High intraocular pressure (IOP), often referred to as ocular hypertension, is a critical concern within the realm of eye health, directly impacting visual function and potentially leading to irreversible vision loss. Understanding what constitutes “dangerously high” IOP is paramount for proactive management and timely intervention. This article delves into the diagnostic parameters, risk factors, and technological advancements that help define and address elevated eye pressure, ensuring that individuals and healthcare providers are equipped with the knowledge to safeguard vision.
Understanding Intraocular Pressure: The Foundation of Eye Health
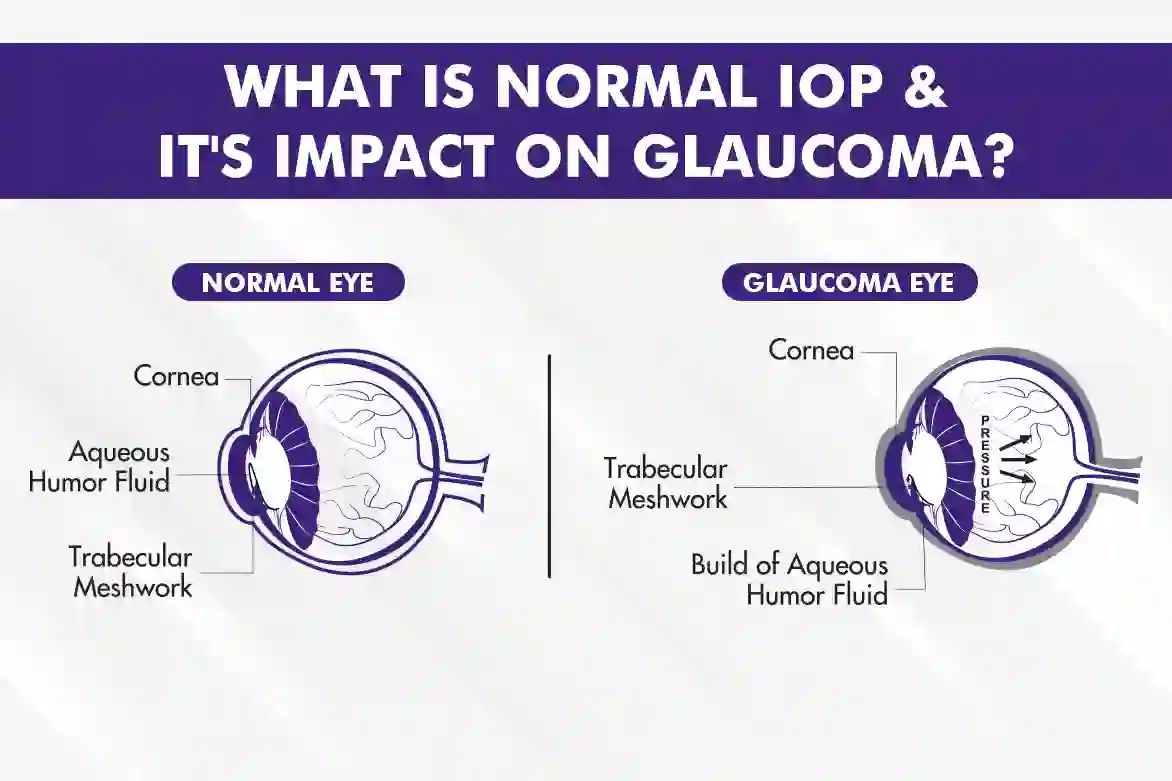
Intraocular pressure is the fluid pressure inside the eye. This pressure is maintained by a delicate balance between the production and drainage of a fluid called aqueous humor. Aqueous humor is continuously produced by the ciliary body and drains out of the eye through the trabecular meshwork, located in the angle where the iris meets the cornea. When this balance is disrupted, either due to overproduction or impaired drainage of aqueous humor, IOP can rise.
The Normal Range of Intraocular Pressure
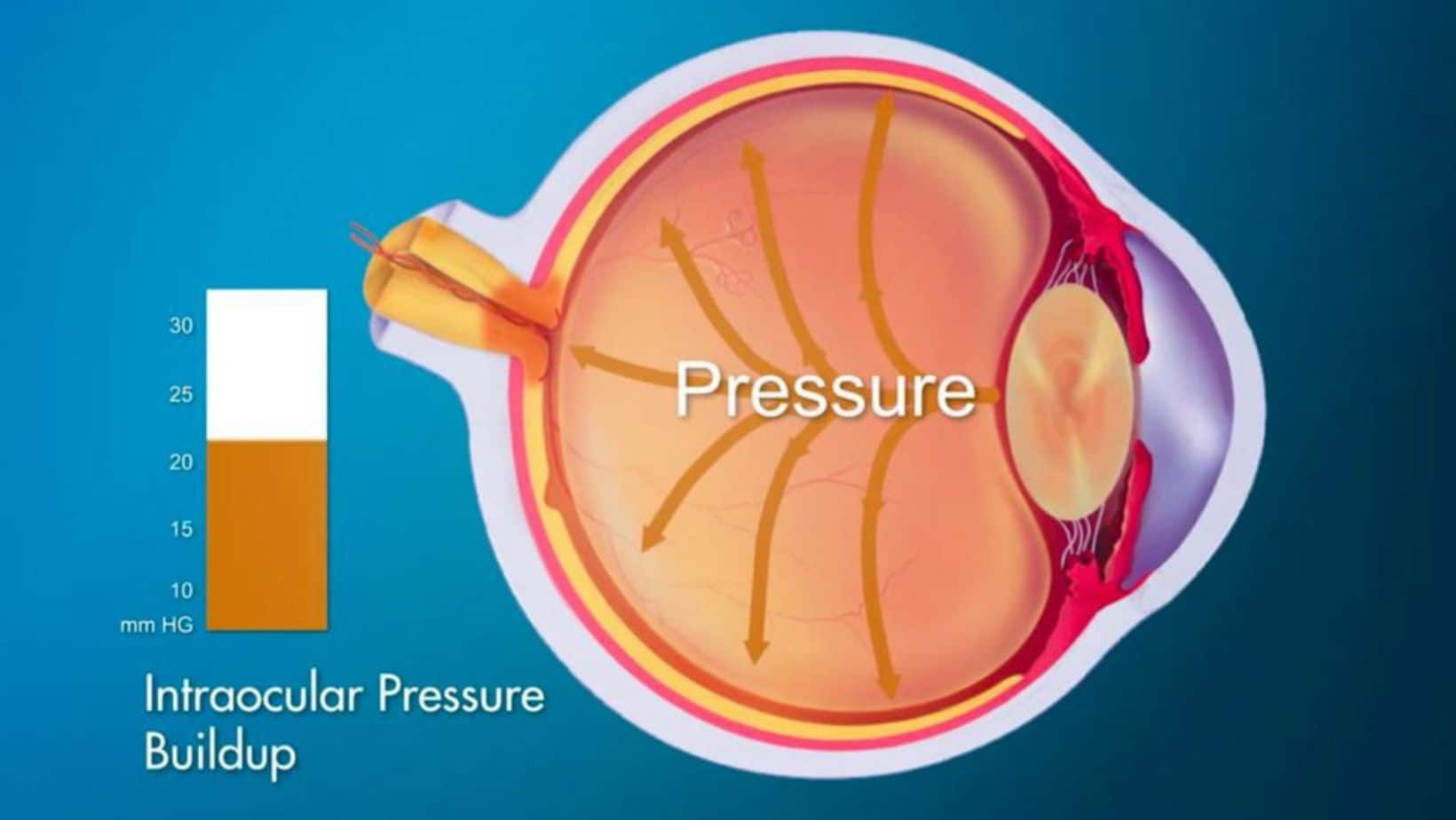
The widely accepted normal range for IOP is typically between 10 and 21 millimeters of mercury (mmHg). This range is based on statistical analysis of large populations and represents the pressure levels at which the risk of optic nerve damage (glaucoma) is generally low. However, it is crucial to understand that this is a range, and individual variations exist. Some individuals may have IOP consistently at the higher end of the normal range (e.g., 19-21 mmHg) without developing glaucoma, while others might experience optic nerve damage at pressures within this “normal” range. This latter condition is often referred to as normal-tension glaucoma.
Factors Influencing Intraocular Pressure
Several factors can influence IOP, some of which are transient and others that contribute to chronic elevation.
Physiological Factors
- Diurnal Variations: IOP naturally fluctuates throughout the day, generally being higher in the morning and lower in the evening. These variations are usually within a few mmHg and are not cause for concern.
- Age: While not a direct cause, the risk of developing conditions that lead to elevated IOP increases with age.
- Genetics: A family history of glaucoma or ocular hypertension significantly increases an individual’s risk. Certain genetic predispositions can affect the structure of the eye or the drainage system.
- Race and Ethnicity: Certain ethnic groups have a higher prevalence of specific types of glaucoma. For instance, individuals of African descent are at higher risk for primary open-angle glaucoma, while those of East Asian descent have a higher risk for primary angle-closure glaucoma.
Lifestyle and Medical Factors
- Medications: Systemic corticosteroids, particularly when taken orally or inhaled for extended periods, are a well-known cause of steroid-induced glaucoma, leading to IOP elevation. Certain other medications can also impact IOP.
- Eye Trauma: Injury to the eye can disrupt the drainage system, leading to either immediate or delayed increases in IOP.
- Certain Medical Conditions: Conditions such as diabetes, hypertension, and hypothyroidism can be associated with an increased risk of developing ocular hypertension or glaucoma.
- Eye Surgery: Previous eye surgeries can sometimes affect the normal fluid dynamics of the eye, leading to IOP changes.
Defining Dangerously High Eye Pressure: Thresholds and Risks
While the 10-21 mmHg range is considered normal, “dangerously high” eye pressure is a dynamic concept that considers not just the numerical value but also the presence of other risk factors and signs of optic nerve damage.
IOP Levels Requiring Close Monitoring and Potential Intervention
Generally, an IOP reading above 21 mmHg is considered elevated and warrants further investigation. However, the threshold for “dangerously high” is more nuanced and is often defined in the context of an individual’s overall risk profile.
- Ocular Hypertension: An IOP of 21 mmHg or higher without any detectable optic nerve damage or visual field loss is termed ocular hypertension. While not immediately dangerous, individuals with ocular hypertension have a significantly higher risk of developing glaucoma compared to those with normal IOP.
- High-Risk Ocular Hypertension: An IOP consistently above 21 mmHg, especially when combined with other risk factors like thin corneas, advanced age, or a family history of glaucoma, pushes the definition towards “dangerously high” and necessitates aggressive management.
- Glaucoma with High IOP: When high IOP is accompanied by characteristic optic nerve damage (e.g., cupping of the optic disc) and/or visual field loss, it is unequivocally considered a serious and dangerous condition. The higher the IOP and the more advanced the damage, the greater the risk of rapid and irreversible vision loss.
The Significance of Optic Nerve Health
The optic nerve is the conduit that transmits visual information from the retina to the brain. Elevated IOP is the primary, though not the only, risk factor for glaucoma, a condition that damages the optic nerve.
Optic Nerve Damage (Glaucoma)
- Cupping: In glaucoma, the optic nerve head can develop a characteristic “cupping” – an enlargement and deepening of the central depression. The ratio of the cup to the disc size (cup-to-disc ratio) is an important indicator of optic nerve damage. A significantly enlarged or asymmetric cup-to-disc ratio, especially when coupled with high IOP, is a warning sign.
- Nerve Fiber Layer Loss: Glaucoma also causes a loss of retinal nerve fiber layer, which can be detected with specialized imaging techniques.
Visual Field Loss
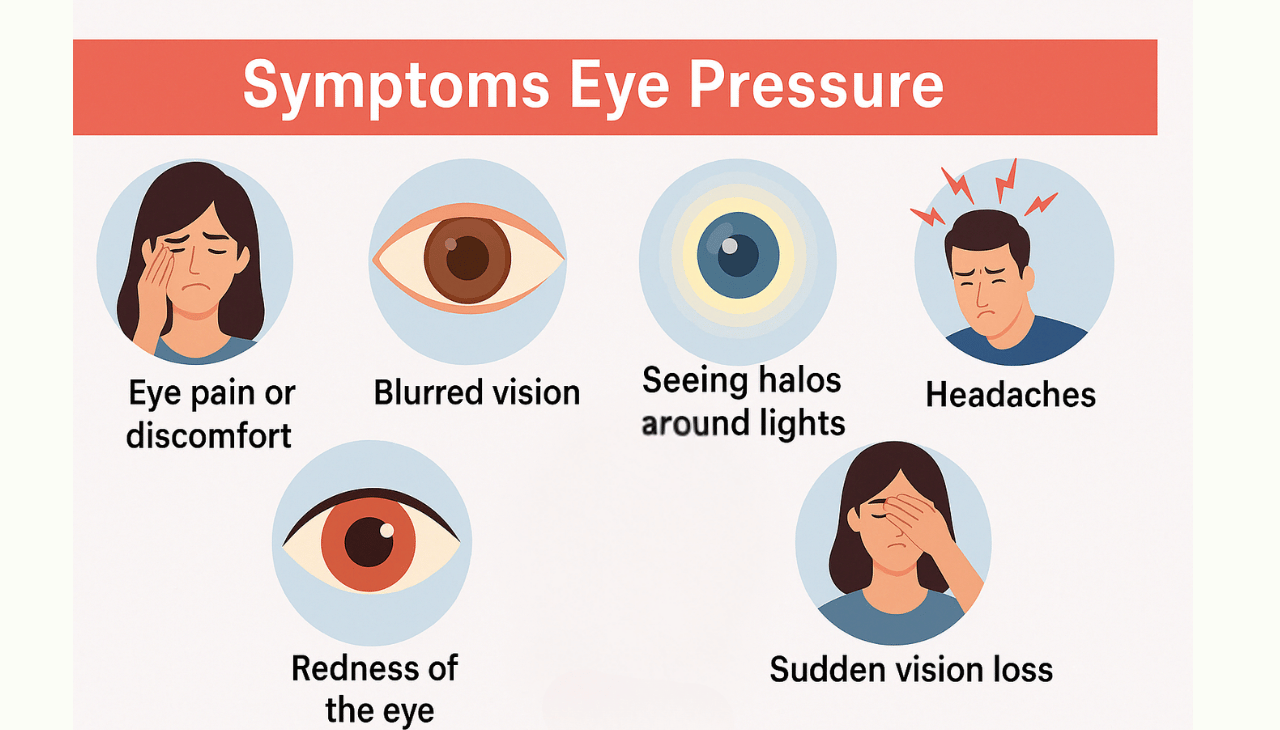
As the optic nerve becomes progressively damaged, blind spots (scotomas) begin to appear in the peripheral vision. Initially, these are often unnoticed as the brain compensates. However, as the condition advances, these blind spots can enlarge and even encroach upon central vision, leading to significant impairment.
Technological Advancements in Detecting and Managing High Eye Pressure
Modern ophthalmology leverages sophisticated technologies to accurately measure IOP, assess optic nerve health, and monitor treatment efficacy, playing a crucial role in identifying and managing “dangerously high” eye pressure.
Advanced IOP Measurement Techniques
While the Goldmann applanation tonometer remains the gold standard for IOP measurement, other devices offer complementary information and ease of use.
- Goldmann Applanation Tonometer (GAT): This device, used with a slit lamp, measures the force required to flatten a small area of the cornea. It is considered the most accurate and reliable method when used correctly.
- Non-Contact Tonometry (NCT) / Air-Puff Tonometry: These devices use a puff of air to flatten the cornea. While convenient and quick, they can be less accurate than GAT, especially in cases of corneal abnormalities.
- Icare® Tonometer: This handheld device uses a rebound tonometer technology, which measures IOP by bouncing a small probe off the cornea. It is portable and can be used without anesthetic drops, making it useful in various settings.
- Pascals® Tonometer: This device measures IOP in a different way, by assessing the pressure required to oscillate a small probe within the cornea. It is considered less affected by corneal properties than applanation tonometry.
Imaging and Diagnostic Tools for Optic Nerve Assessment
Beyond IOP measurements, advanced imaging techniques are indispensable for detecting and quantifying optic nerve damage, crucial for defining “dangerously high” pressure in the context of glaucoma.
- Optical Coherence Tomography (OCT): OCT is a non-invasive imaging technique that provides cross-sectional views of the retina and optic nerve. It allows for precise measurement of the retinal nerve fiber layer thickness and analysis of the optic disc’s morphology. OCT is invaluable for detecting early signs of glaucomatous damage, even before visual field loss becomes apparent, and for monitoring disease progression.
- Heidelberg Retina Tomograph (HRT): HRT uses confocal scanning laser technology to create a 3D map of the optic disc. It measures various parameters of the optic nerve head and can detect subtle changes over time that may indicate progressive damage.
- Visual Field Testing (Perimetry): This functional test assesses an individual’s peripheral and central vision. It helps detect blind spots caused by optic nerve damage and monitors the progression of visual field loss, a key indicator of glaucoma’s impact on sight. Automated perimetry, such as Humphrey Field Analyzer, is the standard.
Future Directions and Emerging Technologies
The field of ophthalmology is continuously evolving, with new technologies promising even more precise diagnosis and personalized treatment for elevated eye pressure.
- AI-Powered Diagnostics: Artificial intelligence is increasingly being integrated into diagnostic software to analyze OCT scans and visual field tests. AI algorithms can detect subtle patterns of damage that might be missed by the human eye, leading to earlier and more accurate diagnoses.
- Advanced Biomarkers: Research is ongoing to identify biomarkers in tears or aqueous humor that could indicate an increased risk of glaucoma or predict response to treatment.
- Minimally Invasive Glaucoma Surgery (MIGS): While not directly diagnostic, advancements in MIGS offer less invasive surgical options for lowering IOP in certain cases, often performed concurrently with cataract surgery.
Risk Factors and Personalized Management of High Eye Pressure
Identifying individuals at risk for dangerously high eye pressure allows for proactive screening and personalized management strategies. The definition of “dangerously high” is not a universal number but is tailored to the individual’s specific risk profile.
Cumulative Risk Assessment
The management of elevated IOP is not solely based on a single IOP reading. Ophthalmologists consider a constellation of factors to determine the level of risk and the urgency of intervention.
- Family History: A strong family history of glaucoma significantly elevates an individual’s risk of developing the condition, even with seemingly normal IOP.
- Age: As mentioned, the risk of glaucoma increases with age, particularly after 40. Regular eye exams become more critical with advancing years.
- Corneal Thickness (Pachymetry): Thinner corneas can lead to underestimation of IOP by certain tonometry methods, making individuals with thin corneas more susceptible to optic nerve damage at a given pressure reading. Conversely, thicker corneas can overestimate IOP.
- Presence of Optic Nerve Changes: Even if IOP is within the “normal” range, the presence of existing optic nerve damage or suspicious changes warrants cautious monitoring and potentially treatment.
- Diabetes and Hypertension: These systemic conditions can exacerbate optic nerve damage and influence the progression of glaucoma.
Treatment Modalities for Lowering Intraocular Pressure
When IOP is deemed dangerously high, either due to elevated levels alone or in combination with risk factors and optic nerve damage, treatment is initiated to lower the pressure and prevent further vision loss.
- Medicated Eye Drops: This is the most common initial treatment. Various classes of eye drops work by either reducing the production of aqueous humor or increasing its drainage. Examples include prostaglandin analogs, beta-blockers, alpha-adrenergic agonists, and carbonic anhydrase inhibitors.
- Laser Therapy: Selective Laser Trabeculoplasty (SLT) and Argon Laser Trabeculoplasty (ALT) are procedures that use a laser to improve the drainage of aqueous humor through the trabecular meshwork. Laser peripheral iridotomy (LPI) is used for angle-closure glaucoma to create a small opening in the iris.
- Surgical Intervention: For individuals who do not respond adequately to medications or laser therapy, or for those with advanced glaucoma, surgery may be recommended. This can include trabeculectomy (creating a new drainage channel) or the implantation of glaucoma drainage devices. Minimally Invasive Glaucoma Surgery (MIGS) represents a newer category of surgical procedures with a favorable safety profile.
The goal of treatment is not necessarily to bring IOP down to a specific “magic number” but to achieve a target IOP that is low enough to prevent further optic nerve damage and preserve vision for the patient’s lifetime. This target IOP is individualized based on the severity of the disease, the rate of progression, and other risk factors.
Conclusion: Proactive Vigilance for Vision Preservation
Determining what constitutes “dangerously high” eye pressure is a multifaceted evaluation that extends beyond a simple numerical threshold. It is a dynamic assessment that considers the individual’s unique ocular anatomy, physiological responses, genetic predispositions, and the presence or absence of optic nerve damage. While an IOP consistently above 21 mmHg is a signal for concern, the true danger lies in the potential for irreversible vision loss through optic nerve damage (glaucoma).
The integration of advanced diagnostic technologies, from precise tonometers to sophisticated OCT imaging, has revolutionized our ability to detect subtle changes and personalize risk assessments. Regular comprehensive eye examinations, especially for individuals with known risk factors, are the cornerstone of early detection and intervention. By understanding the factors that influence IOP and by leveraging the diagnostic and therapeutic tools available, patients and eye care professionals can work collaboratively to safeguard vision and mitigate the risks associated with dangerously high eye pressure. Proactive vigilance remains the most powerful strategy in the fight against vision-threatening eye conditions.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.