In the rapidly evolving landscape of medical technology (MedTech), the miniaturization of surgical devices has become a cornerstone of patient-centric innovation. Among the most significant advancements in the dental sector is the development and refinement of mini dental implants (MDIs). Once considered a secondary alternative to traditional restorative hardware, mini implants now represent a sophisticated intersection of material science, precision engineering, and digital diagnostic workflows. This article explores the technical architecture of mini implants, the digital technologies that facilitate their placement, and the future of minimally invasive prosthetic integration.
The Engineering Behind the Miniaturization of Dental Implants
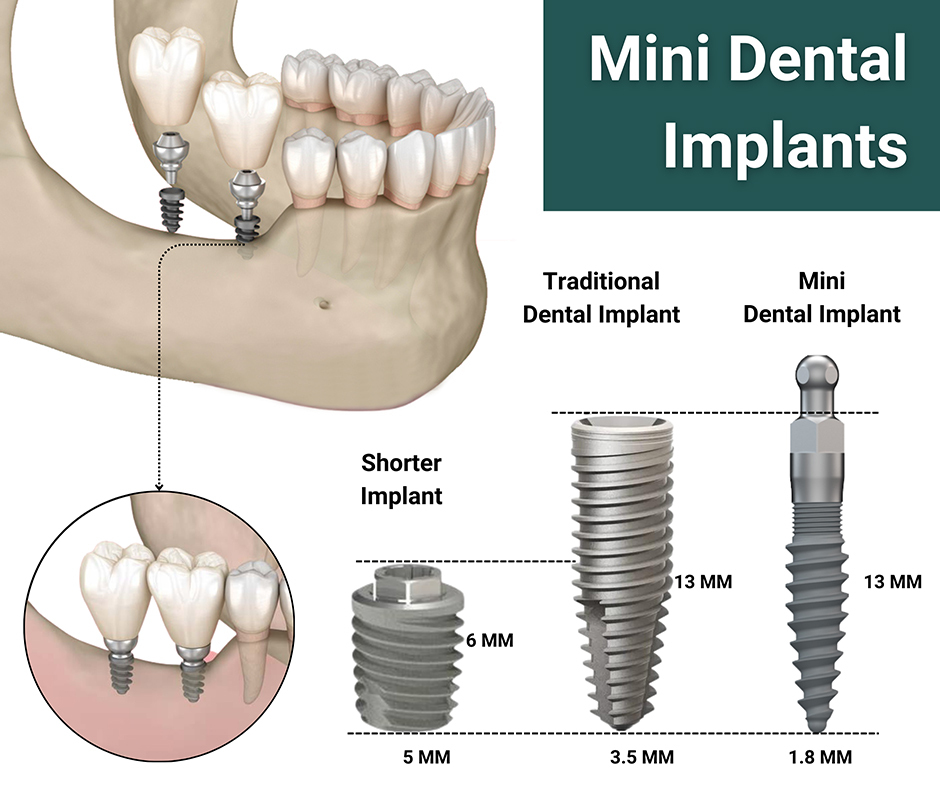
The transition from traditional dental implants to mini implants is not merely a reduction in size; it is a fundamental shift in mechanical engineering and structural design. Standard implants typically range from 3.4 to 5.8 millimeters in diameter, whereas mini implants are engineered with a diameter of less than 3 millimeters—usually hovering between 1.8 and 2.9 millimeters.
Material Science: Titanium Alloys and Surface Texturing
At the heart of mini implant technology is the use of high-grade titanium alloys. Most MDIs are fabricated from Grade 5 Titanium (Ti-6Al-4V), which offers a higher tensile strength than the pure titanium often used in larger implants. This is a critical technological requirement; because the device is thinner, the metal must be significantly more resilient to withstand the mechanical stresses of mastication (chewing).
Furthermore, the “tech” of the implant extends to its surface. Manufacturers utilize Acid-Etching and Sandblasted, Large-grit, Acid-etched (SLA) technologies to create a micro-porous surface at the molecular level. This topographical engineering increases the surface area for osseointegration—the biological process where bone cells fuse with the titanium hardware. By optimizing the surface texture through chemical engineering, mini implants can achieve high stability despite their reduced physical footprint.
Structural Differences: One-Piece vs. Modular Design
Technologically, the most distinct feature of a mini implant is its “monoblock” or one-piece construction. Traditional implants are modular, consisting of the implant body, an internal screw, and a separate abutment. The mini implant integrates the screw and the abutment into a single solid unit.
This design choice eliminates the “micro-gap” found in modular systems, which can sometimes harbor bacteria or suffer from screw loosening. From a mechanical perspective, the one-piece design simplifies the distribution of force, allowing the slim device to act as a singular, robust anchor within the alveolar bone.
The Digital Workflow: Tech-Driven Placement and Precision
The success of mini implants is heavily dependent on the digital ecosystem that surrounds modern dentistry. The precision required to place a 2-millimeter post into a narrow ridge of bone leaves zero room for manual error. Consequently, the procedure has become a showcase for advanced imaging and AI-assisted planning.
3D Imaging and CBCT Scanning
The primary technological prerequisite for mini implant placement is Cone Beam Computed Tomography (CBCT). Unlike traditional 2D X-rays, CBCT scans provide a high-resolution 3D rendering of the patient’s craniofacial structure. This allows practitioners to analyze bone density and volume with sub-millimeter accuracy.
Software suites integrated with CBCT hardware enable “virtual surgery,” where the technician can simulate the placement of the mini implant to avoid nerve canals and sinus cavities. This digital mapping ensures that the implant is positioned in the “corridor of bone” that provides the highest primary stability, a process dictated entirely by data rather than visual estimation.
Computer-Guided Surgery and CAD/CAM
The integration of Computer-Aided Design and Computer-Aided Manufacturing (CAD/CAM) has revolutionized the application of mini implants. Once the virtual plan is finalized in the software, a physical surgical guide is 3D-printed. This guide fits over the patient’s teeth or gums, featuring precision-drilled holes that dictate the exact angle, depth, and position of the mini implant.

By utilizing this “GPS for the mouth,” the technology allows for flapless surgery—where the implant is placed directly through the soft tissue without the need for incisions or sutures. This is a hallmark of minimally invasive MedTech, reducing recovery times and post-operative complications through sheer digital precision.
Comparing High-Tech Solutions: Mini vs. Traditional Implants
When evaluating the technological merits of mini implants, it is essential to compare their mechanical behavior and integration protocols with their full-sized counterparts. The choice between the two often comes down to the “biological real estate” available and the specific load-bearing requirements of the prosthetic.
Load-Bearing Mechanics and Stress Distribution
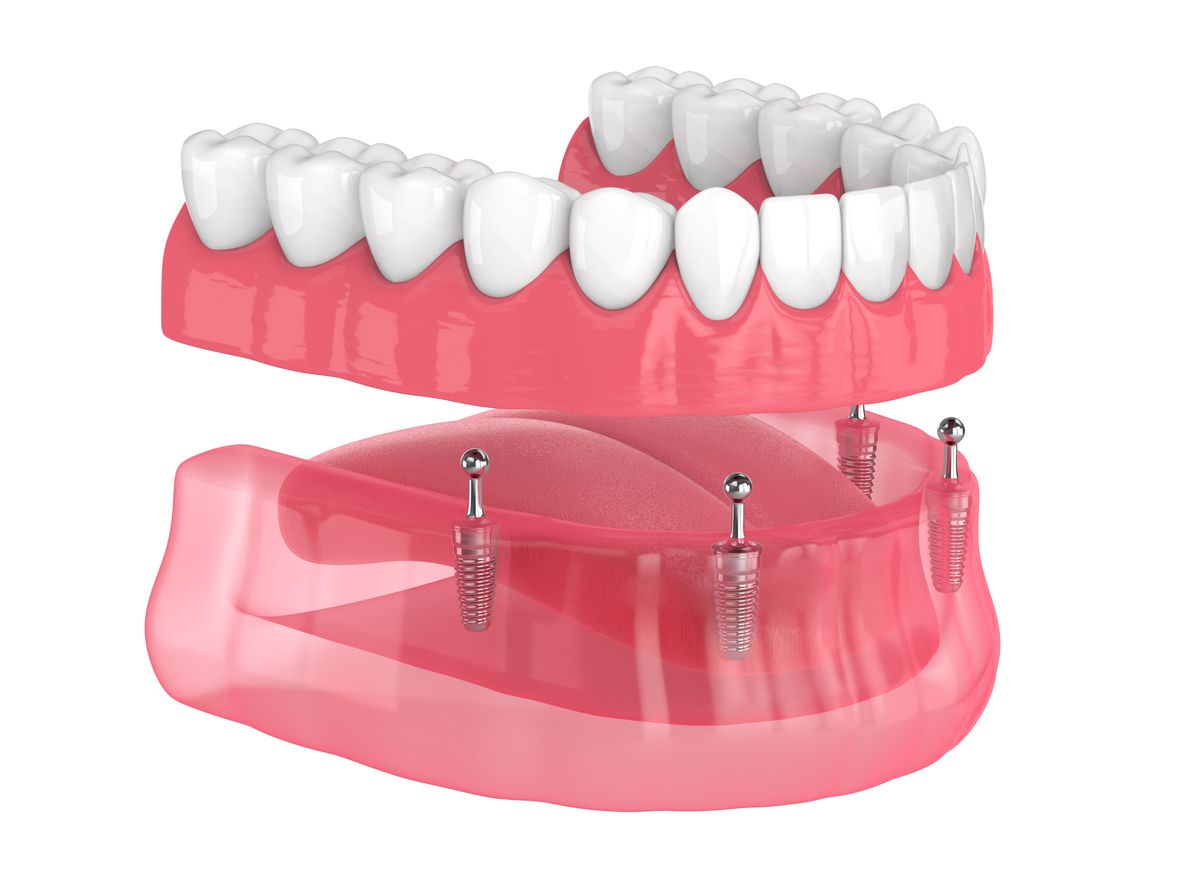
From a physics perspective, a thinner implant changes how force is transmitted to the jawbone. Traditional implants rely on a larger surface area to dissipate the pressure of biting. Mini implants, due to their slim profile, are often utilized in “multi-unit” configurations. For example, instead of two large implants supporting a bridge, four or five mini implants might be used to distribute the load more evenly across a wider section of bone.
This technological strategy is particularly useful for patients with bone atrophy. In cases where the jawbone has thinned, there isn’t enough space for a traditional 4mm wide screw. The mini implant’s technology allows for a “bone-conservative” approach, navigating narrow anatomical spaces that were previously untreatable without extensive bone grafting surgery.
Osseointegration and Immediate Loading Protocols
One of the most significant technological advantages of the mini implant is the capability for “immediate loading.” Because of the thread design and the way the one-piece titanium body interacts with the bone, mini implants often achieve high primary stability immediately upon insertion.
In many digital workflows, the prosthetic (such as a denture or crown) can be attached to the mini implant on the same day it is placed. This is a massive leap over traditional protocols, which often require a 3-to-6-month healing period before the hardware can support any weight. The specialized thread patterns on MDIs are engineered to compress the bone as they are inserted, creating a mechanical “lock” that facilitates this rapid functional transition.
The Future Landscape of Minimally Invasive MedTech
As we look toward the next decade, mini implant technology is poised to integrate even more deeply with emerging fields such as biotechnology and robotics. The trend is moving toward “smart” hardware that does more than just sit in the bone; it actively monitors and promotes health.
Smart Implants and Bio-Sensor Integration
The next frontier for mini implants involves the integration of micro-sensors. Research is currently underway into implants equipped with biosensors that can monitor local pH levels, temperature, and pressure. Such a device could theoretically alert a patient or doctor to the early signs of infection (peri-implantitis) or mechanical failure long before symptoms become visible. This shift from reactive to proactive monitoring represents the pinnacle of “Smart MedTech.”
3D Printing and Personalized Metallurgy
While most mini implants today are mass-produced in specific sizes, the future lies in personalized 3D-printed titanium implants. Using Direct Metal Laser Sintering (DMLS), it may soon be possible to print a mini implant that perfectly matches the unique internal architecture of a specific patient’s bone, as identified by their CBCT scan. This would allow for an even more conservative approach, as the hardware would be custom-engineered for the specific density and shape of the host site.
Robotics and Automated Placement
The intersection of mini implants and robotics is also expanding. Robotic-assisted surgical arms, such as the Yomi system, are already being used to assist in standard implant placement. As these robotic tools become more refined, their application in the delicate, high-precision placement of mini implants will likely become the gold standard. These systems can compensate for even the slightest patient movement in real-time, ensuring that the technology of the mini implant is backed by the highest possible level of procedural accuracy.
Conclusion
Mini implants represent a significant milestone in the technological evolution of restorative medicine. By leveraging advancements in Grade 5 titanium alloys, 3D digital imaging, and CAD/CAM manufacturing, these devices provide a high-tech solution for complex anatomical challenges. While their size is “mini,” their impact on the field of medical technology is immense, offering a glimpse into a future where surgical interventions are increasingly precise, minimally invasive, and digitally integrated. As the industry moves toward smart sensors and personalized 3D printing, the mini implant will remain at the forefront of the digital transformation of healthcare.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.