In the contemporary landscape of preventive medicine, the intersection of cardiovascular health and digital innovation has revolutionized how we understand and manage critical physiological thresholds. One of the most urgent questions in this domain—particularly for female patients—is: “What is stroke-level blood pressure for a woman?” While the medical answer remains consistent at a clinical level, the technological answer involves a complex ecosystem of wearable sensors, artificial intelligence (AI), and data-driven diagnostic tools.
For women, identifying the onset of a hypertensive crisis—the “stroke level”—is no longer solely dependent on a biannual visit to a primary care physician. Today, the tech sector provides the infrastructure necessary to monitor, interpret, and act upon blood pressure readings that signal immediate danger. This article explores the technological advancements in monitoring hypertension, the software algorithms that identify stroke risks, and how gender-specific data integration is shaping the future of women’s health technology.

The Digital Threshold: Defining Hypertensive Crisis Through Software
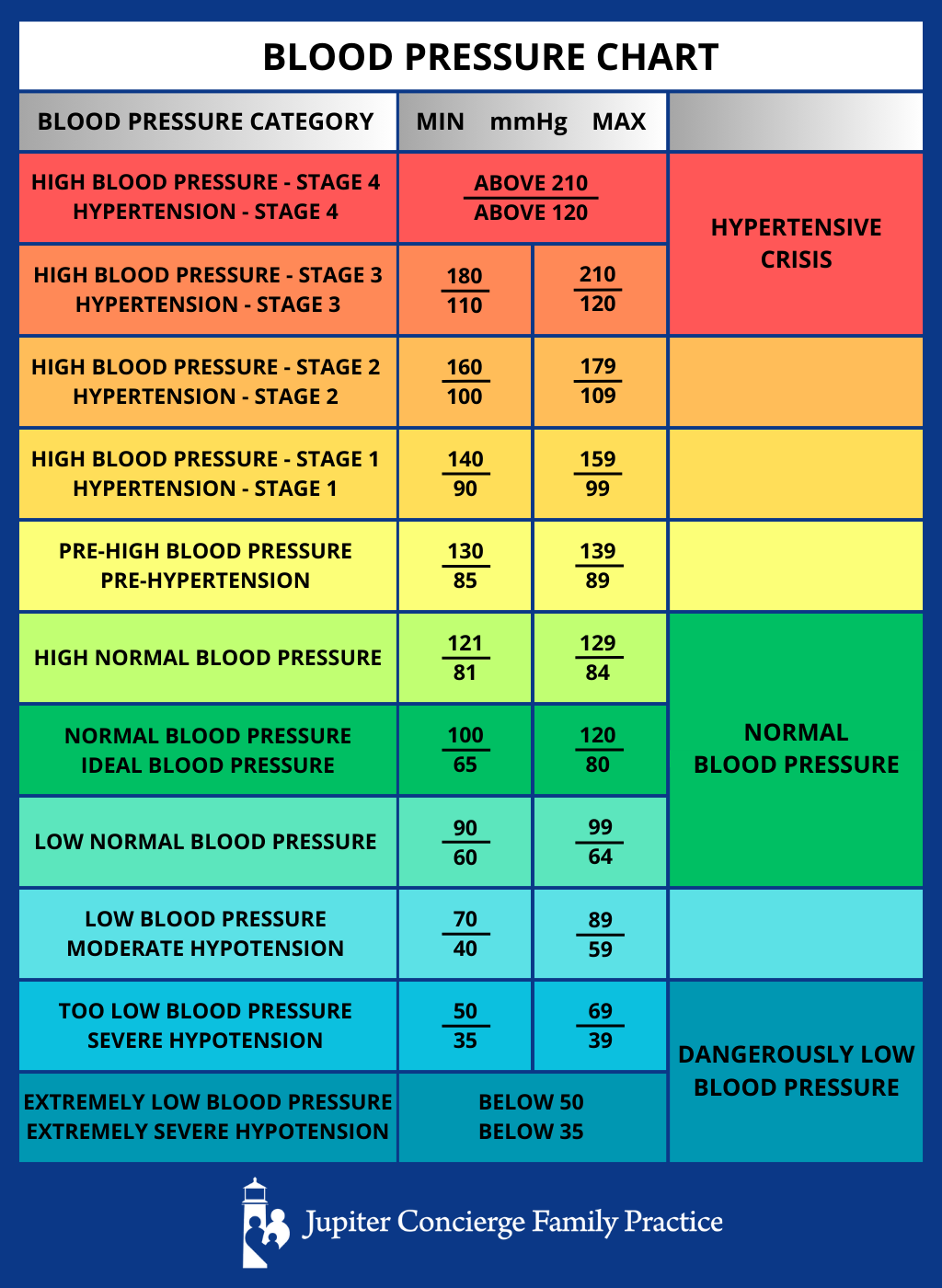
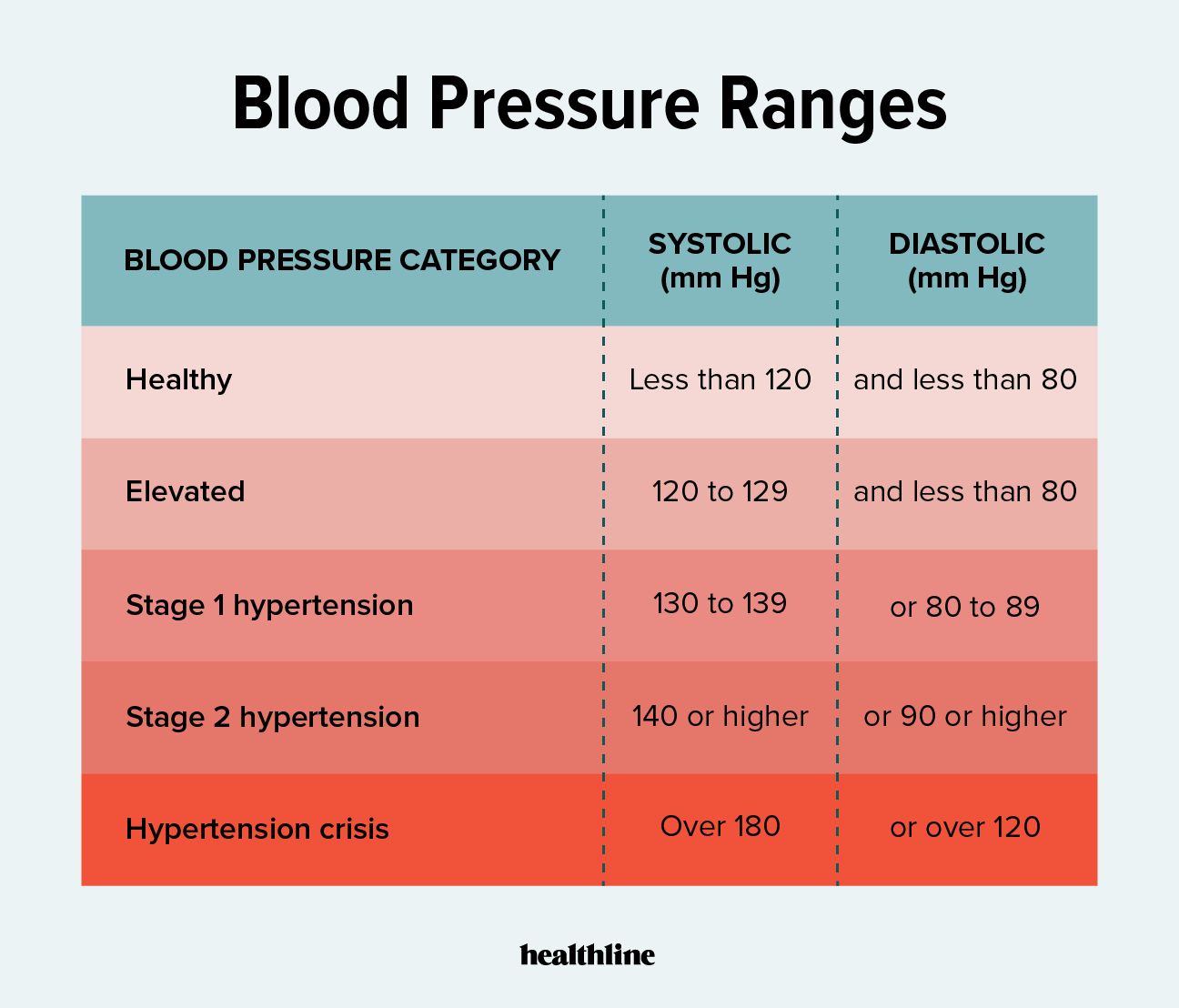
Understanding what constitutes “stroke level” blood pressure requires a look at how health software categorizes data points. In clinical terms, a hypertensive crisis is typically defined as a reading of 180/120 mmHg or higher. However, modern health technology treats these numbers not just as static figures, but as critical data triggers within an automated monitoring system.
AI Interpretation of Blood Pressure Tiers
Health applications and cloud-based medical platforms utilize specific algorithms to categorize blood pressure into actionable tiers. When a woman uses a smart device to log her vitals, the software immediately filters the input through established medical guidelines (such as those from the American Heart Association).
The “stroke level” is categorized in these systems as a “red-tier” alert. Sophisticated AI tools go a step further by analyzing the rate of change. If a woman’s blood pressure climbs rapidly from a baseline of 120/80 to 160/100 within a short window, the software may trigger an early warning before the 180/120 “stroke level” is even reached. This predictive capability is a cornerstone of modern HealthTech, moving the needle from reactive treatment to proactive prevention.
Digital Accuracy and Calibration Tools
One of the primary challenges in the tech niche has been ensuring the accuracy of non-invasive blood pressure (NIBP) monitoring. Tech developers are increasingly focused on “cuffless” technology, utilizing photoplethysmography (PPG) sensors—the same technology used in heart rate monitors—to estimate blood pressure. To ensure these devices can accurately detect stroke-level readings, companies are integrating advanced calibration software that syncs with traditional oscillometric cuffs, creating a dual-layered verification system that minimizes false negatives.
The Wearable Revolution: Continuous Monitoring vs. Spot Checks
The transition from “spot-check” medicine to continuous health monitoring represents one of the most significant shifts in 21st-century technology. For a woman at risk of stroke, the ability to monitor blood pressure continuously through wearable devices can be a life-saving intervention.
The Rise of Medical-Grade Wearables
While early fitness trackers were designed for step counting, the latest generation of wearables focuses on medical-grade metrics. Companies like Omron and various startups in the Silicon Valley ecosystem have developed wrist-worn devices that house miniaturized pumps and bladders. These devices act as a “watch” but function as a professional blood pressure cuff.
The software integrated into these wearables allows for “nocturnal monitoring.” Research suggests that “dipping” or “non-dipping” blood pressure patterns during sleep are significant indicators of stroke risk in women. By capturing these trends automatically, the technology provides a comprehensive data set that a single office visit could never replicate.
Data Visualization and User Interface (UI) for Patients
Tech innovation isn’t just about sensors; it’s about communication. Modern HealthTech focuses on the UI/UX of health apps to ensure that when a woman reaches a “stroke level” reading, the information is communicated clearly and urgently.
Insightful data visualization—using heat maps, trend lines, and color-coded alerts—helps users distinguish between a temporary spike due to stress and a sustained hypertensive crisis. For a woman managing her health, these interfaces translate complex medical data into a narrative that highlights when immediate medical intervention is required.
FemTech and Gender-Specific Algorithms in Cardiovascular Health
Historically, medical technology and research were often centered on male physiology. However, the rise of “FemTech” (Female Technology) has led to the development of software and hardware specifically tuned to the unique cardiovascular markers of women.
Accounting for Hormonal Fluctuations in Data
A woman’s blood pressure can be influenced by biological factors that do not affect men, such as pregnancy, hormonal contraceptive use, and menopause. Advanced health platforms now incorporate “gender-specific variables” into their predictive models.
For instance, during pregnancy, a blood pressure reading that might be considered “elevated” in a general context could be a sign of preeclampsia—a condition that significantly increases stroke risk. FemTech apps use machine learning to adjust “normal” baselines based on the user’s biological profile, ensuring that “stroke level” warnings are calibrated to the individual’s specific physiological state.
The Role of Big Data in Understanding Women’s Stroke Risks
By aggregating anonymized data from millions of female users, tech companies are building the largest repositories of cardiovascular data in history. This “Big Data” approach allows researchers to identify subtle patterns that precede a stroke in women. AI tools can analyze this data to find correlations between lifestyle, age, and blood pressure spikes, leading to more refined software updates that provide personalized risk assessments for female users worldwide.
Telehealth Integration and Automated Emergency Protocols
The final piece of the technology puzzle is the bridge between the home-monitored “stroke level” reading and the emergency room. Telehealth and Remote Patient Monitoring (RPM) have closed the gap between data collection and clinical action.
Automated Alerts and Emergency Response
The most advanced health ecosystems are now linked directly to emergency services. If a wearable device detects a sustained reading of 180/120 mmHg—the stroke level—and the user does not dismiss the alert, the software can be programmed to automatically notify a designated emergency contact or even dispatch local EMS with the user’s GPS coordinates.
This automation is critical for stroke cases, where “time is brain.” Technology ensures that even if a woman is incapacitated by a sudden hypertensive event, the device on her wrist acts as a silent guardian, initiating the rescue protocol based on the data it has captured.
The Integration with Electronic Health Records (EHR)
Data silos are the enemy of effective healthcare. Modern HealthTech solutions prioritize interoperability, allowing blood pressure data to flow seamlessly from a smartphone app into a hospital’s Electronic Health Record system.
When a woman arrives at the hospital after a stroke-level event, her physicians don’t have to rely on her memory. They can access a digital dashboard showing her blood pressure trends over the previous weeks, months, or years. This longitudinal data provides the context necessary for tech-enabled precision medicine, allowing for more accurate post-stroke care and medication adjustments.
The Future Frontier: Neural Sensors and Predictive Analytics
As we look toward the future of technology in managing stroke-level blood pressure, the focus is shifting toward even more non-invasive and predictive tools.
Neural Monitoring and Bio-Electronic Medicine
New frontiers in tech are exploring the “brain-heart” connection. Experimental neural sensors can now monitor the signals the brain sends to the heart and blood vessels. By interpreting these neural impulses, software may soon be able to predict a hypertensive crisis minutes or even hours before it manifests physically in a blood pressure reading. This level of foresight would represent the ultimate achievement in stroke prevention technology.
The Edge Computing Advantage
As processors become smaller and more powerful, “edge computing”—processing data on the device itself rather than in the cloud—is becoming more prevalent. This means that a woman’s wearable device can perform complex calculations and identify stroke-level threats in real-time, even without an internet connection. This autonomy is vital for users in remote areas or for those who travel frequently, ensuring that their technological safety net is always active.
In conclusion, while the clinical answer to “what is stroke level blood pressure for a woman” is a clear-cut 180/120 mmHg, the technological response is a multi-faceted system of protection. Through the lens of Tech, managing blood pressure is no longer a matter of chance, but a matter of data precision. From AI-driven predictive analytics and gender-specific FemTech to automated emergency responses, the technology of today is dedicated to ensuring that a crisis level is never just a number on a screen, but a catalyst for life-saving action.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.