Breast cancer remains a formidable global health challenge, making early and accurate diagnosis paramount for effective treatment and improved patient outcomes. Among the array of diagnostic tools available, ultrasound plays a crucial, often complementary, role to mammography, especially for younger women, those with dense breast tissue, or as a follow-up to suspicious mammogram findings. However, understanding “what breast cancer looks like on an ultrasound” is not just a medical question; it’s an inquiry deeply intertwined with the advancements in technology, the strategic branding of healthcare providers and equipment manufacturers, and the complex financial dynamics that govern access and innovation in medicine. This article delves into the visual characteristics of breast cancer on an ultrasound, not as a purely clinical guide, but through the lenses of Technology, Brand, and Money, demonstrating how these seemingly disparate fields converge to shape the landscape of modern diagnostics.
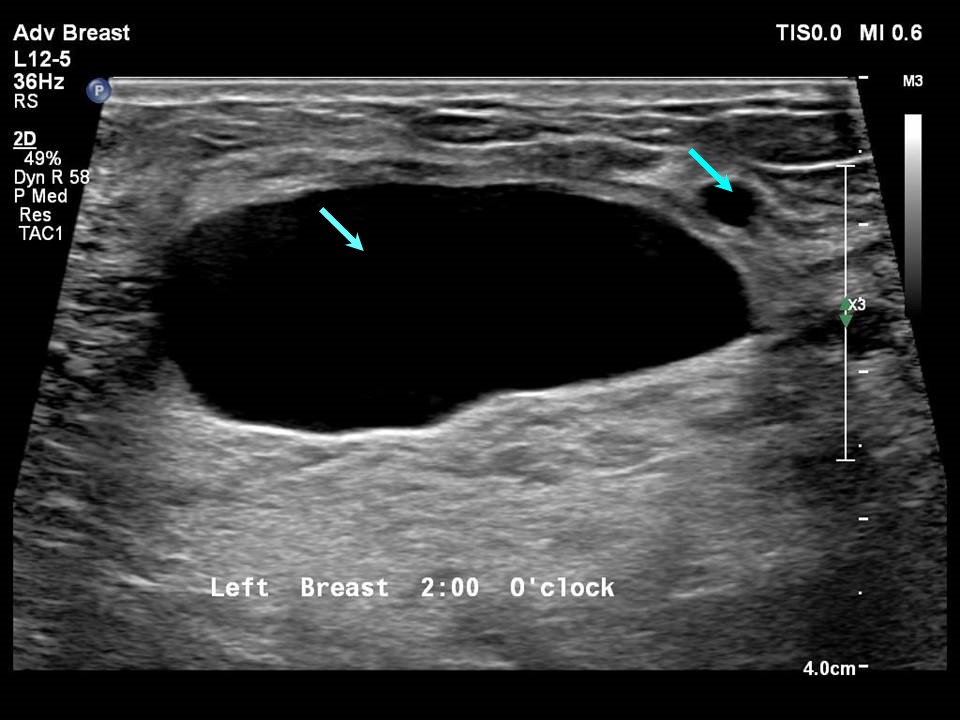
In essence, an ultrasound machine uses high-frequency sound waves to create real-time images of internal body structures. For breast imaging, these sound waves bounce off tissues and return to the transducer, which then converts them into electrical signals displayed as images on a screen. Cancerous lesions often present distinct characteristics compared to benign ones or normal breast tissue. Typically, a malignant mass might appear as a hypoechoic (darker than surrounding tissue) lesion with an irregular shape, spiculated margins (jagged edges radiating outwards), taller-than-wide orientation, posterior shadowing (reduced sound transmission behind the lesion), and increased vascularity (more blood flow) as detected by Doppler ultrasound. Microcalcifications, though often seen on mammograms, can sometimes be indirectly inferred or correlated with suspicious areas on ultrasound. The radiologist’s expertise in interpreting these visual cues is critical, yet it’s increasingly augmented by sophisticated technological tools that enhance visualization, aid analysis, and integrate seamlessly into broader healthcare ecosystems—systems themselves shaped by brand perceptions and financial realities.
The Technological Edge: How Advanced Imaging Transforms Diagnostics
The journey from a basic black-and-white ultrasound image to the high-resolution, AI-assisted diagnostics of today is a testament to relentless technological innovation. Understanding what breast cancer looks like on an ultrasound is fundamentally an exercise in interpreting visual data, and the precision of this interpretation is directly proportional to the sophistication of the technology employed.
Evolution of Ultrasound Technology: From Basic Scans to AI-Powered Insights
The core of breast ultrasound diagnostics lies in the imaging equipment itself. Modern ultrasound machines are far cry from their predecessors. Today’s “gadgets” feature high-frequency transducers capable of producing incredibly detailed images, revealing subtle tissue differences that were previously indistinguishable. Advances like 3D and 4D ultrasound imaging provide volumetric data, allowing radiologists to examine a lesion from multiple planes and gain a more comprehensive understanding of its architecture. This improved resolution and multi-dimensional viewing capabilities are crucial for identifying the tell-tale signs of malignancy, such as irregular shapes, angulated margins, and microlobulations, with greater clarity.
Beyond hardware, the “software” aspect has revolutionized how these images are processed and analyzed. Advanced image processing algorithms can reduce noise, enhance contrast, and automatically highlight areas of interest. This brings us to the exciting frontier of AI tools in medical imaging. Artificial intelligence, particularly machine learning and deep learning, is increasingly being integrated into ultrasound platforms. AI algorithms are trained on vast datasets of ultrasound images, learning to recognize patterns associated with malignant tumors. They can assist radiologists by:
- Pattern Recognition: Automatically identifying suspicious features like spiculated margins, irregular shapes, and posterior shadowing.
- Lesion Classification: Providing a probability score for malignancy, helping distinguish between benign and malignant lesions, which can reduce the need for unnecessary biopsies.
- Workflow Optimization: Flagging areas that warrant closer scrutiny, improving diagnostic speed and reducing radiologist fatigue.
- Reducing Variability: Standardizing interpretation across different radiologists, leading to more consistent diagnoses.
These AI tools don’t replace human expertise but rather augment it, acting as an intelligent second pair of eyes. They represent a significant leap in productivity and accuracy within the diagnostic process, directly addressing some of the challenges in identifying elusive characteristics of early-stage breast cancer on an ultrasound. As AI continues to evolve, its capacity to interpret complex visual data and provide actionable insights will only grow, fundamentally changing how breast cancer looks to the diagnostic eye—and how accurately we can identify it.
Digitalization and Data: Securing and Sharing Critical Health Information
The shift towards digital imaging has profound implications for how breast cancer ultrasound images are managed, stored, and accessed. Picture Archiving and Communication Systems (PACS) are now standard in most healthcare facilities, allowing for the digital storage and retrieval of ultrasound images. This digitalization offers numerous benefits: instant access to patient histories, the ability to compare current scans with previous ones side-by-side, and simplified sharing of images between specialists for multidisciplinary consultations. This streamlined workflow dramatically enhances productivity and collaboration among healthcare professionals.
However, the proliferation of digital health data also introduces significant challenges, particularly concerning digital security. Medical images, like all patient health information, are highly sensitive. Protecting these images from cyber threats—unauthorized access, data breaches, or ransomware attacks—is paramount. Robust encryption protocols, secure network infrastructures, and strict access controls are essential for maintaining patient privacy and compliance with regulations like HIPAA. Data governance policies must ensure that while images can be easily shared for diagnostic purposes, they are equally well-protected from misuse.
Furthermore, the concept of remote diagnostics and telemedicine benefits significantly from digital imaging. Specialists can review ultrasound images and reports from different locations, facilitating expert opinions in underserved areas or during emergencies. This capability is not just about convenience; it’s about extending the reach of high-quality diagnostic expertise, democratizing access to specialized medical opinions, and ensuring that geographical barriers do not impede timely diagnosis and treatment planning for breast cancer patients. The seamless and secure flow of this critical data is as vital as the imaging technology itself in the modern healthcare ecosystem.
Building Trust and Awareness: The Branding of Early Detection
In the competitive landscape of modern healthcare, the visual interpretation of breast cancer on an ultrasound is not merely a scientific exercise but is also deeply influenced by the ‘Brand’ dimension. This involves how healthcare providers position themselves, how medical technology companies market their innovations, and how public awareness campaigns shape perceptions around early detection.
Healthcare Providers as Brands: Reputation, Patient Experience, and Trust
Hospitals, clinics, and diagnostic centers operate as distinct brands within the healthcare industry. For a patient facing a potential breast cancer diagnosis, the choice of where to go for an ultrasound is often influenced by the institution’s reputation. A strong brand in this context is built on several pillars: the perceived expertise of their radiologists and sonographers, the modernity of their equipment, the efficiency of their services, and crucially, the patient experience.
Healthcare providers brand themselves around their commitment to cutting-edge technology, often highlighting the latest ultrasound machines with AI integration as a differentiator. They also emphasize their team of expert radiologists, touting their specialized training and experience in breast imaging. This “corporate identity” is not just about logos and marketing; it’s about delivering consistent, high-quality care that fosters trust. A positive patient experience—from the ease of scheduling an appointment, to the comfort during the scan, to the clarity with which results are communicated—is paramount. A brand that is perceived as compassionate, transparent, and highly competent will attract more patients and build stronger community ties.
In the context of breast cancer diagnosis, where anxiety levels are naturally high, the brand’s promise of accuracy, speed, and empathetic care can significantly reduce patient stress. For instance, a facility that offers rapid result turnaround times or provides clear, easy-to-understand explanations of what breast cancer might look like on an ultrasound (and what their specific findings mean) builds invaluable trust. This focus on patient-centric care and transparent communication forms the bedrock of a robust healthcare brand, influencing patient choices and, ultimately, impacting early detection rates.
The Branding of Medical Technology: Innovators and Market Leaders
Behind every advanced ultrasound machine, there are powerful medical technology companies vying for market leadership. Companies like GE Healthcare, Siemens Healthineers, Philips, and Canon Medical Systems invest heavily in research and development to produce the next generation of imaging devices. Their “brand strategy” revolves around innovation, reliability, and diagnostic superiority.
These companies strategically market their ultrasound systems, highlighting features that directly impact how effectively clinicians can identify breast cancer characteristics. They showcase the high-resolution transducers, the sophisticated image processing software, and increasingly, the integrated AI tools designed to enhance diagnostic accuracy and workflow. For example, a company might brand a new AI feature as “ClarityAssist” or “OncoDetect,” signaling its specific benefit in cancer detection. The “design” of these machines also plays a role, with user-friendly interfaces and ergonomic considerations for sonographers being key selling points.
Through strategic marketing and case studies demonstrating improved diagnostic outcomes, these tech giants aim to establish their products as indispensable tools for breast cancer screening and diagnosis. Their branding efforts target not only hospital procurement departments but also radiologists and sonographers who influence purchasing decisions. By positioning their technology as essential for precision diagnostics, these companies indirectly contribute to the overall understanding and identification of what breast cancer looks like on an ultrasound, by making the subtle visual cues more apparent and interpretable. Ultimately, the perceived quality and reliability of these medical “gadgets” directly contribute to a healthcare provider’s ability to deliver accurate diagnoses, thus forming a crucial link in the chain of trust and patient care.
The Financial Footprint: Investing in Early Detection and Future Health
The ability to accurately determine what breast cancer looks like on an ultrasound, and to access the technology that enables such identification, is profoundly shaped by financial considerations. From the costs of the diagnostic tools themselves to the economic benefits of early intervention, money plays a pivotal role in the entire ecosystem of breast cancer care.
The Economics of Early Diagnosis: Long-Term Savings vs. Upfront Costs
The investment in breast cancer ultrasound equipment, training, and staffing represents significant upfront costs for healthcare facilities. A high-end ultrasound system with advanced features and AI integration can cost hundreds of thousands of dollars. These “business finance” decisions are weighed against anticipated patient volume, reimbursement rates from insurance providers, and the overall financial health of the institution. For individual patients, the cost of an ultrasound scan can range from a few hundred to over a thousand dollars, depending on the facility, geographical location, and whether additional procedures like Doppler are included. While many health insurance plans cover breast ultrasounds, particularly when medically indicated, out-of-pocket expenses, deductibles, and co-pays can still be a burden, falling under “personal finance” considerations.
However, the “money” equation dramatically shifts when considering the long-term economic benefits of early diagnosis. Detecting breast cancer at an early stage, often when it’s small and confined to the breast (stage I or II), significantly improves the chances of successful treatment and survival. Early-stage cancers typically require less aggressive and less extensive treatments compared to advanced-stage cancers. For instance, treatment for localized breast cancer might involve lumpectomy and radiation, whereas metastatic cancer often requires prolonged chemotherapy, multiple surgeries, and more intensive supportive care. The cost difference between treating early-stage and late-stage breast cancer can be tens of thousands of dollars, if not more, per patient.
From a societal perspective, early diagnosis means that individuals can return to work and maintain productivity sooner, reducing the economic burden of chronic illness. It also reduces the strain on the healthcare system by minimizing the need for complex, long-term care. Therefore, while there are upfront costs associated with comprehensive screening programs and advanced diagnostic technologies like ultrasound, these are often dwarfed by the massive long-term financial savings and improved quality of life that early detection affords. Investing in technologies that can more accurately and earlier identify what breast cancer looks like on an ultrasound is, in essence, an investment in future health and economic stability.
Funding Innovation: Investments in Medical Tech and Accessibility
The continuous innovation in ultrasound technology, particularly the integration of AI and more sophisticated imaging capabilities, relies heavily on significant “investing” – both from venture capital in startups and substantial R&D budgets within established medical device companies. These investments drive the creation of new “financial tools” and solutions that make diagnostics more accurate, faster, and eventually, more affordable. For example, venture capitalists pouring money into companies developing novel AI algorithms for medical image analysis are directly fueling the next generation of diagnostic capabilities, which will further refine our understanding of breast cancer’s subtle ultrasound signatures.
Accessibility is another critical financial aspect. Even the most advanced technology is ineffective if it cannot reach the patients who need it most. This is where government policies and health insurance play a vital role. Public health initiatives and subsidies can help make screening programs, including ultrasounds, more widely available, particularly in underserved communities or for populations at higher risk. The challenge lies in balancing the cost of cutting-edge technology with the imperative of universal access, ensuring that financial barriers do not prevent early detection.
Furthermore, the rise of “online income” and “side hustles” within the digital economy can even indirectly contribute to this sector. For instance, developers creating educational apps about breast health, or freelancers specializing in data annotation for AI medical imaging training, are part of a broader ecosystem that supports and disseminates health information and technological advancements. While not directly funding large-scale equipment purchases, these smaller, agile financial flows contribute to awareness, education, and the refinement of the digital tools that underpin modern diagnostics. Ultimately, the intricate financial ecosystem, encompassing private investment, public funding, and individual financial choices, dictates the pace of innovation and the breadth of access to technologies that help us precisely identify and combat breast cancer.
In conclusion, “what does breast cancer look like on an ultrasound” is a question that leads us beyond simple medical imagery into a sophisticated interplay of cutting-edge technology, strategic brand building, and complex financial decisions. The evolution of ultrasound machines, the integration of AI, and the digitalization of health data exemplify how technological advancements enhance diagnostic accuracy and efficiency. Concurrently, healthcare providers and medical technology companies leverage branding to build trust and market innovation, reassuring patients and driving the adoption of superior diagnostic tools. Finally, the financial dynamics—from the costs of equipment and procedures to the profound long-term savings of early detection and the investment in future innovations—underscore the economic imperative and societal benefits of ensuring broad access to these critical diagnostic capabilities. Together, these three dimensions form an interconnected framework that is continually reshaping our approach to breast cancer detection, offering hope for more precise diagnoses and improved outcomes globally.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.