Chronic Kidney Disease (CKD) is a progressive condition characterized by a gradual loss of kidney function over time. The kidneys are vital organs, responsible for filtering waste products and excess fluid from the blood, regulating blood pressure, producing red blood cells, and maintaining bone health. When the kidneys are damaged and cannot perform these essential functions adequately, it leads to a buildup of toxins and fluid in the body, causing a range of health problems.
CKD is a silent epidemic, often progressing without noticeable symptoms in its early stages. This makes early detection and management crucial to prevent severe complications and improve patient outcomes. Understanding what CKD is, its causes, symptoms, and available management strategies is paramount for individuals and healthcare providers alike.

Understanding the Mechanics of Kidney Function and Damage
To truly grasp what Chronic Kidney Disease is, it’s essential to first understand how healthy kidneys operate and what constitutes damage. The kidneys are complex filtering units, composed of millions of tiny structures called nephrons. Each nephron contains a glomerulus, a small network of blood vessels, and a tubule, a tiny tube. As blood flows through the glomeruli, waste products, excess salts, and water are filtered out, forming urine. This urine then travels through the tubules, where essential substances like glucose, amino acids, and water are reabsorbed back into the bloodstream. The remaining waste products and excess fluid are expelled from the body as urine.
When CKD develops, these nephrons become damaged. This damage can occur due to a variety of factors, leading to a progressive decline in the kidneys’ ability to filter blood. Initially, the remaining healthy nephrons can compensate for the damaged ones, maintaining near-normal kidney function. However, as more nephrons are destroyed, the burden on the remaining units increases, and eventually, the kidneys can no longer keep up.
The Glomeruli: The Kidney’s Primary Filtration System
The glomeruli are the workhorses of the kidney, responsible for the initial filtering of blood. Imagine them as microscopic sieves. Blood enters the glomerulus under pressure, and water, waste products, and small molecules are forced through the filtration barrier, while larger components like blood cells and proteins remain in the bloodstream. This filtered fluid, now called glomerular filtrate, then enters the renal tubules for further processing.
Damage to the glomeruli, often caused by conditions like high blood pressure or diabetes, impairs their ability to filter effectively. This can lead to:
- Proteinuria (or albuminuria): When the glomeruli are damaged, they can allow proteins, particularly albumin, to leak from the blood into the urine. This is often one of the earliest signs of kidney damage and can be detected through urine tests.
- Reduced Filtration Rate: As more glomeruli are damaged, the overall filtering capacity of the kidneys diminishes. This is measured by the Glomerular Filtration Rate (GFR), a key indicator of kidney function.
The Renal Tubules: Fine-Tuning and Reabsorption
The renal tubules play a crucial role in refining the filtrate produced by the glomeruli. They reabsorb essential substances that the body needs back into the bloodstream, such as glucose, amino acids, electrolytes (like sodium, potassium, and calcium), and a significant portion of the water. Simultaneously, the tubules secrete certain waste products and excess ions into the filtrate, further concentrating the urine.
Damage to the tubules can disrupt this delicate balance, leading to:
- Electrolyte Imbalances: The inability to reabsorb or secrete electrolytes properly can lead to dangerous fluctuations in their levels in the blood, affecting nerve and muscle function, heart rhythm, and fluid balance.
- Acid-Base Imbalances: The kidneys play a vital role in maintaining the body’s acid-base balance. Tubular damage can impair this function, leading to the buildup of acids or bases.
- Impaired Water Reabsorption: This can result in excessive urination and dehydration, or conversely, the inability to excrete excess water, leading to fluid overload.
Causes and Risk Factors: Unpacking the Triggers of CKD
The development of Chronic Kidney Disease is rarely due to a single factor. Instead, it is often the result of underlying medical conditions that progressively damage the kidneys over time. Identifying these causes and understanding the risk factors is essential for prevention and early intervention.
The Leading Culprits: Diabetes and Hypertension
The two most prevalent causes of CKD globally are diabetes and high blood pressure (hypertension). These conditions, if left unmanaged, wreak havoc on the delicate blood vessels within the kidneys, leading to their gradual destruction.
- Diabetes Mellitus: In people with diabetes, high blood sugar levels can damage the small blood vessels in the kidneys over time, including those in the glomeruli. This damage, known as diabetic nephropathy, impairs the kidneys’ ability to filter blood effectively. Uncontrolled diabetes is a leading cause of kidney failure.
- Hypertension (High Blood Pressure): High blood pressure exerts excessive force on the walls of the blood vessels throughout the body, including those in the kidneys. This constant pressure can damage the glomeruli and arteries in the kidneys, reducing blood flow and impairing their function. Hypertension can both cause and be exacerbated by kidney disease, creating a vicious cycle.
Other Significant Contributors to Kidney Damage
While diabetes and hypertension are the primary drivers, several other conditions and factors can also lead to CKD:
- Glomerulonephritis: This is a group of diseases that cause inflammation of the glomeruli. It can be caused by infections, autoimmune diseases (like lupus), or unknown reasons.
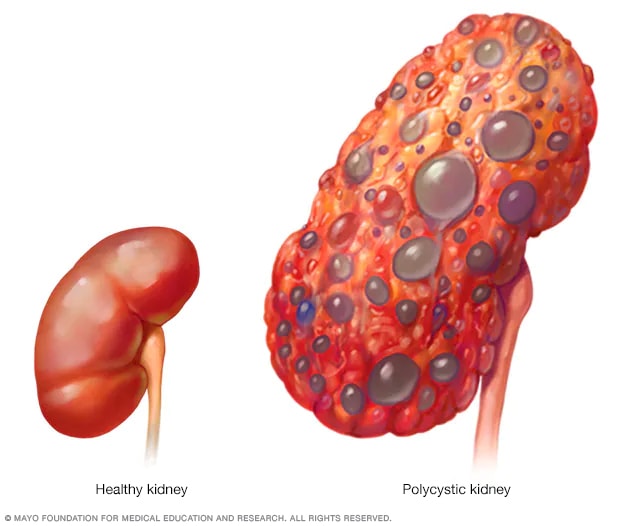
- Polycystic Kidney Disease (PKD): This is a genetic disorder characterized by the growth of numerous cysts in the kidneys, which can enlarge the kidneys and impair their function.
- Interstitial Nephritis: This condition involves inflammation of the tubules and surrounding structures of the kidneys. It is often caused by allergic reactions to certain medications, infections, or autoimmune diseases.
- Obstructive Nephropathy: This occurs when there is a blockage in the urinary tract, preventing urine from draining properly. This blockage can cause urine to back up into the kidneys, leading to damage. Causes include kidney stones, enlarged prostate, or tumors.
- Recurrent Kidney Infections (Pyelonephritis): Frequent and severe kidney infections can lead to scarring and permanent kidney damage.
- Long-term Use of Certain Medications: Some medications, particularly nonsteroidal anti-inflammatory drugs (NSAIDs) taken regularly for long periods, can harm the kidneys.
Recognizing Your Risk: Key Risk Factors

Certain factors increase an individual’s likelihood of developing CKD. Being aware of these can empower proactive health management:
- Family History of Kidney Disease: A genetic predisposition can significantly increase risk.
- Age: The risk of CKD increases with age, as kidney function naturally declines over time.
- Race and Ethnicity: Certain racial and ethnic groups, including African Americans, Hispanics, Native Americans, and Asians, have a higher risk of developing CKD. This can be due to a combination of genetic, social, and environmental factors.
- Obesity: Excess body weight can contribute to diabetes and hypertension, both major risk factors for CKD.
- Cardiovascular Disease: Conditions affecting the heart and blood vessels are closely linked to kidney health.
- Autoimmune Diseases: Conditions like lupus and rheumatoid arthritis can trigger inflammation that affects the kidneys.
Symptoms and Diagnosis: Unmasking the Silent Threat
As mentioned, CKD often progresses silently, especially in its early stages. This is why regular health check-ups and awareness of potential symptoms are crucial. When symptoms do appear, they are often non-specific and can be mistaken for other ailments.
The Subtle Signals: Early and Advanced Symptoms
In the initial stages of CKD, individuals may experience no symptoms at all. As kidney function declines, however, a range of subtle and then more pronounced symptoms can emerge:
- Changes in Urination: This can include increased frequency of urination (especially at night), foamy or bubbly urine (indicating protein), blood in the urine (hematuria), or decreased urine output.
- Swelling (Edema): Fluid retention due to impaired kidney function can cause swelling in the legs, ankles, feet, and face.
- Fatigue and Weakness: The buildup of waste products in the blood can lead to persistent tiredness and a general lack of energy.
- Loss of Appetite and Nausea/Vomiting: Uremia, the buildup of toxins, can affect the digestive system.
- Itchy Skin: Waste products accumulating in the blood can cause persistent itching.
- Muscle Cramps: Electrolyte imbalances can contribute to muscle spasms and cramps.
- Shortness of Breath: Fluid buildup in the lungs can lead to difficulty breathing.
- High Blood Pressure: As mentioned, CKD can cause or worsen hypertension.
- Difficulty Concentrating: Uremia can affect cognitive function.
It is vital to understand that these symptoms are not exclusive to CKD and can be indicative of other health issues. This underscores the importance of professional medical evaluation for accurate diagnosis.
The Diagnostic Toolkit: How CKD is Identified
Diagnosing CKD involves a combination of medical history, physical examination, and laboratory tests. Healthcare providers use these tools to assess kidney function and identify the extent of damage.
- Blood Tests:
- Blood Urea Nitrogen (BUN) and Creatinine: These are waste products filtered by the kidneys. Elevated levels in the blood indicate that the kidneys are not effectively removing them.
- Estimated Glomerular Filtration Rate (eGFR): This is a calculation based on serum creatinine levels, age, sex, and race to estimate how well the kidneys are filtering waste. An eGFR below 60 mL/min/1.73 m² for three months or longer is a key indicator of CKD.
- Electrolytes: Tests for sodium, potassium, chloride, and bicarbonate help assess electrolyte balance.
- Complete Blood Count (CBC): This can reveal anemia, which is common in CKD due to reduced production of erythropoietin.
- Urine Tests:
- Urinalysis: This basic test checks for the presence of protein, blood, white blood cells, and other abnormalities in the urine.
- Urine Albumin-to-Creatinine Ratio (UACR): This test specifically measures the amount of albumin in the urine, a sensitive indicator of early kidney damage.
- Imaging Tests:
- Kidney Ultrasound: This imaging technique uses sound waves to create pictures of the kidneys, allowing doctors to assess their size, shape, and look for any abnormalities like cysts or tumors.
- CT Scan and MRI: These more detailed imaging tests can provide further information about the structure of the kidneys and surrounding organs.
- Kidney Biopsy: In some cases, a small sample of kidney tissue may be taken and examined under a microscope to determine the specific cause and extent of kidney damage. This is usually performed when the cause of CKD is unclear.
By combining these diagnostic tools, healthcare professionals can accurately diagnose CKD, determine its stage, and develop an appropriate management plan.
Managing CKD: Strategies for Slowing Progression and Improving Quality of Life
While Chronic Kidney Disease is often progressive, there are many strategies available to slow its advancement, manage its symptoms, and significantly improve the quality of life for those affected. The focus of management is on addressing the underlying causes, protecting remaining kidney function, and preventing complications.
Lifestyle Modifications: The Foundation of CKD Management
Making significant lifestyle changes is a cornerstone of CKD management. These modifications, when consistently applied, can have a profound impact on kidney health and overall well-being.
- Dietary Adjustments: A kidney-friendly diet is crucial. This often involves:
- Sodium Restriction: Reducing salt intake helps control blood pressure and reduce fluid retention.
- Protein Management: While adequate protein is necessary, excessive intake can burden the kidneys. The specific protein recommendation will vary depending on the stage of CKD and individual needs.
- Potassium and Phosphorus Control: As kidney function declines, the body may struggle to excrete these minerals, leading to dangerous levels. Foods high in potassium (e.g., bananas, potatoes) and phosphorus (e.g., dairy, nuts) may need to be limited.
- Fluid Management: In some stages of CKD, fluid intake may need to be restricted to prevent fluid overload.
- Limiting Processed Foods: Processed foods are often high in sodium, phosphorus, and unhealthy fats.
- Regular Exercise: Moderate physical activity can help manage blood pressure, improve cardiovascular health, and maintain a healthy weight, all of which are beneficial for kidney function.
- Weight Management: Losing excess weight can significantly reduce the strain on the kidneys, especially for individuals with obesity-related conditions like diabetes and hypertension.
- Smoking Cessation: Smoking damages blood vessels and can worsen kidney disease. Quitting smoking is one of the most impactful steps an individual can take.
- Limiting Alcohol Intake: Excessive alcohol consumption can negatively affect blood pressure and kidney function.
Medical Interventions: Targeting Underlying Causes and Complications
Beyond lifestyle changes, various medical treatments are employed to manage CKD:
- Blood Pressure Control: Medications such as ACE inhibitors and ARBs are often prescribed to lower blood pressure and protect the kidneys from further damage.
- Diabetes Management: Strict control of blood glucose levels through diet, exercise, and medication is essential for individuals with diabetic kidney disease.
- Medication Review: Doctors will carefully review all medications, including over-the-counter drugs and supplements, to ensure they are not harming the kidneys.
- Treatment of Underlying Causes: If CKD is caused by conditions like glomerulonephritis or urinary tract obstructions, specific treatments will be implemented to address those issues.
- Medications for Complications: As CKD progresses, patients may develop anemia, bone disease, or electrolyte imbalances, requiring specific medications to manage these complications.
Renal Replacement Therapy: When Kidneys Fail
For individuals with end-stage renal disease (ESRD), where kidney function has severely declined, renal replacement therapy becomes necessary to sustain life. The two primary options are:
- Dialysis: This process artificially filters waste products and excess fluid from the blood. There are two main types:
- Hemodialysis: Blood is pumped from the body through an artificial kidney (dialyzer) and then returned to the body.
- Peritoneal Dialysis: A special fluid is introduced into the abdominal cavity, and waste products and excess fluid are filtered from the blood into this fluid, which is then drained from the body.
- Kidney Transplantation: This surgical procedure involves replacing a diseased kidney with a healthy kidney from a donor. It is often considered the preferred treatment option for eligible patients, offering a better quality of life and longer survival rates.
By embracing a proactive approach to their health, individuals with or at risk of CKD can significantly impact their disease trajectory and live healthier, more fulfilling lives. Understanding “what is chronic kidney disease” is the first, crucial step in this journey.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.