The presence and quantity of epithelial cells in a urine sample are crucial indicators within the realm of medical diagnostics, offering insights into the health of the urinary tract. While often overlooked, these cells play a vital role in maintaining the integrity and function of the kidneys, ureters, bladder, and urethra. A routine urinalysis, a cornerstone of basic medical assessment, frequently examines these cellular components to detect potential abnormalities or diseases. Understanding what epithelial cells are, where they originate from, and what their presence signifies can empower individuals to better comprehend their health status and engage more effectively with their healthcare providers. This article will delve into the nature of epithelial cells in urine, their diagnostic significance, and the various factors influencing their detection.
The Cellular Landscape of the Urinary Tract
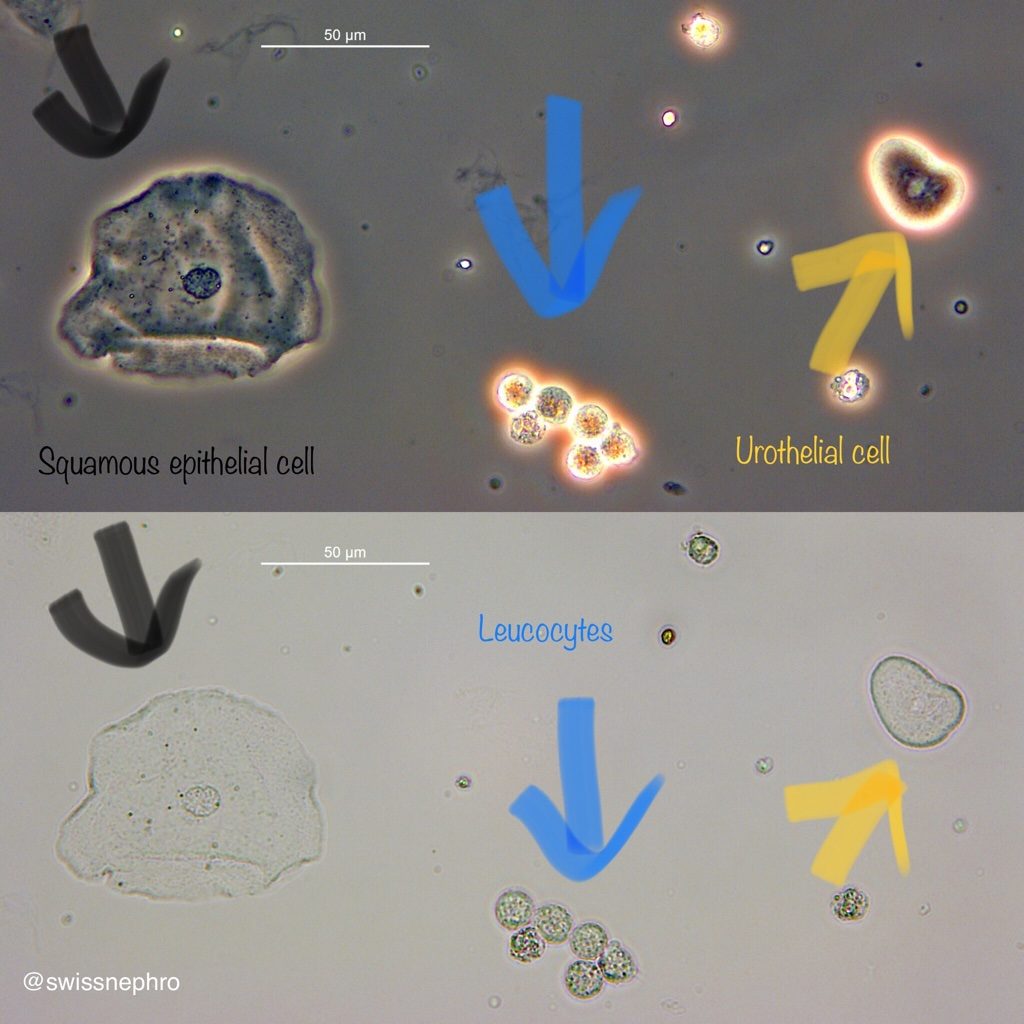
Epithelial cells form the protective lining of numerous organs and cavities within the body, and the urinary tract is no exception. These cells are essential for creating a barrier against pathogens and facilitating transport processes. Within the urinary system, different types of epithelial cells are found, each with distinct origins and characteristics. The distinction between these cell types is often key to interpreting urinalysis results.
Squamous Epithelial Cells: The Outermost Layer
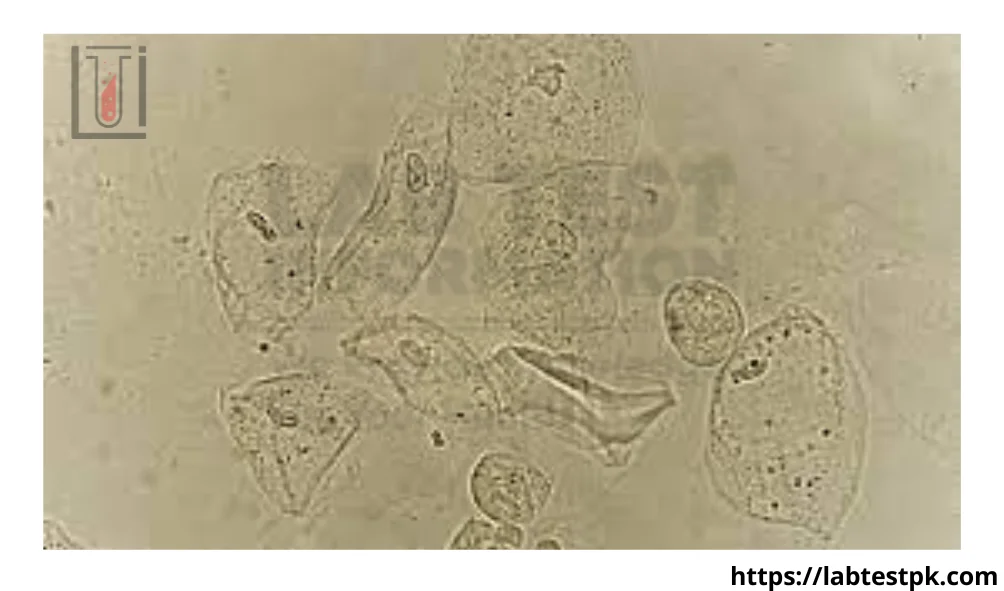
Squamous epithelial cells are flat, thin, and irregularly shaped cells that originate from the outer lining of the genitourinary tract. In females, these cells are most commonly found in the lower portion of the urethra and the external genitalia. In males, they can also be present in the distal urethra. Their presence in urine is generally considered normal, especially in small numbers. They are shed continuously as part of the natural turnover of the epithelial lining.
- Origin and Characteristics: These cells are characterized by their large size, polygonal shape, and a small, centrally located nucleus. They are readily identified under a microscope due to their distinct morphology.
- Normal Presence: A few squamous epithelial cells in a urine sample are not usually a cause for concern. They often indicate that the sample may have been collected with some contamination from the external genital area. Proper hygiene during sample collection, such as cleaning the periurethral area before urinating, can minimize their presence.
- When to Be Concerned: A significantly increased number of squamous epithelial cells, particularly if they are accompanied by other abnormal findings, might suggest a potential issue. However, in isolation, a high count is more likely to be a reflection of collection technique rather than an underlying pathology.
Transitional Epithelial Cells: The Inner Lining
Transitional epithelial cells, also known as urothelial cells, are found lining the renal pelvis, ureters, bladder, and the upper part of the urethra. This type of epithelium is unique in its ability to stretch and contract, accommodating changes in bladder volume. These cells are typically rounded or pear-shaped with a relatively large, often centrally located nucleus.
- Origin and Characteristics: Transitional cells are more varied in shape than squamous cells. They can appear rounded, oval, or even somewhat columnar depending on their degree of hydration and functional state. Their nucleus is generally larger and more prominent than that of squamous cells.
- Normal Presence: A small to moderate number of transitional epithelial cells in urine can be considered normal. Like squamous cells, they are continuously shed from the lining of the urinary tract.
- Diagnostic Significance: An increased number of transitional epithelial cells, especially when they appear atypical (e.g., larger, with irregular nuclei, or in clusters), can be a significant finding. It may indicate inflammation, infection, or, in more serious cases, the presence of a tumor within the urinary tract, such as bladder cancer or urothelial carcinoma. Certain medical procedures, like catheterization, can also lead to increased shedding of these cells.
Renal Tubular Epithelial Cells: The Kidney’s Workhorses
Renal tubular epithelial cells are the primary cells that make up the tubules of the kidney nephrons. These cells are responsible for reabsorbing essential substances from the filtrate and secreting waste products, playing a critical role in regulating blood pressure, electrolyte balance, and waste removal. These cells are typically smaller than squamous or transitional cells and often have a more rounded shape with a visible nucleus.
- Origin and Characteristics: These cells are smaller and often more rounded than transitional or squamous cells. They may appear singly or in small clumps. Their nucleus is typically round and centrally located.
- Normal Presence: In a healthy individual, very few renal tubular epithelial cells are normally found in the urine. Their presence in larger quantities is a strong indicator of kidney damage or disease.
- Diagnostic Significance: The presence of renal tubular epithelial cells in urine is a sensitive marker for acute tubular injury or necrosis (ATN), a condition often caused by reduced blood flow to the kidneys or exposure to nephrotoxic substances. Diseases affecting the glomeruli or interstitium of the kidney can also lead to increased shedding of these cells. Conditions like acute kidney injury (AKI), chronic kidney disease (CKD), and certain types of glomerulonephritis can result in elevated levels. Their appearance can also signify toxic damage to the kidneys from medications or heavy metals.
Interpreting Epithelial Cells in Urinalysis
The findings from a urinalysis, including the type and quantity of epithelial cells present, are interpreted by a healthcare professional in the context of the patient’s overall health, symptoms, and other laboratory results. It is important to remember that a single finding of epithelial cells, especially squamous cells, may not be indicative of a serious problem.
Quantifying Epithelial Cells: The Standard Approach
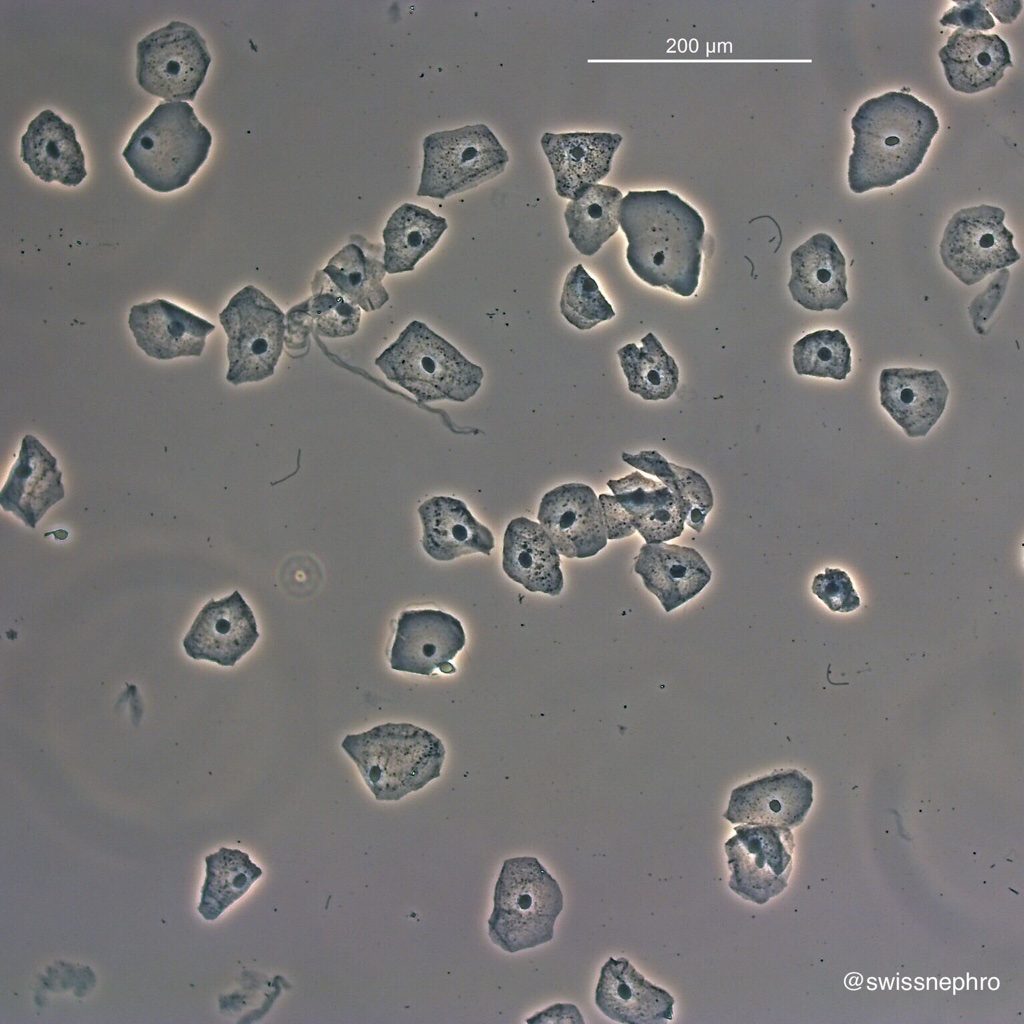
When examining a urine sample under a microscope, the pathologist or laboratory technician will typically count the number of epithelial cells seen per high-power field (HPF). The interpretation of these counts is often standardized within laboratory guidelines.
- Squamous Epithelial Cells: Generally, fewer than 15-20 squamous epithelial cells per HPF are considered within normal limits, often suggesting proper sample collection. A significantly higher number might prompt a recommendation for re-collection.
- Transitional Epithelial Cells: A few transitional cells per HPF are normal. An increased number (e.g., >5-10 per HPF) may warrant further investigation, especially if they appear abnormal.
- Renal Tubular Epithelial Cells: The presence of even a few renal tubular epithelial cells (e.g., 1-3 per HPF) can be concerning, and higher counts are strongly suggestive of kidney pathology.
Factors Influencing Epithelial Cell Presence
Several factors can influence the number and type of epithelial cells found in a urine sample, beyond underlying medical conditions.
- Sample Collection Technique: As mentioned, improper hygiene during collection can lead to contamination with squamous epithelial cells.
- Hydration Status: Dehydration can concentrate the urine, potentially leading to a higher perceived number of cells per field, even if the actual shedding rate remains the same.
- Urinary Tract Infections (UTIs): UTIs can cause inflammation of the urinary tract lining, leading to increased shedding of transitional and sometimes squamous epithelial cells.
- Medications and Toxins: Certain medications and exposure to toxins can damage the lining of the urinary tract, particularly the renal tubules, resulting in increased shedding of epithelial cells.
- Trauma or Procedures: Catheterization, cystoscopy, or other urological procedures can cause temporary trauma to the lining, leading to increased cell shedding.
- Pregnancy: Hormonal changes during pregnancy can sometimes lead to increased shedding of epithelial cells.
When to Seek Medical Advice
The presence of epithelial cells in a urine test is just one piece of the diagnostic puzzle. It is crucial not to self-diagnose based solely on this finding. If your urinalysis report indicates an unusual number or type of epithelial cells, it is essential to discuss these results with your doctor.
Understanding Your Urinalysis Report
Your doctor will review your urinalysis report in conjunction with your medical history, symptoms, and other diagnostic tests. They will consider:
- The specific type of epithelial cells found: Renal tubular cells are generally more concerning than squamous cells.
- The quantity of epithelial cells: A small increase may be insignificant, while a large increase warrants attention.
- The presence of other abnormalities: For example, the presence of white blood cells, red blood cells, bacteria, or protein in the urine alongside epithelial cells can provide more clues about the underlying condition.
- Your symptoms: Symptoms such as pain during urination, frequent urination, cloudy or bloody urine, flank pain, or swelling can help your doctor narrow down the potential causes.
Potential Underlying Conditions
The significance of epithelial cells in urine lies in their potential to signal a variety of conditions affecting the urinary tract and kidneys. These can range from minor irritations to serious diseases.
- Urinary Tract Infections (UTIs): Inflammation caused by bacterial infections is a common reason for increased epithelial cell shedding.
- Kidney Diseases: Conditions such as acute kidney injury (AKI), chronic kidney disease (CKD), glomerulonephritis, and interstitial nephritis can all lead to the presence of renal tubular epithelial cells.
- Kidney Stones: Stones can cause irritation and inflammation, leading to increased cell shedding.
- Bladder Cancer and Other Urological Malignancies: The presence of atypical transitional epithelial cells can be an early indicator of cancer within the urinary tract.
- Drug-Induced Nephrotoxicity: Certain medications, including some antibiotics, NSAIDs, and chemotherapy drugs, can be toxic to the kidneys and cause damage to the tubular cells.
- Glomerular Diseases: While glomerular cells themselves are not typically shed into the urine, damage to the glomeruli can indirectly affect tubular function and lead to the presence of tubular cells.
- Viral Infections: Some viral infections can impact the urinary tract and kidneys, leading to epithelial cell abnormalities.
Next Steps in Diagnosis and Management
If your doctor identifies a concerning number or type of epithelial cells in your urine, they may recommend further investigations. These could include:
- Repeat Urinalysis: To confirm the initial findings and assess for changes.
- Urine Culture: To identify the presence and type of bacteria in case of a suspected UTI.
- Blood Tests: To assess kidney function (e.g., creatinine, BUN) and electrolyte balance.
- Imaging Studies: Ultrasound, CT scan, or MRI of the kidneys and urinary tract to visualize structural abnormalities.
- Cystoscopy: A procedure to visually examine the bladder and urethra using a flexible scope.
- Renal Biopsy: In some cases, a small sample of kidney tissue may be taken for microscopic examination to diagnose specific kidney diseases.
By understanding the role of epithelial cells in a urine test and knowing when to consult a healthcare professional, individuals can take proactive steps towards maintaining their urinary tract and kidney health.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.