While not directly aligned with the core technological, branding, or financial themes of this website, understanding basal cell carcinoma (BCC) of the skin touches upon a crucial aspect of personal well-being and proactive health management, areas that are undeniably intertwined with an individual’s ability to thrive in any of these domains. A healthy body and mind are fundamental to sustained productivity, effective branding, and sound financial decision-making. Therefore, dedicating some attention to this common form of skin cancer serves as a vital reminder for our audience to prioritize their health.
Basal cell carcinoma (BCC) is the most prevalent type of skin cancer globally, arising from the basal cells, which are found in the lower part of the epidermis, the outermost layer of our skin. These cells are responsible for producing new skin cells as old ones die off. While BCCs are generally slow-growing and rarely spread to other parts of the body (metastasize), early detection and treatment are crucial to prevent them from becoming locally invasive, potentially causing significant damage to surrounding tissues, including nerves, blood vessels, and bone.
Understanding BCC involves delving into its origins, how it manifests, the factors that increase risk, and, most importantly, how it can be effectively managed and prevented. This knowledge empowers individuals to take proactive steps in protecting their skin and recognizing potential warning signs.
Understanding the Genesis and Appearance of Basal Cell Carcinoma
The development of basal cell carcinoma is primarily linked to prolonged and cumulative exposure to ultraviolet (UV) radiation, most commonly from sunlight. The DNA within basal cells can be damaged by UV rays, leading to uncontrolled growth and the formation of a cancerous tumor. This is why individuals with a history of significant sun exposure, particularly those who have experienced blistering sunburns, are at higher risk. Other contributing factors can include genetic predisposition, fair skin, a weakened immune system, and exposure to certain environmental toxins or radiation therapy.
The visual presentation of BCCs can vary significantly, making them sometimes difficult to recognize without a trained eye. However, several common characteristics can serve as red flags. These often appear on sun-exposed areas of the body, such as the face, ears, neck, and hands, but can occur anywhere on the skin.
Common Presentations of Basal Cell Carcinoma
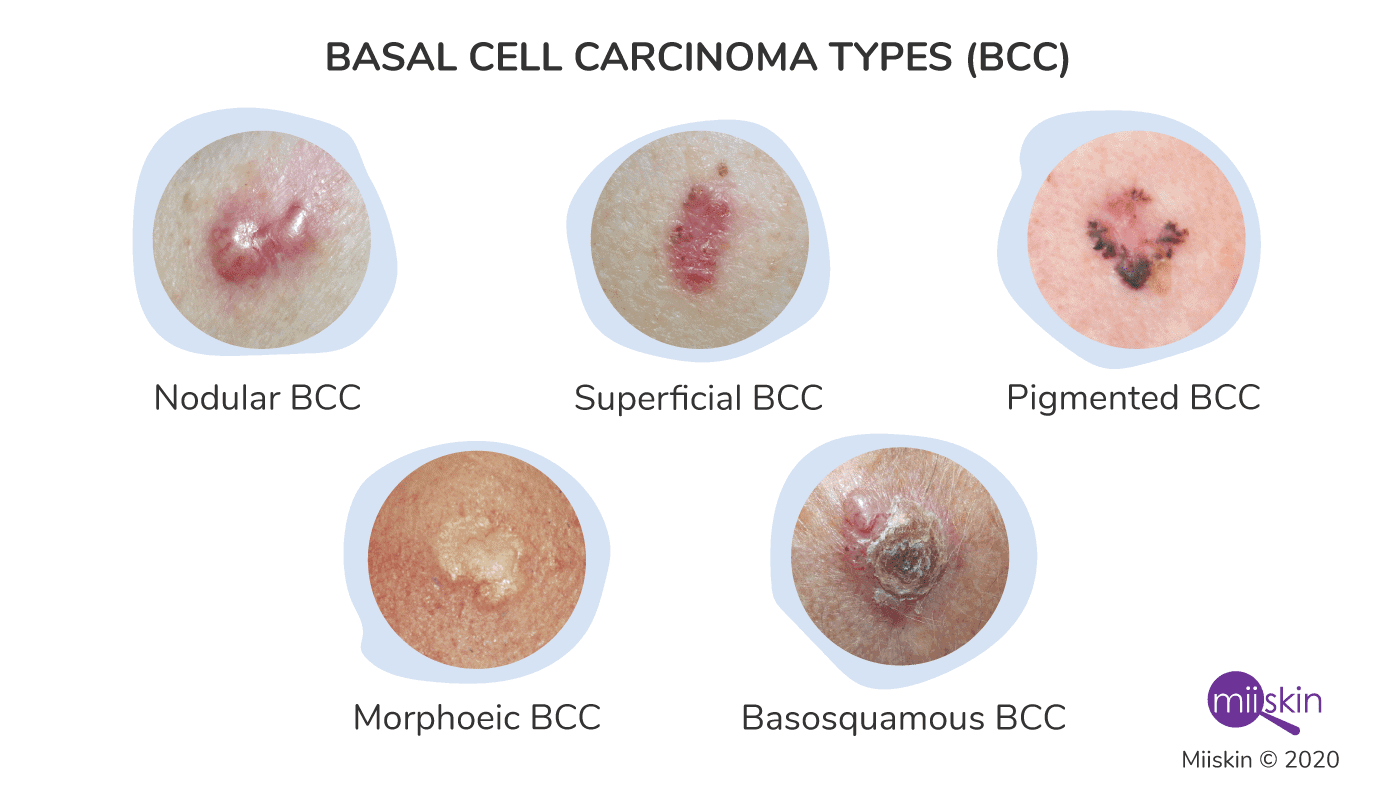
Recognizing the diverse appearances of BCC is a key step in early detection. While professional diagnosis is always necessary, being aware of these common forms can prompt individuals to seek medical attention sooner.
Pearly or Waxy Bumps
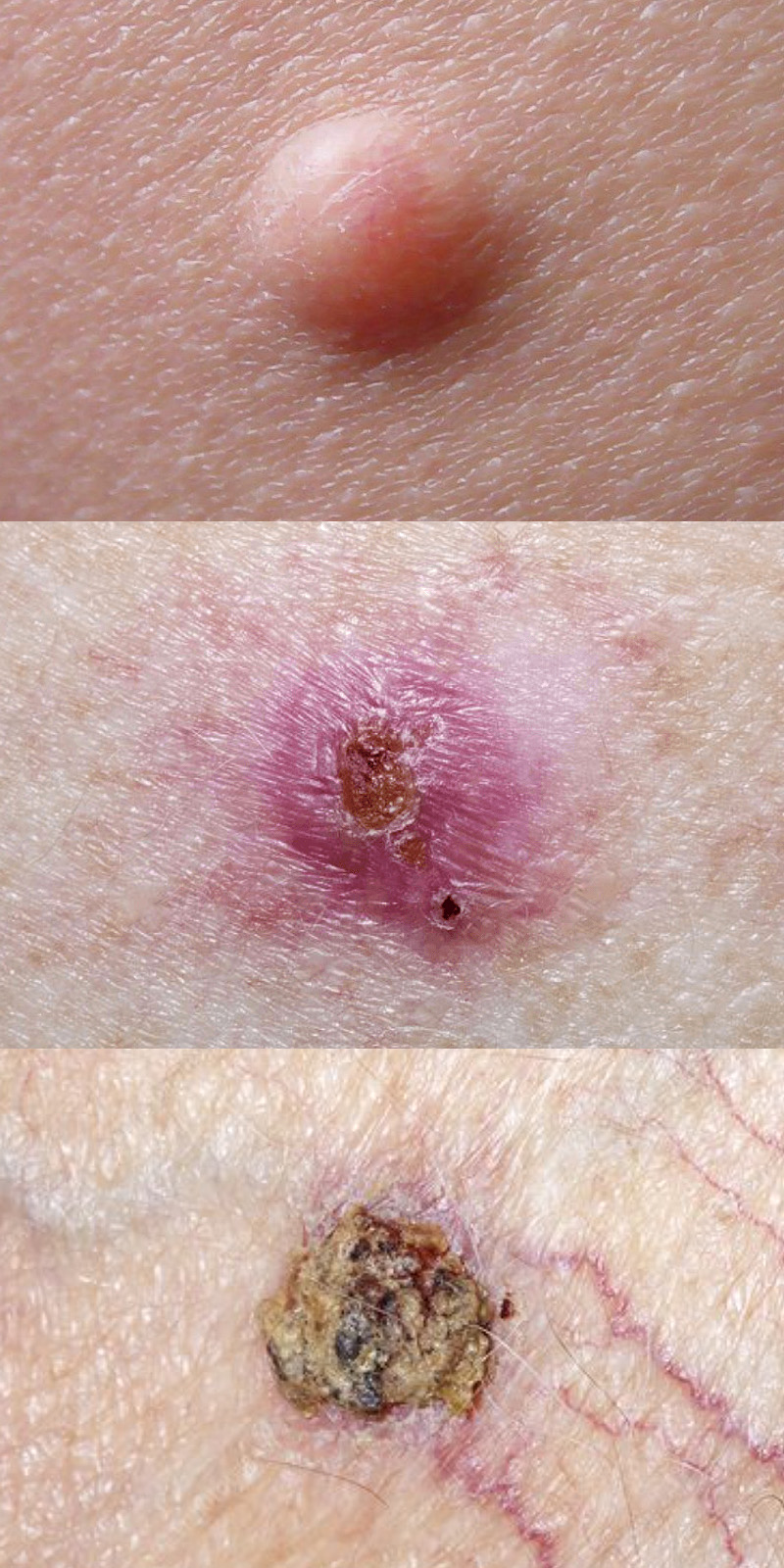
One of the most characteristic appearances of BCC is a pearly or waxy-looking bump. These lesions may have a translucent quality, and upon closer inspection, small blood vessels (telangiectasias) might be visible on the surface. They can vary in size and may be flesh-colored, pink, or even slightly brown or black, especially in individuals with darker skin tones. These bumps can sometimes be mistaken for benign skin growths like moles or skin tags, highlighting the importance of a medical evaluation.
A Flat, Flesh-Colored or Brown Scar-Like Lesion
Another common presentation is a flat, firm, and slightly raised lesion that can resemble a scar. These can be skin-colored, flesh-colored, or have a brownish hue. They might grow slowly and often have indistinct borders, making them easy to overlook. This type of BCC can be particularly insidious as it may not cause pain or itching, leading individuals to delay seeking medical advice.
A Sore That Bleeds and Scabs Over
A BCC can also manifest as a sore that repeatedly bleeds, heals partially, and then reopens. This non-healing ulcer is a significant warning sign. The edges of such a sore may be raised or rolled. It’s crucial to remember that any persistent, non-healing sore on the skin should be evaluated by a dermatologist.
A Reddish or Pinkish Patch
Sometimes, BCCs can present as a reddish or pinkish patch of skin that may be slightly scaly or itchy. These patches can be mistaken for eczema or other inflammatory skin conditions, but their persistence and potential for slow growth warrant closer examination.
Risk Factors and Prevention Strategies for Basal Cell Carcinoma
While BCC is common, several factors increase an individual’s susceptibility to developing it. Understanding these risk factors allows for targeted prevention strategies, minimizing the chances of developing this skin cancer.
Key Risk Factors for BCC Development
The primary culprit behind BCC is UV radiation. However, a combination of intrinsic and extrinsic factors can significantly elevate an individual’s risk profile.
- Sun Exposure History: This is the most significant risk factor. Cumulative UV exposure over a lifetime, especially from recreational sunbathing, tanning beds, and occupational exposure to the sun, dramatically increases the risk. Experiencing blistering sunburns during childhood or adolescence is particularly detrimental.
- Skin Type and Tone: Individuals with fair skin that burns easily, freckles, light-colored hair (blond or red), and blue or green eyes are at a higher risk. This is because they have less melanin, the pigment that provides natural protection against UV radiation.
- Age: The risk of BCC generally increases with age, as cumulative sun damage builds up over time. However, BCC can occur in younger individuals, especially those with intense sun exposure histories.
- Genetics and Family History: A personal or family history of skin cancer, including BCC, melanoma, or squamous cell carcinoma, can increase an individual’s risk. Certain genetic syndromes, such as basal cell nevus syndrome (Gorlin syndrome), are associated with a very high incidence of BCC.
- Weakened Immune System: Individuals with compromised immune systems, due to conditions like HIV/AIDS, organ transplantation, or certain medications (immunosuppressants), are more susceptible to developing skin cancers, including BCC.
- Exposure to Ionizing Radiation: Prior exposure to radiation therapy for medical treatments can also increase the risk of BCC in the treated areas.
- Exposure to Certain Chemicals: While less common, exposure to certain chemicals like arsenic has been linked to an increased risk of BCC.
Proactive Measures for BCC Prevention
Given the significant role of UV radiation, prevention largely revolves around protecting the skin from excessive sun exposure. These strategies are vital for everyone, regardless of their risk factors.
- Sun Protection: The cornerstone of BCC prevention is consistent and diligent sun protection. This includes:
- Seeking Shade: Limiting direct sun exposure, especially during peak hours (typically 10 a.m. to 4 p.m.), is crucial.
- Wearing Protective Clothing: Long-sleeved shirts, long pants, wide-brimmed hats, and UV-blocking sunglasses offer excellent physical barriers against UV rays.
- Using Sunscreen: Applying a broad-spectrum sunscreen with an SPF of 30 or higher daily, and reapplying every two hours (or more frequently if swimming or sweating), is essential. Sunscreen should be used even on cloudy days, as UV rays can penetrate cloud cover.
- Avoiding Tanning Beds: Tanning beds emit harmful UV radiation and significantly increase the risk of all types of skin cancer, including BCC. It is strongly advised to avoid their use entirely.
- Regular Skin Self-Examinations: Becoming familiar with your skin and performing regular self-examinations can help you identify any new or changing moles or lesions. The “ABCDE” rule, commonly used for melanoma detection, can also be helpful for identifying suspicious skin changes. Look for asymmetry, irregular borders, color variations, a diameter larger than 6mm, and any evolving changes.
- Professional Skin Checks: In addition to self-examinations, regular professional skin checks by a dermatologist are highly recommended, especially for individuals with a higher risk profile. Dermatologists can identify suspicious lesions that may be missed during self-examination.
- Awareness of Medications and Treatments: If undergoing treatments involving radiation or immunosuppressants, discuss skin cancer risks and preventive measures with your healthcare provider.
Diagnosis and Treatment Options for Basal Cell Carcinoma
The diagnosis of basal cell carcinoma is typically straightforward for a dermatologist. Once a suspicious lesion is identified, a biopsy is usually performed. This involves removing a small sample of the lesion, which is then examined under a microscope by a pathologist to confirm the diagnosis and determine the type of skin cancer.
The treatment approach for BCC depends on several factors, including the size, location, and depth of the tumor, as well as the patient’s overall health. The good news is that BCCs are highly treatable, with a very high cure rate when addressed promptly.
Diagnostic Procedures
- Visual Examination: A dermatologist will carefully examine the skin, looking for suspicious moles or lesions.
- Dermoscopy: This non-invasive technique uses a specialized magnifying instrument to examine the skin lesion in greater detail.
- Biopsy: This is the definitive diagnostic step. A small piece of the suspicious lesion is removed and sent to a laboratory for microscopic examination. Common biopsy methods include shave biopsy, punch biopsy, and excisional biopsy.
Treatment Modalities for BCC
Once diagnosed, several treatment options are available:
- Surgical Excision: This is a common and highly effective treatment. The cancerous lesion is surgically removed, along with a small margin of healthy surrounding tissue. The removed tissue is sent to a lab to ensure all cancer cells have been cleared.
- Mohs Surgery: This specialized surgical technique is particularly useful for BCCs that are located in cosmetically sensitive areas (like the face), are large, recurrent, or have indistinct borders. During Mohs surgery, the tumor is removed layer by layer, and each layer is examined under a microscope immediately. This process continues until no cancer cells remain, maximizing the preservation of healthy tissue.
- Curettage and Electrodesiccation: This method involves scraping away the cancerous cells with a curette (a sharp, spoon-shaped instrument) and then using an electric needle to cauterize (burn) the base of the wound to stop bleeding and destroy any remaining cancer cells. This is often used for smaller, superficial BCCs.
- Radiation Therapy: For some BCCs, especially those that are difficult to treat surgically or in patients who are not good surgical candidates, radiation therapy may be an option. High-energy rays are used to destroy cancer cells.
- Topical Treatments: For very superficial BCCs, topical creams like imiquimod or 5-fluorouracil may be prescribed. These medications stimulate the immune system to fight the cancer cells or directly kill them.
- Photodynamic Therapy (PDT): This treatment involves applying a light-sensitizing agent to the skin, which is then activated by a specific wavelength of light, destroying the cancer cells. PDT is typically used for superficial BCCs.
- Oral Medications: In rare cases where BCC has spread or is advanced and cannot be treated with surgery or radiation, oral medications like vismodegib or sonidegib may be used. These drugs target specific pathways involved in BCC growth.
Long-Term Outlook and the Importance of Continued Vigilance
The prognosis for basal cell carcinoma is generally excellent, especially with early detection and appropriate treatment. The vast majority of BCCs are cured with minimal to no long-term consequences. However, it is crucial to understand that developing one BCC increases the likelihood of developing others in the future, as the underlying risk factors, particularly cumulative sun damage, remain.
Therefore, continued vigilance and proactive skin care are paramount even after successful treatment. This includes adhering to the prevention strategies outlined earlier, performing regular self-examinations, and attending scheduled follow-up appointments with your dermatologist.

Post-Treatment Care and Follow-Up
- Regular Dermatologist Visits: Following treatment, your dermatologist will likely recommend regular skin checks to monitor for any new suspicious lesions. The frequency of these visits will depend on your individual risk factors and the type of BCC you had.
- Continued Sun Protection: Reinforcing the habit of rigorous sun protection is non-negotiable. This includes daily sunscreen application, protective clothing, and seeking shade.
- Prompt Evaluation of Any Changes: Any new or changing skin lesions, persistent sores, or unusual moles should be promptly evaluated by a dermatologist. Early detection remains the most effective strategy for managing any recurrence or new skin cancers.
By understanding what basal cell carcinoma is, recognizing its signs, taking proactive steps to prevent it, and remaining vigilant after treatment, individuals can significantly reduce their risk and ensure their long-term skin health. This proactive approach to personal well-being is a foundational element for sustained success and fulfillment in all aspects of life.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.