The recent emergence and spread of the monkeypox virus (now known as mpox) has brought public health and scientific communities into sharp focus. While not a new virus, its increased global activity has sparked widespread concern and a flurry of questions. This article aims to demystify mpox, exploring its origins, how it spreads, its symptoms, and crucially, what steps individuals and public health organizations can take to mitigate its impact. Drawing on the principles of understanding complex phenomena, much like how we dissect technological advancements or analyze brand strategies, we will break down the multifaceted nature of this viral illness.
Understanding the Mpox Virus: Origins and Evolution
Mpox is a zoonotic disease, meaning it can be transmitted from animals to humans. It is caused by the monkeypox virus, a member of the Orthopoxvirus genus, which also includes smallpox and vaccinia virus. Historically, mpox has been endemic in West and Central Africa, with sporadic outbreaks reported in these regions. The virus is believed to have originated in rodents, such as squirrels and rats, which then transmit it to monkeys. Humans typically contract the virus through direct contact with an infected animal’s blood, bodily fluids, or lesions, or by consuming undercooked meat from an infected animal.
The current global outbreak, which gained significant attention in 2022, represented a departure from previous patterns. Unlike earlier outbreaks that were largely confined to endemic regions and often linked to animal-to-human transmission, the 2022 surge saw a significant number of cases spread through human-to-human transmission, primarily through close physical contact. This shift highlighted the virus’s potential for adaptation and efficient spread within human populations, prompting a global response akin to how the tech industry rapidly adapts to new threats or how brands pivot their strategies in response to evolving market dynamics.
The Genetic Landscape of Mpox: Clades and Transmission
The monkeypox virus exists in two distinct genetic clades: the West African clade and the Congo Basin (Central African) clade. The West African clade is generally associated with less severe illness and has a lower transmission rate compared to the Congo Basin clade. Historically, outbreaks in West Africa have been attributed to the West African clade, while the Congo Basin clade has been responsible for more severe and often fatal cases in Central Africa.
The 2022 global outbreak was primarily driven by the West African clade. However, the pattern of its spread has raised important questions about transmission dynamics. While historically associated with close contact with infected animals, the widespread human-to-human transmission observed in recent years suggests a greater efficiency in person-to-person spread than previously understood. This can occur through several routes:
- Direct contact with the rash, scabs, or bodily fluids of an infected person. This is considered the most common mode of transmission in recent outbreaks. Intimate contact, including sexual contact, has been a significant factor in the spread among specific communities.
- Respiratory secretions during prolonged face-to-face contact. While less common than direct contact, prolonged close contact with someone who has mpox and is experiencing respiratory symptoms can lead to transmission.
- Touching objects, clothes, or surfaces used by an infected person. This can include bedding, towels, and clothing that have come into contact with the virus.
Understanding these transmission routes is crucial, much like understanding the user pathways for a new app or the communication channels a brand utilizes. It allows for targeted prevention efforts and public health messaging.
Recognizing the Signs: Mpox Symptoms and Progression
The incubation period for mpox typically ranges from 5 to 21 days, meaning a person can be infected for up to three weeks before showing any symptoms. The illness usually progresses through distinct stages, and it’s important to note that not everyone experiences all symptoms, and the severity can vary.
The Initial Phase: Flu-Like Symptoms
The onset of mpox often begins with non-specific, flu-like symptoms. These can include:
- Fever: A sudden elevation in body temperature.
- Headache: Often severe and persistent.
- Muscle aches (myalgia): Generalized pain and discomfort in the muscles.
- Backache: Aching in the lower back.
- Swollen lymph nodes (lymphadenopathy): This is a characteristic symptom that helps distinguish mpox from other viral illnesses like chickenpox or measles. The lymph nodes, particularly in the neck, armpits, and groin, become enlarged and tender.
- Chills: Feeling cold and shivering.
- Extreme fatigue: Profound tiredness and lack of energy.
This initial stage can last for one to a few days, and it’s during this period that an individual may be infectious, even before the characteristic rash appears.
The Dermatological Manifestation: The Mpox Rash
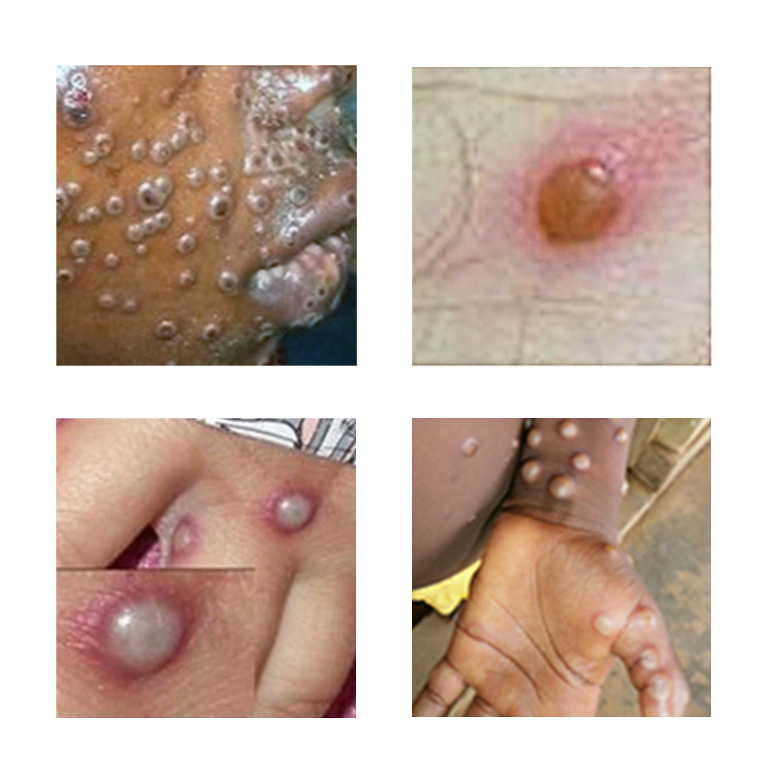
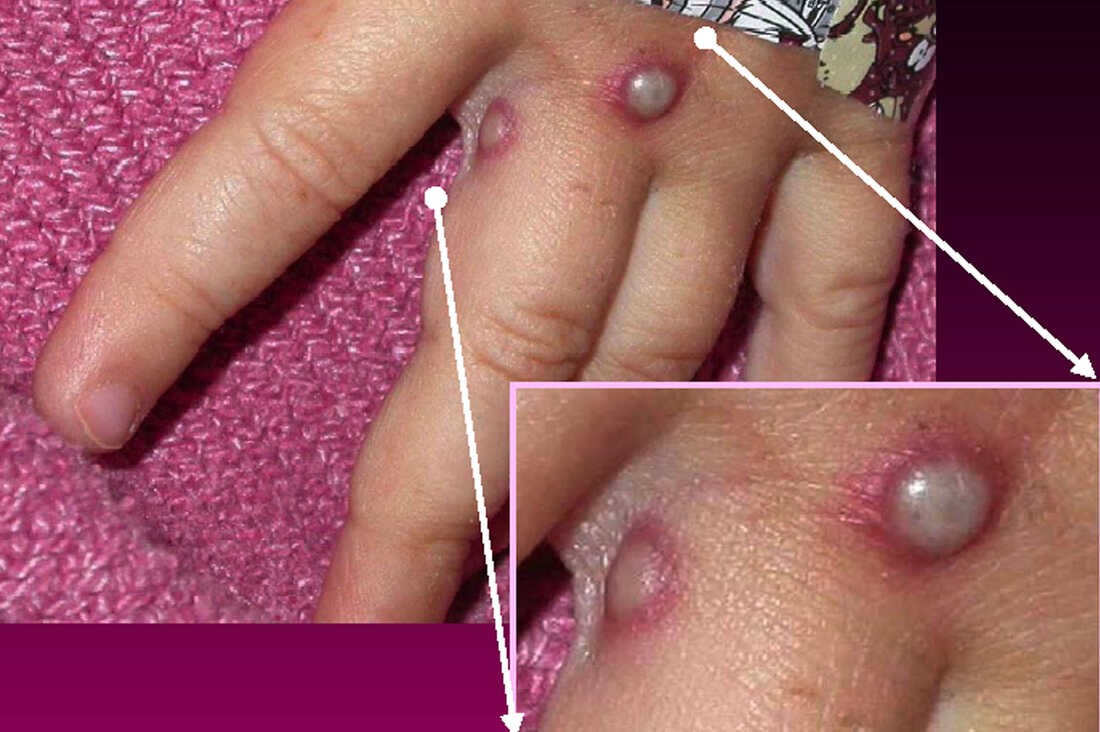
Following the initial flu-like symptoms, the hallmark of mpox emerges: a rash. This rash typically develops one to three days after the onset of fever. Its appearance and progression are key to diagnosis.
The rash usually starts as flat, red spots (macules) that gradually transform into raised bumps (papules). These papules then fill with fluid, becoming vesicles, and eventually turn into pustules, which are filled with yellowish pus. Finally, these pustules rupture, forming scabs that eventually fall off.
The distribution of the rash is another important characteristic. While it can appear anywhere on the body, it often begins on the face and then spreads to other parts of the body, including the palms of the hands, soles of the feet, mouth, genitals, and eyes. The lesions can vary in size and appearance and may be itchy or painful.
It’s crucial to understand that the rash can present differently in individuals, especially with the recent surge in cases. Some individuals may experience a limited number of lesions, or the rash might appear in different stages of development simultaneously. This variability can make early diagnosis challenging, similar to how a novel software feature might have unexpected user interaction patterns.
The Contagious Period: When is Mpox Transmissible?
An individual is considered contagious with mpox from the onset of symptoms until all the scabs have fallen off and a fresh layer of skin has formed underneath. This entire process can take anywhere from two to four weeks. During this period, close contact with an infected person, whether direct physical contact or exposure to respiratory droplets, can lead to transmission. This prolonged contagious period underscores the importance of isolation and careful hygiene practices for those infected.
Prevention and Mitigation: Strategies Against Mpox
Combating the spread of mpox requires a multi-pronged approach involving public health measures, individual responsibility, and medical interventions. Similar to how technology companies build robust security protocols or how brands implement comprehensive marketing campaigns, proactive and informed strategies are essential.
Public Health Responses: Surveillance, Testing, and Vaccination
Public health agencies play a critical role in monitoring outbreaks, identifying cases, and implementing control measures. This includes:
- Surveillance: Actively tracking the incidence and spread of mpox to understand transmission patterns and identify areas of concern. This is akin to monitoring network traffic for anomalies or tracking consumer sentiment for a brand.
- Testing: Developing and deploying rapid diagnostic tests to accurately identify mpox infections. Early and accurate diagnosis is key to prompt isolation and contact tracing.
- Contact Tracing: Identifying individuals who have been in close contact with confirmed cases and providing them with guidance on monitoring for symptoms and potential vaccination.
- Public Awareness Campaigns: Educating the public about mpox, its symptoms, transmission routes, and preventive measures. Clear and consistent communication is vital, much like a well-executed branding message.
Vaccination has emerged as a significant tool in the mpox response. Vaccines developed for smallpox have been shown to be effective in preventing or reducing the severity of mpox. Public health authorities have prioritized vaccination for individuals at higher risk of exposure, including close contacts of confirmed cases and certain occupational groups. The availability and equitable distribution of these vaccines are critical public health objectives.
Individual Responsibility: Protecting Yourself and Others
While public health measures are paramount, individual actions are equally crucial in preventing the spread of mpox.
- Awareness of Symptoms: Being aware of the signs and symptoms of mpox and seeking medical attention if you suspect an infection.
- Practicing Good Hygiene: Frequent handwashing with soap and water or using alcohol-based hand sanitizer, especially after contact with potentially infected individuals or surfaces.
- Avoiding Close Contact: Minimizing close, skin-to-skin contact with individuals who have a rash that resembles mpox.
- Safe Sex Practices: Given the role of close physical contact in transmission, engaging in safer sex practices, including open communication with partners about their health status, can reduce the risk.
- Isolation: If you are diagnosed with mpox, isolating yourself from others until you are no longer contagious is essential to prevent further spread. This involves staying home and avoiding close contact with household members and pets.

Medical Management and Treatment
Currently, there is no specific cure for mpox. However, antiviral medications used to treat smallpox can be effective in treating mpox. These are typically reserved for individuals with severe illness or those at high risk of complications. Treatment focuses on managing symptoms, preventing secondary bacterial infections, and supporting the body’s immune response. Supportive care, including pain relief, fever reduction, and wound care for the lesions, is also an important part of management.
In conclusion, understanding mpox requires a comprehensive approach. By learning about its origins, recognizing its symptoms, and actively participating in prevention strategies, individuals and communities can work together to mitigate the impact of this viral threat. As with navigating the fast-paced world of technology, the evolving landscape of brand perception, or the intricacies of personal finance, staying informed and adopting proactive measures are our strongest allies. The ongoing scientific research and public health efforts are vital in our collective endeavor to control and ultimately overcome the challenges posed by mpox.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.