Dementia with Lewy Bodies (DLB) stands as one of the most challenging and often misdiagnosed forms of dementia, characterized by a complex interplay of cognitive, motor, and psychiatric symptoms. Unlike Alzheimer’s disease, which primarily affects memory, or Parkinson’s disease, which is predominantly a motor disorder, DLB presents a unique clinical picture that bridges both worlds. Its insidious onset and fluctuating nature make accurate diagnosis difficult, often leading to delays in appropriate care and treatment. However, in an era defined by rapid technological advancements, our understanding, diagnosis, and management of DLB are being profoundly transformed. Technology is not merely an auxiliary tool; it is becoming an integral lens through which we comprehend this complex neurological condition, offering unprecedented insights and innovative solutions.

This exploration delves into how cutting-edge technologies—from artificial intelligence and advanced imaging to wearables and smart home systems—are redefining our approach to DLB. We will examine how these digital innovations are not only enhancing diagnostic accuracy and accelerating research but also empowering individuals living with DLB and their caregivers to navigate the daily challenges with greater support and insight. As we move towards an increasingly interconnected and data-driven healthcare landscape, the fusion of neurology and technology holds immense promise for illuminating the mysteries of DLB and improving countless lives.
Understanding Dementia with Lewy Bodies Through Digital Lenses
The journey to effectively manage and eventually cure DLB begins with a comprehensive understanding of its pathophysiology and clinical manifestations. Technology plays a crucial role in disseminating this knowledge and facilitating deeper insights into the disease’s mechanisms.
The Neurological Basis: A Acknowledgment of Complexity for Technological Solutions
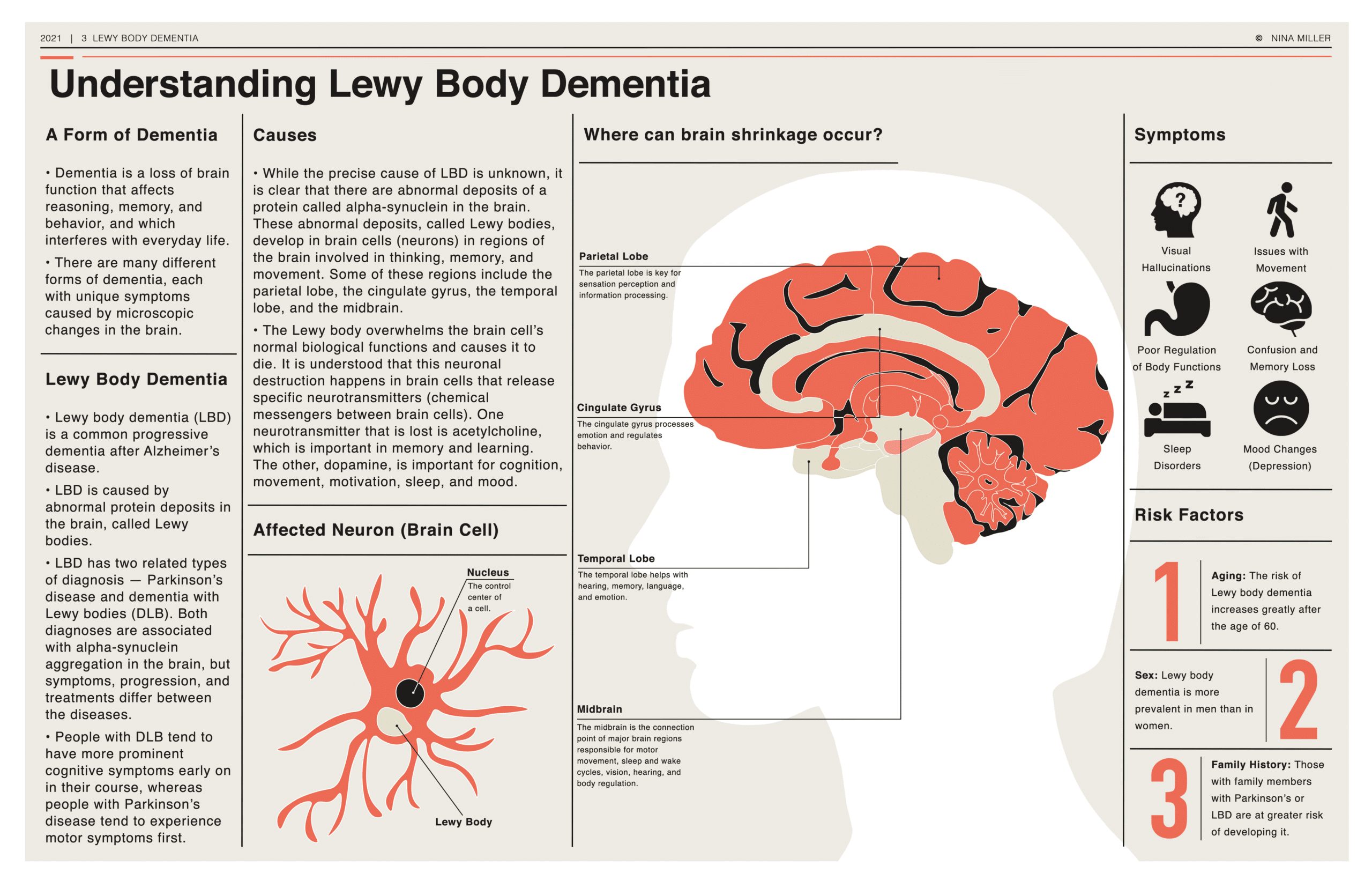
Dementia with Lewy Bodies is characterized by the abnormal accumulation of alpha-synuclein proteins into clumps called Lewy bodies within brain cells. These deposits disrupt normal brain function, leading to a spectrum of symptoms including cognitive fluctuations, recurrent visual hallucinations, and spontaneous parkinsonism (tremor, rigidity, slow movement). The diagnostic challenge lies in distinguishing DLB from Alzheimer’s disease, Parkinson’s disease dementia, and other conditions, as initial symptoms can overlap. It is precisely this complexity and the need for objective, quantifiable data that invite technological intervention. Digital platforms, advanced imaging, and data analytics become essential tools in unraveling these intricate neurological puzzles.
Bridging the Information Gap with Digital Platforms
For patients, caregivers, and even healthcare professionals, accessing accurate and up-to-date information about DLB can be daunting. Digital platforms have emerged as indispensable resources, democratizing access to knowledge and support. Online health portals, specialized forums, and dedicated mobile applications provide comprehensive educational materials, symptom trackers, and shared experiences from a global community. Telehealth services have also revolutionized the initial assessment and ongoing consultation processes, particularly for individuals in remote areas or those with mobility challenges. Through secure video conferencing, neurologists and specialists can conduct preliminary evaluations, monitor progress, and offer guidance, significantly reducing the burden of travel and improving access to expert care. These digital conduits ensure that vital information and support systems are just a click or tap away, fostering informed decision-making and enhancing patient engagement.
Imaging Technologies for Enhanced Visualization
Neuroimaging has long been a cornerstone of neurological diagnosis, but recent advancements, coupled with sophisticated computational analysis, are providing unprecedented clarity in diagnosing DLB. Traditional MRI scans help rule out other conditions like strokes or tumors, but specialized techniques offer more specific insights. SPECT (Single-Photon Emission Computed Tomography) and PET (Positron Emission Tomography) scans, particularly those targeting dopamine transporters (DaTscans), are invaluable. DaTscans, for instance, can detect the loss of dopamine-producing neurons, a hallmark of DLB and Parkinson’s disease, helping differentiate them from Alzheimer’s. The crucial “digital lens” here is the software that processes, reconstructs, and analyzes the vast datasets generated by these scans. Advanced algorithms can highlight subtle volumetric changes, metabolic patterns, or connectivity alterations indicative of DLB, aiding clinicians in making earlier and more accurate diagnoses than ever before. This digital interpretation layer transforms raw imaging data into actionable diagnostic insights.
Leveraging AI and Machine Learning in LBD Diagnosis and Research
Artificial intelligence (AI) and machine learning (ML) are rapidly transforming the landscape of medical science, offering powerful tools to process, analyze, and interpret complex data in ways human cognition cannot. For a condition as multifaceted as DLB, these technologies hold immense promise.
AI-Powered Diagnostic Tools
The diagnostic challenges of DLB, stemming from its fluctuating symptoms and overlap with other conditions, make it an ideal candidate for AI intervention. Machine learning algorithms can analyze vast datasets comprising medical histories, neurological assessments, imaging results, genetic markers, and even subtle behavioral patterns captured by sensors. For example, AI can be trained to identify specific gait abnormalities, speech patterns, or eye-movement irregularities that are characteristic of DLB, even before they become overtly apparent to a human observer. By processing hundreds or thousands of data points per patient, AI can detect correlations and predictive markers that enhance diagnostic accuracy, potentially distinguishing DLB from Alzheimer’s or Parkinson’s disease dementia with greater precision and at earlier stages. This not only reduces diagnostic delays but also ensures patients receive appropriate interventions sooner.
Accelerating Drug Discovery and Biomarker Identification
Developing new treatments for neurological disorders is a notoriously slow and expensive process. AI and machine learning are revolutionizing drug discovery by streamlining several key stages. ML algorithms can analyze massive chemical libraries to identify potential drug candidates that might interact with specific disease pathways, like those involved in alpha-synuclein aggregation. They can predict the efficacy and toxicity of compounds in silico, significantly reducing the need for costly and time-consuming laboratory experiments. Furthermore, AI is crucial in identifying novel biomarkers—measurable indicators of a disease state. By analyzing genetic data, proteomic profiles, and imaging patterns, ML can pinpoint specific proteins, genetic variations, or brain changes that signal the presence of DLB, its progression, or its response to treatment. This data-driven approach accelerates the identification of therapeutic targets and the development of personalized medicine strategies.
Predictive Analytics for Disease Progression
Beyond diagnosis, AI’s capability in predictive analytics offers profound implications for managing DLB. By analyzing an individual’s unique data profile and comparing it against historical data from thousands of other patients, AI models can forecast the likely trajectory of the disease. This includes predicting the onset of specific symptoms (e.g., severe hallucinations, increased parkinsonism), the rate of cognitive decline, or the risk of complications like falls. Such predictive insights empower clinicians to proactively adjust treatment plans, recommend timely interventions, and prepare patients and caregivers for future challenges. For families, this foresight can be invaluable for long-term planning, care coordination, and accessing support services at critical junctures, thus enhancing the overall quality of life.
Assistive Technologies and Digital Tools for Living with LBD
Living with DLB presents daily challenges that impact independence, safety, and communication. Fortunately, a growing array of assistive technologies and digital tools are designed to mitigate these difficulties, offering practical support and enhancing the quality of life for both individuals with DLB and their caregivers.
Cognitive Support and Memory Aids
One of the defining features of DLB is fluctuating cognition, making memory and organization particularly challenging. Digital memory aids and cognitive support apps can significantly help. These include smart calendars with automated reminders for medication, appointments, and daily tasks, often integrated with voice assistants that can be easily queried. Specialized apps can help with task sequencing, breaking down complex activities into manageable steps. Voice recorders can capture important conversations, while digital photo albums with descriptive tags can aid memory recall. These tools are designed to be user-friendly, often with simplified interfaces, helping individuals maintain a semblance of routine and independence while minimizing frustration.
Enhancing Safety and Security through Smart Homes
The fluctuating nature of DLB symptoms, including visual hallucinations and motor difficulties, can pose significant safety risks such as wandering, falls, or confusion. Smart home technologies offer an intelligent layer of protection and monitoring. IoT (Internet of Things) devices like smart sensors can detect if a person gets out of bed at unusual times, opens doors, or enters restricted areas, sending alerts to caregivers. Motion sensors can turn lights on automatically to prevent falls in poorly lit areas. GPS trackers, often integrated into wearable devices or shoes, provide peace of mind by allowing caregivers to locate individuals who may wander. Smart cameras with privacy features can monitor activity in common areas without being overly intrusive, while smart locks can provide enhanced security. These systems empower caregivers to maintain a safe environment while respecting the individual’s dignity and desire for independence.
Communication and Social Connection Tools
Social isolation can be a significant issue for individuals with DLB and their caregivers. Digital communication tools can help bridge this gap. Video conferencing platforms allow families and friends to connect face-to-face, even across long distances, fostering a sense of connection and reducing loneliness. Simpler interfaces for tablets or smart displays can make video calls more accessible for those with cognitive impairments. Social media platforms, when managed appropriately, can also serve as channels for maintaining relationships and sharing updates. Furthermore, specialized communication apps designed for individuals with speech difficulties or cognitive challenges can provide augmented communication support, enabling them to express their needs and preferences more effectively, thereby enhancing social engagement and reducing feelings of isolation.
The Role of Wearables and IoT in Monitoring and Care
Wearable technology and the Internet of Things (IoT) are revolutionizing personal health monitoring, offering continuous, real-time data that can provide invaluable insights into the daily lives and health status of individuals with DLB. These discreet devices transform passive observation into active, data-driven care.
Continuous Health Monitoring
Smartwatches, fitness trackers, and smart patches are no longer just for fitness enthusiasts; they are powerful tools for continuous health monitoring in clinical settings and at home. For individuals with DLB, these devices can track vital signs like heart rate, sleep patterns, and oxygen saturation. Crucially, they can also monitor activity levels, gait speed, and detect subtle tremors or changes in movement patterns indicative of parkinsonism symptoms. The data collected provides a comprehensive, objective record of how symptoms fluctuate throughout the day, offering a much more accurate picture than intermittent clinical assessments or subjective self-reports. This continuous stream of data helps identify patterns, triggers, and the effectiveness of medications.
Remote Patient Monitoring and Telehealth Integration
The data harvested from wearables and IoT devices can be seamlessly integrated into remote patient monitoring (RPM) platforms. This allows healthcare providers to access real-time information about their patients’ health status from a distance. For individuals with DLB, this means clinicians can monitor changes in gait, sleep disturbances, or activity levels, potentially identifying symptom exacerbations or adverse drug reactions much earlier. RPM, combined with telehealth, facilitates proactive care adjustments. A doctor could review a week’s worth of sleep data showing increased restlessness and adjust medication remotely, or initiate a telehealth consultation based on changes in activity patterns. This reduces the need for frequent in-person clinic visits, which can be stressful for individuals with DLB, while ensuring continuous and responsive care.
Data-Driven Insights for Personalized Care
The aggregation of data from various IoT devices and wearables provides a holistic view of an individual’s daily life, environment, and health fluctuations. This rich dataset allows for truly personalized care. By analyzing how different environmental factors (e.g., light levels, noise), activities, or medication timings correlate with symptom severity, caregivers and clinicians can develop highly tailored strategies. For example, if data shows increased agitation during certain times of day or in specific settings, interventions can be implemented to modify those conditions. This data-driven approach moves beyond a one-size-fits-all model, enabling care plans that are specifically designed to meet the unique and changing needs of each individual with DLB, enhancing comfort, safety, and overall well-being.
Future Frontiers: Big Data, Neurotech, and Personalized Medicine for LBD
The rapid pace of technological innovation suggests that the future holds even more transformative possibilities for understanding and treating DLB. Emerging fields like big data analytics, advanced neurotechnology, and precision medicine promise to push the boundaries of what is currently achievable.
The Promise of Big Data and Data Lakes
The exponential growth of health data—from electronic health records and clinical trials to genomic sequences and real-world data from wearables—is creating unprecedented opportunities. “Big data” refers to the ability to collect, store, and analyze these massive, diverse datasets. For DLB, this means creating “data lakes” that pool information from thousands, or even millions, of individuals worldwide. By applying advanced analytical techniques to these vast reservoirs of information, researchers can identify subtle genetic predispositions, environmental risk factors, and complex disease patterns that are impossible to discern from smaller, isolated studies. This comprehensive approach is crucial for uncovering the underlying mechanisms of DLB, identifying novel subtypes of the disease, and discovering entirely new avenues for intervention.
Advancements in Neurotechnology
Neurotechnology, which involves devices and methods to interact with the nervous system, is an exciting frontier. While still largely experimental for DLB, techniques like non-invasive brain stimulation (e.g., Transcranial Magnetic Stimulation – TMS, or transcranial Direct Current Stimulation – tDCS) are being explored for their potential to modulate brain activity and improve cognitive or motor symptoms in various neurological conditions. Though not yet standard for DLB, future research may identify specific stimulation protocols that could help manage symptoms like hallucinations or cognitive fluctuations. More futuristic concepts, such as advanced brain-computer interfaces (BCIs), which allow direct communication between the brain and external devices, could one day offer profound ways to restore function or facilitate communication, although their application in complex conditions like DLB is a distant prospect. Nevertheless, these developments highlight the potential for technology to directly intervene and modify neurological processes.

Towards Precision Medicine
The ultimate goal in the treatment of complex diseases like DLB is personalized medicine—an approach that tailors medical treatment to each patient’s individual characteristics. Enabled by advancements in genomics, proteomics, and sophisticated data analytics, precision medicine for DLB aims to move beyond a “one-size-fits-all” approach. By analyzing an individual’s unique genetic makeup, protein profiles, and specific biomarkers, clinicians will be able to predict their response to particular medications, anticipate disease progression, and select therapies that are most likely to be effective with the fewest side effects. Imagine a future where a simple blood test or brain scan, analyzed by AI, can determine not just that you have DLB, but precisely which subtype you have, what treatments you will respond to best, and how your disease will likely evolve. This highly individualized approach, driven by technology and big data, holds the key to developing truly effective and targeted interventions for Dementia with Lewy Bodies, offering hope for a future with improved outcomes and a better quality of life for those affected.
In conclusion, while Dementia with Lewy Bodies presents formidable challenges, the relentless march of technological innovation offers a beacon of hope. From enhancing our fundamental understanding and refining diagnostic accuracy to providing practical tools for daily living and paving the way for personalized therapies, technology is fundamentally reshaping our fight against DLB. As these digital frontiers continue to expand, they promise not only to demystify this complex condition but also to empower patients, support caregivers, and ultimately lead us closer to effective treatments and a future where DLB is better understood, managed, and perhaps, even cured.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.