The intersection of medical engineering and human physiology has reached a pinnacle in the field of urological prosthetics. For decades, the penile implant—specifically the Inflatable Penile Prosthesis (IPP)—has served as the gold standard for treating refractory erectile dysfunction. However, as we approach an era defined by bionic integration and refined MedTech “user experience,” the focus has shifted from mere mechanical functionality to the nuance of anatomical aesthetics and sensory feedback. One of the most common technical inquiries from both clinicians and patients involves the “terminal” point of the device’s impact: the glans penis, or the penis head.

Understanding what happens to the penis head after a penile implant requires a deep dive into hydraulic engineering, material science, and the biological limitations of current-generation hardware.
The Hardware Interface: How Inflatable Prosthetics Redefine Physiology
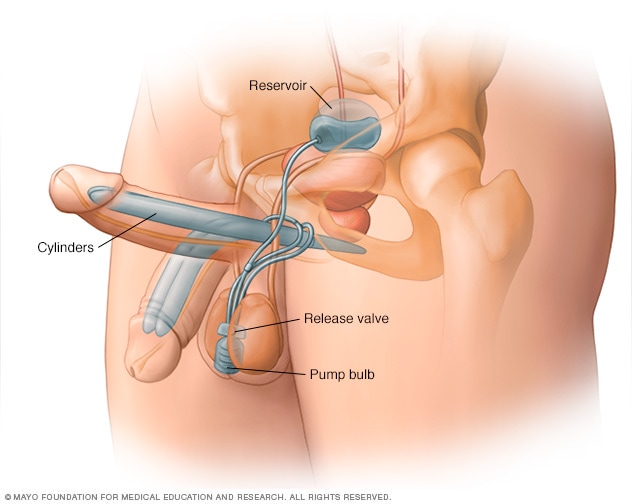
To understand the post-operative state of the penis head, one must first understand the mechanical architecture of the device itself. A modern three-piece inflatable implant is a masterpiece of fluid dynamics, typically consisting of a reservoir, a pump, and two cylinders.
The Mechanism of Action
The cylinders are surgically integrated into the corpora cavernosa, the two lateral chambers of the penis that naturally fill with blood during a biological erection. When the user activates the scrotal pump, saline is transferred from the pelvic reservoir into these cylinders. From a tech perspective, this is a closed-loop hydraulic system designed to provide structural rigidity.
The Anatomical Decoupling
The primary technical challenge lies in the fact that the glans (the penis head) is anatomically part of the corpus spongiosum, not the corpora cavernosa. Because the implant cylinders are housed within the cavernosa, the hydraulic pressure generated by the device does not directly reach the glans. In a natural erection, the glans engorges due to increased blood flow; in a prosthetic-assisted erection, the glans remains a separate “module” that does not automatically respond to the activation of the pump hardware.
Material Science and Pressure Distribution
Leading MedTech manufacturers, such as Boston Scientific (AMS 700) and Coloplast (Titan), have spent years refining cylinder coating and expansion capabilities. While these materials allow for girth and length optimization within the cavernosa, they are designed to terminate just before the glans to avoid “supersonic” tip deformities or erosion. This creates a unique physiological state where the shaft is rigid (Tech-driven) while the head may remain soft (Bio-driven).
The Sensory Gap: Why the Glans Behaves Differently Post-Integration
In the tech world, a “bottleneck” occurs when one component cannot keep up with the performance of another. In the context of a penile implant, the “Sensory Gap” is a frequent post-operative observation. This refers to the Glans Engorgement Insufficiency (GEI), where the penis head does not match the turgidity of the implanted shaft.
The Impact on Sensory Feedback Loops
The glans is the most nerve-dense region of the male anatomy, serving as the primary sensory interface. Because the implant provides mechanical rigidity without necessarily stimulating the vascular engorgement of the glans, some users report a “cold glans” sensation. From a technical standpoint, the sensory “input” remains intact—the nerves are generally not damaged during the procedure—but the “output” (physical swelling) is absent because the implant does not interact with the spongiosum.
Thermoregulation and Aesthetics
A common observation in post-implant patients is the difference in temperature. Since the cylinders are filled with room-temperature or body-temperature saline and do not rely on active blood flow for rigidity, the glans may appear paler or feel cooler than the rest of the shaft. This is an expected outcome of current prosthetic architecture, though engineers are constantly looking for ways to improve thermal conductivity within the device materials.
The “SST” Deformity (Supersonic Tip)
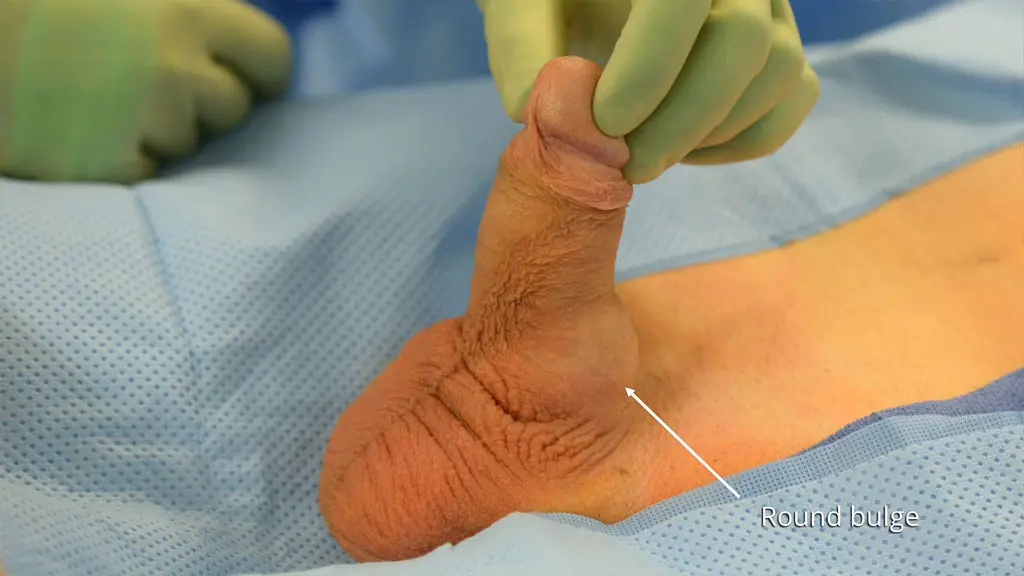
If the implant cylinders are not sized correctly or if the distal ligaments are weak, the glans may droop over the end of the rigid cylinders. In the industry, this is known as a “SST” deformity. It is essentially a mechanical misalignment where the hardware (the cylinders) and the “software” (the anatomical tip) are out of sync. Modern surgical techniques have largely mitigated this through more precise “mapping” of the distal space during implantation.
MedTech Innovations Addressing Glans Engorgement Insufficiency (GEI)
As patient expectations evolve, the MedTech industry has moved beyond “functional rigidity” toward “anatomical harmony.” Several “tech patches” and supplementary protocols have been developed to address the behavior of the penis head post-implant.
Pharmacological Integration
To compensate for the lack of natural engorgement in the glans, many clinicians recommend a “hybrid” approach. This involves using low-dose PDE5 inhibitors (like Sildenafil or Tadalafil) or topical alprostadil. In tech terms, this is an “analog override”—using chemistry to stimulate the corpus spongiosum to fill the glans while the implant provides the structural backbone. This creates a more natural-looking and feeling result.
Surgical “Glanulopexy” Patches
For patients prone to “floppy glans” syndrome, surgeons utilize a technique called Glanulopexy. This is essentially a “hardware fix” where the glans is internally sutured to the tips of the corporal bodies. This prevents the head from shifting or drooping during use, ensuring that the mechanical energy of the implant is correctly channeled through the tip of the device.
Advanced Imaging and Sizing Tools
The use of intraoperative ultrasound and specialized measuring tools (like the Furlow Inserter) allows for a more “bespoke” fit. By maximizing the cylinder length to the very edge of the distal corpora, surgeons can ensure that the penis head is better supported by the internal hardware, reducing the appearance of a “detached” tip.
Data-Driven Outcomes: The UX of Post-Operative Recovery
When evaluating any technology, the “User Experience” (UX) is the ultimate metric of success. For penile implants, the satisfaction rates are remarkably high—often exceeding 90%—but the “behavior” of the penis head remains a key point of post-operative adjustment.
Managing Expectations Through Data
Clinical data suggests that while the glans may not engorge as it once did, the overall utility of the device far outweighs the aesthetic trade-off for the vast majority of users. Data sets from long-term follow-ups show that the “soft glans” actually provides a safety benefit, acting as a “buffer” during intercourse that prevents tissue erosion and discomfort for the partner.
The Learning Curve of the Interface
The first 6–12 weeks post-surgery are critical for “cycling” the device. This process is akin to breaking in a new piece of hardware. Frequent inflation and deflation help the tissue—including the glans—expand and accommodate the new internal pressures. Over time, the “integrated” look of the penis improves as the internal scarring softens and the cylinders settle into their permanent housing.
Psychological Integration and “The New Normal”
From a branding perspective, the penile implant is often marketed as a “return to form.” However, from a technical perspective, it is a “replacement of function.” Patients who view the device as a high-performance medical tool rather than a 1:1 biological replica tend to report higher satisfaction. The “head” of the penis becomes a sensory cap on a sophisticated hydraulic system, a shift in perspective that is vital for long-term success.
The Horizon of Bionic Phalloplasty: From Hydraulics to Neural Linkage
The future of penile implants lies in the transition from purely mechanical devices to “smart” prosthetics. Research is currently underway to determine how MedTech can better simulate the biological nuances of the glans.
Responsive Materials
The next generation of implants may utilize shape-memory alloys or advanced polymers that can change shape or volume more dynamically. Imagine a cylinder that doesn’t just expand in girth, but has a distal “bulb” designed to specifically support the glans. This would solve the “decoupling” issue by providing direct mechanical support to the penis head.
Electronic Activation and IoT Integration
While current models are manually pumped, the concept of a “micro-pump” activated via a discreet remote or even a smartphone app is within the realm of possibility. Such a system could allow for granular control over pressure, potentially allowing for a “pre-load” phase that encourages what little natural blood flow remains to enter the glans before full rigidity is achieved.
Neural Interface and Sensory Restoration
The “holy grail” of this tech niche is the restoration of active engorgement through neural stimulation. By integrating the implant with neuro-modulators, it may one day be possible to trigger the body’s natural “swelling” response in the glans while the mechanical cylinders provide the necessary stiffness. This would create a truly seamless integration between man and machine.
In conclusion, while the penis head undergoes a transition from a biologically-driven component to a supported anatomical tip after an implant, the technology behind this shift is nothing short of revolutionary. The “soft glans” is not a bug in the system, but a current limitation of hydraulic design that is being actively addressed through surgical innovation, pharmacological supplements, and the future of bionic engineering. For those navigating this tech-heavy medical journey, understanding the “hardware/software” split of the anatomy is the first step toward a successful and satisfying outcome.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.