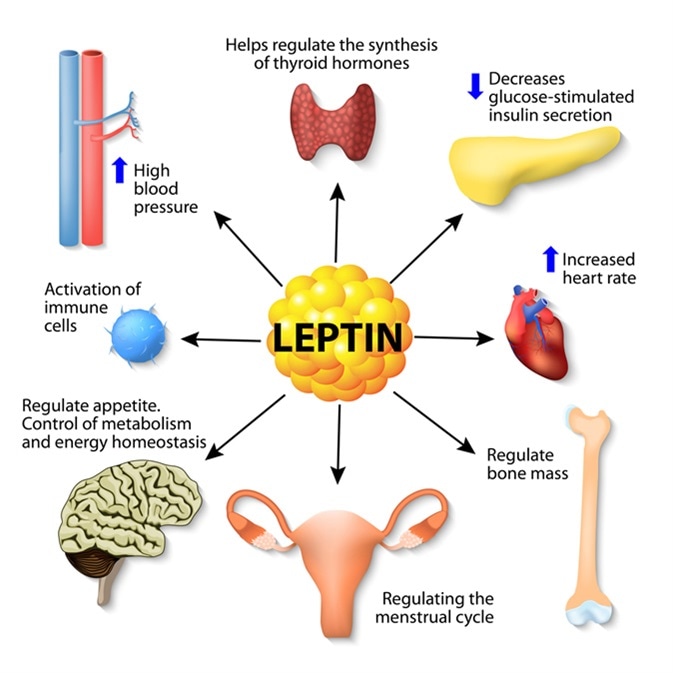
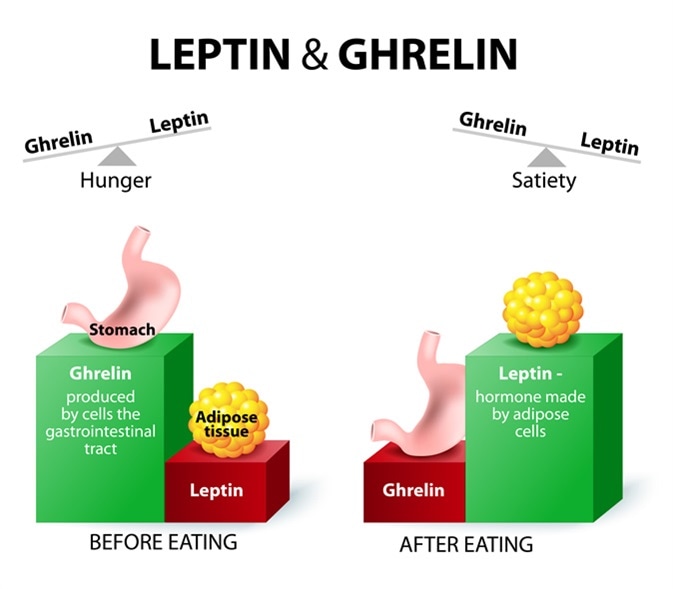
The hormone leptin, often dubbed the “satiety hormone,” plays a pivotal role in regulating appetite, metabolism, and energy balance. Produced primarily by adipose (fat) cells, leptin signals to the brain, specifically the hypothalamus, to inform it about the body’s energy reserves. When leptin levels are high, indicating ample fat stores, the brain is signaled to suppress appetite and increase energy expenditure. Conversely, low leptin levels signal hunger and a reduction in energy consumption. This delicate biochemical dance is fundamental to maintaining a healthy weight and preventing metabolic disorders. However, the complexity of leptin’s actions, particularly in conditions like obesity where “leptin resistance” can occur, has necessitated increasingly sophisticated technological approaches to unravel its mysteries and harness its therapeutic potential. From advanced diagnostic techniques to AI-driven research and personalized digital health interventions, technology is redefining our understanding and management of this crucial hormone.
The Biological Imperative of Leptin and Early Technological Insights
Before diving into the bleeding edge of technology, it’s essential to grasp the foundational biology of leptin and how initial scientific investigations laid the groundwork for future innovation. Leptin’s discovery in 1994 was a landmark event, shifting paradigms in obesity research from a simplistic view of willpower to a more nuanced understanding of hormonal regulation.
Leptin’s Core Role in Energy Homeostasis
At its heart, leptin is an adipokine, a signaling molecule secreted by fat cells, designed to communicate the state of energy stores to the central nervous system. Its primary function is to prevent both starvation and excessive weight gain by finely tuning hunger, satiety, and metabolic rate. In a healthy system, leptin acts as a critical feedback loop: more fat equals more leptin, leading to reduced food intake and increased energy burn; less fat equals less leptin, stimulating appetite and conserving energy. Disruptions in this pathway, whether due to genetic mutations affecting leptin production or receptor function, or the more common phenomenon of leptin resistance where the brain fails to respond adequately to high leptin levels, can lead to severe metabolic imbalances, including morbid obesity. Understanding this biological imperative is the starting point for any technological intervention.
Initial Discoveries and Lab-Based Diagnostics
The initial identification of leptin was a triumph of molecular biology, relying on advanced genetic sequencing and animal models. Scientists used techniques like positional cloning to pinpoint the ob gene in mice, which, when mutated, led to profound obesity. This discovery opened the floodgates for developing assays to measure leptin levels in human blood. Early diagnostic tools were largely enzyme-linked immunosorbent assays (ELISAs) and radioimmunoassays (RIAs)—benchtop laboratory technologies that, while revolutionary at the time, were labor-intensive, required specialized equipment, and provided only snapshots of leptin concentrations. These methods, still foundational in clinical research, represent the first wave of technology applied to understanding and diagnosing leptin-related conditions, providing the initial data sets upon which more advanced digital and AI-driven analyses could later build.
AI and Machine Learning: Revolutionizing Leptin Research
The advent of artificial intelligence (AI) and machine learning (ML) has dramatically accelerated our ability to process complex biological data, offering unprecedented insights into leptin’s multifaceted roles and potential therapeutic targets. These advanced computational tools are moving beyond simple correlations to predictive modeling and personalized strategies.
Predictive Modeling for Metabolic Health Outcomes
AI algorithms can sift through vast datasets comprising genetic information, metabolic profiles, dietary habits, and leptin levels from thousands of individuals. By identifying intricate patterns and relationships that are imperceptible to the human eye, AI can develop sophisticated predictive models. These models can forecast an individual’s risk of developing leptin resistance, type 2 diabetes, or obesity-related complications based on a confluence of biomarkers, including baseline leptin levels, genetic predispositions, and lifestyle factors. Such predictive capabilities allow for early risk stratification and proactive intervention strategies, moving healthcare from reactive treatment to preventive management. For instance, AI could predict which individuals are most likely to respond positively to leptin-sensitizing therapies, optimizing treatment efficacy.
Data Analysis for Personalized Interventions
The power of machine learning extends to personalizing health interventions. By analyzing an individual’s unique biological fingerprint—including their specific leptin dynamics, genetic variants, microbiome composition, and physiological responses to diet and exercise—AI can recommend tailored lifestyle modifications. This level of personalization far surpasses general dietary guidelines. For example, an ML model might suggest a particular macronutrient ratio or exercise regimen that is optimally designed to improve leptin sensitivity for a given individual, based on their metabolic responses observed through continuous monitoring. This data-driven precision medicine approach promises to revolutionize how metabolic disorders are managed.
Drug Discovery and Therapeutic Development
AI is also transforming the notoriously long and expensive process of drug discovery. In the context of leptin, AI can identify novel compounds that modulate leptin production, enhance leptin receptor sensitivity, or mimic leptin’s effects more effectively. By simulating molecular interactions and predicting the efficacy and potential side effects of drug candidates in silico, AI significantly narrows down the pool of promising molecules, reducing the need for extensive wet-lab experimentation. This acceleration in preclinical development holds immense promise for developing new treatments for obesity and metabolic syndrome, particularly for individuals suffering from severe leptin resistance.
Wearable Technology and Biosensors for Real-time Monitoring
The ability to monitor physiological parameters in real-time and non-invasively is a cornerstone of digital health, and this technological leap is gradually extending to hormonal assays, including leptin. Wearable technology and advanced biosensors are paving the way for a more dynamic understanding of leptin’s fluctuations.
Non-Invasive Leptin Measurement Innovations

While direct, real-time measurement of leptin through wearables is still largely in the research and development phase, significant strides are being made. Researchers are exploring various non-invasive methods, such as microfluidic patches that analyze interstitial fluid, smart tattoos embedded with biosensors, or even advanced optical sensors that could detect biomarkers in sweat or saliva. These innovations aim to move beyond traditional blood tests, offering continuous or on-demand measurements of leptin levels without the need for clinical visits. Such technologies would provide unprecedented insights into how leptin levels respond to meals, exercise, stress, and sleep patterns throughout the day, offering a much richer context than single-point blood samples.
Integrating Wearable Data for Holistic Health Views
The true power of emerging leptin-sensing technologies lies in their integration with other wearable data. Imagine a scenario where a smartwatch tracks sleep quality, heart rate variability, activity levels, and potentially even early indicators of metabolic stress, while a complementary biosensor continuously monitors leptin. AI algorithms could then synthesize these diverse data streams to create a holistic, real-time profile of an individual’s metabolic health. This integrated data could identify correlations between specific lifestyle choices (e.g., late-night eating, sedentary periods) and leptin dysregulation, providing actionable insights for immediate behavioral modification or clinical intervention.
Challenges and Future of Continuous Monitoring
Despite the exciting potential, significant challenges remain. Accuracy, reliability, and calibration of non-invasive sensors are paramount. The ability to distinguish leptin from other circulating molecules in complex biological fluids requires highly specific and sensitive detection mechanisms. Furthermore, ensuring data privacy and security for such intimate physiological data is a critical ethical and technological hurdle. However, the rapid advancement in materials science, nanotechnology, and microelectronics suggests that fully functional, highly accurate wearable leptin monitors could become a reality within the next decade, transforming personal health management.
Digital Health Platforms and Personalized Nutrition Strategies
The convergence of biological insights, AI, and continuous monitoring is culminating in sophisticated digital health platforms that empower individuals to take a proactive role in managing their metabolic health, with leptin at the core.
AI-Powered Dietary Recommendations and Behavioral Nudges
Digital health platforms, often delivered via mobile applications, are leveraging AI to provide highly personalized dietary and exercise recommendations. Unlike generic diet plans, these platforms analyze an individual’s unique metabolic profile, which increasingly incorporates data indicative of leptin sensitivity or resistance. For example, if continuous monitoring suggests a dip in leptin sensitivity after consuming certain types of foods, the platform can immediately recommend alternatives or portion adjustments. Beyond just recommendations, these platforms employ AI-driven behavioral nudges—personalized alerts, motivational messages, and habit-formation strategies—to help users adhere to their plans and cultivate healthier behaviors over the long term.
Telemedicine and Remote Management of Metabolic Conditions
Digital health has significantly expanded the reach of healthcare through telemedicine, enabling remote consultations and continuous care. For individuals struggling with obesity, diabetes, or other metabolic conditions, remote monitoring of factors influencing leptin levels (like weight, glucose, activity) coupled with virtual consultations with dietitians, endocrinologists, and health coaches, can offer consistent support and timely adjustments to treatment plans. This is particularly crucial for complex conditions where frequent monitoring and expert guidance are essential, transcending geographical barriers and improving access to specialized care.
The Ethical Imperatives of Data Privacy and AI Bias
As digital health platforms collect and process sensitive biological data, including those related to leptin, ethical considerations become paramount. Ensuring robust data privacy and security protocols is non-negotiable to protect personal health information from misuse. Furthermore, the algorithms powering these platforms must be developed and scrutinized for potential biases. If the training data for AI models disproportionately represents certain demographics, the resulting recommendations or predictions may not be equally effective or even safe for underrepresented groups, potentially exacerbating health disparities. Addressing these ethical imperatives is crucial for the responsible and equitable deployment of leptin-related digital health solutions.
The Future Horizon: Synthetic Biology, Gene Editing, and Leptin
Looking further into the future, biotechnological advancements in synthetic biology and gene editing hold revolutionary potential for addressing leptin-related disorders at their genetic roots.
CRISPR and Genetic Interventions for Leptin Resistance
CRISPR-Cas9 and other gene-editing technologies offer the unprecedented ability to precisely modify DNA sequences. For individuals with rare genetic mutations causing leptin deficiency (e.g., mutations in the LEP gene or LEPR gene), gene editing could theoretically correct the underlying genetic flaw, restoring normal leptin production or receptor function. While clinical applications are still in early stages and ethical considerations are complex, the promise for curing monogenic forms of obesity linked to leptin is profound. For the more common challenge of acquired leptin resistance, future research might explore gene-editing strategies to enhance the expression or sensitivity of leptin receptors in specific brain regions, effectively “rewiring” the brain’s response to leptin.
Bioprinting and Advanced Therapeutic Delivery Systems
Beyond gene editing, technologies like bioprinting and advanced drug delivery systems could revolutionize how leptin-based therapies are administered. Imagine bio-engineered pancreatic islets or fat cells, created through 3D bioprinting, designed to produce and secrete leptin in a highly regulated, physiological manner. This could offer a more natural and sustained delivery of the hormone compared to traditional injections. Similarly, smart drug delivery systems, perhaps implantable micro-devices, could release leptin or leptin-sensitizing compounds precisely when and where they are needed, responding to real-time physiological cues. These futuristic technologies promise to overcome many of the current limitations in leptin replacement therapy and could unlock new avenues for treating severe metabolic diseases.
In conclusion, while leptin itself is a fundamental biological molecule, our journey to understand, measure, and leverage its power is inextricably linked with technological innovation. From early laboratory diagnostics to advanced AI, real-time biosensors, personalized digital health platforms, and revolutionary gene-editing tools, technology is continually pushing the boundaries of what is possible, transforming our approach to metabolic health and offering new hope for individuals grappling with disorders of energy balance. The digital dimensions of leptin are not just an adjunct to its biology but are becoming integral to its future.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.