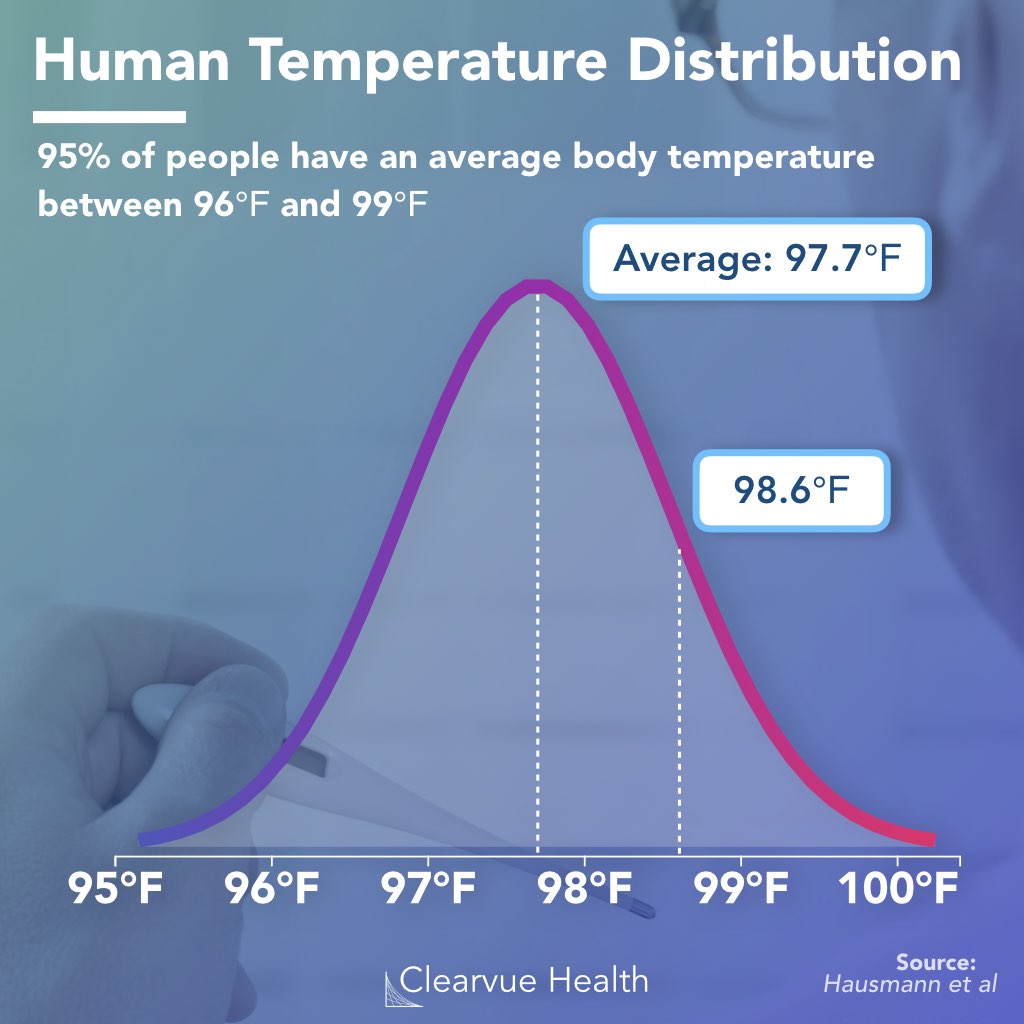
For over 150 years, the global standard for a “normal” human body temperature has been fixed at 98.6°F (37°C). Established by German physician Carl Wunderlich in 1851, this figure became a cornerstone of medical diagnostics. However, as we move deeper into the era of high-precision health technology, the tech industry is challenging this static number. Through the lens of wearable sensors, artificial intelligence, and big data analytics, we are discovering that “normal” is not a single point on a scale, but a dynamic, individualized data range.
In the modern technological landscape, temperature is no longer just a vital sign recorded during a doctor’s visit; it is a continuous stream of data points that provide a window into human biology. This article explores how emerging technologies are redefining our understanding of human temperature, the hardware driving this revolution, and the software infrastructures that transform raw thermal data into actionable health insights.
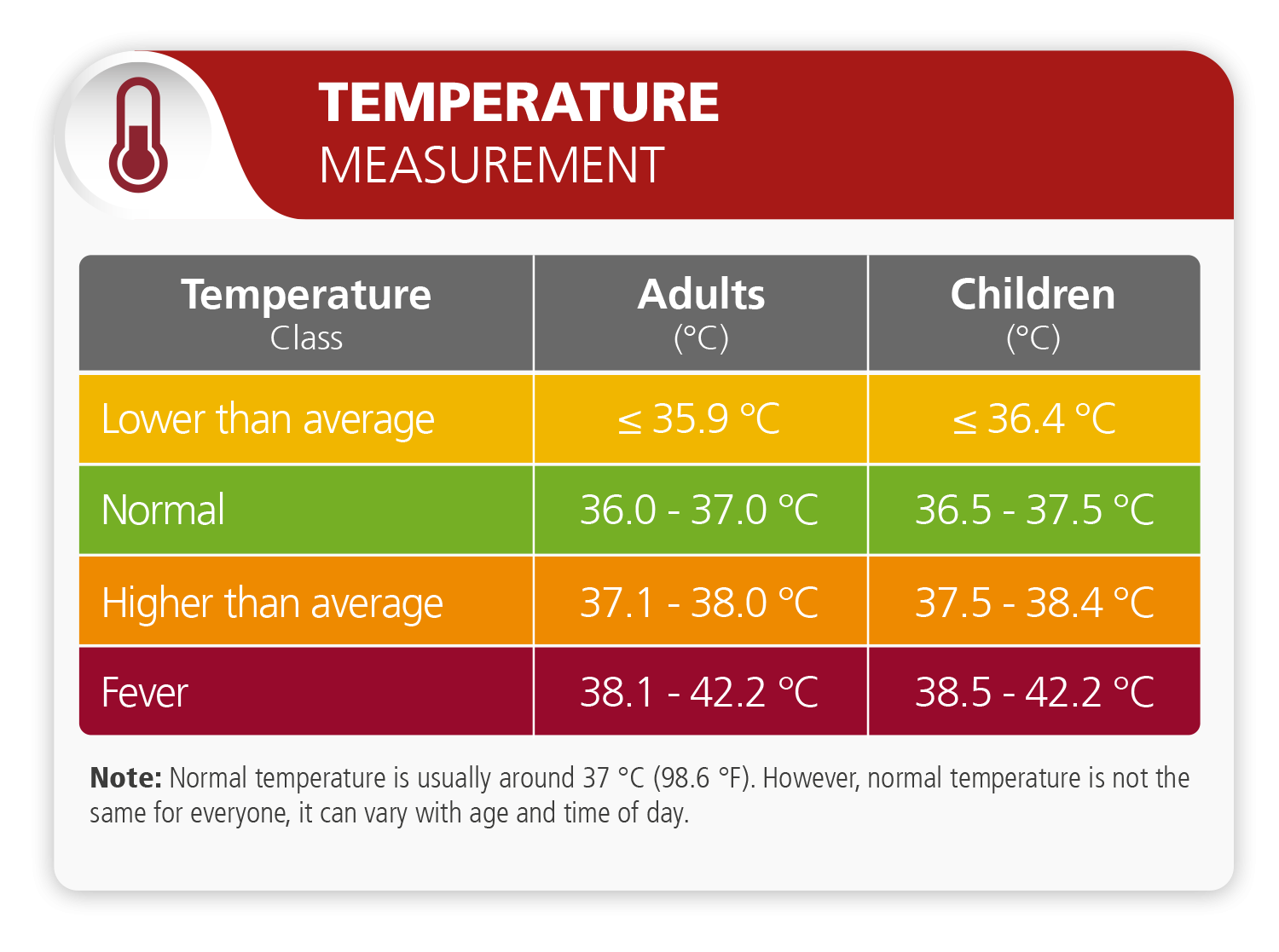
The Evolution of Thermal Sensing Technology
The journey from the mercury glass thermometer to the sophisticated sensors found in today’s gadgets represents one of the most significant leaps in medical instrumentation. In the tech sector, the focus has shifted from “intermittent checking” to “continuous monitoring,” necessitating a complete overhaul of how we capture thermal energy from the human body.
From Mercury to Infrared and Beyond
Traditional thermometers relied on physical expansion—mercury or alcohol rising in a tube. In the digital age, this was replaced by thermistors and, eventually, infrared (IR) sensors. The tech industry revolutionized temperature measurement during the global health crises of the last decade, perfecting non-contact IR sensors that can detect thermal radiation from the temporal artery in milliseconds. This transition from physical contact to digital sensing allowed for the mass deployment of temperature-screening kiosks in smart buildings and airports, integrating health tech directly into the physical infrastructure of our cities.
The Rise of IoT in Clinical Monitoring
The Internet of Things (IoT) has brought thermal sensing into the cloud. In hospital settings and smart homes, “connected” thermometers now sync data directly to Electronic Health Records (EHR). For the tech enthusiast and the healthcare provider alike, this means that a spike in temperature is no longer an isolated event. It is a time-stamped data point that can be cross-referenced with heart rate, oxygen saturation, and sleep cycles, providing a holistic view of a user’s physiological state.
Wearables and Continuous Biometric Monitoring
The most significant disruption in how we define a normal temperature comes from the wearable technology sector. Devices like the Apple Watch, Oura Ring, and Whoop strap have moved the thermometer from the medicine cabinet to the wrist and finger, providing a 24/7 look at the body’s thermal fluctuations.
Smartwatches and Rings: The Hardware Challenge
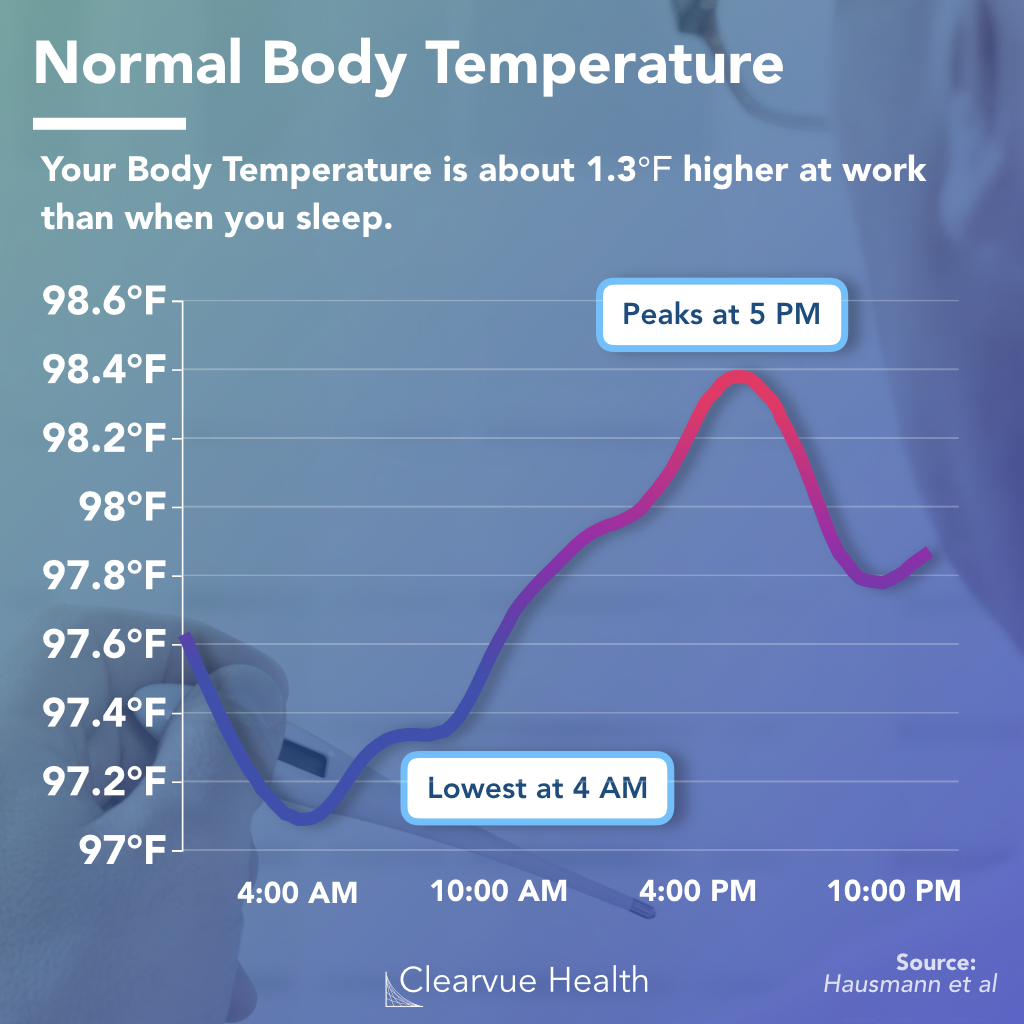
Measuring temperature from the skin’s surface—specifically the wrist or finger—is a complex engineering feat. Unlike internal “core” temperature, skin temperature is highly susceptible to environmental factors. Tech giants have solved this by using dual-sensor arrays: one sensor to measure the skin and another to measure the ambient temperature. Sophisticated heat-flux algorithms then calculate the bridge between the two, providing a reliable estimate of the body’s internal state. This continuous stream of data has revealed that a “normal” temperature fluctuates significantly throughout the day based on circadian rhythms, activity levels, and even metabolic rate.
Defining the “Personal Baseline”
Perhaps the greatest contribution of wearable tech is the move toward the “Personal Baseline.” Instead of comparing a user to the 98.6°F average, software platforms now use the first 14 to 30 days of data to establish what is normal for that specific individual. If a user’s baseline is 97.9°F, a reading of 98.8°F—which would be considered “normal” by traditional standards—might actually trigger a notification of a potential illness or recovery deficit. This shift from population averages to individualized data is the essence of precision health tech.
AI and Predictive Diagnostics: Analyzing the Thermal Signal
Raw data is of little use without the analytical power to interpret it. This is where Artificial Intelligence (AI) and Machine Learning (ML) become the primary tools for understanding human temperature.
Machine Learning in Febrile Detection
AI models are now being trained on millions of nights of temperature data to identify the “thermal signature” of an oncoming illness. Researchers have found that subtle rises in skin temperature, often invisible to the user and below the threshold of a clinical fever, can predict the onset of viral infections days before symptoms appear. By analyzing the rate of change and the deviation from the personal baseline, ML algorithms provide a predictive edge that traditional medicine simply cannot match.
Personalized Health Insights and Women’s Tech (FemTech)
One of the most robust applications of thermal tech is in the FemTech sector. Temperature is a key biomarker for tracking hormonal cycles. Apps and wearables use high-precision thermal sensors to detect the slight increase in basal body temperature (BBT) that occurs after ovulation. By applying AI to these data points, technology provides users with deep insights into their reproductive health, transforming temperature from a simple “illness gauge” into a sophisticated tool for biological planning and wellness.
Digital Security and Health Data Privacy
As temperature monitoring becomes a standard feature in consumer tech, the “digital twin” of our biological selves is increasingly stored in the cloud. This brings the critical issue of digital security and data ethics to the forefront of the conversation.
Safeguarding Biometric Data
Biometric data, including continuous temperature logs, is highly sensitive. If leaked, it can reveal intimate details about an individual’s health, habits, and even pregnancy status. Tech companies are now implementing end-to-end encryption and “On-Device Processing” to ensure that thermal data never leaves the user’s hardware without explicit consent. In the realm of enterprise tech, companies are developing “Zero-Knowledge” architectures where the service provider can verify a health status (e.g., “User is not febrile”) without actually seeing or storing the specific temperature data.
The Ethics of Remote Monitoring
The ability of employers or governments to monitor “normal temperature” through tech-enabled infrastructure raises significant ethical questions. As we integrate thermal scanning into smart office entry systems, the industry must navigate the balance between public safety and individual privacy. The development of robust “privacy-by-design” frameworks is essential to ensure that temperature-tracking technology remains a tool for empowerment rather than surveillance.
The Future: Toward Autonomous Health Management
Looking ahead, the technology surrounding human temperature is moving toward even greater integration and automation. We are moving past the era of “checking” and into the era of “sensing.”
Implantable Sensors and Bio-Hacking
The next frontier in thermal tech is the implantable sensor. For high-performance athletes or individuals with chronic conditions, “smart pills” or sub-dermal sensors can provide the most accurate core temperature data possible. These devices communicate via Near-Field Communication (NFC) or Bluetooth Low Energy (BLE) to a smartphone, providing a direct, unfiltered link to the body’s internal thermostat. This represents the ultimate convergence of human biology and digital hardware.
Closing the Feedback Loop
In the near future, your “normal temperature” data won’t just reside in an app; it will interact with your environment. Imagine a smart home that detects a slight rise in your body temperature during sleep and automatically adjusts the smart thermostat or the cooling settings of a high-tech mattress to optimize your recovery. This “closed-loop” system, where tech senses a biological need and autonomously adjusts the environment to meet it, is the logical conclusion of our current trajectory in health technology.
Conclusion
The question of “what is a normal temperature for a human” is no longer a simple medical inquiry; it is a complex technological challenge. Through high-precision sensors, individualized baselines, and AI-driven analytics, the tech industry has proven that the old standards are too narrow for the complexities of human biology.
By treating temperature as a dynamic stream of data rather than a static number, we are unlocking new possibilities for early disease detection, reproductive health, and personalized wellness. As we continue to integrate these sensors into our lives, the focus will remain on refining the hardware, securing the data, and using AI to turn “normal” into a personalized roadmap for better health. The 98.6°F standard served us well for a century, but in the age of tech, our baselines are as unique as our digital fingerprints.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.