The question of “what organ produces cholesterol” delves into a fundamental aspect of human biology that has significant implications for our health and, consequently, our financial well-being. While the immediate association might be with dietary intake, the reality is that our bodies are remarkably adept at synthesizing this vital lipid. Understanding the organs responsible for cholesterol production is not merely an academic pursuit; it’s a cornerstone for informed decision-making regarding personal finance, particularly in areas related to health insurance, preventative care, and even long-term investment in one’s own human capital.
Cholesterol, often maligned in public discourse, is not inherently “bad.” It is an essential component of cell membranes, a precursor to vital hormones like estrogen and testosterone, and a building block for vitamin D and bile acids, which aid in digestion. The body’s intricate system of producing and regulating cholesterol is a marvel of biological engineering. However, when this system becomes dysregulated, it can lead to serious health issues that have far-reaching financial consequences. This article will explore the primary organs involved in cholesterol synthesis, the biological processes at play, and crucially, how understanding these biological realities can empower individuals to make more financially prudent decisions concerning their health and future.

The Liver: The Master Regulator of Cholesterol Synthesis
The liver stands as the undisputed heavyweight champion when it comes to cholesterol production. This multifaceted organ, weighing approximately 3 pounds in an adult, is a chemical factory responsible for a vast array of metabolic functions, including the de novo synthesis of cholesterol.
The De Novo Synthesis Pathway
The liver’s production of cholesterol, known as de novo synthesis, is a complex multi-step process that begins with simple precursors, primarily acetyl-CoA. This pathway, occurring within the liver cells (hepatocytes), involves numerous enzymatic reactions, the most critical of which is the conversion of HMG-CoA to mevalonate, catalyzed by the enzyme HMG-CoA reductase. This enzyme is a key regulatory point in cholesterol synthesis and is the target of statin medications, a multi-billion dollar pharmaceutical class designed to lower cholesterol levels.
The synthesis pathway can be broadly divided into several stages:
- Mevalonate Pathway: This initial phase is crucial for producing cholesterol and other isoprenoids. It involves the condensation of acetyl-CoA molecules to form HMG-CoA, which is then reduced to mevalonate.
- Squalene Synthesis: Mevalonate is then converted through a series of steps into squalene, a 30-carbon hydrocarbon.
- Sterol Ring Formation: Squalene undergoes cyclization and further modifications to form lanosterol, which is then converted into cholesterol.
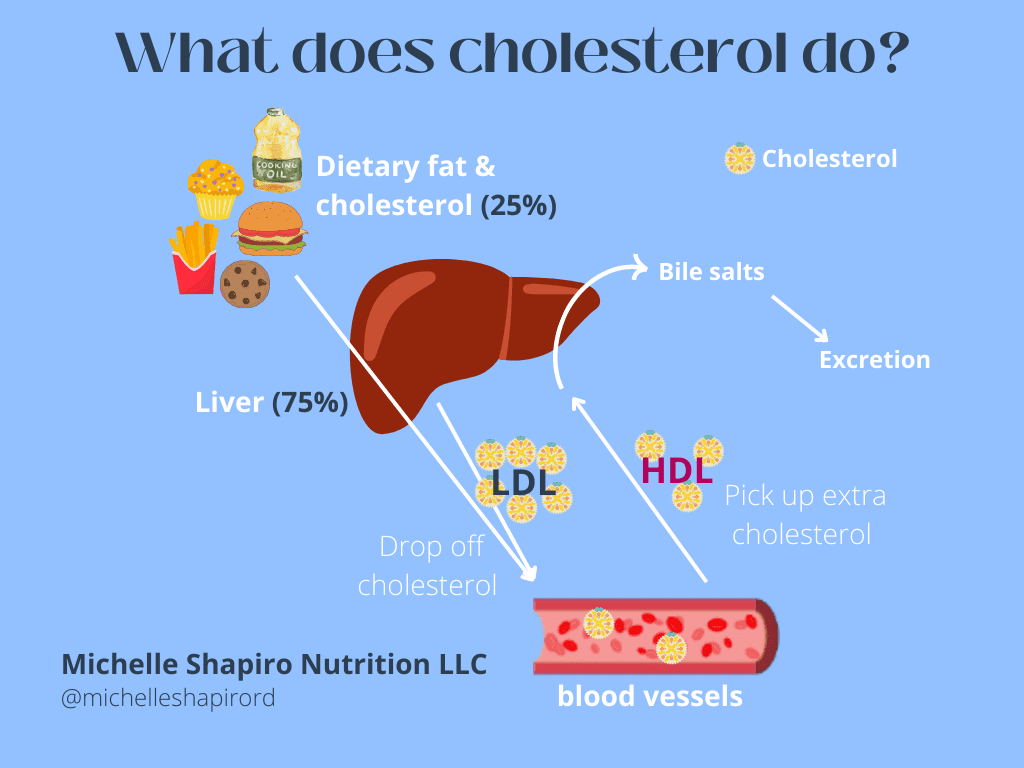
The liver synthesizes a substantial portion of the body’s cholesterol requirements, estimated to be around 75-80%. This internal production is vital because dietary cholesterol absorption, while contributing to the body’s cholesterol pool, is not as significant as endogenous synthesis. The liver meticulously balances the amount of cholesterol it produces with what the body needs and what is absorbed from the diet.
Cholesterol Transport and Metabolism
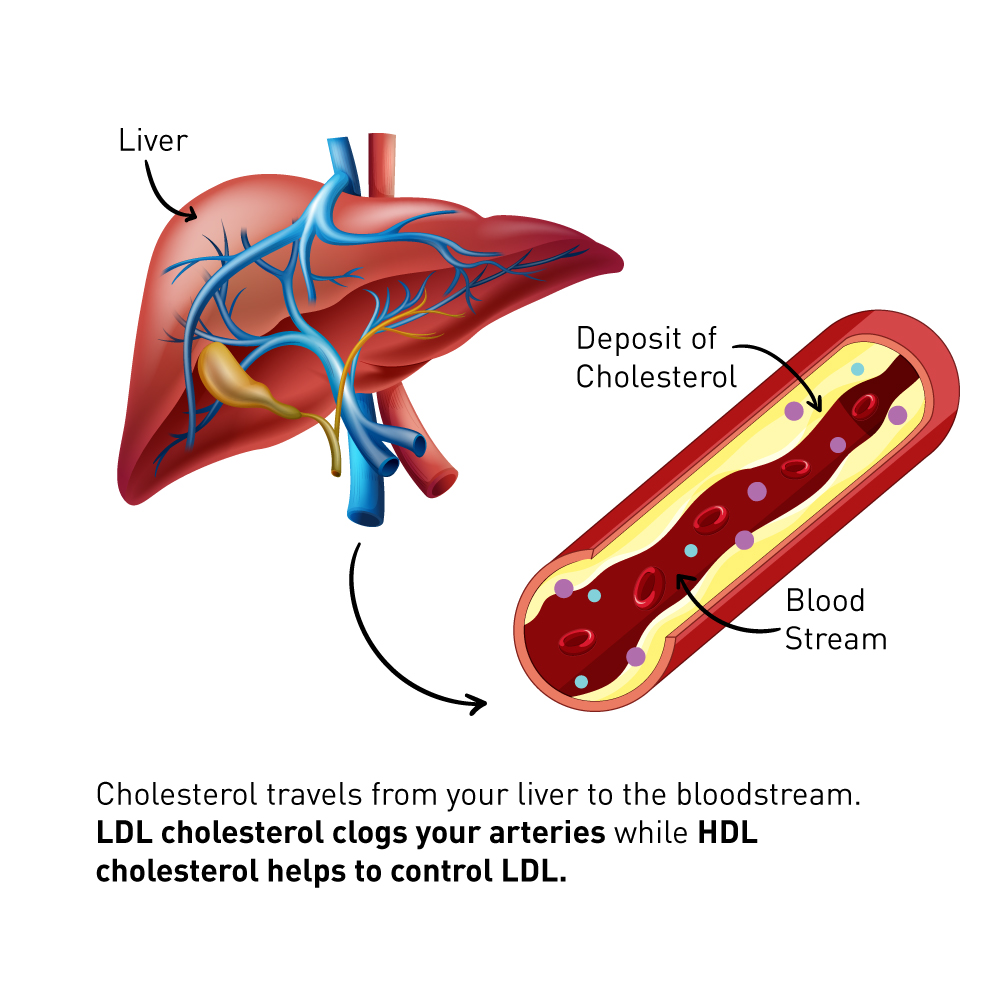
Beyond production, the liver plays a pivotal role in cholesterol transport and metabolism. It packages cholesterol and triglycerides into very-low-density lipoproteins (VLDL), which are then secreted into the bloodstream. As VLDL circulates, it delivers triglycerides to tissues and eventually transforms into low-density lipoprotein (LDL). LDL, often referred to as “bad” cholesterol, carries cholesterol from the liver to peripheral tissues.
Conversely, the liver is also responsible for clearing excess cholesterol from the body. It does this by converting cholesterol into bile acids, which are secreted into the bile and eliminated in the feces. High-density lipoprotein (HDL), often called “good” cholesterol, picks up excess cholesterol from peripheral tissues and transports it back to the liver for excretion. This intricate interplay between production, distribution, and excretion is a delicate balancing act managed primarily by the liver.
The Intestines: A Significant Contributor to Cholesterol Pool
While the liver is the primary site of cholesterol synthesis, the intestines, particularly the small intestine, also contribute to the body’s cholesterol, though through a different mechanism: absorption.
Absorption of Dietary Cholesterol
The small intestine is the primary site for absorbing cholesterol that we consume in our diet. Cholesterol from food, along with cholesterol secreted in bile, is incorporated into micelles within the intestinal lumen. These micelles then facilitate the absorption of cholesterol and other lipids across the intestinal cell membranes.
Once inside the intestinal cells (enterocytes), cholesterol is packaged into chylomicrons, large lipoprotein particles that are then released into the lymphatic system. From the lymphatic system, chylomicrons eventually enter the bloodstream, delivering dietary fats and cholesterol to various tissues throughout the body.
Endogenous Synthesis in Intestinal Cells
It’s important to note that intestinal cells themselves are also capable of synthesizing cholesterol, albeit to a lesser extent than the liver. This endogenous synthesis within the intestine adds to the total cholesterol available for absorption and incorporation into the body’s pool. The balance between dietary cholesterol absorption and endogenous synthesis in the intestine is a complex physiological process that can be influenced by various factors, including diet and genetics.
The intestinal contribution, while significant, is primarily focused on absorbing what we eat. The liver’s role is far more extensive, involving the production of the majority of the cholesterol the body requires for its fundamental functions.
Other Organs and Their Roles in Cholesterol Regulation
While the liver and intestines are the stars of the cholesterol production and absorption show, other organs play crucial supporting roles in maintaining cholesterol homeostasis and influencing its overall levels within the body.
Adrenal Glands and Gonads: Steroid Hormone Production
The adrenal glands and gonads (testes in males, ovaries in females) are significant consumers of cholesterol, utilizing it as a precursor for the synthesis of steroid hormones. These hormones, including cortisol, aldosterone, sex hormones like testosterone and estrogen, and progesterone, are vital for a myriad of physiological processes.
- Adrenal Glands: These glands, located atop the kidneys, use cholesterol to produce glucocorticoids (like cortisol), mineralocorticoids (like aldosterone), and androgens.
- Gonads: The testes produce testosterone, while the ovaries produce estrogen and progesterone, all of which are synthesized from cholesterol.
The demand for cholesterol by these endocrine organs influences the body’s overall cholesterol metabolism. When the body requires more steroid hormones, it can increase cholesterol synthesis or uptake to meet these demands. This highlights the essential role of cholesterol for reproductive health and stress response, underscoring its importance beyond just being a component of cell membranes.
Reproductive System and Cholesterol
The reproductive system, in particular, has a high requirement for cholesterol. Estrogen, a key hormone in female reproductive health, is synthesized from cholesterol. Similarly, testosterone, crucial for male development and function, also originates from cholesterol. The health and functionality of these systems are intrinsically linked to adequate cholesterol availability.
Financial Ramifications of Cholesterol Management
Understanding which organs produce cholesterol and how the body regulates it is not just a biological curiosity; it has profound implications for personal finance and long-term financial planning. Dysregulated cholesterol levels, particularly elevated LDL or low HDL, are significant risk factors for cardiovascular diseases (CVDs), a leading cause of death and disability globally. The financial burden associated with CVDs is staggering, encompassing direct medical costs and indirect costs related to lost productivity and reduced earning potential.
Health Insurance and Cholesterol
For individuals, managing cholesterol levels is directly tied to their health insurance premiums and coverage. High cholesterol often necessitates more frequent doctor visits, prescription medications, and potentially, more invasive medical procedures. This can lead to:
- Higher Premiums: Insurance providers may classify individuals with high cholesterol as having a higher risk, resulting in increased premium costs.
- Increased Out-of-Pocket Expenses: Even with insurance, deductibles, co-pays, and co-insurance for medications and treatments can accumulate significantly.
- Limited Coverage: In some cases, pre-existing conditions like high cholesterol might affect the extent of coverage for certain treatments or procedures.
Proactive management of cholesterol through lifestyle changes and, if necessary, medical intervention can potentially lead to lower insurance costs over time and better overall health coverage.
Investment in Preventative Care and Human Capital
Viewing cholesterol management through a financial lens encourages an investment in preventative care. This includes:
- Dietary Choices: Opting for healthier food choices, rich in fiber and healthy fats while limiting saturated and trans fats, can impact cholesterol levels. While the initial cost of healthy food might sometimes seem higher, the long-term benefits in terms of reduced healthcare expenditure are substantial.
- Regular Exercise: Physical activity has a positive impact on cholesterol profiles, increasing HDL and lowering LDL. Investing time in exercise can be seen as an investment in one’s physical and financial future, reducing the likelihood of costly health interventions down the line.
- Medical Screenings: Regular cholesterol checks, recommended by healthcare professionals, allow for early detection and intervention. This proactive approach can prevent the progression of conditions that would otherwise lead to more expensive treatments.
Essentially, investing in one’s health through mindful cholesterol management is an investment in human capital. A healthy individual is more productive, has a higher earning potential, and is less likely to incur significant unexpected medical expenses that can derail financial plans.
The Pharmaceutical Industry and Cholesterol
The global pharmaceutical market for cholesterol-lowering drugs, particularly statins, is a multi-billion dollar industry. This highlights the economic significance of cholesterol management. While these medications can be life-saving and essential for many, understanding the underlying biological processes and the role of organs like the liver can empower patients to have more informed discussions with their doctors. This might involve exploring lifestyle modifications as a primary strategy, potentially reducing reliance on or the dosage of medication, thereby impacting long-term personal financial outlays. Furthermore, understanding the science behind these drugs can also inform investment decisions for individuals interested in the healthcare sector.
In conclusion, while the question “what organ produces cholesterol” might seem purely biological, its answer resonates deeply within the financial landscape. The liver’s sophisticated machinery for cholesterol synthesis, the intestines’ role in absorption, and the hormonal demands of other organs all contribute to a complex system that, when out of balance, can lead to significant health and financial consequences. By understanding these biological underpinnings, individuals can make more informed decisions about their health, leading to better financial outcomes and a more secure future. Proactive health management, driven by biological understanding, is a critical component of sound personal finance.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.