The intersection of medicine and technology has birthed some of the most significant advancements in human longevity, but few tools have undergone as radical a digital transformation as the electrocardiogram (ECG). Once a bulky machine confined to the sterile environments of hospitals and specialized clinics, the ECG has transitioned from a stationary clinical procedure into a ubiquitous piece of consumer hardware. In the modern tech landscape, an electrocardiogram is no longer just a medical test; it is a data-driven interface between the human heart and the digital world.
Understanding the technological architecture of the ECG is essential for anyone interested in the future of health-tech, wearable gadgets, and the Internet of Medical Things (IoMT). By examining the shift from analog signals to AI-driven diagnostics, we can see how this century-old concept is being reimagined for a hyper-connected era.
The Evolution of ECG Technology: From Clinical Towers to Personal Gadgets
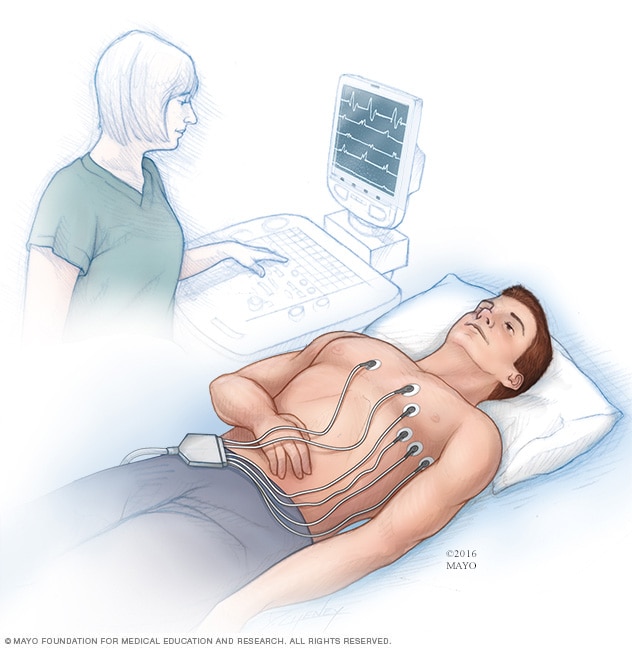
The fundamental principle of an electrocardiogram—recording the electrical activity of the heart over a period of time—has remained constant since its invention. However, the hardware used to capture these signals has undergone several “Moore’s Law” style iterations. In the early 20th century, the apparatus required a patient to submerge their limbs in buckets of salt water. Today, the same fidelity of data can be captured by a silicon chip smaller than a grain of rice.
The Shift to Micro-Sensors and MEMS
The primary driver behind the miniaturization of the ECG is the advancement of Micro-Electro-Mechanical Systems (MEMS). Modern tech companies have successfully integrated high-impedance biopotential amplifiers into ultra-small form factors. These sensors are designed to filter out “noise”—the electrical interference from muscle movements or external electronics—while amplifying the millivolt-level signals produced by the heart’s sinoatrial node. This technological leap allows for “dry electrode” technology, which replaces the sticky, conductive gels used in hospitals with the stainless steel or titanium surfaces found on the back of a smartwatch.
Digital Signal Processing in Cardiac Monitoring
Capturing an electrical signal is only half the battle; the real tech-heavy lifting occurs during Digital Signal Processing (DSP). When a user touches the digital crown of their watch to take an ECG, the device converts an analog bio-electrical signal into a digital format. Sophisticated algorithms then perform real-time baseline wandering correction and high-frequency noise filtering. This ensures that the resulting waveform, which appears on a smartphone screen, is clean enough for clinical interpretation, representing a masterpiece of software engineering and signal theory.
Wearable ECGs: The Rise of Consumer Health Hardware
The integration of ECG sensors into consumer electronics like the Apple Watch, Fitbit, and Samsung Galaxy Watch has democratized cardiac monitoring. This shift represents a pivot in the “Gadget” niche, where the value proposition of a device is no longer just connectivity or entertainment, but life-saving utility.
The Engineering Behind Smartwatch ECGs
While a standard clinical ECG uses 12 leads (sensors) to provide a 3D view of the heart’s electrical activity, most wearable tech utilizes a “Single-Lead” ECG. From a technical standpoint, this is a feat of circuit design. The circuit is completed when the user touches a sensor on the top of the device while the back of the device remains in contact with their wrist. This creates a “Lead I” configuration, measuring the potential difference between the left and right arms. The engineering challenge involves maintaining a stable signal despite the lack of medical-grade adhesive, requiring advanced firmware to detect when a “good” contact is made.
Data Connectivity and the Internet of Medical Things (IoMT)
The modern ECG is a cornerstone of the Internet of Medical Things. Once the hardware captures the heart’s rhythm, the data is not localized; it is synced via Bluetooth or Wi-Fi to a cloud-based ecosystem. This connectivity allows for the seamless sharing of PDF reports with physicians and the integration of cardiac data into broader health platforms like Apple HealthKit or Google Fit. This ecosystem relies on robust API (Application Programming Interface) structures that allow different software tools to communicate, ensuring that a heart rhythm captured in a coffee shop can be viewed by a cardiologist miles away.
AI and Machine Learning in Electrocardiogram Interpretation
Perhaps the most significant “Tech” development in the world of ECGs is the application of Artificial Intelligence (AI). Raw ECG data is complex, and until recently, it required a trained human eye to interpret. Today, machine learning models are augmenting—and in some cases, surpassing—human capabilities in rhythm analysis.
Pattern Recognition and Arrhythmia Detection
AI models, specifically Convolutional Neural Networks (CNNs), are trained on millions of ECG strips to recognize the specific patterns associated with conditions like Atrial Fibrillation (AFib), bradycardia, and tachycardia. Unlike a human doctor who looks at a snapshot in time, these AI tools can process continuous data streams from wearables, identifying transient “blips” in the heart’s rhythm that might be missed during a 10-minute clinic visit. The “tech” here lies in the training sets and the optimization of the model to run on the low-power processors found in mobile devices (Edge AI).
Predictive Analytics for Early Intervention
Beyond mere detection, the next frontier in ECG tech is predictive analytics. Researchers are now using deep learning to identify subtle changes in an ECG waveform—invisible to the naked eye—that may predict the onset of heart failure or a future stroke. By analyzing the “QT interval” or the “P-wave morphology” through high-throughput computing, software can flag users who are at high risk before they ever feel a symptom. This transition from “reactive” to “proactive” health is a direct result of software engineering advancements.
Software Solutions and the Cloud-Based Health Ecosystem
The hardware is only the tip of the iceberg. The infrastructure that supports the ECG data—the software—is where the digital security and data management challenges reside.
HIPAA-Compliant Data Storage and Remote Monitoring
Because an ECG is sensitive medical information, the tech companies providing these services must build infrastructure that adheres to strict digital security standards, such as HIPAA in the United States or GDPR in Europe. This involves end-to-end encryption for data in transit and at rest. The software architecture must be “hardened” against cyber threats, as a breach of cardiac data is a significant privacy violation. For tech developers, this means implementing rigorous authentication protocols and secure cloud storage solutions.
Integrating ECG Data with Telehealth Platforms
The COVID-19 pandemic accelerated the integration of ECG tech into telehealth software. Developers are now creating dashboards that allow doctors to monitor hundreds of patients’ ECG data in real-time. This “Remote Patient Monitoring” (RPM) software utilizes data visualization tools to highlight anomalies, allowing clinicians to focus on patients who need immediate attention. The tech stack for these platforms often involves real-time data streaming (WebSockets) and sophisticated backend databases (NoSQL) capable of handling massive amounts of time-series data.
The Future of Cardiac Tech: Beyond the Wrist
As we look toward the next decade, electrocardiogram technology is moving beyond the standard smartwatch form factor into even more integrated “Invisible Tech.”
Flexible Electronics and Smart Textiles
The next generation of ECG tech involves “electronic skin” or smart textiles. These are flexible, stretchable sensors that can be printed directly onto clothing or adhered to the skin like a temporary tattoo. This requires breakthroughs in material science and conductive polymers. Imagine a shirt that functions as a continuous 12-lead ECG, providing clinical-grade data during a marathon or a high-stress work meeting. The tech challenges here involve maintaining signal integrity as the fabric stretches and washes.
The Ethical Frontier: Digital Privacy and Bio-Sensing
As ECG sensors become more common in gadgets, we face new questions regarding “Bio-Sensing” ethics. Can a company use your heart rate variability (HRV) or ECG data to determine your emotional state or stress level for targeted advertising? The technology is certainly capable of it. As we continue to develop these tools, the tech community must lead the conversation on “Data Sovereignty”—the idea that the user, not the device manufacturer, owns the electrical signatures of their own heart.
In conclusion, the electrocardiogram has evolved from a medical curiosity into a cornerstone of the modern technological ecosystem. By combining advanced MEMS hardware, sophisticated digital signal processing, AI-driven diagnostics, and secure cloud infrastructure, we have turned the human heart into a source of actionable data. As we move forward, the “Tech” of the ECG will continue to blur the lines between consumer electronics and professional healthcare, making the proactive monitoring of our most vital organ a standard feature of the digital age.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.