In an increasingly data-driven world, our understanding and management of personal health metrics have undergone a profound transformation, largely fueled by advancements in technology. The Body Mass Index (BMI), a simple calculation derived from an individual’s weight and height, has long served as a foundational tool for assessing general health and identifying potential risks. However, its interpretation, particularly at the extremes, requires nuance and careful consideration. The question “what BMI is anorexic” points to a critical area where data, interpretation, and intervention intersect, making it fertile ground for exploring how technology assists in identifying, monitoring, and supporting individuals with health challenges, without ever replacing professional medical judgment.
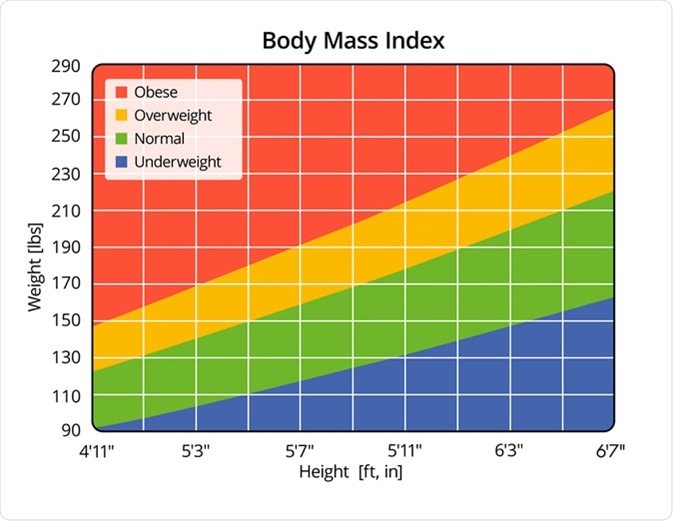
This article will delve into the technological landscape surrounding BMI, exploring how digital tools, applications, and artificial intelligence contribute to our understanding of health metrics. We will examine how technology aids in tracking and interpreting BMI, how AI can offer predictive insights, the role of digital platforms in health support, and the paramount importance of data security—all viewed through the lens of understanding and addressing the complexities associated with BMI, including those values that may indicate a serious condition like anorexia nervosa. It’s crucial to state upfront that while technology can provide valuable data and flags, it is no substitute for a qualified healthcare professional’s diagnosis and care.
The Digital Frontier of BMI Calculation and Tracking
The days of manual calculations and static charts for BMI are largely behind us. Modern technology has ushered in an era of seamless, continuous, and often automated BMI tracking, integrating it into our daily lives and broader health profiles. This shift has democratized access to health data, allowing individuals to monitor their metrics with unprecedented ease, though with it comes the responsibility of accurate interpretation and the need for professional guidance when values fall outside healthy ranges.
Wearable Tech and Automated BMI Assessment
Wearable technology has become ubiquitous, offering a suite of health monitoring features, from heart rate and sleep patterns to activity levels. While most wearables don’t directly measure BMI in real-time, many sophisticated smart scales integrate with wearable ecosystems and companion apps to provide automated BMI calculations. Users input their height once, and subsequent weigh-ins automatically update their BMI, often displaying trends over time. This continuous data stream allows individuals and, with consent, their healthcare providers to observe fluctuations and identify patterns that might warrant further investigation.
For instance, a sharp, unexplainable decline in BMI over a short period, as might be observed in someone developing anorexia nervosa, could be a flag raised by such integrated systems. These technologies do not diagnose, but they act as passive data collectors that can highlight deviations from established baselines or healthy ranges, prompting the user to seek professional medical advice. The convenience of these tools means that such crucial data points are less likely to be missed, potentially enabling earlier intervention.
Mobile Applications for Personalized Health Data
Beyond wearables, a vast ecosystem of mobile applications dedicates itself to health and nutrition tracking. These apps often allow users to log their weight, height, and other relevant metrics, instantly calculating and visualizing their BMI. Many go further, integrating with food diaries, exercise logs, and even mood trackers to provide a holistic view of an individual’s lifestyle and its impact on their physical metrics.
For someone tracking their health, these apps can be incredibly insightful. They can show how dietary changes affect weight and BMI, or how exercise impacts body composition. However, in the context of conditions like anorexia nervosa, the same tools can become problematic if used obsessively or without proper guidance. A key challenge for app developers is to design interfaces that promote healthy monitoring without inadvertently facilitating unhealthy obsessions. Features like setting “healthy range” alerts rather than specific weight goals, or integrating direct links to professional medical advice, are crucial for responsible app design. The data compiled in these apps, when shared with a doctor, can provide a comprehensive historical record that greatly assists in diagnosis and treatment planning.
AI and Predictive Analytics in Identifying Health Risks
Artificial intelligence and machine learning are rapidly transforming the landscape of healthcare, moving beyond simple data collection to sophisticated analysis and predictive modeling. When applied to health metrics like BMI, AI has the potential to offer unprecedented insights, aiding in the early identification of potential health risks, including those associated with dangerously low BMIs.
Machine Learning for Early Detection of Anomaly
Machine learning algorithms excel at pattern recognition in large datasets. In the context of health, this means AI can analyze a combination of BMI trends, dietary intake patterns, activity levels, and even psychological markers (if collected and consented to) to identify anomalies that might suggest the onset or progression of an eating disorder like anorexia nervosa. For example, an AI model could flag an individual whose BMI is consistently trending downwards into a clinically underweight category, especially if combined with self-reported restrictive eating patterns or an unusual increase in exercise intensity.
These AI systems are not designed to diagnose anorexia; rather, they are built to identify risk factors and patterns of concern that warrant professional clinical evaluation. They act as sophisticated early warning systems for healthcare providers, allowing for targeted interventions before a condition becomes critical. The power lies in their ability to process vast amounts of data more rapidly and comprehensively than a human could, sifting through noise to pinpoint signals of potential distress.
Ethical Considerations in AI-Driven Health Alerts
While the potential of AI in health risk identification is immense, it also presents significant ethical challenges. The sensitive nature of conditions like anorexia nervosa demands careful consideration regarding privacy, data accuracy, and the potential for misinterpretation or over-alerting. AI models must be trained on diverse and representative datasets to avoid bias, and their outputs must always be understood as probabilistic indicators, not definitive diagnoses.
Furthermore, the implementation of AI-driven alerts for conditions like eating disorders requires a robust ethical framework. Who receives the alert? How is it communicated? How is patient autonomy respected? It’s critical that any system designed to flag concerning BMI trends or related behaviors prioritizes patient well-being, respects privacy, and always channels individuals towards qualified human medical professionals for diagnosis, counseling, and treatment. The technology should empower, not alarm, and certainly not replace the empathetic and informed judgment of a medical expert.
The Role of Digital Platforms in Supporting Health and Wellness
Beyond individual tracking and AI-driven insights, digital platforms play a crucial role in creating ecosystems for health support and information dissemination. These platforms can be instrumental in connecting individuals with resources, professional help, and communities that foster recovery and well-being.
Telehealth and Remote Monitoring for Nutritional Support
Telehealth has revolutionized access to healthcare, particularly for conditions that benefit from ongoing consultation and support, such as eating disorders. For individuals managing their BMI and health in general, telehealth platforms allow for remote consultations with dietitians, nutritionists, therapists, and doctors. This accessibility is particularly vital for those living in rural areas, individuals with mobility challenges, or those who face social stigma in seeking in-person care.
Remote monitoring, facilitated by connected devices and apps, enables healthcare professionals to track a patient’s progress, including BMI changes, nutritional intake, and activity levels, in real-time. This continuous oversight allows for timely adjustments to treatment plans and provides a safety net, ensuring that concerning trends, such as a dangerously low BMI in someone recovering from anorexia, are quickly identified and addressed. The ability to maintain regular contact with a support team without the burden of constant physical appointments significantly enhances the continuity of care.
Online Communities and Responsible Information Sharing
The internet hosts countless online communities dedicated to health, wellness, and specific conditions. For individuals struggling with body image issues or eating disorders, these communities can be a source of both support and significant risk. On the one hand, well-moderated forums and support groups can offer a sense of belonging, shared experience, and encouragement for recovery. They can be a place where individuals feel understood and less isolated, sharing strategies for coping and celebrating progress.
On the other hand, the unmoderated nature of some online spaces can lead to the proliferation of harmful content, including pro-anorexia (“pro-ana”) websites and social media groups that glorify dangerously low BMIs and disordered eating behaviors. Technology companies and platform providers bear a significant responsibility to monitor and remove such content, promoting environments that prioritize user safety and well-being. For health-focused platforms, ensuring that information shared is evidence-based, reviewed by experts, and encourages professional medical consultation is paramount. The goal is to leverage the connective power of digital platforms to build positive, supportive communities that guide individuals towards healthy habits and professional help when needed, rather than inadvertently exacerbating conditions like anorexia.
Data Security and Privacy in Health Tracking Apps
The extensive collection and analysis of personal health data, including sensitive metrics like BMI and information related to mental health conditions, necessitate an unwavering commitment to data security and user privacy. Without robust protections, the very tools designed to help us can expose us to significant risks.
Protecting Sensitive BMI and Health Records
Health tracking apps and platforms often collect a wealth of deeply personal information, ranging from physical measurements and dietary habits to location data and even biometric identifiers. This data, especially when it hints at a condition like anorexia nervosa, is exceptionally sensitive and must be protected with the highest standards of cybersecurity. Breaches of such data can lead to identity theft, discrimination, and severe emotional distress.
Developers of health technology must implement end-to-end encryption, secure server infrastructure, and strict access controls. Regular security audits and compliance with international data protection regulations (like GDPR and HIPAA) are not just good practice but essential requirements. Users, in turn, must be diligent in understanding privacy policies, using strong, unique passwords, and enabling multi-factor authentication for their health accounts. The trust placed in these digital health tools is directly proportional to their demonstrable commitment to safeguarding personal information.
User Empowerment Through Data Control
Beyond technical security measures, empowering users with control over their own health data is a fundamental ethical imperative. Individuals should have clear, easy-to-understand options for managing who can access their BMI and other health information, how it is used, and for how long it is stored. This includes the ability to grant and revoke consent for data sharing with third-party applications, researchers, or even family members.
Transparency about data practices is key. Users should know exactly what data is being collected, why it’s being collected, and what algorithms are being applied to it. In the context of sensitive topics like BMI and potential eating disorders, empowering individuals with granular control over their data can foster greater trust and encourage responsible engagement with digital health tools. Ultimately, technology should serve as an enabling force, providing individuals with tools to understand and manage their health, while always upholding their right to privacy and self-determination regarding their most personal information.
In conclusion, while the question “what BMI is anorexic” primarily pertains to a medical diagnosis, the technological ecosystem surrounding health metrics like BMI plays a crucial, multifaceted role. From automated tracking and AI-driven risk identification to remote support and community platforms, technology offers powerful tools to collect, analyze, and act upon health data. However, its responsible application demands a commitment to ethical design, stringent data security, and an unwavering acknowledgment that technology augments, but never replaces, the expertise and empathy of human healthcare professionals. By leveraging technology wisely, we can enhance our collective ability to understand, monitor, and compassionately support individuals facing complex health challenges.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.