For decades, the medical community viewed pain as a simple “alarm” system—a direct wire from a stubbed toe to the brain. However, as our understanding of neuroscience has evolved alongside leaps in high-performance computing and medical technology, we have discovered that pain is not a single sensation, but a complex, multi-dimensional construct. To answer the question of what part of the brain controls pain, we must look beyond biology and into the realm of neurotech, where software, hardware, and artificial intelligence are mapping the “pain matrix” with unprecedented precision.

In the modern tech landscape, pain is no longer just a biological mystery; it is a data problem. By identifying the specific neural circuits involved in pain perception, developers and engineers are creating digital therapeutics (DTx) and neural interfaces that promise to revolutionize how we manage chronic conditions without the need for systemic pharmacology.
The Biological Blueprint: How Technology Maps the Pain Matrix
To understand the tech-driven future of pain management, we must first define the hardware it interacts with: the human brain. There is no single “pain center” in the brain. Instead, pain is governed by a distributed network known as the “pain matrix.” Technology, specifically advanced neuroimaging, has been the primary tool in identifying the distinct roles of these regions.
fMRI and PET Scans: Visualizing the Unseen
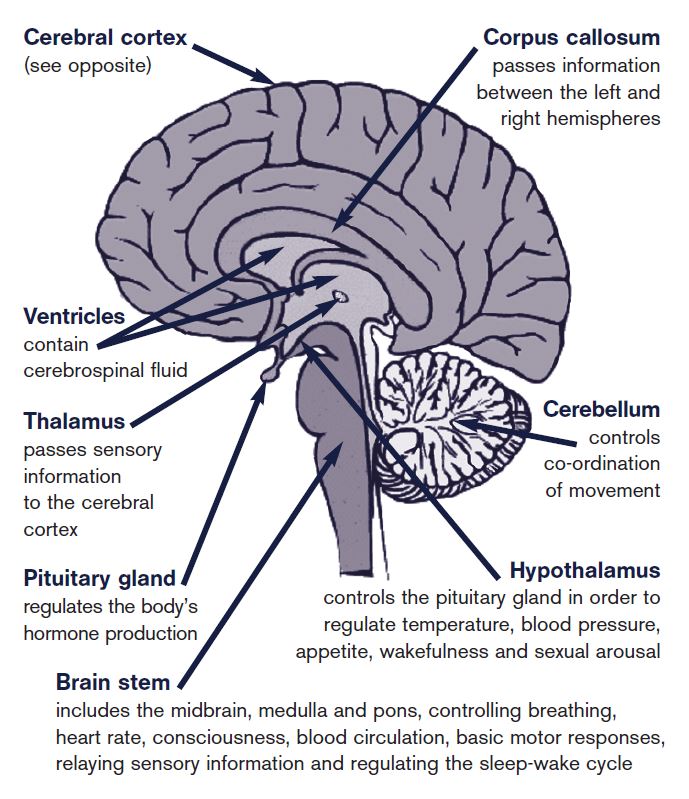
Functional Magnetic Resonance Imaging (fMRI) and Positron Emission Tomography (PET) have allowed tech-focused researchers to see the brain in action. These tools measure blood flow and metabolic activity, identifying which regions ignite when a patient experiences discomfort. Through high-resolution imaging, we have identified that the Thalamus acts as the brain’s grand relay station. It receives raw signals from the peripheral nervous system and decides where to send them for processing. Without the Thalamus, the “data” of pain would never reach the consciousness of the user.
The Role of the Somatosensory Cortex and the ACC
Once the Thalamus relays the signal, the Somatosensory Cortex (specifically areas S1 and S2) decodes the location and intensity of the pain—the “where” and “how much.” However, the technological interest often lies in the Anterior Cingulate Cortex (ACC) and the Insula. These areas control the emotional and “unpleasantness” aspect of pain. Tech developers are particularly focused on these regions because they represent the psychological software of pain, which can be modulated through digital interventions like biofeedback and Virtual Reality (VR).
Neural Interfaces and the Decoupling of Chronic Pain
As we identify the parts of the brain that control pain, the next frontier in technology is the development of Brain-Computer Interfaces (BCI) and neurostimulation devices. These technologies aim to “hack” the neural pathways to interrupt pain signals before they reach the conscious mind.
Brain-Computer Interfaces (BCI): Rerouting Neural Signals
Companies like Neuralink and Synchron are exploring how BCI technology can interface directly with the motor and sensory cortices. For patients with phantom limb pain or chronic neuropathic conditions, the brain often misfires, creating pain signals in the absence of a physical stimulus. BCI hardware can detect these aberrant firing patterns in real-time. By utilizing machine learning models, these devices can eventually learn to “cancel out” the noise, effectively acting as a digital firewall for the brain’s pain centers.
Neurostimulation: The Hardware Solution to Chronic Suffering
Spinal Cord Stimulation (SCS) and Deep Brain Stimulation (DBS) are two of the most successful tech applications in this niche. DBS involves the surgical implantation of electrodes into specific parts of the brain, such as the Periaqueductal Gray (PAG). By delivering precise electrical pulses, these devices can trigger the release of endogenous opioids or inhibit the Thalamus from passing pain signals upward. This is the ultimate example of “hardware-as-medicine,” where a lithium-ion powered device replaces a chemical prescription.
AI and Predictive Analytics: Decoding the Subjective Experience
One of the greatest challenges in treating the brain’s pain centers is the subjectivity of the experience. Pain cannot be measured like blood pressure. However, Artificial Intelligence (AI) is changing the game by turning subjective reports into objective data.

Machine Learning Algorithms as Diagnostic Tools
Artificial Intelligence is now being used to analyze EEG (electroencephalogram) patterns to create “pain biomarkers.” By feeding thousands of brain scans into a neural network, AI can identify the specific “signature” of chronic pain in the Prefrontal Cortex. This allows tech-enabled clinics to diagnose the severity of a patient’s condition without relying on the traditional 1-10 pain scale. These algorithms can differentiate between “nociceptive pain” (physical damage) and “nociplastic pain” (the brain’s nervous system malfunctioning), ensuring that the correct technological or medical intervention is applied.
Digital Biomarkers: Moving Beyond the Clinic
Wearable technology is the frontline of pain data collection. Smartwatches and rings now track heart rate variability (HRV), sleep patterns, and galvanic skin response—all of which are controlled by the Autonomic Nervous System, which is deeply intertwined with the brain’s pain processing units (specifically the Amygdala and Insula). By aggregating this data, AI platforms can predict “pain flares” before the user even feels them, suggesting preemptive digital interventions such as guided meditation or thermal regulation through smart devices.
Virtual Reality and the Amygdala: Rewiring the Emotional Response
The Amygdala is the part of the brain responsible for the fear and anxiety associated with pain. Chronic pain often creates a feedback loop where the fear of pain causes the brain to become hyper-vigilant, lowering the threshold for discomfort. Virtual Reality (VR) is proving to be a powerful technological tool in breaking this loop.
Therapeutic VR: Distraction as a Digital Narcotic
High-end VR headsets like the Apple Vision Pro or Meta Quest are being utilized for “Digital Sedation.” By immersing a patient in a highly engaging, 360-degree environment, the tech effectively “overloads” the Somatosensory Cortex and the Thalamus with non-painful stimuli. When the brain is busy processing a complex visual and auditory digital world, it has less “bandwidth” to process pain signals. Research shows that VR can reduce pain perception by up to 50% during acute procedures, offering a non-addictive tech alternative to traditional painkillers.
Neuroplasticity and Tech-Enabled Rehabilitation
The brain is “plastic,” meaning it can be rewired. Tech platforms are using gamified rehabilitation to exploit this. By engaging the Prefrontal Cortex through cognitive tasks while a patient is in a low-pain VR state, these platforms help the brain “unlearn” chronic pain patterns. This is the intersection of software engineering and behavioral neuroscience, aimed at permanently altering the way the brain’s pain matrix functions.
Ethical Implications and the Security of the Sentient Mind
As we develop the technology to monitor and modulate the parts of the brain that control pain, we enter a new era of digital ethics. The “Tech” niche is not just about gadgets; it is about the security and privacy of our most intimate data: our thoughts and sensations.
Data Privacy in Neurotechnology
The brain-sensing wearables and BCI devices of the future will collect “neuro-data.” If a company knows exactly how your Thalamus reacts to certain stimuli, they possess a map of your vulnerabilities. As we build tools to control pain, we must also build robust digital security frameworks to ensure that neural data is encrypted and owned by the user, not the provider.
The Future of “Neural Rights”
As tech-driven pain management becomes more common, the conversation will shift toward “Neural Rights.” This involves the right to mental privacy and the right to not have one’s brain activity manipulated by external software without informed consent. As we map the parts of the brain that control pain, we must be careful not to create a world where our sensory experiences can be “hacked” or commercialized.
Conclusion: The Convergence of Mind and Machine
The question “what part of the brain controls pain?” no longer has a purely biological answer. While the Thalamus, ACC, and Somatosensory Cortex are the physical infrastructure, the future of pain management lies in the digital tools we use to interface with them. From AI-driven diagnostics and BCI implants to therapeutic VR environments, technology is providing us with the “admin access” to the human nervous system.
By treating pain as a complex data network rather than a simple symptom, the tech industry is paving the way for a future where chronic suffering can be modulated, managed, and perhaps eventually “patched” through software updates and hardware innovations. In this new frontier, the most powerful tool for the brain is the technology we build to understand it.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.