The medical landscape has undergone a tectonic shift over the last decade, transitioning from generalized treatment protocols to highly specialized, data-driven interventions. When discussing the chances of surviving ovarian cancer, the conversation is no longer strictly limited to biological factors or surgical skill; it is now inextricably linked to the rapid advancement of technology. From artificial intelligence and machine learning to genomic sequencing and robotic-assisted surgery, the “silent killer” is finally being met with a suite of digital and mechanical tools designed to detect it earlier and treat it with unprecedented precision.
In the past, ovarian cancer survival rates were largely dictated by the stage at which the disease was discovered, often hampered by the lack of clear symptoms. However, the integration of high-tech diagnostic software and innovative biotech platforms is fundamentally altering the statistical outlook for patients. By examining the intersection of oncology and technology, we can see how the digital revolution is providing new hope and tangible improvements in survival outcomes.
The AI Revolution in Early Detection and Diagnosis
One of the primary reasons ovarian cancer has historically carried a daunting prognosis is the difficulty of early detection. Conventional imaging often fails to distinguish between benign cysts and malignant tumors until the disease has progressed. Today, artificial intelligence (AI) is bridging this gap, acting as a powerful secondary eye for radiologists.
Machine Learning and Radiomics: Seeing the Invisible
Machine learning algorithms are now being trained on millions of historical ultrasound and CT scan images to identify patterns that are imperceptible to the human eye. This field, known as radiomics, extracts high-dimensional data from clinical images, allowing computers to identify textural features of a tumor that correlate with malignancy.
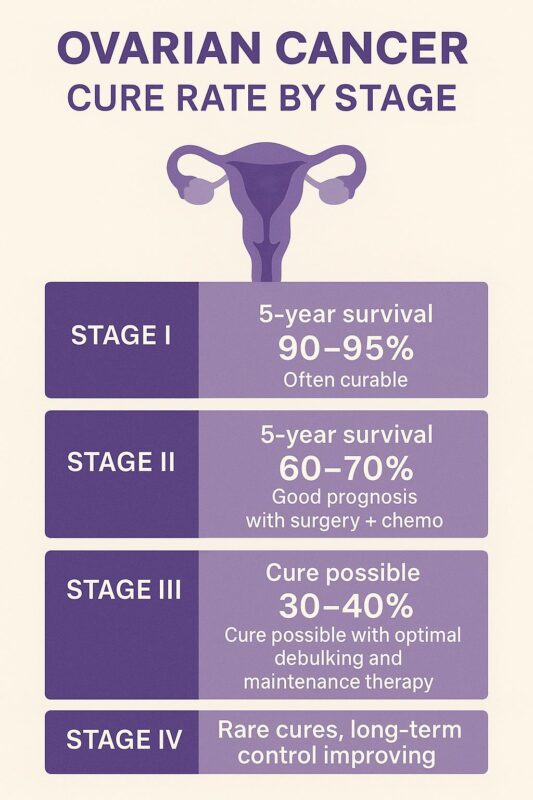
By utilizing deep learning neural networks, these software tools can provide a “probability score” for malignancy with a higher degree of accuracy than traditional methods. This early intervention is critical; when ovarian cancer is detected at Stage I, the five-year survival rate is approximately 90%. Technology is the primary vehicle moving us toward a future where “early detection” is the norm rather than the exception.
Liquid Biopsies: The Tech Behind Minimally Invasive Screening
Beyond imaging, the tech sector has pioneered “liquid biopsy” platforms. These are highly sensitive diagnostic tools that look for circulating tumor DNA (ctDNA) or specific protein biomarkers in a simple blood sample. The technology relies on ultra-sensitive sequencing platforms and bioinformatics software that can filter out “noise” to find microscopic fragments of cancer. For patients at high genetic risk, this tech-enabled monitoring offers a non-invasive way to track health in real-time, significantly boosting the chances of catching a recurrence or a primary tumor at its most treatable phase.
Precision Medicine: Coding the Path to Long-Term Survival
Once a diagnosis is made, the technological focus shifts from detection to personalization. The “one-size-fits-all” approach to chemotherapy is being replaced by precision medicine, a field where software and biology converge to create a custom roadmap for every patient.
Genomic Sequencing and Personalized Treatment Protocols
The advent of Next-Generation Sequencing (NGS) has been a game-changer for ovarian cancer survival. NGS allows doctors to sequence the entire genome of a tumor quickly and affordably. Once the data is captured, sophisticated bioinformatics software analyzes the mutations—such as BRCA1, BRCA2, or HRD (Homologous Recombination Deficiency).
This data is then cross-referenced with massive databases of clinical trials and pharmacological profiles to determine which specific drugs will be most effective. This “matching software” ensures that patients do not waste precious time on treatments that their specific tumor is genetically programmed to resist. By narrowing the target, technology reduces toxicity and increases the efficacy of the intervention, directly correlating to improved long-term survival rates.
CRISPR and Targeted Gene Editing Technologies
While still in the investigative and early clinical stages, CRISPR-Cas9 and other gene-editing technologies represent the frontier of ovarian cancer tech. These tools allow researchers to “snip” out or deactivate the genetic instructions that allow cancer cells to replicate or evade the immune system. The software used to design these genetic “guides” must be perfect, representing a pinnacle of computational biology. As these technologies mature, they offer a future where we don’t just treat cancer; we reprogram the body’s cellular logic to defeat it.
The Role of Big Data and Predictive Analytics in Prognosis
Surviving cancer is a long-term journey that requires constant monitoring and adjustment. This is where big data and predictive analytics play a crucial role. By aggregating data from thousands of patients globally, technology is providing clinicians with a “predictive crystal ball” that helps manage the chances of survival over a 10-year horizon.
Real-World Evidence (RWE) and Longitudinal Patient Tracking
Real-World Evidence platforms collect data from electronic health records (EHRs), wearable devices, and insurance claims to see how treatments perform outside of controlled clinical trials. For an ovarian cancer survivor, this might involve using an app to track symptoms or wearable tech to monitor vital signs during recovery.
Algorithms analyze this longitudinal data to spot “red flags” that might indicate a recurrence weeks before a physical symptom appears. By treating a recurrence while it is still at a molecular level, the technological ecosystem surrounding the patient significantly extends their life expectancy.
Cloud Computing and Global Research Collaboration
The sheer volume of data required to solve the complexities of ovarian cancer is too large for any single hospital to manage. Cloud computing platforms allow researchers in London, Tokyo, and New York to share genomic data and treatment outcomes in real-time. This global “hive mind,” powered by high-performance computing (HPC), accelerates the pace of discovery. A breakthrough in a tech lab in Silicon Valley can be implemented in a clinic in rural Europe within months, rather than years, ensuring that the latest survival-enhancing protocols are available to all.
Emerging Surgical Robotics and Minimally Invasive Innovation
Surgery remains a cornerstone of ovarian cancer treatment, often involving the removal of the primary tumor (debulking). However, the “chances of survival” are often tied to how well a patient recovers from the surgery itself. This is where surgical robotics and augmented reality (AR) are making an impact.
Robotic-Assisted Surgery: Enhancing Precision and Recovery
Systems like the Da Vinci surgical robot allow surgeons to perform complex procedures through tiny incisions with a level of precision that exceeds the human hand. These robots utilize high-definition 3D vision systems and “wristed” instruments that can rotate further than a human wrist.
From a survival perspective, the benefits are clear: less blood loss, lower risk of infection, and a faster return to chemotherapy. In ovarian cancer, the time between surgery and the start of systemic treatment is a critical window; robotic tech ensures that the patient’s body is ready for the next phase of the fight as quickly as possible.
Smart Post-Operative Monitoring and Telehealth
The integration of IoT (Internet of Things) devices in the post-operative phase has revolutionized recovery. Smart sensors can monitor a patient’s internal healing, while telehealth platforms allow for immediate consultation with specialists. This tech-heavy approach to “aftercare” ensures that complications—which can often be fatal for cancer patients with suppressed immune systems—are caught and treated immediately. By safeguarding the patient during their most vulnerable moments, these tools provide a safety net that reinforces the statistical chances of survival.

The Future Outlook: Tech-Driven Survival Metrics
As we look toward the future, the question “what are the chances of surviving ovarian cancer” will increasingly be answered by the sophistication of the technology stack available to the patient. We are moving toward a reality where “digital twins”—virtual models of a patient’s unique anatomy and tumor biology—are used to simulate surgeries and drug reactions before they ever happen in the real world.
The synthesis of AI, genomics, and robotics is creating a formidable barrier against a disease that was once considered an unbeatable foe. While the biological challenges of ovarian cancer remain significant, the technological tools we are building to combat it are evolving at an exponential rate. For patients and clinicians alike, the “tech” in oncology is not just a collection of gadgets; it is the very infrastructure of hope, providing the precision, speed, and data necessary to tilt the scales of survival in the patient’s favor.
In this new era, survival is a data-driven outcome. By leveraging the power of advanced software and hardware, the medical community is turning the tide, ensuring that every patient has the best possible technological advantage in their fight for life.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.