For decades, the cervical screening process, commonly known as the Pap smear, remained largely unchanged in its fundamental methodology. However, the intersection of healthcare and technology—often referred to as MedTech or FemTech—has revolutionized what happens from the moment a patient enters the examination room to the millisecond a diagnostic result is generated. Today, a Pap smear is no longer just a manual clinical procedure; it is a complex data-gathering mission supported by advanced hardware, cloud-based laboratory information systems, and artificial intelligence (AI).
Understanding the technology behind modern cervical screening reveals a sophisticated ecosystem designed to maximize accuracy, streamline patient data, and ensure early intervention through high-tech diagnostics.
The Hardware Evolution: From Manual Sampling to Precision Engineering
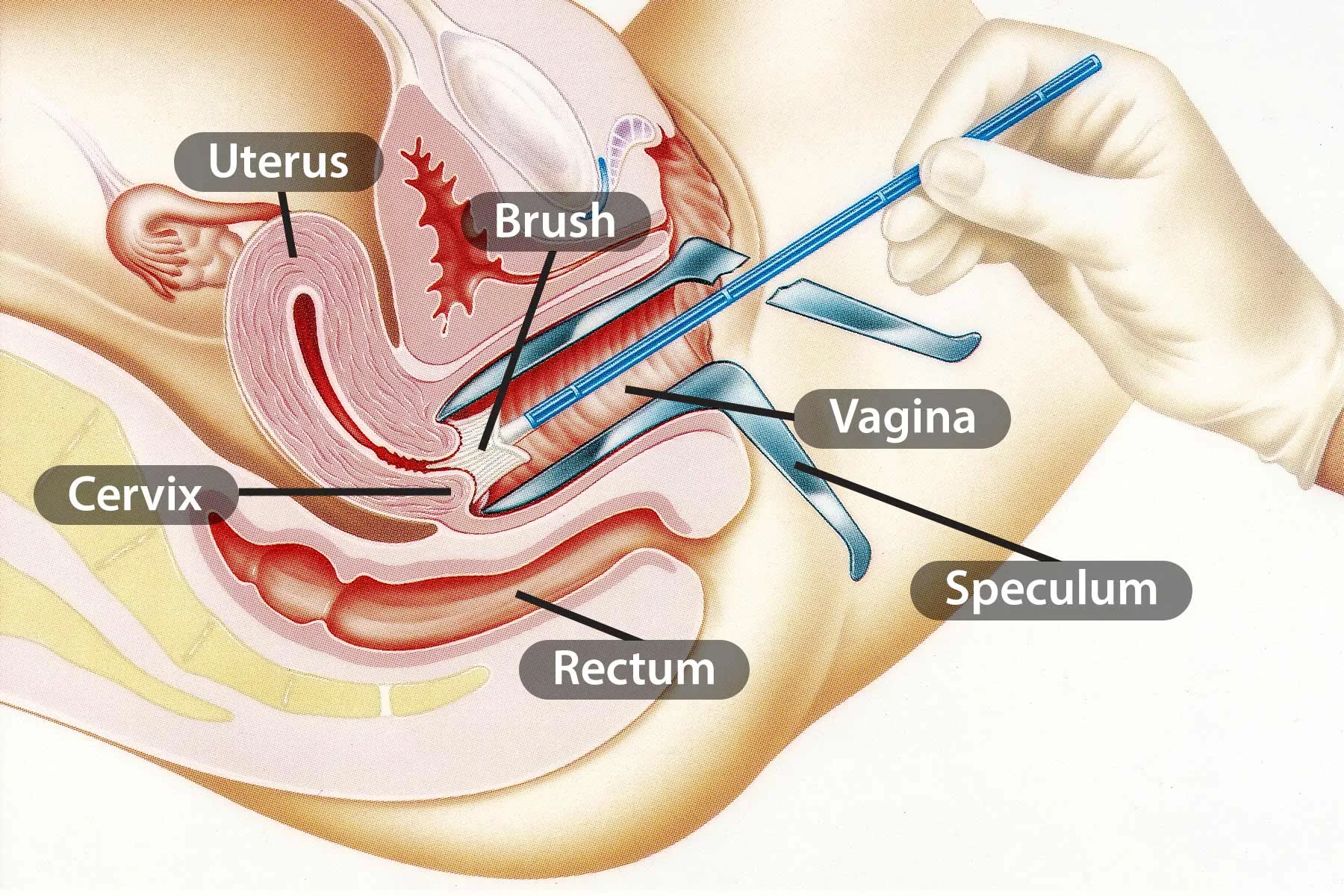
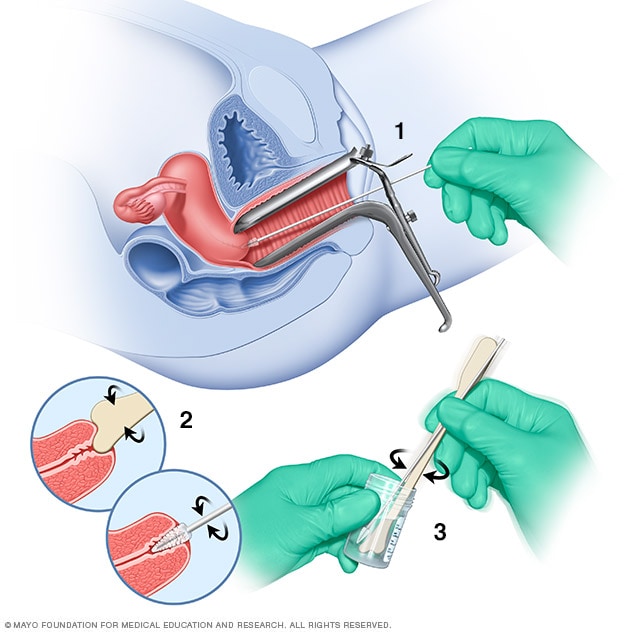
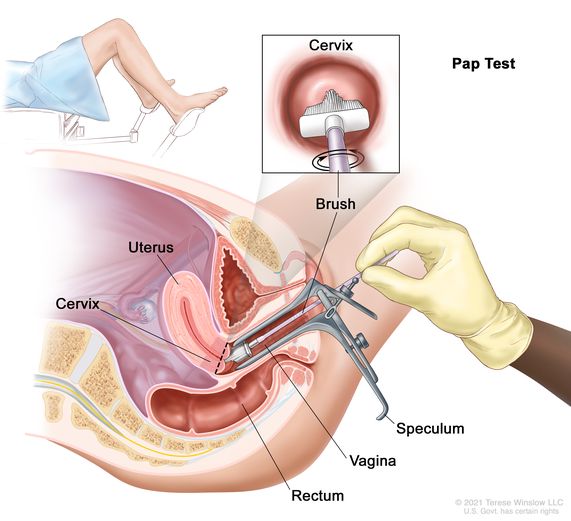
The physical procedure of a Pap smear involves collecting a sample of cells from the cervix. While the basic mechanics remain familiar, the tools used to facilitate this process have undergone a significant technological overhaul to improve sample viability and diagnostic yield.
Smart Speculums and High-Resolution Imaging
Traditional stainless steel instruments are being replaced or augmented by ergonomically engineered, single-use high-tech alternatives. Some modern clinical settings now utilize “smart speculums” equipped with integrated LED lighting and high-definition cameras. These devices allow for digital colposcopy—a process where the clinician can capture high-resolution images of the cervix in real-time. These images are not just for immediate viewing; they are uploaded to a patient’s electronic health record (EHR), allowing for longitudinal tracking of tissue changes over years with pixel-perfect precision.
Liquid-Based Cytology (LBC) and Automated Processing
The most significant tech shift in the collection phase is the transition from the “conventional smear” to Liquid-Based Cytology (LBC). In the past, cells were smeared directly onto a glass slide, often resulting in “clumping” or obscured views due to blood or mucus.
Current technology utilizes a specialized preservative fluid. Once the sample is collected, the brush head is detached into a vial of liquid. This vial is then processed by an automated system in the lab, such as the ThinPrep or SurePath systems. These machines use sophisticated filtration and sedimentation technology to separate debris from diagnostic cells, creating a thin, uniform layer of cells on a slide. This technological intervention ensures that the “data” (the cells) is presented in the cleanest possible format for analysis.
The Role of Artificial Intelligence in Cytopathology
Once the sample reaches the laboratory, the most impressive technological phase begins. The analysis of cervical cells is a high-stakes task that requires detecting microscopic abnormalities among hundreds of thousands of healthy cells. This is where Artificial Intelligence and Machine Learning (ML) have become indispensable.
AI-Driven Slide Analysis and Pattern Recognition
Modern labs utilize automated screening devices powered by AI. These systems scan every slide and identify the most “suspicious” cells based on vast databases of known morphological patterns. For instance, the AI evaluates the nuclear-to-cytoplasmic ratio, the texture of the chromatin, and the shape of the cell wall.
Instead of a cytotechnologist spending hours looking at every single slide, the AI acts as a first-tier filter. It highlights specific “fields of interest” for the human professional to review. This synergy between human expertise and algorithmic speed significantly reduces “false negatives”—cases where abnormal cells might have been overlooked due to human fatigue or oversight.
Deep Learning and Predictive Diagnostics
Beyond simple pattern recognition, the next generation of cervical tech involves deep learning models trained on millions of historical screening images. These models can sometimes detect subtle “pre-cytological” changes—morphological shifts that are invisible to the human eye but indicate a high statistical probability of future cellular transformation. By integrating these predictive analytics, the “results” of a Pap smear are evolving from a simple “normal/abnormal” binary into a comprehensive risk profile.
Data Security and Patient Privacy in Diagnostic Tech
As the Pap smear process becomes increasingly digitized, the management of the resulting data has become a critical pillar of the technology. The journey from a physical cell to a digital result involves multiple touchpoints where data integrity and security are paramount.
Laboratory Information Management Systems (LIMS)
Every vial in a modern screening program is barcoded and tracked through a Laboratory Information Management System (LIMS). This software ensures a digital chain of custody, preventing sample mix-ups and ensuring that the right data is attached to the right patient profile. A LIMS integrates seamlessly with the clinic’s software, allowing for the automated delivery of results.
The Intersection of HIPAA and Cloud Computing
Storing high-resolution diagnostic images and genetic data (if HPV DNA testing is performed alongside the Pap) requires robust cloud infrastructure. Tech providers in this space must comply with strict regulations like HIPAA in the United States or GDPR in Europe.
End-to-end encryption is used when transmitting results from the lab to the provider’s portal. Furthermore, many tech platforms now offer patient-facing apps where individuals can securely access their results, receive automated reminders for their next screening based on algorithmic risk-assessment, and communicate with providers through encrypted channels.
FemTech and the Disruption of the Clinic Visit
The most recent technological frontier in cervical health is the move toward decentralization. Technology is now enabling “what happens during a Pap smear” to occur outside the traditional four walls of a doctor’s office.
HPV Self-Sampling Kits and App Integration
While a traditional Pap smear focuses on cytology (looking at cells), many screening programs are shifting toward HPV DNA testing as a primary screen. This has paved the way for “at-home” tech kits. These kits include high-tech brushes and stabilized transport media that allow a user to collect their own sample.
The tech component here is the integration with mobile platforms. Users scan their kit via an app, which tracks the sample to the lab and provides a digital interface for result interpretation. This removes the “white coat” barrier and utilizes logistics technology to increase screening rates in underserved populations.
Telehealth and Virtual Consultations
If the diagnostic hardware identifies an abnormality, the subsequent step—the consultation—is also being transformed by tech. Telehealth platforms allow specialists to review the digital images captured during the initial procedure with the patient via screen-sharing. This allows for a more visual and educational patient experience, as the individual can see exactly what the AI and the clinician are seeing, fostering a deeper understanding of their own health data.
The Future of Screening: Multi-Omics and Beyond
As we look toward the future, the technology involved in a Pap smear is likely to merge with other “omic” technologies. We are moving toward a “multi-omic” approach where a single cervical sample can provide a wealth of digital information.
Proteomics and Molecular Diagnostics
Future iterations of screening hardware will likely include sensors capable of immediate molecular analysis at the point of care. Imagine a speculum that doesn’t just see, but “smells” or chemically analyzes the environment for biomarkers of malignancy. This would turn a weeks-long lab process into a real-time data readout.
Global Health Tech and AI Portability
One of the most exciting aspects of this technological evolution is portability. High-tech screening used to require a multi-million dollar lab. Now, researchers are developing smartphone-based colposcopy tools and AI algorithms that can run on basic mobile hardware. This means that the high-standard of care provided by a modern Pap smear can be “exported” to remote regions of the world, where a mobile phone and a simple attachment can perform the work of a sophisticated diagnostic suite.
Conclusion
The question of “what happens during a Pap smear” is no longer answered by a simple clinical description of a physical exam. It is a story of a sample’s journey through a high-tech pipeline of automated processing, AI-driven analysis, and secure data management.
By leveraging the power of modern software and hardware, the medical community has turned a routine check-up into a powerful engine of preventative data science. As AI continues to refine its predictive capabilities and hardware becomes even more non-invasive and precise, the “tech” of the Pap smear will continue to be our most effective weapon in the early detection and eventual eradication of cervical cancer. The fusion of healthcare and technology ensures that every cell collected is a data point contributing to a healthier, more informed future.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.