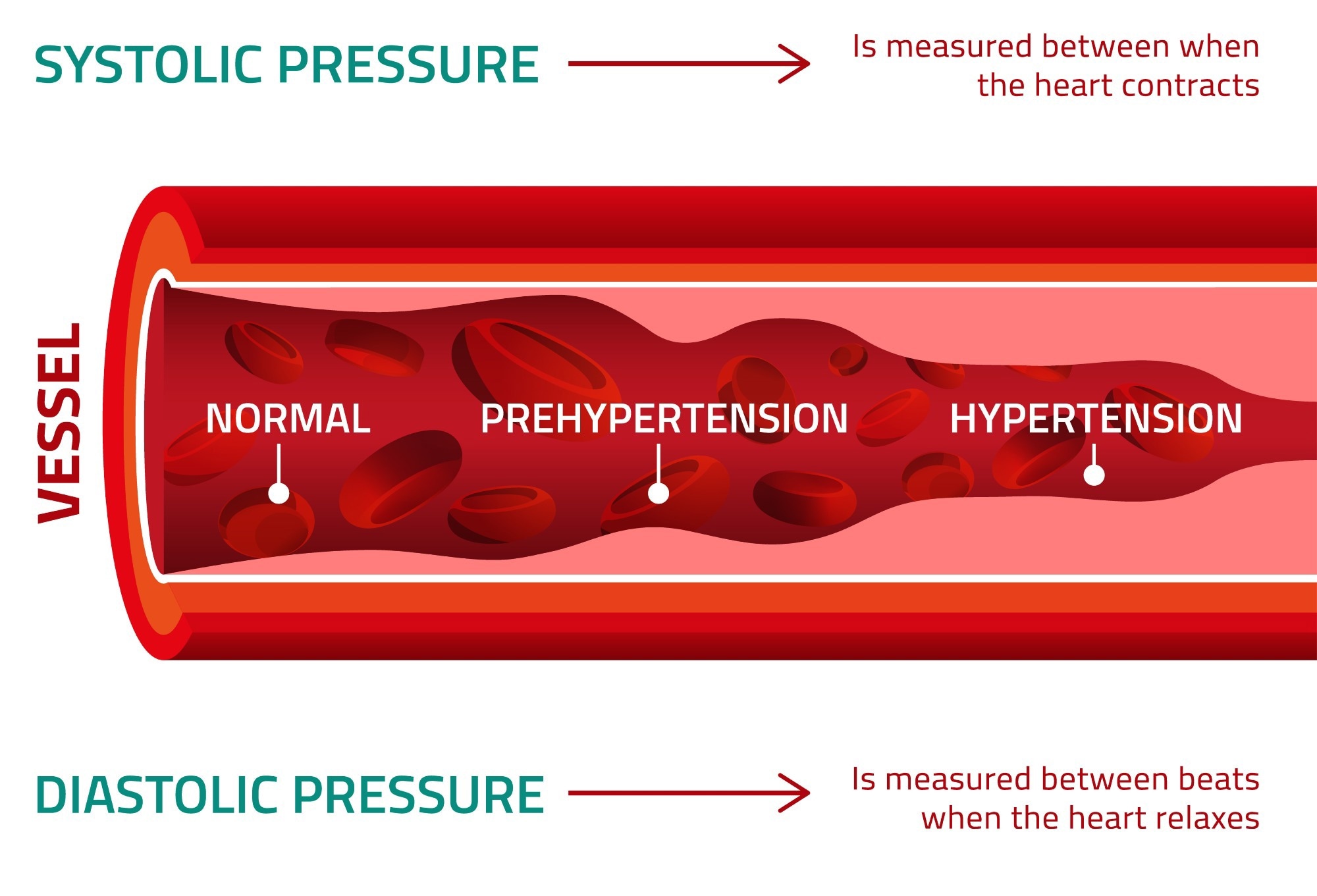
Understanding the forces that drive our blood pressure is crucial for maintaining long-term health. While systolic blood pressure, the top number, reflects the pressure in your arteries when your heart beats, diastolic blood pressure, the bottom number, indicates the pressure in your arteries when your heart rests between beats. An elevated diastolic number, often a concern in medical diagnostics, signals that your arteries are experiencing higher resistance even when your heart isn’t actively pumping. This persistent pressure can put undue strain on your cardiovascular system.
While the initial impulse might be to seek a quick fix or a single definitive answer, the reality is far more nuanced. The causes of rising diastolic blood pressure are often multifactorial, intertwining physiological responses with lifestyle choices and environmental influences. This article will explore these causes, drawing parallels and insights from the interconnected worlds of technology, brand perception, and financial well-being, demonstrating how seemingly disparate fields can offer valuable perspectives on a fundamental aspect of our health.

The Silent Squeeze: Understanding Arterial Resistance and Diastolic Pressure
Diastolic blood pressure is a reflection of the elasticity and resistance within your arterial walls. When your heart pumps, blood surges through arteries that should ideally be supple and able to expand to accommodate the flow. As the heart relaxes, these elastic walls recoil, maintaining pressure and ensuring blood continues to circulate throughout the body. However, when these walls become stiffer or the volume of blood circulating is higher than the vessels can comfortably handle during the resting phase, diastolic pressure rises.
Think of it like a high-pressure hose. If the hose is old and hardened, it can’t expand much when water is forced through. When the water flow stops, the hose retains a significant internal pressure due to its lack of flexibility. Similarly, hardened or constricted arteries require more force to push blood through them, and this force doesn’t dissipate as effectively when the heart is at rest.
Factors Contributing to Arterial Stiffening and Resistance
Several physiological processes and lifestyle choices can lead to the stiffening of arteries and increased vascular resistance, directly impacting diastolic blood pressure:
- Aging: As we age, our arteries naturally lose some of their elasticity. Collagen and elastin fibers in the arterial walls break down, leading to a less pliable structure. This is a natural part of the aging process, but it can be exacerbated by other risk factors.
- Atherosclerosis: This is a condition where plaque (a buildup of fat, cholesterol, and other substances) accumulates inside the arteries. This plaque narrows the arteries, making them less flexible and harder for blood to flow through, increasing resistance. The process of atherosclerosis is often driven by high cholesterol levels, inflammation, and other cardiovascular risk factors.
- Endothelial Dysfunction: The endothelium is the inner lining of blood vessels. It plays a critical role in regulating blood vessel tone, blood clotting, and inflammation. When the endothelium is damaged or not functioning properly, blood vessels can become less able to relax, leading to increased resistance. Factors like smoking, high blood sugar, and certain chronic diseases can impair endothelial function.
- Hormonal Changes: Fluctuations in certain hormones, particularly during menopause in women, can influence arterial stiffness and blood pressure. Estrogen plays a protective role in maintaining arterial elasticity, and its decline can contribute to increased diastolic pressure.
The Lifestyle Algorithm: How Our Habits Impact Diastolic Pressure
Beyond inherent physiological changes, our daily routines and lifestyle choices act as powerful algorithms influencing our diastolic blood pressure. These are areas where proactive management can yield significant results.
Diet: The Fuel for Arterial Health
What we consume directly impacts our cardiovascular system, from cholesterol levels to inflammation.
- High Sodium Intake: Excessive sodium consumption causes the body to retain water, which increases the volume of blood circulating. This extra volume puts more pressure on artery walls, both during systole and diastole. Furthermore, high sodium can interfere with the natural function of the endothelium.
- Unhealthy Fats: Diets high in saturated and trans fats contribute to the buildup of plaque in the arteries (atherosclerosis), leading to stiffening and narrowing. This makes it harder for blood to flow and increases resistance.
- Excessive Sugar: High sugar intake can lead to insulin resistance and inflammation, both of which negatively impact arterial health and function. Chronic inflammation can damage the endothelial lining.
- Low Potassium and Magnesium: These minerals play vital roles in regulating blood pressure. Potassium helps balance sodium levels and relax blood vessel walls, while magnesium is involved in muscle relaxation, including that of the blood vessels. Deficiencies can contribute to higher diastolic pressure.
Physical Activity: The Dynamic Regulator
Regular exercise is a cornerstone of cardiovascular health, acting as a powerful counterbalance to sedentary living.
- Sedentary Lifestyle: A lack of physical activity leads to deconditioning of the cardiovascular system. Muscles become weaker, and the heart has to work harder. Importantly, regular aerobic exercise helps improve the elasticity of blood vessels and can reduce arterial stiffness over time, thereby lowering diastolic pressure.
- Weight Management: Being overweight or obese significantly increases the risk of high blood pressure. Excess body fat, particularly around the abdomen, can disrupt hormonal balance and contribute to inflammation and insulin resistance, all of which negatively affect arterial function.
Stress and Sleep: The Unseen Drivers
Our mental and emotional states have a profound impact on our physical health, including blood pressure.
- Chronic Stress: When we experience prolonged stress, our bodies release hormones like cortisol and adrenaline. These hormones can cause blood vessels to constrict and heart rate to increase, leading to a temporary rise in blood pressure. Over time, chronic stress can contribute to lasting arterial damage and elevated diastolic pressure. This can be likened to a constant, low-level system alert that keeps your body in a state of heightened tension, impacting its core functions.
- Poor Sleep Quality: Inadequate or disrupted sleep can disrupt the body’s natural hormonal rhythms and stress response systems. This can lead to increased inflammation and impaired blood vessel function, contributing to elevated blood pressure, including diastolic pressure.

The Digital Echo: Technology and its Influence on Our Blood Pressure
In our increasingly digitized world, technology plays an unexpected role in shaping our physiological responses, including blood pressure regulation. While technology offers incredible tools for monitoring and managing health, certain aspects can inadvertently contribute to its rise.
The Screen Time Strain: Sedentary Habits and Mental Load
- Prolonged Screen Use: The ubiquitous nature of smartphones, computers, and tablets often leads to extended periods of sedentary behavior. This lack of physical activity directly contributes to the issues mentioned earlier regarding a sedentary lifestyle. Hours spent sitting at a desk or on a couch, absorbed in digital content, mean less time for movement that would benefit arterial elasticity and blood flow.
- Information Overload and Digital Stress: The constant barrage of information, notifications, and the pressure to be perpetually “online” can induce chronic stress. The need to process, respond, and engage with digital stimuli can keep our nervous systems in a heightened state, mirroring the effects of psychological stress on blood vessel constriction and overall cardiovascular strain. This constant mental engagement, without adequate rest or decompression, can become a significant contributor to elevated diastolic pressure.
- Sleep Disruption from Blue Light: The blue light emitted from screens can interfere with melatonin production, the hormone that regulates sleep. Late-night screen use can therefore lead to poor sleep quality, further exacerbating the stress response and negatively impacting blood pressure.
The Tech Solution: Leveraging Tools for Better Health
Despite the potential downsides, technology also offers powerful solutions for monitoring and managing blood pressure.
- Smart Health Devices and Apps: Wearable devices (smartwatches, fitness trackers) and dedicated blood pressure monitors are becoming increasingly sophisticated. These tools allow for continuous or frequent monitoring of blood pressure, providing valuable data to individuals and their healthcare providers. Apps can help track trends, identify patterns associated with lifestyle choices, and offer personalized reminders for medication or healthy habits. This data-driven approach can empower individuals to take a more proactive role in their health management.
- AI-Powered Health Insights: Artificial intelligence is being integrated into health platforms to analyze complex data sets from wearables and medical records. AI can identify subtle correlations between lifestyle factors, biometric data, and blood pressure fluctuations, offering personalized recommendations for diet, exercise, and stress management. These tools can provide a level of insight that might be difficult to discern through manual tracking alone.
- Telemedicine and Digital Health Platforms: Access to healthcare professionals through telemedicine can be crucial for individuals who struggle with consistent in-person appointments. Digital platforms can facilitate remote monitoring, medication management, and access to educational resources, making it easier to stay on track with treatment plans and address concerns promptly.
The Brand of Well-being: Perception, Marketing, and Personal Identity
While not as immediately direct as physiological factors, our perception of health, the way we brand ourselves as healthy individuals, and the marketing messages we encounter can subtly influence our behavior and, consequently, our blood pressure.
The Marketing Matrix: Influence and Choice
- Food Marketing: The pervasive marketing of processed foods, often high in sodium, sugar, and unhealthy fats, can influence dietary choices. Appealing advertising, particularly targeting children and young adults, can shape eating habits from an early age, contributing to the long-term development of hypertension. The branding of convenience and indulgence can overshadow the importance of balanced nutrition.
- Fitness and Wellness Branding: Conversely, the rise of positive branding around fitness, healthy eating, and mindfulness can encourage positive lifestyle changes. Inspiring campaigns and the portrayal of healthy living as aspirational can motivate individuals to adopt better habits, leading to improved cardiovascular health. The perceived “brand” of a healthy lifestyle can be a powerful motivator.
- Societal Norms and Peer Influence: The social environment and the prevailing attitudes towards health and lifestyle can significantly impact personal choices. If unhealthy habits are normalized or even celebrated, it can be more challenging to resist them. Conversely, a strong community or social circle that prioritizes well-being can provide support and accountability.
Personal Branding for Health: Self-Perception and Responsibility
- Taking Ownership: How we perceive our own health and our responsibility for it plays a crucial role. Individuals who “brand” themselves as health-conscious are more likely to actively seek information, make healthy choices, and adhere to treatment plans. This self-perception can be a powerful driver of positive behavioral change.
- Information Consumption: The way we consume information about health is also influenced by our personal branding. We are more likely to engage with content that aligns with our existing beliefs and aspirations. This can be a double-edged sword: it can reinforce healthy habits but also lead to confirmation bias, where individuals ignore information that contradicts their current lifestyle.
The Financial Foundation: Money, Stress, and Health Outcomes
Financial well-being is intrinsically linked to our overall health, with financial strain being a significant contributor to stress and its cascading effects on blood pressure.
The Stress of Scarcity: Economic Hardship and Health
- Financial Strain and Chronic Stress: Worries about debt, job security, and the ability to meet basic needs can lead to chronic stress. As previously discussed, this persistent stress response triggers the release of hormones that can elevate blood pressure. The constant anxiety associated with financial instability can have a detrimental and sustained impact on the cardiovascular system.
- Limited Access to Healthy Resources: Individuals facing financial difficulties may have limited access to nutritious food, safe environments for exercise, or quality healthcare. The cost of healthy groceries, gym memberships, or even doctor’s visits can be prohibitive, creating a cycle where poor financial health directly contributes to poorer physical health.
- Impact on Healthcare Adherence: Financial constraints can affect a person’s ability to afford medications, follow recommended dietary changes, or attend follow-up medical appointments. This can hinder effective management of existing hypertension or other health conditions, leading to a worsening of their condition, including elevated diastolic blood pressure.
Financial Tools for Health: Empowering Well-being
- Budgeting and Financial Planning: Effective budgeting and financial planning can alleviate financial stress. By understanding and managing their finances, individuals can reduce anxiety and create a sense of control, which can positively impact their overall well-being and, by extension, their blood pressure.
- Investing in Health: Viewing health as an investment rather than an expense can shift financial priorities. Allocating resources towards preventative care, healthy foods, and physical activity can yield significant returns in terms of long-term health and reduced healthcare costs down the line.
- Financial Literacy and Health Literacy: The intersection of financial literacy and health literacy is crucial. Understanding how to navigate healthcare systems, insurance plans, and the cost of various treatments empowers individuals to make informed decisions that benefit both their financial and physical health.
In conclusion, the rise in diastolic blood pressure is not a singular event but a complex interplay of physiological, lifestyle, technological, perceptual, and financial factors. By understanding these interconnected influences, we can adopt a holistic approach to managing our cardiovascular health, leveraging insights from diverse fields to cultivate a life of greater well-being.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.