The question, “What doctor checks prostate?” is fundamental to men’s health and underscores the importance of understanding specialized medical care. While a general practitioner often serves as the first point of contact, a deeper dive into urology reveals the dedicated expertise required for comprehensive prostate health management. This article will explore the roles of various medical professionals involved in prostate care, the technologies they utilize, and the proactive approaches to maintaining optimal prostate health.
The Urologist: The Specialist at the Forefront of Prostate Care
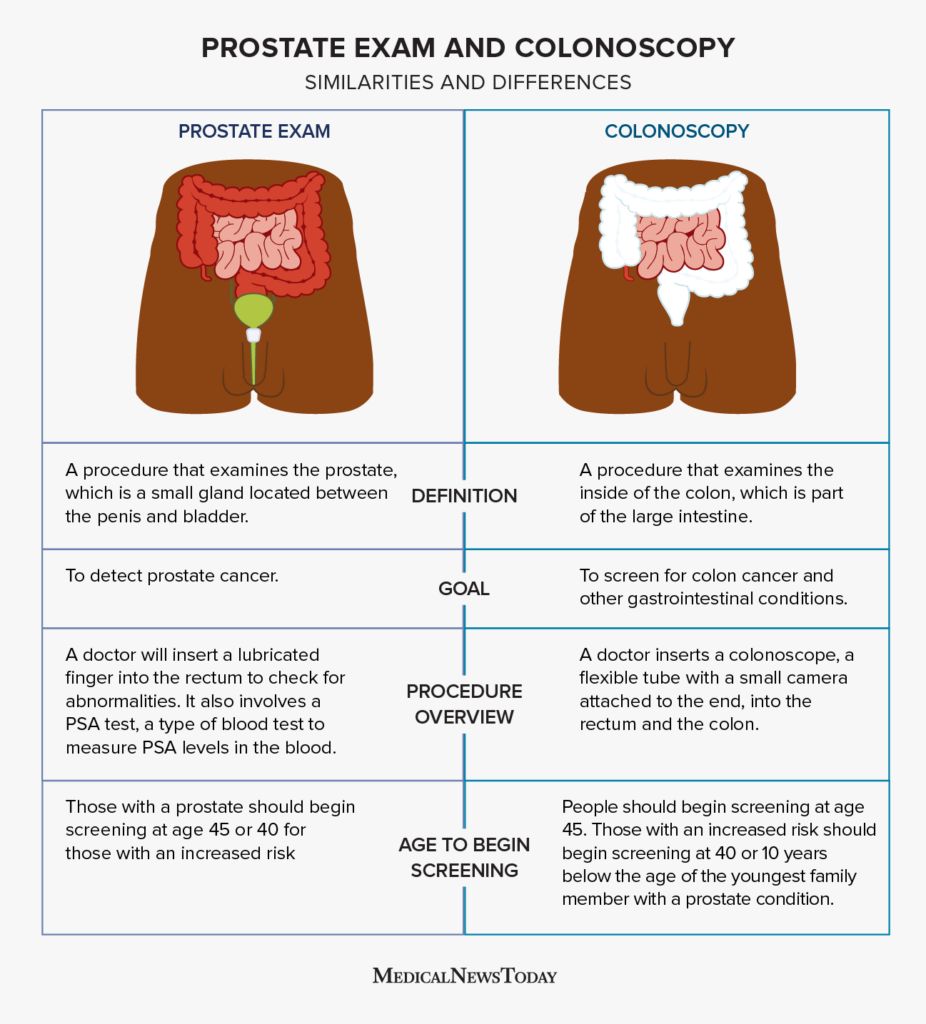
The primary physician responsible for checking and managing prostate health is the urologist. Urology is a surgical specialty that focuses on the urinary tract of males and females, and the reproductive system of males. This means urologists are uniquely qualified to diagnose and treat conditions affecting the prostate gland, as well as other organs like the bladder, kidneys, and testes.
What is a Urologist and Why Are They Crucial?
A urologist is a medical doctor who has completed extensive training in the diagnosis, treatment, and surgical management of diseases and disorders of the urinary system and male reproductive organs. Their expertise encompasses a wide range of conditions, from common issues like benign prostatic hyperplasia (BPH) and urinary tract infections (UTIs) to more serious concerns such as prostate cancer, prostatitis, and kidney stones.
For prostate-specific concerns, urologists are the go-to specialists. They possess in-depth knowledge of the prostate’s anatomy, physiology, and common pathologies. This specialized knowledge allows them to accurately interpret diagnostic tests, develop effective treatment plans, and perform necessary procedures, including biopsies and surgeries.
The Urologist’s Toolkit: Diagnostic and Treatment Modalities
Urologists employ a variety of tools and techniques to assess prostate health. These can be broadly categorized into diagnostic methods and treatment options.
Diagnostic Methods in Urology
The initial assessment by a urologist typically involves a combination of methods to gather comprehensive information about the prostate.
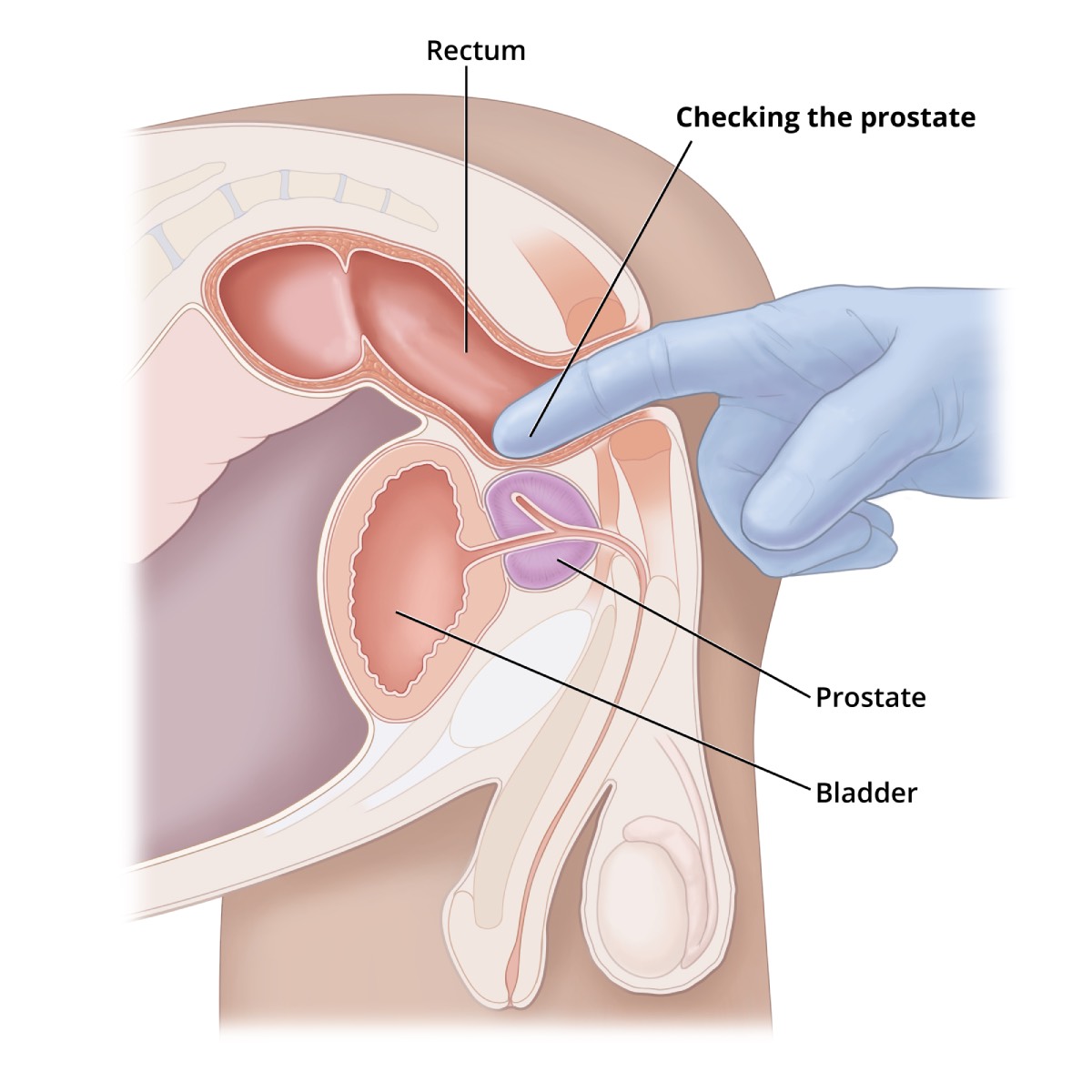
- Digital Rectal Exam (DRE): This is often one of the first steps in a prostate examination. The urologist inserts a gloved, lubricated finger into the rectum to feel the prostate gland for any abnormalities in size, shape, or texture, such as lumps or hard spots. While it can detect some changes, it’s not always conclusive on its own.
- Prostate-Specific Antigen (PSA) Blood Test: The PSA test measures the level of prostate-specific antigen, a protein produced by the prostate gland, in the blood. Elevated PSA levels can indicate a problem with the prostate, including an enlarged prostate, inflammation (prostatitis), or prostate cancer. However, it’s important to note that PSA levels can be affected by other factors besides cancer, such as infection or recent ejaculation.
- Urinalysis and Urine Culture: These tests help detect any signs of infection or inflammation in the urinary tract, which can sometimes be related to prostate issues.
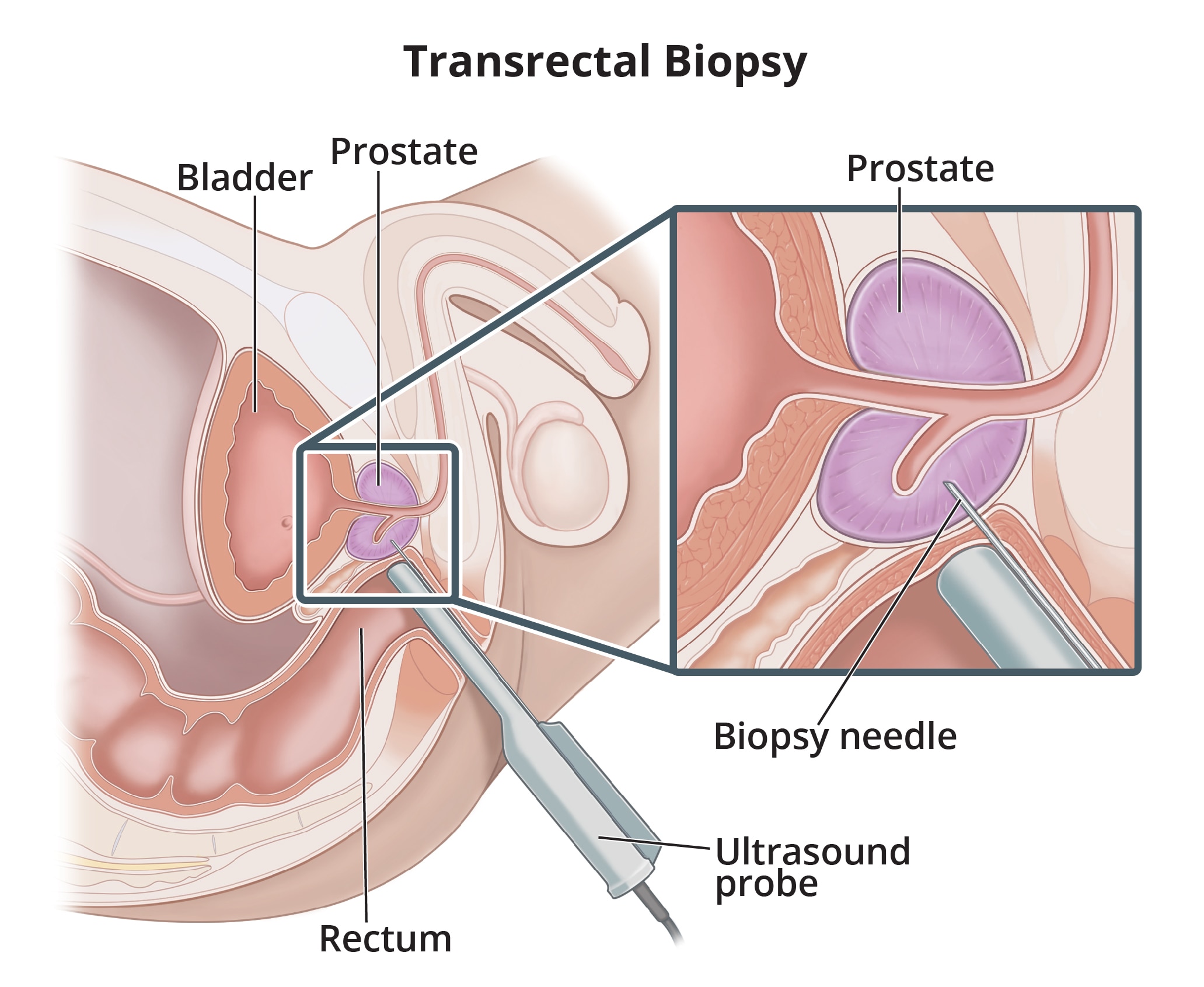
- Transrectal Ultrasound (TRUS): In this procedure, a small ultrasound probe is inserted into the rectum, allowing for detailed imaging of the prostate. TRUS can help visualize the size and structure of the prostate and guide biopsies if necessary.
- Prostate Biopsy: If suspicious findings are detected through DRE or PSA levels, a biopsy is often recommended. This involves taking small tissue samples from the prostate for microscopic examination by a pathologist to determine if cancer cells are present and, if so, their aggressiveness.
- Uroflowmetry: This test measures the speed and volume of urine flow, which can help identify blockages or issues with bladder function that might be related to prostate enlargement.
- Cystoscopy: In some cases, a cystoscope (a thin, flexible tube with a camera) may be inserted into the urethra to examine the bladder and urethra for any abnormalities, which can sometimes be influenced by prostate conditions.
Treatment Strategies for Prostate Conditions
Once a diagnosis is made, the urologist will discuss appropriate treatment options, which vary widely depending on the specific condition.
- Medications: For conditions like BPH, medications can be prescribed to relax the prostate muscles or shrink the prostate gland, improving urinary flow. Antibiotics are used to treat prostatitis.
- Minimally Invasive Procedures: Techniques like transurethral resection of the prostate (TURP) or laser ablation can be used to remove or reduce enlarged prostate tissue.
- Surgery: In cases of prostate cancer or severe BPH, surgical options may be considered, ranging from radical prostatectomy (removal of the prostate) to other surgical interventions.
- Radiation Therapy and Chemotherapy: For prostate cancer, these therapies are often used, sometimes in conjunction with surgery.
- Active Surveillance: For very early-stage, slow-growing prostate cancers, a urologist might recommend active surveillance, which involves regular monitoring without immediate treatment.
The General Practitioner: Your First Line of Defense in Men’s Health
While the urologist is the specialist, the general practitioner (GP) or primary care physician (PCP) plays a crucial role in the initial assessment and ongoing management of men’s health, including prostate health. They are often the first medical professional a man sees when experiencing symptoms or for routine check-ups.
The GP’s Role in Prostate Health Screening
General practitioners are trained to identify potential health issues and refer patients to specialists when necessary. For prostate health, their responsibilities include:
- Initial Symptom Assessment: If a man experiences symptoms like frequent urination, difficulty starting or stopping urination, or pain during urination, the GP will conduct an initial evaluation. This might include discussing medical history, performing a basic physical examination, and ordering preliminary tests like a PSA test or urinalysis.
- Routine Health Screenings: As part of a man’s regular physicals, GPs often discuss prostate health and may recommend or perform a PSA test based on age, family history, and individual risk factors. Current guidelines from various health organizations suggest a discussion about PSA screening should occur between the ages of 50 and 70, with earlier discussions for those at higher risk (e.g., African American men, men with a family history of prostate cancer).
- Referral to a Urologist: If the GP suspects a prostate issue, whether due to concerning symptoms or abnormal test results, they will refer the patient to a urologist for further investigation and specialized care. This referral ensures that the patient receives expert diagnosis and treatment from a doctor who focuses specifically on the prostate and urinary system.
- Management of Mild Conditions: In some cases, a GP might manage very mild conditions or follow up on test results that are within a normal range, providing reassurance and guidance.
The Importance of the Patient-GP Relationship
The relationship with a GP is vital for proactive health management. They have a holistic view of a patient’s health and can recognize how prostate health might intersect with other aspects of well-being. Regular visits to a GP allow for the establishment of a baseline of health, making it easier to detect subtle changes over time. This ongoing dialogue also empowers patients to ask questions and voice concerns about their health, including those related to their prostate.
Beyond the Urologist: Allied Health Professionals in Prostate Care
While the urologist and GP are central to prostate health, a network of other healthcare professionals can contribute to a patient’s overall care and recovery.
The Role of Radiologists and Pathologists
These specialists are critical behind-the-scenes players in prostate diagnostics.
- Radiologists: These physicians interpret medical imaging scans. In the context of prostate health, radiologists analyze ultrasounds (like TRUS), MRIs, and CT scans that are used to visualize the prostate gland, detect abnormalities, and guide biopsies. Their expertise is essential for accurate imaging-based diagnoses.
- Pathologists: When a prostate biopsy is performed, the tissue samples are sent to a pathologist. This doctor specializes in examining tissues and cells under a microscope to identify diseases. Pathologists determine if cancer cells are present, their type, and their grade (how aggressive they appear), which are crucial factors in determining treatment.
Other Allied Health Professionals
Depending on the diagnosis and treatment plan, other healthcare providers may become involved:
- Oncologists: For prostate cancer patients, medical oncologists (who administer chemotherapy and other systemic treatments) and radiation oncologists (who administer radiation therapy) are vital members of the care team.
- Nurses: Specialized nurses, such as urology nurses or oncology nurses, provide patient education, administer treatments, monitor patients, and offer emotional support.
- Physiotherapists: In some cases, particularly after prostate surgery, physiotherapists may help patients with pelvic floor exercises to regain urinary control.
- Dietitians and Nutritionists: While not directly involved in the medical diagnosis, they can provide guidance on dietary choices that may support overall health or help manage side effects of treatments.
Proactive Prostate Health: Understanding Risk Factors and Prevention
While specific doctors are responsible for checking the prostate, maintaining its health is a continuous effort that involves understanding risk factors and adopting preventive measures.
Modifiable Risk Factors and Lifestyle Choices
Certain lifestyle choices can significantly impact prostate health:
- Diet: A diet rich in fruits, vegetables, and whole grains, and low in red meat and processed foods, is generally beneficial for overall health, including prostate health. Some studies suggest that foods high in lycopene (like tomatoes) and selenium may offer protective benefits, though more research is needed.
- Weight Management: Maintaining a healthy weight through diet and exercise can reduce the risk of various health problems, including potentially aggressive prostate cancer.
- Exercise: Regular physical activity is associated with better overall health and may play a role in preventing certain cancers.
- Smoking and Alcohol: Limiting alcohol intake and avoiding smoking are crucial for general well-being and can contribute to better prostate health.
Non-Modifiable Risk Factors and Regular Screening
Some risk factors cannot be changed, making regular medical check-ups even more important:
- Age: The risk of prostate problems, including cancer, increases significantly with age, particularly after 50.
- Family History: A family history of prostate cancer (especially in a father or brother) increases a man’s risk.
- Ethnicity: African American men have a higher risk of developing prostate cancer and are more likely to develop it at a younger age and in a more aggressive form.
The role of regular screening, as discussed with a GP and potentially a urologist, becomes paramount for individuals with these risk factors. Early detection through methods like the PSA test and DRE, followed by specialized urological assessment, significantly improves the chances of successful treatment and positive outcomes.
In conclusion, the question “What doctor checks prostate?” leads us to the dedicated expertise of the urologist. However, it also highlights the integrated nature of healthcare, where general practitioners serve as crucial gatekeepers, and a team of allied health professionals supports comprehensive patient care. By understanding these roles and actively participating in proactive health management, men can navigate their prostate health journey with confidence and ensure timely access to the specialized medical attention they may need.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.