Hemodialysis technicians, often referred to as nephrology technologists or dialysis technologists, are essential members of the healthcare team responsible for administering and monitoring hemodialysis treatments. These treatments are life-sustaining for individuals suffering from kidney failure, where their kidneys are no longer able to effectively filter waste products and excess fluid from the blood. While the core function of a hemodialysis technician is to facilitate this crucial medical procedure, their role extends far beyond simply operating machinery. They are integral to patient care, safety, and the overall efficient functioning of dialysis centers. This article will delve into the multifaceted responsibilities of a hemodialysis technician, focusing on the technical aspects of their role and the critical technological integration that underpins their practice.

The Technical Backbone of Hemodialysis
At the heart of a hemodialysis technician’s work lies a deep understanding and proficient operation of sophisticated medical technology. The hemodialysis machine itself is a complex piece of equipment, and the technician is responsible for its preparation, operation, and maintenance to ensure patient safety and treatment efficacy.
Understanding and Operating Hemodialysis Machines
The hemodialysis machine, also known as an artificial kidney, is the central piece of technology used in the treatment. These machines are designed to mimic the function of healthy kidneys by cleaning the blood of waste products like urea and creatinine, and by removing excess fluid. Technicians must be thoroughly trained on the specific models of machines used in their facility, as different manufacturers and models can have varying interfaces, protocols, and functionalities.
This training involves understanding the various components of the machine, including:
- Blood Pump: This component controls the flow rate of blood from the patient’s access point, through the dialyzer, and back to the patient. Technicians must ensure the pump is set to the prescribed rate for each patient.
- Dialyzer (Artificial Kidney): This is where the actual filtration of blood occurs. It contains a semipermeable membrane that allows waste products and excess fluid to pass from the blood into the dialysate, while keeping essential components like blood cells and proteins in the blood. Technicians are responsible for setting up the dialyzer, ensuring it is properly connected, and monitoring its performance.
- Dialysate Delivery System: This system prepares and delivers the dialysate, a sterile solution that draws waste products from the blood. Technicians monitor the composition, temperature, and conductivity of the dialysate to ensure it meets the patient’s prescribed needs.
- Monitoring and Alarm Systems: Hemodialysis machines are equipped with advanced sensors and alarm systems to continuously monitor critical parameters such as blood pressure, blood flow rate, fluid removal rate, and potential air in the bloodline. Technicians must be vigilant in responding to any alarms, which can indicate a potential complication.
The technician’s role begins before the patient even connects to the machine. They meticulously prepare the equipment, checking for any signs of damage, ensuring all components are sterile and correctly assembled. This pre-treatment check is paramount in preventing infections and ensuring the machine functions flawlessly.
Setting Up and Managing Vascular Access
A critical technical aspect of hemodialysis is the management of vascular access, which is the pathway through which blood is taken from and returned to the patient’s body. Technicians play a vital role in preparing and managing these access points, ensuring a smooth and safe treatment.
There are three primary types of vascular access used for hemodialysis:
- Arteriovenous (AV) Fistula: This is a surgically created connection between an artery and a vein, typically in the arm. Over time, the vein enlarges and thickens, making it suitable for repeated needle insertions. Technicians are responsible for assessing the fistula for patency and adequacy before each treatment, which may involve feeling for a thrill (vibration) and listening for a bruit (sound).
- Arteriovenous (AV) Graft: This involves using a synthetic tube to connect an artery and a vein. Grafts are used when AV fistulas are not possible. Similar to fistulas, technicians assess grafts for signs of infection or clotting.
- Central Venous Catheter: This is a temporary or permanent tube inserted into a large vein, usually in the neck or chest. Catheters are often used when AV fistulas or grafts are not yet ready or are not feasible. Technicians are responsible for the meticulous aseptic technique required for accessing and disconnecting catheters, and for monitoring for signs of infection at the insertion site.
The technician’s technical skill extends to cannulating AV fistulas and grafts with specialized needles, ensuring proper placement to facilitate adequate blood flow without causing undue trauma to the access site. They must also be adept at managing catheters, including flushing and dressing changes, adhering to strict sterile protocols.
Patient Monitoring and Safety Protocols
Beyond the mechanical operation of dialysis equipment, hemodialysis technicians are front-line observers of patient well-being during treatment. Their technical understanding allows them to interpret physiological data and respond proactively to ensure patient safety.
Vital Sign Monitoring and Data Interpretation
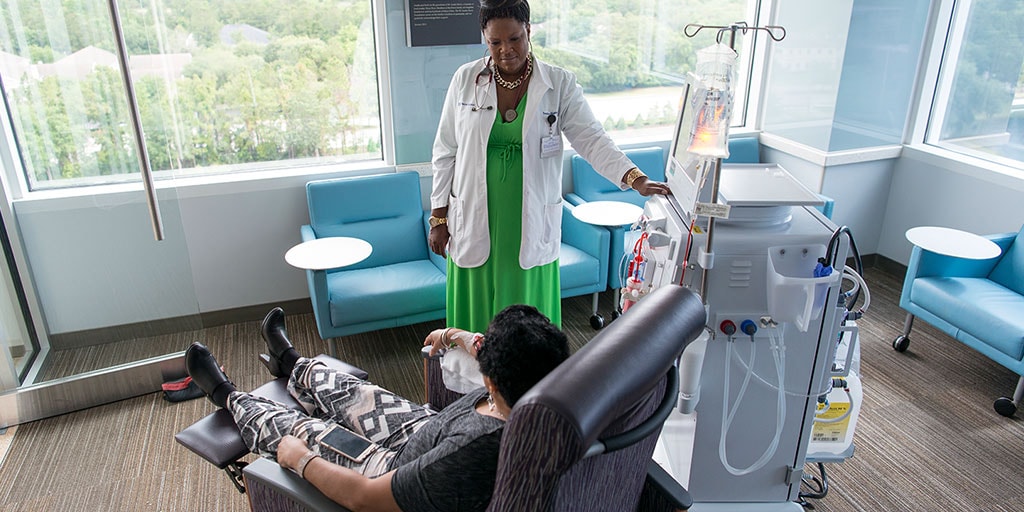
Throughout the hemodialysis session, which typically lasts 3-5 hours, the technician meticulously monitors the patient’s vital signs. This includes:
- Blood Pressure: Significant fluctuations can occur during dialysis due to fluid removal, requiring careful observation and adjustment.
- Heart Rate and Rhythm: Technicians monitor for any irregularities or changes that might indicate cardiac distress.
- Temperature: To detect potential signs of infection or fever.
- Fluid Balance: Tracking the amount of fluid removed and ensuring it aligns with the prescribed prescription.
- Blood Flow Rate: Monitoring the speed at which blood is circulating through the dialyzer.
The hemodialysis machine itself provides a constant stream of data related to the treatment process. Technicians are trained to interpret this data, understanding what constitutes normal parameters and what might indicate a deviation. For example, a sudden drop in blood pressure or an increase in the rate of fluid removal could signal a developing complication. Their ability to quickly analyze this information and react appropriately is critical.
Recognizing and Responding to Complications
Despite the advanced technology, complications can arise during hemodialysis. Hemodialysis technicians are trained to recognize the early signs and symptoms of various potential issues, including:
- Hypotension (Low Blood Pressure): This is a common complication, often characterized by dizziness, nausea, and sweating. Technicians will typically slow the blood flow rate, reduce the rate of fluid removal, or administer saline to stabilize the patient.
- Hypertension (High Blood Pressure): Less common but still a concern, requiring intervention to manage.
- Cramps: Muscle cramps are frequent and can be addressed by slowing the fluid removal.
- Nausea and Vomiting: Often associated with rapid fluid or solute removal.
- Allergic Reactions: To the dialyzer or dialysate.
- Air Embolism: A potentially life-threatening event where air enters the bloodstream. Technicians are trained in procedures to prevent and manage this.
- Infections: At the vascular access site.
Prompt and accurate recognition of these issues, coupled with immediate intervention according to established protocols, is a hallmark of a skilled hemodialysis technician. They often work under the direct supervision of a registered nurse, who provides advanced medical assessment and management, but the technician’s initial actions can significantly influence the outcome of a complication.
Maintaining Equipment and Ensuring Sterility
The sterile environment and meticulously maintained equipment are fundamental to the safety and efficacy of hemodialysis. Technicians play a crucial role in upholding these standards through their diligent practices.
Disinfection and Sterilization Procedures
Hemodialysis machines and their components, particularly the dialyzer and bloodlines, must be thoroughly disinfected or sterilized between patient uses. Technicians are responsible for:
- Machine Disinfection: Performing chemical or heat disinfection cycles on the dialysis machines according to manufacturer guidelines and facility protocols. This process kills microorganisms that could be transmitted between patients.
- Dialyzer Reprocessing (where applicable): In some facilities, dialyzers are reprocessed for reuse by patients. This is a highly technical and regulated process that involves cleaning, testing, and sterilization of used dialyzers. Technicians involved in reprocessing must adhere to stringent guidelines to ensure the safety and effectiveness of the reused equipment.
- Sterilization of Accessories: Ensuring that all ancillary equipment, such as dialysate delivery lines, blood pumps, and monitoring sensors, are properly sterilized or are single-use and disposed of appropriately.
The strict adherence to disinfection and sterilization protocols is a critical technical skill that directly prevents the spread of infections, a significant risk in any healthcare setting, especially one involving direct blood contact.
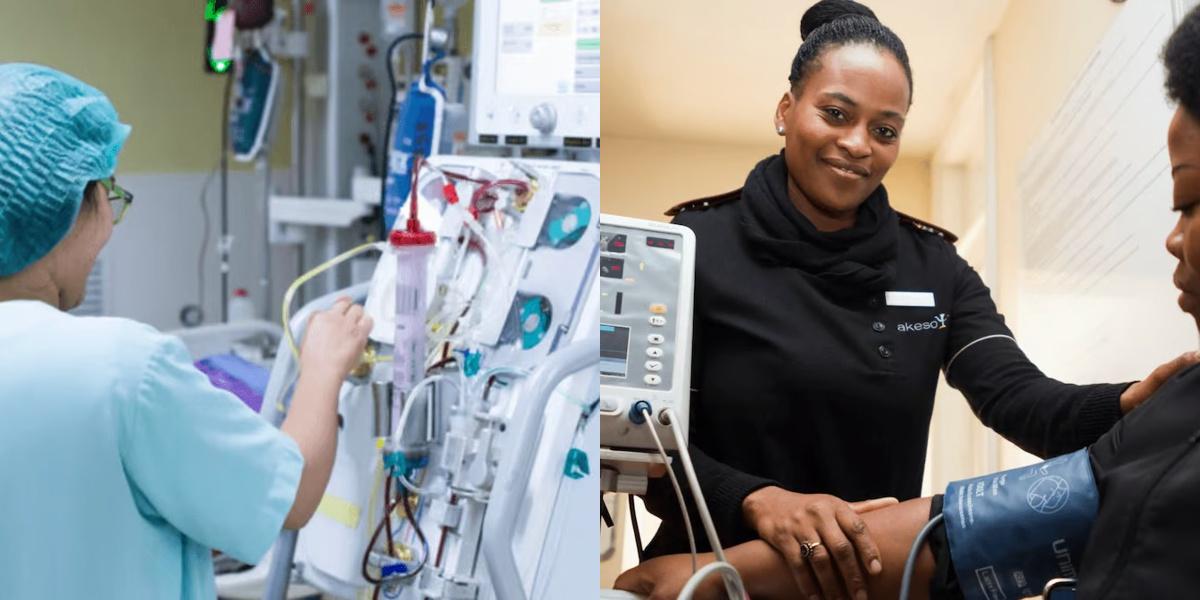
Quality Control and Troubleshooting
Beyond routine maintenance, technicians are often the first line of defense in identifying and addressing equipment malfunctions. This involves:
- Routine Equipment Checks: Performing daily and weekly checks on all dialysis machines and related equipment to ensure they are functioning optimally.
- Troubleshooting Minor Issues: Identifying and resolving minor technical glitches, such as sensor errors, pump malfunctions, or alarm system issues. They may refer more complex problems to biomedical engineers.
- Documentation: Maintaining detailed records of equipment maintenance, repairs, and quality control checks. This documentation is vital for regulatory compliance and for tracking equipment performance over time.
Their technical acumen in identifying and reporting potential problems before they escalate into serious issues ensures the continuous operation of the dialysis unit and minimizes disruptions to patient care. This proactive approach to equipment management is a testament to the technical expertise required in this specialized healthcare role.
In conclusion, the role of a hemodialysis technician is a technically demanding one, requiring a blend of precise mechanical operation, sharp observational skills, and a commitment to sterile technique. They are the custodians of life-sustaining technology, ensuring that patients with kidney failure receive safe and effective treatment. Their expertise in operating and maintaining complex dialysis machines, managing vascular access, and vigilantly monitoring patients underscores their indispensable contribution to the healthcare of individuals with end-stage renal disease.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.