The distinct sensation of a torn bicep muscle is a potent and often alarming indicator of a significant musculoskeletal injury. While medical professionals have long relied on patient descriptions to aid in diagnosis, the advent of advanced technology is revolutionizing our understanding and management of such conditions. From sophisticated diagnostic imaging and wearable sensors to AI-powered rehabilitation programs, technology offers unprecedented insights into the physical experience of a torn bicep and the pathways to recovery. This exploration delves into what a torn bicep muscle feels like, viewed through the prism of technological advancements that are transforming how we perceive, treat, and overcome these injuries.
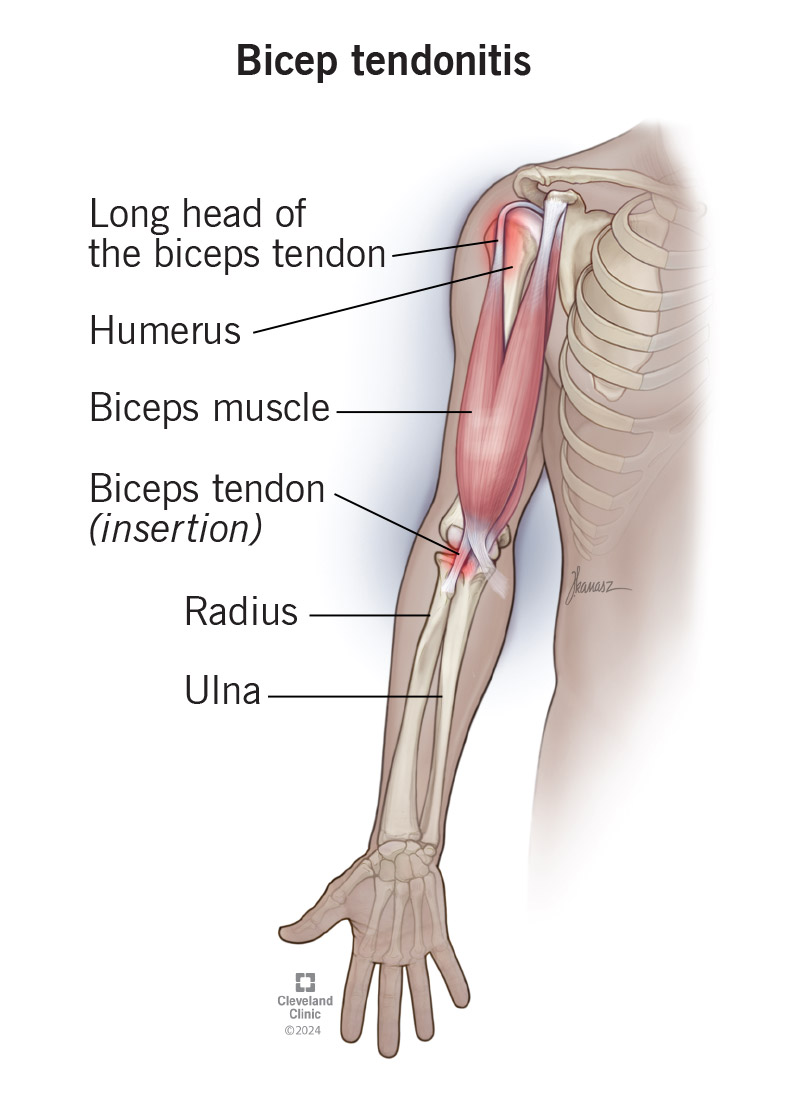
The Immediate Onset: A Symphony of Sharp Sensations and Audible Clues
The initial moments following a bicep tear are often characterized by a dramatic and unmistakable physical response. The tearing of muscle fibers, whether partial or complete, triggers a cascade of sensory signals that are difficult to ignore. Understanding these initial sensations is the first step in recognizing the potential severity of the injury, and increasingly, technology plays a role in capturing and analyzing these subtle yet crucial data points.
The “Pop” or “Snap”: Acoustic Signatures of Injury
Many individuals report hearing or feeling a distinct “pop” or “snap” at the moment of injury. This auditory and tactile sensation is often described as a sharp, forceful event, akin to a rubber band breaking under tension. This is the sound of tendon detaching from bone or substantial muscle fibers rupturing. While historically anecdotal, advances in wearable biosensors are beginning to explore the possibility of capturing such acoustic events. Inertial Measurement Units (IMUs) and sensitive microphones embedded in athletic apparel or smartwatches could potentially detect and record the unique frequency and amplitude patterns associated with this type of trauma. This data, when correlated with other physiological readings like sudden acceleration or deceleration, could offer an objective timestamp and intensity measurement for the initial injury, aiding in later diagnostic assessments and even informing the development of predictive models for injury risk.
The Palpable Defect and Swelling: Visible and Tactile Changes
Following the initial trauma, a characteristic palpable defect or indentation may become apparent in the bicep muscle, particularly with more severe tears. This is where the torn muscle fibers have retracted, creating a noticeable gap. The area will often become exquisitely tender to the touch. Simultaneously, rapid swelling, known as edema, begins to develop around the injured site. This swelling is the body’s inflammatory response, sending fluid to the damaged area to initiate the healing process. High-resolution ultrasound and MRI, while medical diagnostic tools, are the technological apex in visualizing these internal changes. However, consumer-level wearable pressure sensors are an emerging area of research, potentially capable of detecting subtle changes in tissue tension and volume that could indicate developing edema or structural alterations in the muscle, providing early warning signs even before significant swelling is visible.
Intense and Localized Pain: The Body’s Alarms
The pain associated with a torn bicep is typically immediate, sharp, and intensely localized to the site of the tear. It is often described as a searing or ripping sensation that intensifies with any attempt to move the arm or contract the bicep muscle. This pain is a direct signal from damaged nerve endings within the muscle and surrounding tissues. Wearable pain monitoring devices, though still in their nascent stages, are exploring ways to quantify pain perception. These devices might integrate multiple biometric readings, such as heart rate variability, galvanic skin response, and even electroencephalogram (EEG) data from headbands, to provide a more objective measure of pain intensity and its impact on the individual’s physiological state. This objective data can be invaluable for tracking pain progression and response to treatment, moving beyond purely subjective reports.
The Lingering Aftermath: Persistent Discomfort and Functional Impairment
Beyond the acute phase, a torn bicep muscle continues to present a spectrum of persistent symptoms that significantly impact daily life and physical capabilities. These lingering effects are areas where technology is making significant inroads in both assessment and rehabilitation.
Bruising and Discoloration: Visual Indicators of Internal Damage
As blood vessels within the torn muscle rupture, blood can seep into the surrounding tissues, leading to the development of bruising (ecchymosis) and discoloration around the bicep and potentially extending down the forearm. The color of the bruise typically progresses from red to purple, then to blue and green as the body begins to break down the pooled blood. While visually evident, the extent and depth of bruising can be more precisely quantified using advanced imaging techniques. Moreover, for those engaged in rigorous physical training, wearable sensors capable of analyzing skin tone variations or subtle thermal changes could potentially offer an early, non-invasive indication of developing hematomas, allowing for more timely interventions.
Weakness and Loss of Strength: Quantifying Functional Deficits
A hallmark of a torn bicep is profound weakness and a significant reduction in the ability to perform actions that require flexing the elbow or supinating the forearm. This loss of strength is directly proportional to the extent of the muscle tear. Historically, strength assessment relied on manual muscle testing by a clinician. However, the proliferation of smart strength training equipment and wearable motion capture systems is revolutionizing this field. Devices like smart dumbbells, resistance bands with integrated sensors, and full-body motion capture suits can objectively measure force output, range of motion, and muscle activation patterns. This granular data allows for precise quantification of strength deficits, tracking recovery progress with objective metrics, and tailoring rehabilitation exercises to specific weaknesses.
Muscle Spasms and Cramping: Involuntary Muscle Reactions
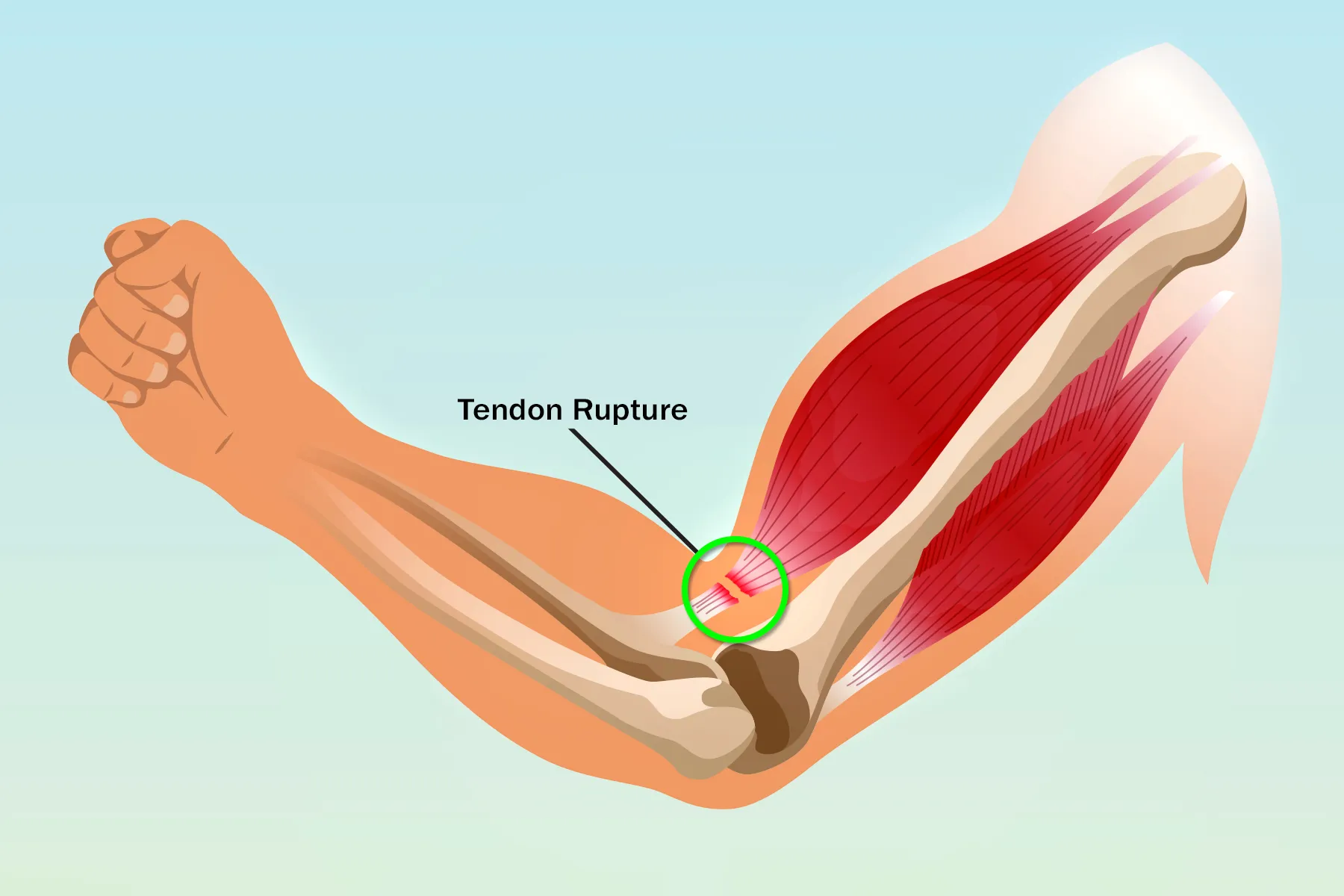
In the aftermath of a tear, the injured muscle and surrounding tissues may experience involuntary spasms and cramping. These are often painful and can occur spontaneously or be triggered by certain movements or positions. These muscle contractions are the body’s attempt to stabilize the injured area, but they can also hinder the healing process and cause additional discomfort. Electromyography (EMG) is a well-established medical technology that measures the electrical activity produced by skeletal muscles. Wearable EMG sensors are becoming increasingly sophisticated and accessible, allowing individuals to monitor muscle activity patterns, identify areas of excessive or abnormal firing, and receive biofeedback to help control spasms. This technology can also inform targeted stretching and relaxation exercises designed to alleviate cramping and improve muscle function.
Navigating Recovery: The Role of Technology in Rehabilitation
The journey back to full function after a torn bicep muscle is often a lengthy and challenging one. Fortunately, technological innovations are transforming the rehabilitation landscape, offering personalized, data-driven, and engaging approaches to recovery.
Virtual Reality (VR) and Augmented Reality (AR) for Engaging Therapy
Rehabilitation can often be monotonous, leading to decreased patient adherence. VR and AR technologies are stepping in to make physical therapy more engaging and interactive. Imagine a VR environment where a patient performs controlled bicep movements to achieve in-game objectives, turning repetitive exercises into a stimulating experience. AR overlays can provide real-time feedback on proper form and technique, guiding patients through exercises with visual cues. These immersive environments can also help desensitize the injured area by gradually exposing the individual to controlled movements in a simulated, low-risk setting. By gamifying the recovery process and providing immediate, visual feedback, VR and AR can significantly boost motivation and adherence to rehabilitation protocols.
Wearable Sensors and AI for Personalized Progress Tracking
Wearable sensors, from accelerometers and gyroscopes in smartwatches to dedicated limb-tracking devices, can continuously monitor a patient’s movement patterns, range of motion, and adherence to prescribed exercises outside of therapy sessions. This data is then fed into AI algorithms that can analyze recovery progress, identify potential plateaus, and alert healthcare providers to any deviations from the expected healing trajectory. AI can personalize exercise prescriptions, adjusting intensity, duration, and type of activity based on real-time performance data. This data-driven approach ensures that rehabilitation programs are optimally tailored to the individual’s needs, maximizing efficiency and promoting faster, more complete recovery.
Tele-Rehabilitation and Remote Monitoring: Bridging the Distance
The integration of technology has paved the way for tele-rehabilitation, allowing patients to receive expert guidance and monitoring remotely. Through video conferencing platforms, coupled with data from wearable sensors, physical therapists can assess progress, provide feedback on exercise technique, and make necessary adjustments to the rehabilitation plan without the patient needing to be physically present. This is particularly beneficial for individuals in rural areas, those with mobility limitations, or during times when in-person visits are difficult. AI-powered chatbots can also provide round-the-clock support, answering common questions, reminding patients about exercises, and gathering initial symptom reports before a scheduled tele-consultation. This democratizes access to high-quality rehabilitation services and ensures continuous oversight of the recovery process.
The Technological Horizon: Future Implications for Bicep Injury Management
The continuous evolution of technology promises even more sophisticated tools for understanding and managing torn bicep muscles, extending beyond diagnosis and rehabilitation into prevention and advanced therapeutic interventions.
Predictive Analytics for Injury Prevention in Athletes
As wearable technology becomes more sophisticated, so too does the potential for predictive analytics in sports. By collecting vast datasets on an athlete’s training load, biomechanics, sleep patterns, and physiological responses, AI algorithms can identify subtle patterns that may indicate an increased risk of bicep injury. This allows for proactive adjustments to training regimens, rest protocols, or the implementation of targeted pre-habilitation exercises to mitigate potential harm. Understanding the specific forces and movements that lead to bicep tears in different sports can inform the design of better protective equipment and training methodologies.
Advanced Biomechanical Analysis for Precise Rehabilitation
Beyond simply tracking movement, future technologies will offer increasingly detailed biomechanical analysis of muscle function. Advanced motion capture systems, coupled with force plates and electromyography, will provide a comprehensive understanding of how muscles are recruited, the efficiency of movement patterns, and the presence of compensatory strategies that could predispose to re-injury. This level of detail will enable physical therapists to design highly precise rehabilitation programs that address the root causes of functional deficits, rather than just the symptoms.

Biofeedback and Neurostimulation for Enhanced Muscle Activation
Emerging biofeedback techniques and wearable neurostimulation devices hold promise for directly influencing muscle function during rehabilitation. Neurostimulation, for example, can be used to elicit muscle contractions, helping to re-educate muscles that have become de-conditioned or have lost their neural pathways due to injury. Advanced biofeedback systems can provide real-time, intuitive information about muscle activation, helping individuals to better control and strengthen their bicep. These technologies represent a frontier in actively guiding and enhancing the body’s natural healing and strengthening processes.
In conclusion, the experience of a torn bicep muscle, from its sharp, immediate onset to its lingering effects and the challenges of recovery, is being fundamentally reshaped by technological advancements. What was once primarily a subjective experience, relying on a patient’s descriptive narrative, is now augmented by objective data captured by sophisticated sensors and analyzed by intelligent algorithms. This technological integration not only enhances our understanding of the physical sensations of injury but also empowers individuals with more effective, personalized, and accessible tools for regaining strength and returning to their full potential. The future of managing musculoskeletal injuries like torn biceps is undeniably intertwined with the innovative applications of technology.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.