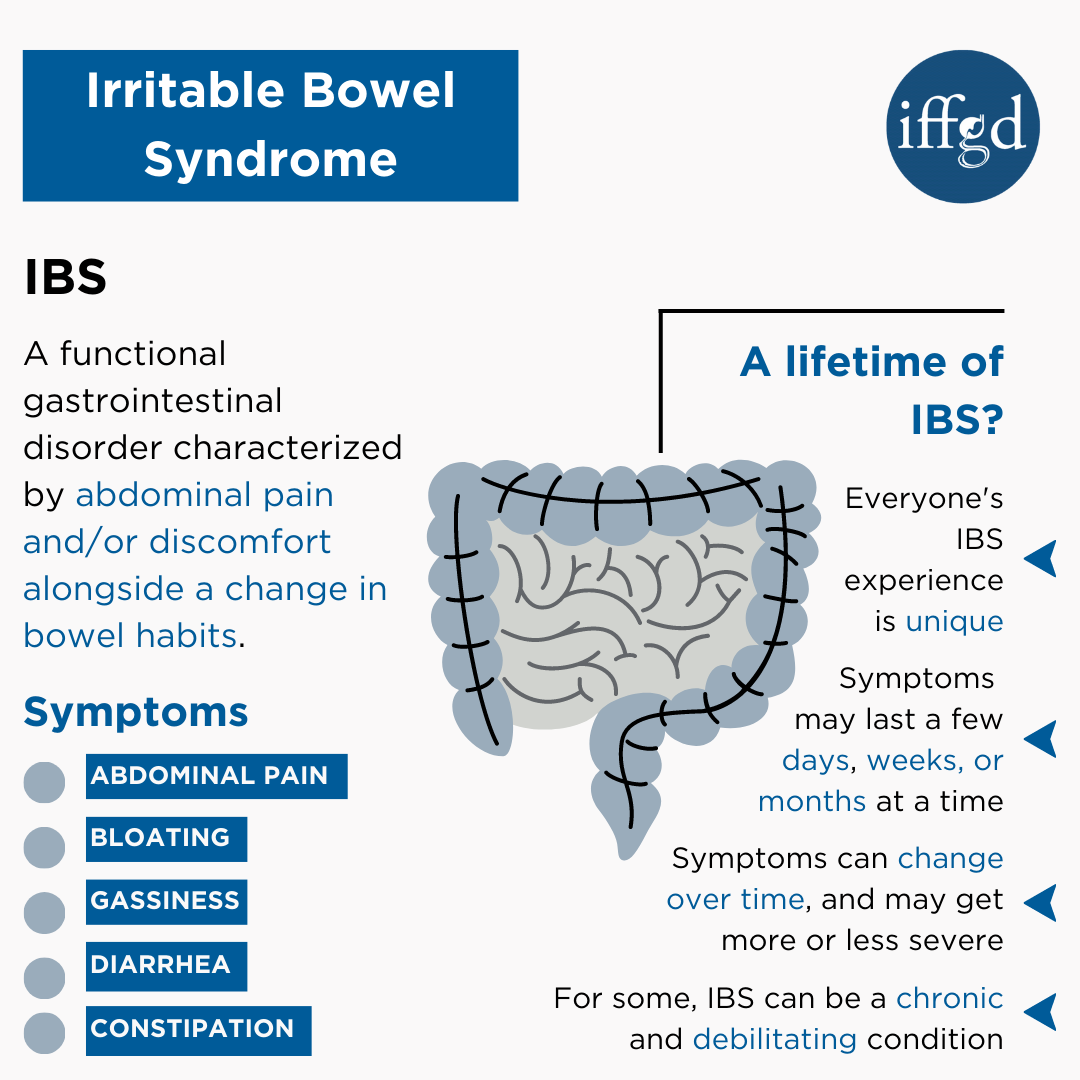
- Altered Gut Motility: The muscles in the intestinal walls contract and relax to move food through the digestive tract. In IBS, these contractions can be too strong or too weak, leading to either diarrhea (rapid transit) or constipation (slow transit), or a combination of both.
- Increased Gut Sensitivity: People with IBS often experience heightened sensitivity to stimuli in the gut. This means that normal amounts of gas or food can trigger pain and discomfort that wouldn’t affect someone without IBS.
- Changes in Gut Microbiome: The balance of bacteria and other microorganisms in the gut (the microbiome) is thought to play a role in IBS. Imbalances or dysbiosis can contribute to inflammation, gas production, and altered bowel habits.
- Visceral Hypersensitivity: This is a key characteristic of IBS, referring to an increased perception of pain and discomfort from the intestines. It’s as if the “volume knob” for pain signals from the gut is turned up too high.
It’s important to distinguish IBS from more serious conditions like Inflammatory Bowel Disease (IBD), which includes Crohn’s disease and ulcerative colitis. IBD involves visible inflammation and damage to the intestinal lining, whereas IBS does not. However, the symptoms can overlap, making accurate diagnosis crucial.
Defining the Spectrum: Types of IBS
IBS is typically categorized into four subtypes based on the predominant bowel habit:
- IBS with constipation (IBS-C): Characterized by infrequent bowel movements and hard, lumpy stools.
- IBS with diarrhea (IBS-D): Characterized by frequent bowel movements and loose, watery stools.
- Mixed IBS (IBS-M): Individuals with IBS-M experience alternating periods of constipation and diarrhea.
- Unspecified IBS (IBS-U): This category is used when symptoms don’t fit neatly into the other three subtypes, but the individual still meets the diagnostic criteria for IBS.
The diagnostic criteria for IBS, known as the Rome IV criteria, typically involve recurrent abdominal pain occurring on average at least one day a week in the last three months, associated with two or more of the following: related to defecation, associated with a change in frequency of stool, and associated with a change in form (appearance) of stool.
Navigating the Digital Frontier: Tech Solutions for IBS Management
In today’s digitally-driven world, technology offers a powerful suite of tools to help individuals manage IBS. From sophisticated diagnostic aids to everyday productivity apps, tech can empower patients to gain insights, track their progress, and communicate more effectively with their healthcare providers.
Smart Tracking and Data-Driven Insights
The cornerstone of effective IBS management often lies in understanding personal triggers and patterns. This is where technology excels.
Symptom and Food Trackers:
Modern apps have transformed the humble diary into a sophisticated data analysis tool. These applications allow users to log their symptoms (pain levels, bowel movements, bloating, fatigue), food intake, hydration, exercise, stress levels, and even sleep patterns.
- AI-Powered Analysis: Many advanced apps leverage Artificial Intelligence (AI) to identify correlations between food intake and symptom flare-ups. By analyzing the logged data, these AI tools can suggest potential trigger foods, helping individuals make informed dietary choices. This moves beyond generic advice to personalized recommendations based on an individual’s unique biological response.
- Personalized Insights: Beyond just identifying trigger foods, these apps can offer insights into how other lifestyle factors, like stress or lack of sleep, might be exacerbating IBS symptoms. This holistic approach is vital for comprehensive management.
- Data Visualization: User-friendly dashboards and graphs provide a clear visual representation of trends over time. This makes it easier to understand the impact of dietary changes, medication, or lifestyle adjustments on symptom severity.
Wearable Technology and Biometrics:
While not as directly focused on IBS as symptom trackers, wearable devices can contribute indirectly by monitoring overall health markers that influence gut health.
- Stress Monitoring: Many smartwatches and fitness trackers can monitor heart rate variability, which is a key indicator of stress. Elevated stress is a well-known IBS trigger, so understanding and managing stress levels through this data can be beneficial.
- Sleep Tracking: Poor sleep quality can negatively impact gut health and exacerbate IBS symptoms. Wearables provide data on sleep duration, depth, and disruptions, allowing individuals to identify areas for improvement.
- Activity Tracking: Regular physical activity can aid digestion and reduce stress. Tracking steps and activity levels can encourage a consistent exercise routine.
Telehealth and Remote Monitoring:
The rise of telehealth has revolutionized healthcare access, and it’s particularly valuable for individuals with chronic conditions like IBS.
- Virtual Consultations: Patients can have consultations with gastroenterologists or dietitians from the comfort of their homes, saving travel time and reducing the stress of hospital visits. This is especially beneficial for those whose symptoms make travel difficult.
- Remote Monitoring of Treatment Efficacy: In some cases, healthcare providers can remotely monitor patient progress through connected devices or data shared from symptom-tracking apps, allowing for timely adjustments to treatment plans.
- Digital Therapeutics: Emerging digital therapeutics (DTx) are showing promise in IBS management. These are software-based interventions designed to prevent, manage, or treat medical conditions. For IBS, some DTx are designed to provide cognitive behavioral therapy (CBT) or other psychological support tailored to gut health, addressing the gut-brain axis component.
Digital Security and Privacy:

Given the sensitive nature of health data, digital security is paramount. Individuals using health apps and platforms must be aware of privacy policies and choose reputable services that prioritize data protection. Strong passwords, two-factor authentication, and being cautious about sharing data with third parties are essential practices.
Building Your Brand of Well-being: Strategic Approaches to Living with IBS
Managing IBS is not just about symptom relief; it’s about building a resilient personal brand centered on well-being. This involves a strategic approach to self-care, effective communication, and a proactive mindset.
The Power of Personal Branding in Health Management
While “personal branding” is often associated with career advancement, its principles can be powerfully applied to managing a chronic condition like IBS.
- Defining Your “Brand” as a Healthy Individual: Your “brand” in this context is the image you project of yourself as someone managing IBS effectively. This involves understanding your condition, being proactive about your health, and communicating your needs clearly.
- Crafting Your Narrative: How you talk about your IBS is crucial. Instead of framing it as an insurmountable burden, frame it as a challenge you are actively navigating. This positive self-talk can influence your mindset and empower you. For instance, instead of saying “I can’t go out because of my IBS,” you might say, “I need to plan my outing carefully to accommodate my IBS.”
- Consistency in Self-Care: Just as a brand maintains consistency in its messaging and offerings, your self-care practices should be consistent. This means sticking to your treatment plan, dietary recommendations, and stress-management techniques even on days when you feel better.
Strategic Lifestyle Design:
Designing your lifestyle to minimize IBS triggers and maximize your ability to cope is a strategic imperative.
- Dietary Strategies and Personalization: This is a cornerstone of IBS management. While there’s no one-size-fits-all diet, many individuals find relief through approaches like:
- Low-FODMAP Diet: This diet restricts fermentable oligosaccharides, disaccharides, monosaccharides, and polyols, which can be poorly absorbed and cause gas and bloating. It’s often implemented under the guidance of a registered dietitian and involves an elimination and reintroduction phase to identify specific triggers.
- Mindful Eating: Paying attention to how you eat – chewing slowly, avoiding distractions, and eating in a relaxed environment – can significantly improve digestion.
- Regular Meal Times: Irregular eating patterns can disrupt gut function. Establishing consistent meal times can help regulate bowel habits.
- Stress Management Techniques: Given the strong gut-brain connection, managing stress is paramount. This can involve:
- Mindfulness and Meditation: Regular practice can calm the nervous system and reduce symptom severity.
- Yoga and Tai Chi: These gentle exercises combine physical movement with breathwork and mindfulness.
- Deep Breathing Exercises: Simple yet effective for immediate stress relief.
- Cognitive Behavioral Therapy (CBT): CBT can help individuals identify and change negative thought patterns and behaviors that contribute to their IBS symptoms.
- Building a Support Network: Connecting with others who understand IBS can be incredibly validating and provide practical advice. This can include online forums, support groups, or simply sharing with trusted friends and family.
Effective Communication and Advocacy:
- Communicating with Healthcare Providers: Be prepared for appointments by tracking your symptoms and having a clear list of questions. Don’t hesitate to advocate for yourself and seek second opinions if you feel your concerns are not being adequately addressed.
- Setting Boundaries with Others: Learn to communicate your needs to friends, family, and colleagues. This might involve explaining why you need to leave an event early, why you can’t eat certain foods, or why you might need a quiet moment. This isn’t about being difficult; it’s about managing your health and ensuring you can participate in life to the fullest.
- Corporate Identity and Workplace Accommodations: For those in the workforce, understanding how your IBS might impact your job and exploring potential accommodations is important. This could involve discussing flexible working hours, access to restrooms, or stress-reducing break options with your employer.
The Financial Landscape of IBS Management
Living with a chronic condition like IBS can also have financial implications. From healthcare costs to dietary adjustments and potential impacts on earning capacity, understanding these financial aspects is crucial for long-term stability.
Financial Planning for Chronic Health Conditions
Managing IBS effectively often involves ongoing costs. Proactive financial planning can help alleviate some of this burden.
Healthcare Costs and Insurance:
- Understanding Your Insurance Coverage: Thoroughly understanding your health insurance plan is essential. This includes co-pays for doctor’s visits, specialist consultations, prescription medications, and diagnostic tests.
- Maximizing Benefits: Explore whether your insurance covers specific treatments like dietary counseling, mindfulness programs, or even certain alternative therapies that you find beneficial.
- Prescription Savings: For prescribed medications, investigate options like generic alternatives, patient assistance programs offered by pharmaceutical companies, or prescription discount cards.
Dietary Expenses and Smart Shopping:
- Cost of Specialized Diets: Some IBS-friendly diets, like the Low-FODMAP diet, can initially involve purchasing specific gluten-free, dairy-free, or low-FODMAP certified products, which can be more expensive.
- Strategic Meal Planning and Preparation: Planning meals in advance, buying in bulk when possible, and cooking from scratch can help control food costs. Focusing on whole, unprocessed foods that are naturally IBS-friendly can also be more economical than relying heavily on pre-packaged specialty items.
- Reducing Food Waste: Effective grocery shopping and storage can minimize waste, saving money in the long run.
Impact on Income and Side Hustles:
- Productivity and Work Capacity: While IBS doesn’t necessarily prevent someone from working, symptom flare-ups can lead to missed workdays, reduced productivity, or the need for flexible work arrangements. This can potentially impact income.
- Exploring Side Hustles and Online Income Streams: For individuals seeking greater flexibility or additional income, exploring online income streams and side hustles can be beneficial. This could involve:
- Freelancing in areas of expertise: Leveraging existing skills in writing, design, programming, or consulting.
- Online Tutoring: Sharing knowledge in academic subjects or specialized skills.
- Creating and Selling Digital Products: E-books, courses, or templates related to health management or other interests.
- Affiliate Marketing: Recommending products or services and earning a commission.
It’s important to choose side hustles that are flexible and can be managed around symptom fluctuations, ensuring they don’t become another source of stress.
Financial Tools and Resources:
- Budgeting Apps: Utilize personal finance apps to track income and expenses, identify areas where money can be saved, and allocate funds for healthcare and dietary needs.
- Emergency Funds: Building an emergency fund can provide a financial safety net for unexpected medical expenses or periods of reduced work capacity.
- Seeking Financial Advice: If managing the financial aspects of chronic illness feels overwhelming, consulting with a financial advisor specializing in personal finance or chronic illness can provide valuable guidance.
In conclusion, while Irritable Bowel Syndrome presents significant challenges, a multi-faceted approach that embraces technological advancements, strategic self-management, and proactive financial planning can empower individuals to live fuller, more comfortable lives. By understanding the condition, leveraging available tools, and building a strong personal foundation of well-being, the impact of IBS can be effectively navigated.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.