In the rapidly evolving landscape of health technology, the traditional boundaries between medical diagnostics and consumer electronics are blurring. For decades, the question of “what are normal blood sugar levels 2 hours after eating” was a query reserved for a doctor’s office or a manual logbook. Today, that data point has become a pillar of the “Quantified Self” movement, powered by sophisticated wearable sensors, artificial intelligence, and cloud-based analytics. As we move toward a future of proactive wellness, understanding the technology behind metabolic monitoring is essential for tech enthusiasts and health-conscious innovators alike.

The Digital Evolution of Metabolic Monitoring
The shift from reactive healthcare to proactive bio-monitoring has been driven by significant leaps in hardware engineering. Historically, checking blood sugar levels required a glucose meter and a painful finger-prick lancet, providing only a single “snapshot” in time. In the tech world, this is equivalent to trying to understand a movie by looking at one still frame.
Beyond the Finger Prick: The Rise of CGMs
Continuous Glucose Monitors (CGMs) represent one of the most significant breakthroughs in medical IoT (Internet of Things). These devices, such as those developed by industry leaders like Dexcom and Abbott, utilize a tiny filament inserted under the skin. This filament measures glucose levels in the interstitial fluid every few minutes, transmitting that data wirelessly via Bluetooth to a smartphone or smartwatch.
From a technical perspective, CGMs have transitioned from bulky medical equipment to sleek, low-profile wearables. The engineering challenge involved minimizing the electrochemical sensor while maintaining a battery life that lasts 10 to 14 days. These devices now utilize sophisticated algorithms to filter “noise” from the sensor, ensuring that the data displayed on the user’s screen is both accurate and actionable.
Integrating Real-Time Data into the Digital Ecosystem
The true power of modern glucose monitoring lies in its integration with the broader digital ecosystem. We are no longer looking at an isolated device; we are looking at a node in a massive data network. Through APIs and HealthKit integrations, blood sugar data can now be layered with sleep data from an Oura ring, heart rate variability (HRV) from an Apple Watch, and caloric intake from apps like MyFitnessPal.
This convergence allows for a holistic view of human biology. For tech developers, the challenge is no longer just collecting data, but synthesizing it. When a user asks what their level should be two hours after a meal, the software doesn’t just provide a static number; it provides context based on their activity levels, stress markers, and historical data patterns.
Defining the “Normal” Range through Algorithmic Precision
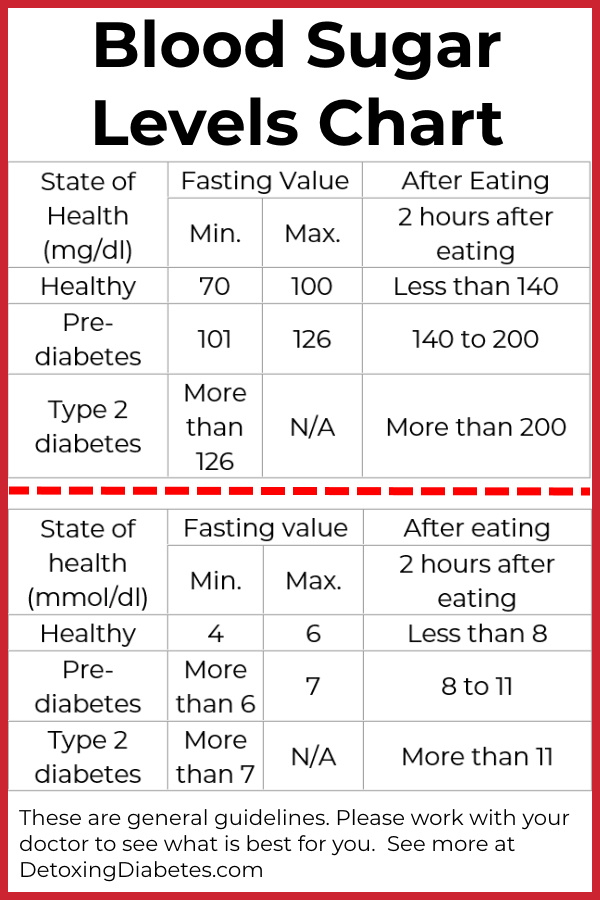
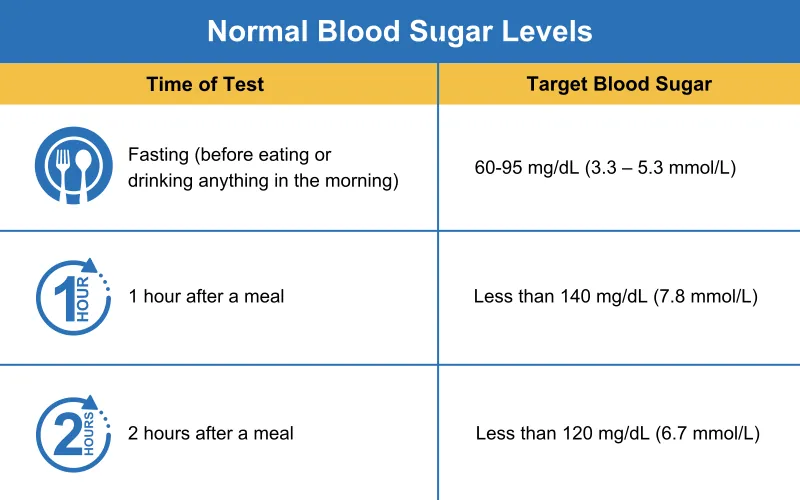
In clinical terms, a “normal” blood sugar level two hours after eating (post-prandial) is generally considered to be less than 140 mg/dL (7.8 mmol/L). However, the tech industry is redefining these benchmarks through the lens of “Personalized Glycemic Responses.”
2 Hours Post-Prandial: The Tech Behind the Metric
Why is the two-hour mark so critical in the digital health space? From a data science perspective, the two-hour window represents the “peak and recovery” phase of the metabolic curve. By analyzing how quickly a user’s glucose levels return to baseline after a spike, algorithms can determine insulin sensitivity and metabolic flexibility.
Advanced health apps use machine learning to categorize these curves. A “flat” curve indicates high metabolic efficiency, while a “jagged” curve—even if it stays within the 140 mg/dL limit—might signal underlying issues that a simple snapshot would miss. The software identifies the “Area Under the Curve” (AUC), a metric far more valuable to a data-driven health regimen than a single numerical value.
AI and Personalized Glycemic Responses
One of the most exciting frontiers in HealthTech is the use of Artificial Intelligence to predict glucose spikes before they happen. Companies like Nutrisense and Levels are leveraging AI to analyze how different individuals react to the same foods.
For example, two users might eat the same banana; one might stay at a steady 110 mg/dL, while the other spikes to 160 mg/dL. The technology analyzes the user’s unique microbiome data, genetic markers, and historical trends to provide a “Stability Score.” This moves the conversation away from generic medical charts and toward a personalized digital twin of the user’s metabolism.
The Intersection of Wearables and Preventative Software
As we look toward the next generation of gadgets, the integration of non-invasive glucose monitoring is the “Holy Grail” of the tech industry. Rumors regarding the integration of such sensors into the Apple Watch or Samsung Galaxy Watch have persisted for years, highlighting the massive engineering hurdle of measuring blood chemistry through the skin without a needle.
Smartwatch Integration and the Internet of Medical Things (IoMT)
The Internet of Medical Things (IoMT) is an infrastructure of health-focused devices and applications that connect to healthcare IT systems. Current technology relies on NFC (Near Field Communication) and Bluetooth Low Energy (BLE) to sync data. However, the future lies in “transdermal optical sensing”—using infrared lasers to measure glucose molecules.
If successful, this would move blood sugar tracking from a niche tool for diabetics to a standard feature for every consumer. The technical complexity lies in the “Signal-to-Noise” ratio; glucose is difficult to distinguish from other molecules in the blood using light alone. Solving this requires incredibly powerful edge computing and sophisticated signal-processing algorithms.
Data Security in Bio-Metric Tracking
With the rise of 24/7 metabolic tracking comes the critical issue of digital security. Blood sugar levels are highly sensitive biometric data. If a hacker gains access to a user’s metabolic history, they have a window into that person’s chronic health risks, diet, and lifestyle habits.
Tech firms are responding by implementing end-to-end encryption and decentralized data storage solutions. As HealthTech becomes more prevalent, the adoption of “Zero Knowledge Proofs” in data sharing will be essential. This allows a user to prove they have “normal” blood sugar levels (perhaps for an insurance discount) without actually revealing their raw glucose data to the third party.
Designing the Future: UX and UI in Glucose Management Apps
Data is only useful if it is understood. The design philosophy of modern health apps has shifted from “clinical and sterile” to “engaging and intuitive.” The User Interface (UI) plays a vital role in how people interact with their blood sugar levels throughout the day.
Gamification of Metabolic Health
To keep users engaged with their “2 hours after eating” metrics, developers are turning to gamification. By assigning a “Zone Score” or “Daily Metabolic Grade,” apps encourage users to keep their glucose levels stable. This uses psychological triggers similar to those found in fitness trackers that encourage “closing your rings.”
The User Experience (UX) focuses on reducing “alert fatigue.” If a CGM pings a user every time their sugar moves, the user will eventually ignore it or turn it off. Smart software now uses predictive analytics to only alert the user if a trend is outside of their personalized “normal” range, making the technology a silent partner rather than a constant nuisance.
The Role of Predictive Analytics
The next step in the software evolution is moving from descriptive analytics (“Your sugar is 130”) to prescriptive analytics (“Your sugar is rising; walk for 10 minutes to stabilize it”). By utilizing the smartphone’s accelerometer and GPS, the app can detect when a user has finished a meal and suggest a “glucose disposal” activity.
This level of tech-human interaction represents the pinnacle of modern software design. It transforms a biological metric—the 2-hour post-meal glucose level—into a real-time coaching opportunity. The software becomes an external pre-frontal cortex, helping the user make better decisions in the moment based on complex biological data.
Conclusion: The New Standard of Digital Wellness
The question “what are normal blood sugar levels 2 hours after eating” is no longer just a medical query; it is a data point at the center of a technological revolution. Through the advancement of CGM hardware, the power of AI-driven personalization, and the integration of the Internet of Medical Things, we are entering an era where our devices know our bodies better than we do.
For the tech industry, the challenge lies in miniaturization, non-invasive sensing, and robust data privacy. For the consumer, the benefit is an unprecedented level of control over their own biology. As we continue to refine these tools, the “normal” range will become less of a static number on a page and more of a dynamic, personalized target achieved through the seamless partnership of human biology and high-tech innovation. Whether through a patch on the arm or a sensor on the wrist, the future of health is digital, data-driven, and deep within the code.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.