Cluster headaches are not your average headaches. They are an excruciatingly painful neurological disorder characterized by recurrent, severe headaches that occur in clusters or cycles. Unlike migraines or tension headaches, cluster headaches are distinct in their intensity, duration, and specific accompanying symptoms. While the immediate thought might be of pain, understanding cluster headaches involves delving into the complex interplay of the brain, genetics, and even lifestyle factors, touching upon themes that resonate with technological advancements in diagnosis, brand recognition in healthcare, and the financial burden on individuals and the economy.
Understanding the Labyrinth of Pain: Symptoms and Triggers
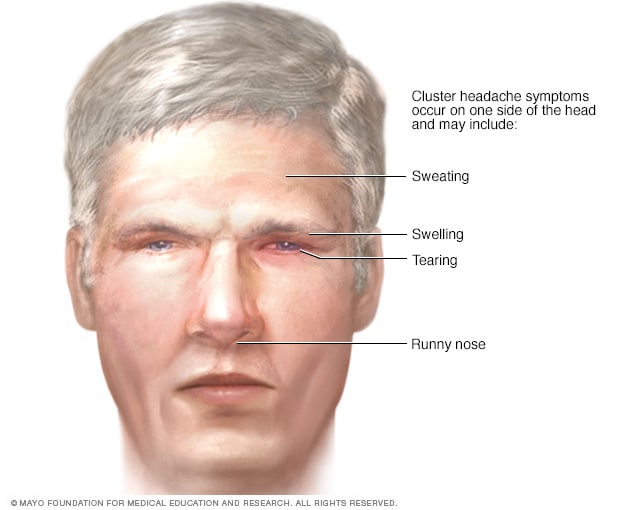
The hallmark of a cluster headache is its sheer, unadulterated pain. Described by sufferers as one of the most agonizing pain experiences known to humanity, it typically strikes one side of the head, often around or behind the eye. The pain is frequently characterized as sharp, piercing, burning, or stabbing. Unlike migraines, which can present with a gradual onset and prodromal symptoms, cluster headaches tend to erupt suddenly, reaching their peak intensity within minutes.
The excruciating pain is usually accompanied by a distinct set of autonomic symptoms on the affected side of the head. These can include:
- Conjunctival injection: Redness of the eye.
- Lacrimation: Tearing from the eye.
- Nasal congestion or rhinorrhea: Stuffy or runny nose.
- Eyelid edema: Swelling of the eyelid.
- Forehead and facial sweating: Particularly on the affected side.
- Miosis: Constriction of the pupil.
- Ptosis: Drooping of the eyelid.
These symptoms are so specific that they are often referred to as “cluster symptoms” or “autonomic features of cluster headache.” The sheer intensity of the pain can lead to restlessness and agitation, with sufferers often pacing or rocking back and forth, a stark contrast to the preference for stillness often seen in migraine sufferers.
The Distinctive Patterns: Episodic vs. Chronic
Cluster headaches manifest in two primary forms: episodic and chronic.
Episodic Cluster Headaches
Episodic cluster headaches are characterized by periods of frequent attacks, known as “cluster periods,” followed by remission periods where the headaches cease. A cluster period can last from a few weeks to several months. During these periods, attacks typically occur once to eight times a day, often at predictable times, frequently waking individuals from sleep. The attacks themselves can last from 15 minutes to three hours. The remission periods can last for months or even years, offering a welcome respite.
Chronic Cluster Headaches
In contrast, chronic cluster headaches are defined by attacks occurring frequently for more than a year without remission, or with remissions lasting less than a month. This form of the disorder presents a relentless challenge for those affected, offering little to no period of freedom from the debilitating pain.
Unraveling the Triggers: What Ignites the Fire?
While the exact cause of cluster headaches remains elusive, certain triggers are known to exacerbate or even initiate attacks. Understanding these triggers is crucial for individuals seeking to manage their condition.
- Alcohol: Even small amounts of alcohol can trigger an attack during a cluster period, making social situations particularly challenging for sufferers.
- Strong Smells: Perfumes, gasoline fumes, and other strong odors can act as triggers.
- Certain Medications: Nitroglycerin, a medication used to treat heart conditions, has been identified as a trigger in some individuals.
- Napping: Napping during the day can sometimes precipitate attacks.
- High Altitude: Changes in altitude have been reported to trigger cluster headaches.
Interestingly, the specific timing of some attacks, particularly their occurrence during the night, has led researchers to investigate the role of the hypothalamus, a region of the brain that plays a crucial role in regulating sleep-wake cycles and other circadian rhythms. This connection highlights the intricate neurological underpinnings of this condition and the potential for technological interventions in understanding and treating it.
Beyond the Pain: The Neurological and Biological Underpinnings
The genesis of cluster headaches is deeply rooted in neurological dysfunction, although the precise mechanisms are still a subject of intense research. The severity and characteristic symptoms point towards a malfunction in the hypothalamus and the trigeminal nerve, the largest cranial nerve responsible for sensory input from the face.
The Hypothalamus: The Body’s Master Clock
The hypothalamus, a small but vital part of the brain, is intricately involved in regulating a vast array of bodily functions, including hormone release, body temperature, hunger, thirst, sleep-wake cycles, and the timing of various biological processes. The cyclical nature of cluster headaches, with their predictable timing and clustering periods, strongly suggests a disruption in the hypothalamus’s ability to regulate these rhythms.
- Circadian Rhythms and Sleep: The tendency for attacks to occur at specific times, often waking individuals from sleep, implicates the hypothalamus’s role in sleep regulation. Disrupted sleep patterns or an altered internal clock are thought to play a significant role.
- Hormonal Influences: The hypothalamus also controls the release of hormones that can influence pain perception and vascular function. Imbalances in these hormonal pathways could contribute to cluster headache development.
The Trigeminal Nerve and Autonomic Nervous System
The trigeminal nerve, with its widespread innervation of the face, is centrally involved in transmitting pain signals. During a cluster headache attack, this nerve appears to become overactive, sending intense pain signals to the brain. Furthermore, the autonomic nervous system, which controls involuntary bodily functions like heart rate, digestion, and pupil dilation, is directly implicated through the cluster symptoms like tearing and nasal congestion.

- Trigeminal Autonomic Cephalgias (TACs): Cluster headaches are classified as a type of Trigeminal Autonomic Cephalgia (TAC), a group of headache disorders characterized by unilateral head pain accompanied by ipsilateral cranial autonomic symptoms. This classification underscores the direct link between trigeminal nerve activation and autonomic dysfunction.
- Neuroinflammation and Vasodilation: Research suggests that during an attack, there might be a process of neuroinflammation and vasodilation (widening of blood vessels) in certain cranial structures, contributing to the pulsating, intense pain experienced.
Genetic Predisposition: A Family Affair?
While not strictly hereditary in a simple Mendelian fashion, there appears to be a genetic predisposition to cluster headaches. Studies have indicated that individuals with a family history of the disorder are more likely to develop it themselves. This suggests that certain genetic variations may increase an individual’s susceptibility to the neurological dysfunctions that lead to cluster headaches.
- Investigating Genetic Markers: Ongoing research aims to identify specific genes or gene mutations associated with cluster headaches, which could pave the way for more targeted diagnostic tools and potential treatments.
The intricate neurological pathways and biological processes involved highlight the complexity of cluster headaches and underscore the need for sophisticated diagnostic tools and a multi-faceted approach to treatment.
Navigating the Landscape: Diagnosis and Treatment Strategies
The diagnosis of cluster headaches relies heavily on a thorough clinical evaluation and the patient’s detailed description of their symptoms and attack patterns. While there are no definitive diagnostic tests, other conditions must be ruled out.
Diagnostic Approaches: Piecing Together the Puzzle
A neurologist will typically conduct a comprehensive interview, gathering information about the frequency, duration, intensity, and associated symptoms of the headaches. They will also inquire about family history and potential triggers.
- Neurological Examination: A physical and neurological examination helps assess for any underlying neurological deficits that might suggest other conditions.
- Imaging Studies: In some cases, particularly when the diagnosis is uncertain or other neurological issues are suspected, imaging studies such as MRI or CT scans of the brain may be performed to rule out structural abnormalities, tumors, or vascular issues that could be causing similar symptoms.
- Excluding Other Conditions: It’s crucial to differentiate cluster headaches from other headache types like migraines, tension headaches, and secondary headaches caused by other medical conditions. The characteristic autonomic symptoms and the unique pain profile are key differentiating factors.
Treatment Strategies: Seeking Relief and Remission
The treatment of cluster headaches is multifaceted and aims to provide immediate relief during an attack and to prevent future attacks.
Acute Treatment: Quelling the Storm
The primary goal of acute treatment is to stop an ongoing attack as quickly as possible.
- High-Flow Oxygen Therapy: Inhaling pure oxygen through a mask at a high flow rate is one of the most effective and rapidly acting acute treatments for cluster headaches. It is thought to work by constricting blood vessels in the brain.
- Triptans: These medications, commonly used for migraines, can also be effective for cluster headaches. They are typically administered as injections or nasal sprays for faster absorption. Sumatriptan is a commonly prescribed triptan for cluster headache.
- Local Anesthetics: In some cases, intranasal lidocaine can provide relief for certain individuals.
Preventive Treatment: Building a Shield
Preventive treatments are initiated to reduce the frequency and severity of attacks during a cluster period.
- Verapamil: This calcium channel blocker is considered a first-line preventive medication for cluster headaches. It helps to stabilize nerve cell activity and reduce the frequency of attacks.
- Corticosteroids: Medications like prednisone can be used for short periods to quickly suppress attacks at the beginning of a cluster period, but they are not suitable for long-term use due to potential side effects.
- Lithium: In some cases, lithium, a mood stabilizer, may be prescribed for chronic cluster headaches.
- Nerve Blocks: Injections of local anesthetics and steroids into specific nerves, such as the occipital nerve, can provide relief for some individuals.
- Newer Treatments: Research is ongoing, and newer medications and treatment modalities, including those targeting specific neurotransmitters, are being investigated.

The Role of Lifestyle and Emerging Technologies
While not a cure, certain lifestyle adjustments can play a supportive role in managing cluster headaches. Avoiding known triggers, maintaining a regular sleep schedule, and managing stress are all important.
The journey of understanding and treating cluster headaches is continually evolving, with advancements in technology playing an increasingly vital role.
- AI-Powered Diagnostic Tools: Artificial intelligence is being explored for its potential to analyze vast datasets of patient symptoms and medical history to identify patterns and aid in earlier and more accurate diagnosis, potentially even predicting cluster periods.
- Wearable Technology: Smartwatches and other wearable devices are being developed to monitor physiological signals that might precede or accompany cluster headache attacks, offering individuals more proactive management strategies.
- Advanced Imaging Techniques: Innovations in neuroimaging allow for a more detailed understanding of the brain structures and pathways involved in cluster headaches, leading to the identification of new therapeutic targets.
- Digital Health Platforms: Online platforms and apps are becoming instrumental in helping individuals track their headache patterns, manage medications, and connect with support communities, contributing to a more informed and empowered patient experience.
The brand recognition and trust in specialized neurology clinics and research institutions are paramount for individuals seeking expert care. The financial implications of chronic cluster headaches are also significant, encompassing healthcare costs, lost productivity, and the overall impact on an individual’s quality of life. Understanding these broader implications is crucial for developing comprehensive support systems and driving further research.
In conclusion, cluster headaches represent a profound neurological challenge, characterized by intense, debilitating pain and a complex interplay of biological factors. While the exact cause remains a subject of ongoing investigation, advancements in technology, a growing understanding of the brain’s intricate workings, and a concerted effort in research are paving the way for more effective diagnosis and treatment, offering hope for those who endure this relentless condition.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.