In the rapidly evolving landscape of medical technology, we often focus on the “visible” hardware: the robotic surgical arms, the high-resolution MRI machines, and the wearable sensors that track our every heartbeat. However, some of the most profound technological advancements occur at the molecular level. When we examine what cortisone shots do, we aren’t just looking at a simple medical procedure; we are looking at a sophisticated biological intervention designed to “reprogram” a localized environment within the human body.
In the world of Bio-Tech and MedTech, cortisone (a synthetic version of the hormone cortisol) represents one of the earliest and most successful examples of chemical engineering used to override natural systemic responses. This article explores the technological sophistication behind these injections, the high-tech guidance systems used to administer them, and the future of precision-targeted anti-inflammatory delivery.
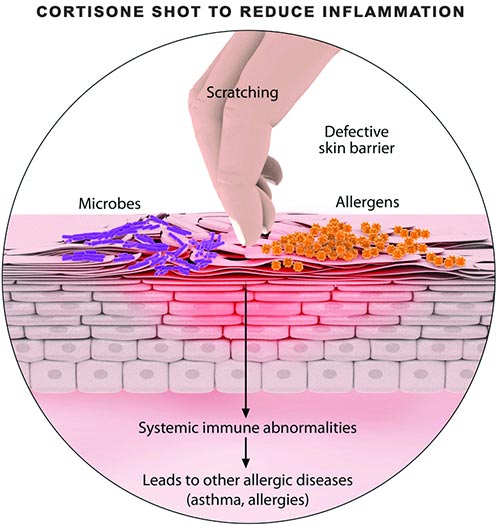
The Molecular Engineering of Inflammation Control
At its core, a cortisone shot is a piece of biological “software” designed to interact with the human body’s complex signaling pathways. While the general public views it as a simple pain reliever, the tech behind it is far more complex. It is a synthetic corticosteroid engineered to mimic the behavior of the adrenal glands but at a much higher, localized concentration.
Synthetic Corticosteroids: A Masterclass in Molecular Design
Natural cortisol is a hormone that regulates a vast array of processes, from metabolism to immune response. However, natural cortisol is metabolized quickly by the body. To create a viable medical tool, biotechnologists had to re-engineer the molecular structure of these hormones to create synthetic versions like triamcinolone, methylprednisolone, and betamethasone.
These synthetic variants are designed for “persistence.” By altering the chemical bonds of the molecule, scientists created a substance that the body cannot break down immediately. This allows the “tech” to remain at the site of the injection—whether it be a knee joint or a bursa—providing sustained suppression of the immune system’s inflammatory signals. This is effectively a “targeted system override” that prevents the body’s hardware (the joints and tendons) from being damaged by its own software (the immune response).
Disrupting the Inflammatory Algorithm
Inflammation is essentially an algorithmic response to perceived damage. When a tissue is injured, the body initiates a cascade of chemical signals—cytokines, prostaglandins, and leukotrienes—that lead to swelling and pain. Cortisone acts as a “firewall.”
Once injected, the cortisone molecules pass through cell membranes and bind to glucocorticoid receptors. This complex then enters the cell nucleus and alters gene expression. In tech terms, it “mutes” the genes responsible for producing pro-inflammatory proteins and “upregulates” the genes that produce anti-inflammatory ones. By changing the transcriptional output of the cell, cortisone shots provide a deep-level system reset to the affected area.
Guided Precision: The Hardware Behind the Needle
The efficacy of the cortisone “software” is entirely dependent on the precision of the delivery “hardware.” Historically, injections were performed “blind,” relying on an anatomical understanding of “surface landmarks.” However, modern MedTech has moved toward high-precision, image-guided delivery systems that ensure the needle reaches the exact millimetre required for maximum impact.
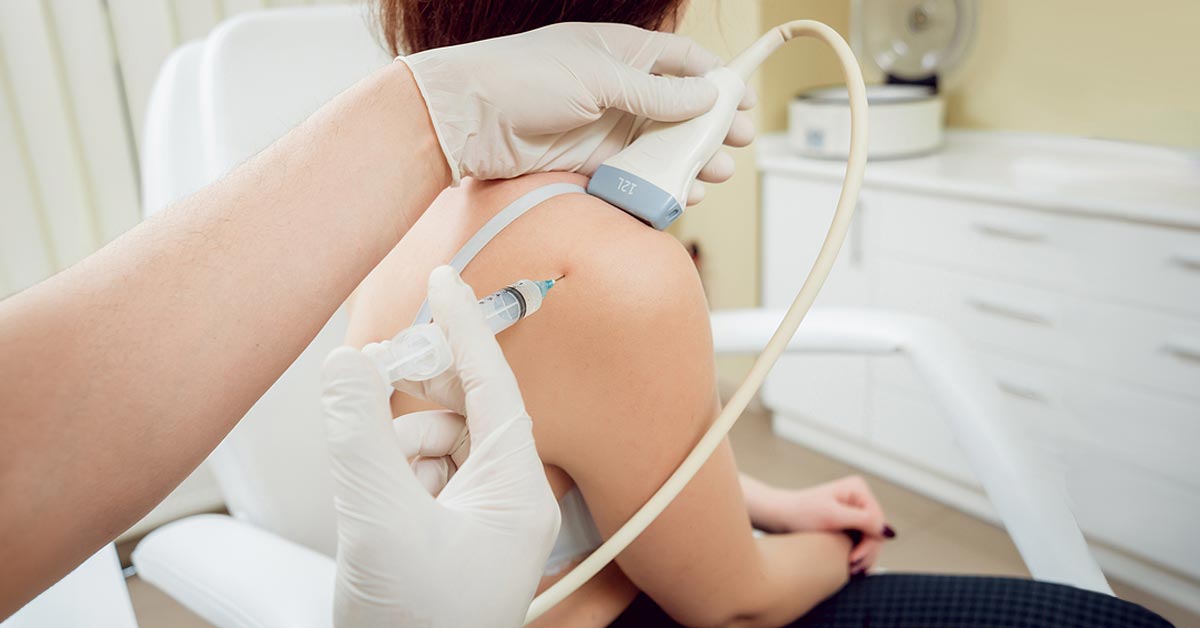
Ultrasound-Guided Visualization: High-Resolution Diagnostics
One of the most significant tech trends in orthopedics is the shift toward ultrasound-guided injections. This involves using high-frequency sound waves to create real-time, high-resolution images of the internal anatomy.
When a specialist uses an ultrasound machine to deliver a cortisone shot, they aren’t just guessing. They are watching the needle tip move through the subcutaneous tissue, past blood vessels and nerves, and directly into the target space—such as the subacromial space in a shoulder or the intra-articular space of a hip. This level of visualization reduces the “margin of error” significantly. Research in medical technology journals suggests that ultrasound-guided injections have a much higher success rate in symptom relief compared to landmark-guided techniques because the “payload” is delivered with surgical accuracy.
Robotic Assistance and AI-Driven Injection Mapping
Looking toward the cutting edge of the Tech niche, we are seeing the emergence of robotic-assisted injection systems. These tools utilize AI to map the patient’s unique anatomy based on pre-procedure scans (CT or MRI). The robotic arm can then stabilize the needle and guide it along a pre-calculated path.
This is particularly useful in spinal injections (epidural steroid injections), where the target zone is incredibly small and surrounded by critical neurological structures. The integration of AI and haptic feedback technology ensures that the physician can feel resistance changes at a level of sensitivity that the human hand cannot detect alone, making “what cortisone shots do” safer and more predictable than ever before.
The Nanotech Frontier: Next-Gen Cortisone Delivery
As we look at the future of biotechnology, the focus is shifting from what is being injected to how it is being packaged. Standard cortisone shots are “bolus” deliveries—the entire dose is released at once. The next evolution of this technology involves nanotechnology and smart materials.
Nanoparticle Carriers and Targeted Bio-Payloads
One of the primary drawbacks of traditional cortisone shots is systemic absorption. Even when injected locally, some of the steroid enters the bloodstream, potentially causing side effects like blood sugar spikes or bone density issues.
Enter Nanomedicine. Tech researchers are currently developing nanoparticle carriers for corticosteroids. These are microscopic “capsules” that can be engineered to only release their payload when they encounter specific biological triggers, such as a certain pH level or a specific enzyme present in inflamed tissue. By “coding” the delivery vehicle to react only to the inflammation, the tech ensures that the drug stays where it is needed, increasing the “signal-to-noise” ratio of the treatment.
Smart Hydrogels: The “Software” of Sustained Release
Another breakthrough in delivery tech is the use of injectable hydrogels. Instead of a liquid solution, the cortisone is embedded in a synthetic polymer matrix. Once injected, this hydrogel acts like a slow-release battery.
As the hydrogel slowly biodegrades over weeks or months, it releases a steady, metered dose of the steroid. This avoids the “peak and trough” effect of traditional shots, where the patient feels great for two weeks and then the pain returns. This “sustained-release tech” represents a shift from reactive medicine to proactive, long-term environmental management within the joint.
Digital Health Integration: Monitoring Recovery via Wearables and IoT
In the modern tech ecosystem, a medical procedure doesn’t end when the patient leaves the clinic. The integration of the Internet of Things (IoT) and wearable technology is changing how we quantify “what cortisone shots do.”
Wearable Integration for Bio-Feedback
Post-injection recovery is now being tracked through sophisticated motion analytics. Patients wearing smartwatches or specialized orthopedic sensors can provide doctors with real-time data on their range of motion, step count, and gait symmetry following a cortisone shot.
This “closed-loop” system allows healthcare providers to see the actual “output” of the intervention. If the data shows that a patient’s mobility hasn’t improved despite the injection, the “system” (the medical team) can pivot to a different treatment faster. This move toward “Quantified Health” ensures that cortisone shots are treated as a data-backed solution rather than a subjective trial-and-error process.
Telehealth and Remote Monitoring of Pharmacological Impact
Furthermore, digital platforms now allow for the remote monitoring of side effects. Mobile apps can prompt patients to log their pain levels and glucose readings (for diabetics) in the days following the procedure. This data is fed into algorithms that can flag potential adverse reactions before they become emergencies. This digital security layer adds a new dimension to the safety profile of corticosteroid treatments, proving that the “Tech” category encompasses not just the drug itself, but the entire digital infrastructure surrounding the patient’s journey.

Conclusion: The Synergy of Biology and Technology
When we ask what cortisone shots do, we find an answer that lies at the intersection of advanced biochemistry, precision imaging, and digital monitoring. These injections are not merely “anti-inflammatory shots”; they are sophisticated tools of biological engineering that have been refined over decades of technological progress.
From the synthetic “reprogramming” of cellular DNA to the AI-guided precision of the needle, and the future of nanomedicine “payloads,” cortisone treatments are a testament to how far MedTech has come. As we move forward, the “Tech” behind pain management will continue to become more precise, more data-driven, and more integrated into our digital lives, ensuring that we aren’t just masking symptoms, but intelligently managing the complex hardware of the human body.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.