Understanding the prevalence of abortion is often discussed through demographic and health lenses. However, from a business and financial standpoint, the question of “what percent of women get abortions” intersects with critical aspects of healthcare economics, access to financial resources for healthcare, and the economic burden on individuals and the broader healthcare system. This article will explore the financial implications surrounding abortion access, focusing on the costs associated with the procedure, the economic factors influencing access, and the broader economic ripple effects.
The Financial Landscape of Abortion Access
The financial reality of obtaining an abortion is a significant determinant of access. The cost of an abortion procedure can vary widely based on several factors, including the stage of pregnancy, the type of procedure, the geographic location, and the healthcare provider. These costs are not merely a transactional expense; they represent a financial hurdle that can disproportionately affect individuals with lower incomes.
Direct Costs of Abortion Procedures
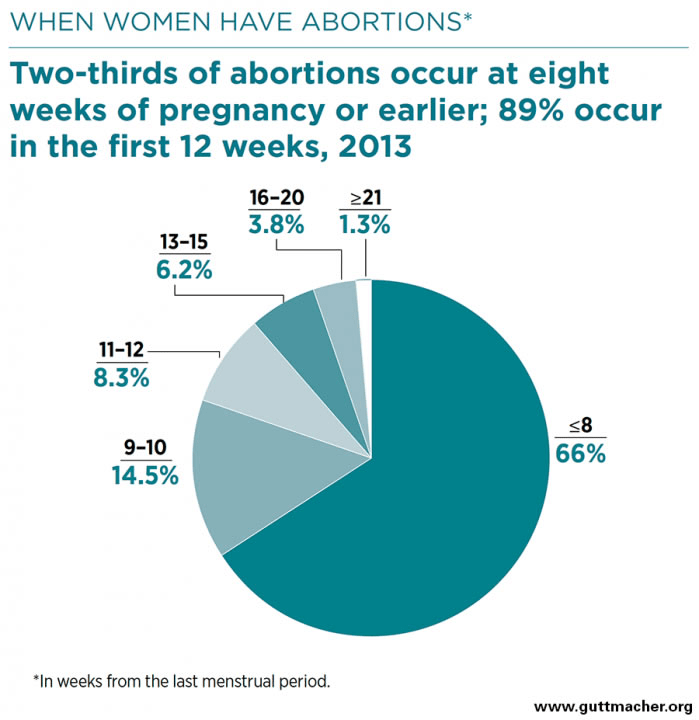
The direct costs of an abortion procedure are often the most immediate financial consideration. These costs can be broadly categorized into the physician’s fee, facility fees, and any associated medical supplies or tests. For early-term abortions, which typically involve medication abortion or a simple aspiration procedure, the costs might range from a few hundred dollars to over a thousand. As the pregnancy progresses, surgical abortions become more complex and therefore more expensive, potentially costing several thousand dollars.
It’s crucial to note that these figures represent the cost of the procedure itself. They do not include potential ancillary costs such as travel to and from the clinic, accommodation if overnight stays are required, childcare expenses, or lost wages due to time taken off work for appointments and recovery. For many individuals, especially those living in areas with limited access to abortion providers, these additional expenses can significantly amplify the financial burden.
Insurance Coverage and Out-of-Pocket Expenses
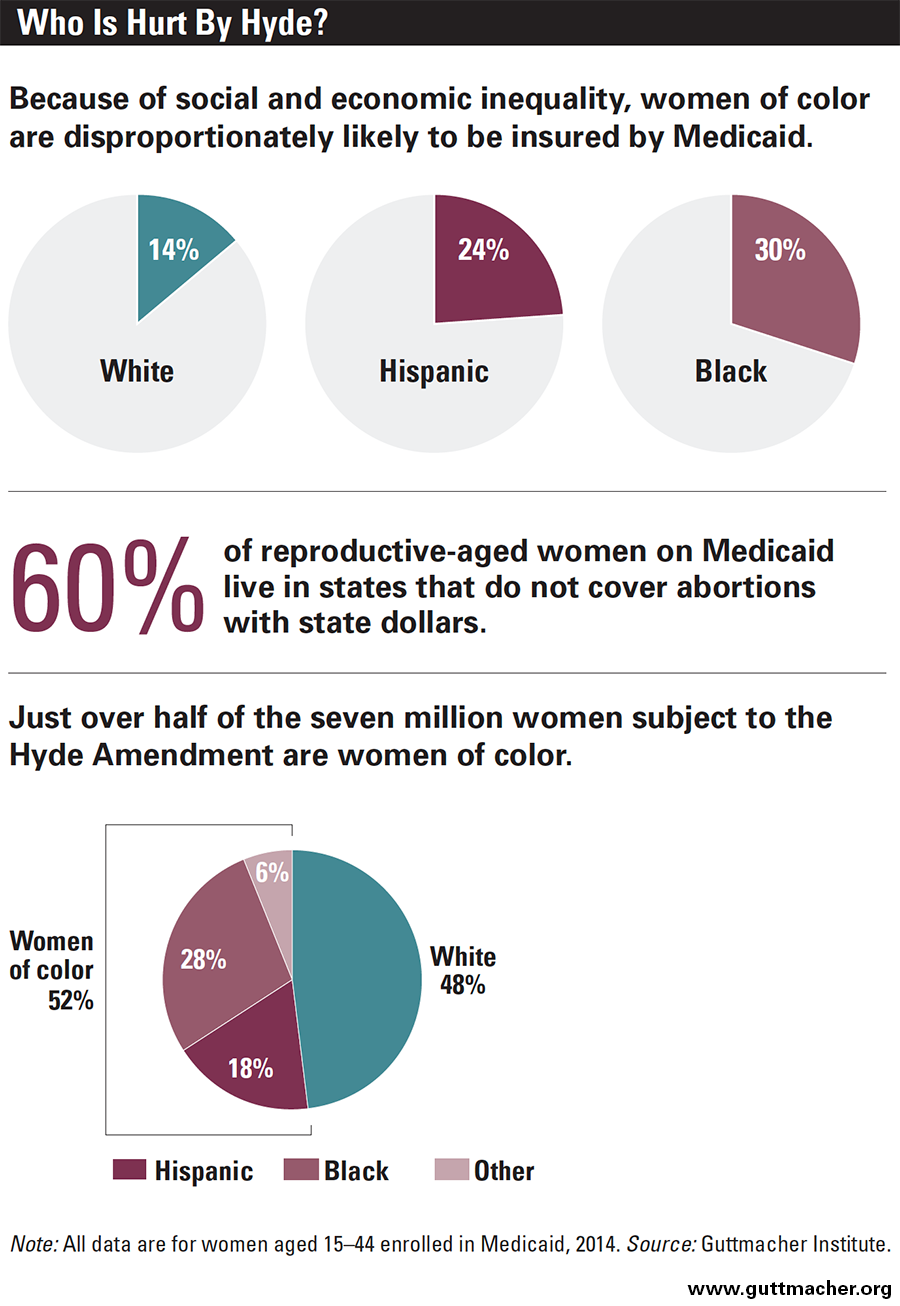
The extent to which insurance plans cover abortion services is a critical factor in determining out-of-pocket expenses for women. Historically, federal funding for abortion services through programs like Medicaid has been heavily restricted, with exceptions primarily for cases of rape, incest, or to save the life of the mother. This has led to a patchwork of coverage across states and private insurance plans.
In states where insurance mandates require coverage, or for individuals with comprehensive private insurance, the out-of-pocket cost might be limited to co-pays, deductibles, or co-insurance. However, in many regions, abortion services are not covered by insurance at all, or only under very specific, limited circumstances. This means that individuals without adequate insurance coverage are solely responsible for the full cost of the procedure. This disparity in insurance coverage directly translates into significant financial barriers for a substantial portion of the population seeking abortion care.
Financial Assistance and Support Organizations
Recognizing the financial challenges, a network of abortion funds and practical support organizations exists to help individuals afford abortion care. These organizations, often non-profits, provide financial assistance, logistical support, and sometimes even direct funding for the procedure itself. They play a vital role in bridging the financial gap for those who cannot afford the full cost.
These funds are typically supported by donations and grants, and their capacity to assist is directly linked to their funding levels. The demand for assistance often outstrips the available resources, highlighting the ongoing financial strain on individuals seeking abortion services. The operational costs of these organizations, including fundraising, administration, and program delivery, also represent a financial ecosystem dedicated to facilitating access to reproductive healthcare.
Economic Factors Influencing Abortion Decisions and Access
Beyond the direct costs of the procedure, broader economic factors significantly influence an individual’s decision-making process regarding pregnancy and their ability to access abortion services. These factors are deeply intertwined with socioeconomic status and financial stability.
Socioeconomic Status and Income Levels
Socioeconomic status is a powerful predictor of both unintended pregnancy rates and the ability to access abortion. Individuals with lower incomes and those in poverty often face greater financial instability, making the prospect of raising a child a more daunting economic challenge. For these individuals, the cost of an abortion, even with assistance, can be a significant decision point.
The economic consequences of an unplanned pregnancy can be profound, potentially exacerbating existing financial vulnerabilities. This includes increased costs associated with prenatal care, childbirth, and raising a child, which can further strain already limited resources. In such circumstances, the financial implications of carrying a pregnancy to term versus seeking an abortion can be a primary driver of the decision.
Employment and Income Stability
Employment and income stability play a crucial role in an individual’s ability to absorb the costs associated with an abortion. Individuals with stable, well-paying jobs and comprehensive benefits are more likely to have insurance coverage or the disposable income to cover out-of-pocket expenses and associated costs like lost wages. Conversely, those in precarious employment situations, with unpredictable hours or low wages, face greater obstacles.
The necessity of taking time off work for appointments and recovery can also be a significant economic deterrent. For hourly workers, missing even a few hours of work can mean a substantial loss of income, making the decision to pursue an abortion even more financially perilous. This highlights how the economic structure of employment directly impacts reproductive health decisions.
Geographic Location and Access to Services
The geographic distribution of abortion providers has a direct economic consequence. In areas with fewer abortion clinics, individuals may need to travel long distances, incurring significant travel, accommodation, and lost wage costs. This “travel burden” can be substantial and is often a prohibitive expense for those with limited financial resources.
The economic impact of such travel can be considerable, impacting not only the individual but also the economies of the areas they travel from and to. Furthermore, the concentration of providers in urban centers can leave rural and underserved populations with limited and financially burdensome access to care. This uneven distribution of healthcare infrastructure creates economic disparities in reproductive health outcomes.
The Broader Economic Implications of Abortion Access
The financial considerations surrounding abortion access extend beyond individual out-of-pocket expenses. There are broader economic implications for families, communities, and the economy as a whole, impacting labor force participation, poverty rates, and healthcare expenditures.
Impact on Women’s Economic Participation and Earnings
Studies have explored the long-term economic effects of having or not having an abortion on women’s lives. Research, such as the Turnaway Study, has indicated that women who are denied abortions and carry unwanted pregnancies to term may experience significant negative economic consequences. These can include increased rates of poverty, decreased labor force participation, and lower educational attainment.
Conversely, having access to abortion services can allow women to better manage their economic circumstances, pursue educational opportunities, and maintain or improve their employment prospects. This has a ripple effect on their earning potential, their ability to contribute to the economy, and their overall financial well-being, which in turn impacts their families and communities.
Healthcare System Costs and Resource Allocation
While often framed as an individual’s expense, abortion access also has implications for the healthcare system’s financial landscape. The costs associated with unintended pregnancies, prenatal care, childbirth, and pediatric care are significant. When abortion is inaccessible, these costs are borne by individuals, families, and publicly funded healthcare programs.
Conversely, providing access to safe and affordable abortion services can, in some economic models, be viewed as a means of preventing more substantial future healthcare costs associated with unintended births, particularly for individuals who are not financially prepared for parenthood. Resource allocation decisions within healthcare systems often involve balancing the immediate costs of certain procedures against the potential long-term economic and health outcomes.

Economic Determinants of Reproductive Health Choices
Ultimately, the “what percent of women get abortions” is influenced by a complex interplay of social, personal, and economic factors. From a financial perspective, understanding the cost of procedures, the availability of insurance, the effectiveness of financial assistance programs, and the broader economic landscape is crucial.
The economic well-being of individuals and communities directly shapes their ability to access reproductive healthcare services, including abortion. Addressing financial barriers through improved insurance coverage, robust abortion funds, and supportive economic policies is not only a matter of reproductive rights but also a consideration for fostering economic stability and opportunity for all. The financial ecosystem surrounding abortion access is a critical, albeit often overlooked, component of the larger discussion.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.