In the era of the “Quantified Self,” the quest for optimal health has moved from the doctor’s office into the palm of our hands. For decades, the definition of “perfect” blood pressure was a static snapshot taken once a year during a physical examination. However, as technology evolves, our understanding of what constitutes ideal cardiovascular health is being redefined by high-precision sensors, artificial intelligence, and real-time data analytics.
Today, perfect blood pressure is no longer just a single set of numbers (120/80 mmHg); it is a dynamic range monitored through sophisticated digital ecosystems. This article explores the intersection of medical science and cutting-edge technology to answer what perfect blood pressure is and how modern tech is helping us achieve and maintain it.
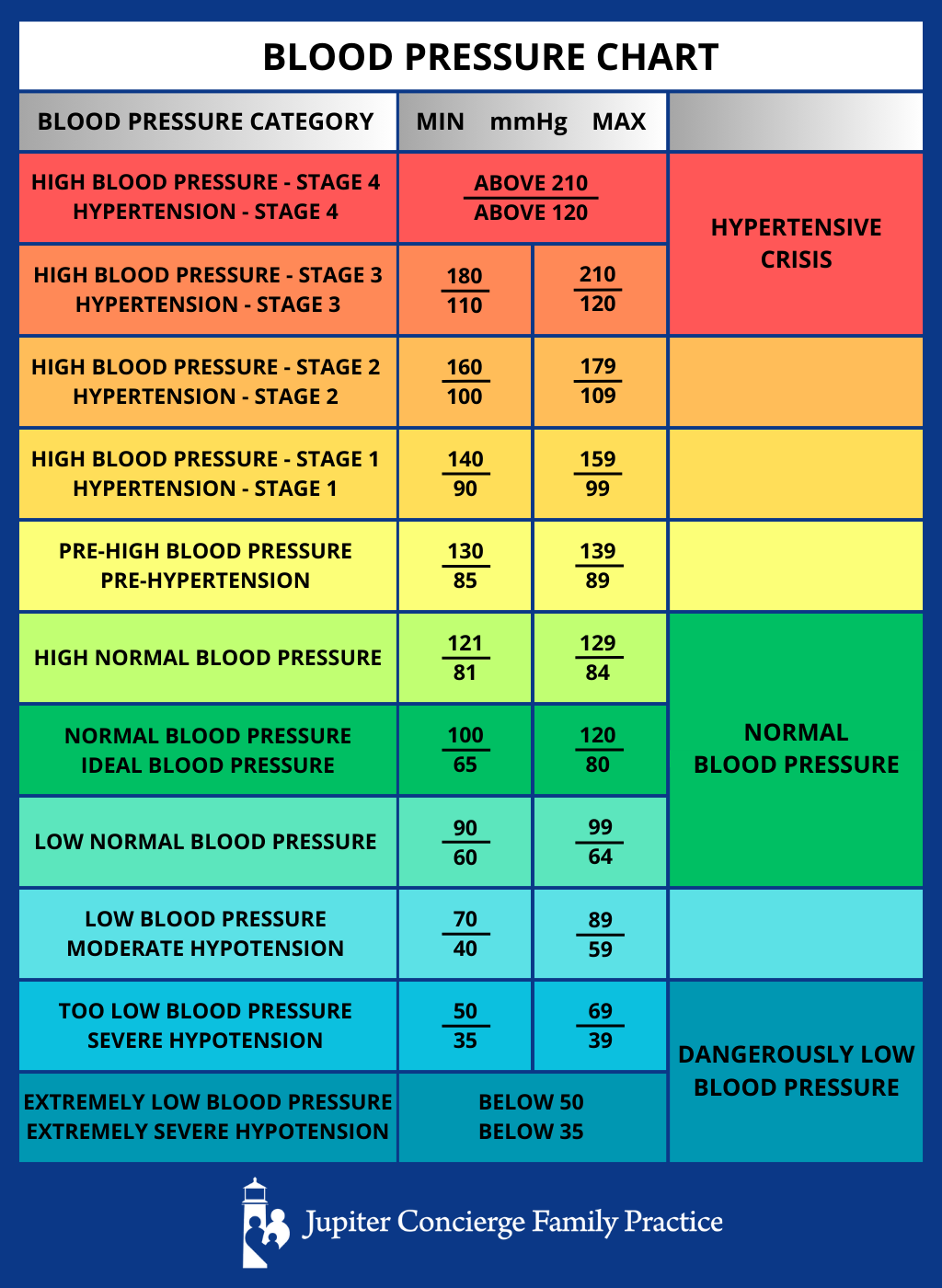
Defining the “Perfect” Metric in the Age of Digital Diagnostics
To understand “perfect” blood pressure, we must first look at the traditional benchmarks and how technology has increased the resolution of these figures. The American Heart Association and the American College of Cardiology currently define “normal” blood pressure as less than 120/80 mmHg. But what does this mean in a world where we can track our vitals 24/7?
From Mercury Sphygmomanometers to Smart Sensors
For over a century, the gold standard for measuring blood pressure was the mercury sphygmomanometer. While accurate, it provided only a momentary glimpse into a patient’s cardiovascular state. The “perfect” reading in a clinical setting was often skewed by “White Coat Syndrome”—a phenomenon where a patient’s blood pressure spikes due to the anxiety of being in a medical environment.
Modern health tech has solved this by moving toward ambulatory and home monitoring. Digital oscillometric monitors and wearable sensors allow for “Perfect Blood Pressure” to be defined by an average of readings over time, providing a much more accurate representation of a person’s true vascular health than a single high-stress clinic visit.
The 120/80 Benchmark and Data Granularity
While 120/80 mmHg remains the target, technology has introduced the concept of “Blood Pressure Variability” (BPV). Digital health platforms now analyze the fluctuations in your pressure throughout the day. A “perfect” profile in the eyes of modern software isn’t just about hitting 120/80 at noon; it’s about how quickly your pressure recovers after exercise and how low it stays during deep sleep (nocturnal dipping). Tech tools have shifted the goalpost from a static number to a healthy, responsive curve.
Wearable Tech: Real-Time Monitoring and the Shift from Snapshots to Trends
The wearable technology market has exploded, transitioning from simple step counters to sophisticated diagnostic tools. For blood pressure, this represents a massive leap in how we maintain “perfect” levels.
PPG vs. Oscillometric Measurements in Consumer Tech
Most traditional blood pressure cuffs use the oscillometric method, which involves inflating a cuff to restrict blood flow and then measuring the vibrations of the arterial wall as the pressure is released. While accurate, this is bulky and inconvenient for continuous monitoring.
Enter Photoplethysmography (PPG). This is the technology found in the green and red lights on the back of your smartwatch. By shining light into the skin and measuring how it scatters off the blood flow, advanced algorithms can now estimate blood pressure. Companies like Samsung and various specialized med-tech startups are refining PPG to provide cuffless, continuous monitoring. The “perfect” blood pressure is easier to maintain when you have a haptic alert on your wrist telling you when your levels are creeping into the “elevated” zone.
Predictive Analytics: Identifying Hypertension Before It Happens
The most significant advantage of integrating tech into blood pressure management is the move from reactive to proactive care. High-end wearables and connected apps use predictive analytics to spot trends. If your blood pressure is consistently 5% higher on Tuesdays, the software can correlate that data with your digital calendar, identifying high-stress meetings or lack of sleep as the culprit. This level of insight allows users to make lifestyle adjustments in real-time to return to that “perfect” 120/80 range before clinical hypertension ever develops.

AI and Machine Learning: Personalizing the Definition of “Normal”
One of the biggest critiques of the “120/80” rule is that it is a one-size-fits-all metric. However, Artificial Intelligence (AI) is beginning to personalize what “perfect” blood pressure looks like for an individual based on their unique biological profile.
Beyond the One-Size-Fits-All Model
AI algorithms can process vast amounts of data—including age, weight, genetic markers, and historical activity levels—to determine a personalized “optimal” blood pressure range. For a 25-year-old marathon runner, “perfect” might be 105/70 mmHg, whereas for a 70-year-old with specific arterial conditions, a slightly higher systolic pressure might be considered healthy by their AI-driven management app.
By using machine learning, health platforms can filter out “noise” (like a temporary spike from a cup of coffee) and focus on the underlying health of the vascular system. This prevents unnecessary medical intervention and focuses on long-term wellness.
Integrating Lifestyle Data into Clinical Outcomes
The “Internet of Medical Things” (IoMT) allows blood pressure monitors to sync with smart scales, diet-tracking apps, and sleep monitors. When these data points are fed into an AI engine, it creates a holistic view of cardiovascular health. Achieving perfect blood pressure becomes a gamified experience: the software shows you exactly how much your pressure drops after a 10-minute meditation session or a reduction in sodium intake, providing immediate positive reinforcement through data visualization.
The Future of Blood Pressure Tech: Non-Invasive and Ambient Sensing
We are standing on the brink of a revolution in how we interact with our cardiovascular data. The future of maintaining perfect blood pressure lies in technology that is so seamless it becomes invisible.
Transdermal Optical Imaging and Smartphone-Based Assessments
One of the most exciting frontiers in health tech is Transdermal Optical Imaging. Researchers are developing software that can measure blood pressure simply by analyzing a 30-second “video selfie” on a smartphone. The camera detects minute changes in facial blood flow that are invisible to the human eye. This tech would make checking for perfect blood pressure as easy as checking a social media notification, removing the “friction” of health monitoring and making cardiovascular awareness a daily habit for billions of people.
The Intersection of Digital Security and Health Data Privacy
As our blood pressure data moves from a paper file in a doctor’s office to the cloud, the “tech” side of health becomes a matter of security. Maintaining a perfect blood pressure profile also requires maintaining a “perfect” digital security posture.
The integration of blockchain technology is being explored to allow patients to own their cardiovascular data securely. This ensures that while your smartwatch and AI coach help you maintain your 120/80 target, your sensitive health metrics are encrypted and accessible only to you and your authorized healthcare providers. As we rely more on AI to tell us if our pressure is “perfect,” the integrity of the data becomes as important as the numbers themselves.

Conclusion: Perfection Through Precision
In summary, “perfect” blood pressure is no longer a static goal of 120/80 mmHg captured once a year. In the tech-driven landscape of the 21st century, perfection is defined by stability, trend analysis, and personalization.
Through the use of wearable sensors, PPG technology, and AI-driven analytics, we have moved into an era of precision medicine. We now have the tools not only to define what perfect blood pressure looks like for our specific bodies but to monitor it in real-time, predict deviations before they become dangerous, and use data-driven insights to live longer, healthier lives. As technology continues to shrink the gap between the human body and digital diagnostics, the path to perfect cardiovascular health has never been clearer.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.