Osteoarthritis (OA) is a pervasive degenerative joint disease that affects millions worldwide, causing pain, stiffness, and reduced mobility. As this chronic condition impacts our lives, understanding who to turn to for expert care becomes paramount. This article delves into the types of medical professionals who diagnose and treat osteoarthritis, framing their roles within the broader context of our modern lives – a world increasingly shaped by technological advancements, the strategic importance of branding, and the critical need for financial prudence. While the initial question might seem purely medical, the journey to managing OA is often intertwined with these other vital aspects of our existence.
Understanding Osteoarthritis: The Foundation of Your Treatment Plan
Before exploring the medical specialists, it’s crucial to grasp what osteoarthritis entails. It’s a condition where the protective cartilage that cushions the ends of your bones wears down over time. This can happen in any joint, but it most commonly affects the hands, knees, hips, and spine. The wear and tear can lead to bone rubbing against bone, resulting in pain, inflammation, and a gradual loss of flexibility.
The causes of osteoarthritis are multifaceted, including age, genetics, previous joint injuries, obesity, and overuse of certain joints. While there’s no cure for osteoarthritis, various treatments can help manage symptoms, improve function, and slow the progression of the disease. This is where understanding the right medical professional becomes essential.
The Primary Care Physician: Your First Line of Defense and Gateway to Specialists
Your journey to managing osteoarthritis often begins with a visit to your primary care physician (PCP). This could be a family doctor or an internist. PCPs are invaluable because they have a holistic view of your health. They can:
Initial Diagnosis and Symptom Assessment
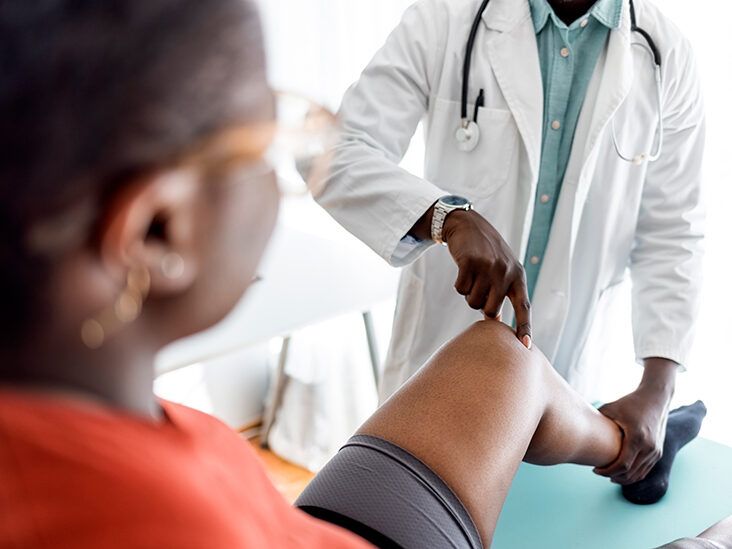
Your PCP will conduct a thorough medical history, asking about your symptoms, their duration, and any factors that seem to exacerbate them. They will perform a physical examination, checking for joint tenderness, swelling, redness, and limitations in your range of motion. This initial assessment is crucial for determining if osteoarthritis is a likely cause of your discomfort.
Ordering Diagnostic Tools: Leveraging Technology for Accuracy
To confirm a diagnosis and rule out other conditions, your PCP will likely order diagnostic tests. This is where the “Tech” pillar of our website’s focus becomes directly relevant to your health.
- X-rays: These are the most common imaging tests used to diagnose osteoarthritis. They can reveal the extent of cartilage loss, bone spurs, and joint space narrowing. Modern digital X-ray machines offer higher resolution and faster processing times, allowing for quicker and more accurate assessments.
- MRI (Magnetic Resonance Imaging): While less common for initial OA diagnosis, MRIs can provide more detailed images of soft tissues, including cartilage, ligaments, and tendons. This can be particularly useful in complex cases or when looking for associated injuries. The advancements in MRI technology, such as faster scan times and improved image clarity, contribute to a more precise understanding of your joint’s condition.
- Blood Tests: Though not used to diagnose OA itself, blood tests can help rule out other inflammatory forms of arthritis, such as rheumatoid arthritis. Modern laboratory equipment and automated analysis systems have made these tests more efficient and accurate.
Developing an Initial Management Plan
Based on the diagnosis and your individual needs, your PCP can initiate a basic treatment plan. This might include:
- Pain Management: Recommending over-the-counter or prescription pain relievers and anti-inflammatory medications.
- Lifestyle Modifications: Advising on weight management, which significantly impacts weight-bearing joints like the knees and hips. This might involve referrals to nutritionists or exercise physiologists.
- Referral to Specialists: If your osteoarthritis is severe, complex, or not responding well to initial treatment, your PCP will refer you to specialists who have more focused expertise.
Specialized Care: Navigating the Landscape of Orthopedic and Rheumatological Expertise
When osteoarthritis requires more in-depth management, several types of specialists can play a crucial role. Their expertise often leverages cutting-edge technology and requires a deep understanding of the underlying biological processes.
The Orthopedic Surgeon: For Structural and Surgical Interventions
Orthopedic surgeons are physicians who specialize in the musculoskeletal system – the bones, joints, ligaments, tendons, and muscles. They are particularly crucial for managing osteoarthritis that significantly impacts joint function and may require surgical intervention.
Diagnosis and Non-Surgical Management by Orthopedists
While surgeons, orthopedic specialists also excel in non-surgical management. They can:
- Provide Advanced Diagnostic Interpretation: Beyond what PCPs can offer, orthopedists are adept at interpreting complex imaging studies, identifying subtle signs of cartilage degeneration and bone damage. They can also assess the biomechanics of your joints, understanding how your body moves and where imbalances might be contributing to OA.
- Offer Specialized Injections: This includes corticosteroid injections, which can provide significant, albeit temporary, relief from inflammation and pain in an affected joint. Hyaluronic acid injections (viscosupplementation) are also an option for some patients, aiming to lubricate the joint. The precise delivery of these injections is often guided by ultrasound technology, another testament to the role of “Tech” in modern medicine.
- Develop Comprehensive Conservative Treatment Plans: This might involve recommending specific physical therapy exercises, assistive devices (like canes or braces), and custom orthotics.
Surgical Options for Severe Osteoarthritis
When conservative measures are no longer effective, orthopedic surgeons are the go-to specialists for surgical interventions. These can range from minimally invasive arthroscopic procedures to total joint replacements.
- Arthroscopy: This minimally invasive surgery uses a small camera and instruments to diagnose and repair damage within a joint. It can be used to remove loose fragments of bone or cartilage or to smooth roughened joint surfaces.
- Osteotomy: In some cases, particularly for knee osteoarthritis, an osteotomy can realign the bones to shift weight away from the damaged part of the joint, relieving pain.
- Joint Replacement Surgery: This is a highly effective treatment for severe osteoarthritis, especially in the hips and knees. The damaged joint is replaced with an artificial prosthetic joint. The design and materials of these prosthetics are constantly evolving, driven by advancements in biomaterials science and engineering. Modern joint replacement surgeries are also benefiting from robotic-assisted surgery, offering enhanced precision and potentially faster recovery times.
The Rheumatologist: For Inflammatory Arthritis and Systemic Considerations

While osteoarthritis is primarily a mechanical “wear and tear” condition, rheumatologists are essential for diagnosing and managing inflammatory arthritis conditions that can sometimes mimic or co-exist with OA. They are specialists in autoimmune diseases and inflammatory conditions of the joints, muscles, and bones.
Differentiating Osteoarthritis from Other Conditions
A rheumatologist’s expertise is invaluable in distinguishing osteoarthritis from other forms of arthritis, such as:
- Rheumatoid Arthritis: An autoimmune disease where the body’s immune system attacks the joints, causing inflammation and damage.
- Gout: A form of inflammatory arthritis caused by a buildup of uric acid crystals in the joints.
- Psoriatic Arthritis: Arthritis that affects some people who have psoriasis, a skin condition.
Their ability to accurately diagnose is crucial because the treatment approaches for these conditions differ significantly from those for osteoarthritis.
Managing Inflammatory Components and Systemic Effects
Rheumatologists are skilled in managing the inflammatory aspects of joint disease, which can sometimes be a component of advanced OA or coexist with it. They prescribe:
- Disease-Modifying Antirheumatic Drugs (DMARDs): These medications can help slow the progression of inflammatory arthritis by suppressing the immune system.
- Biologics: A newer class of drugs that target specific parts of the immune system to reduce inflammation.
Their holistic approach also considers how joint health impacts overall well-being and may coordinate care with other specialists for systemic complications.
The Role of Allied Health Professionals: A Collaborative Approach to Wellness
Beyond physicians, a dedicated team of allied health professionals plays a vital role in managing osteoarthritis, often working in conjunction with your doctor. Their input is crucial for a comprehensive and personalized treatment plan, often supported by “Tech” and requiring a “Brand” of self-care.
Physical Therapists: Restoring Movement and Function
Physical therapists (PTs) are indispensable for individuals with osteoarthritis. They develop tailored exercise programs to:
- Strengthen Muscles Around the Joint: Stronger muscles provide better support and stability for the joint, reducing stress on the cartilage.
- Improve Flexibility and Range of Motion: Gentle stretching can help combat stiffness and improve mobility.
- Enhance Balance and Proprioception: This is crucial for preventing falls, especially in individuals with lower limb osteoarthritis.
- Educate on Joint Protection Techniques: PTs teach patients how to modify activities to reduce strain on affected joints.
The delivery of some physical therapy programs is increasingly enhanced by technology, with apps offering guided exercises, progress tracking, and even virtual reality rehabilitation. This fusion of human expertise and digital tools exemplifies the “Tech” integration in modern healthcare.
Occupational Therapists: Adapting Your Environment and Daily Life
Occupational therapists (OTs) focus on helping individuals maintain their independence and perform daily activities despite their osteoarthritis. They can:
- Recommend Assistive Devices: This includes adaptive equipment for cooking, dressing, bathing, and writing.
- Modify Your Home or Workplace: OTs can assess your environment and suggest modifications to make it more accessible and reduce physical strain.
- Teach Energy Conservation Techniques: Helping you pace your activities and manage your energy levels to prevent fatigue and exacerbation of pain.
- Provide Splinting and Bracing: For hand and wrist osteoarthritis, OTs can create custom splints to support and protect joints.
The “Brand” of self-management and adopting new habits that an OT helps you build is as crucial as the medical diagnosis.
Dietitians and Nutritionists: Fueling Your Body for Joint Health
While not directly treating the joint itself, dietitians and nutritionists can significantly impact osteoarthritis management, especially concerning weight control.
- Weight Management: For individuals who are overweight or obese, losing even a small amount of weight can dramatically reduce the stress on weight-bearing joints, alleviating pain and slowing disease progression. Dietitians create personalized eating plans to achieve and maintain a healthy weight.
- Anti-Inflammatory Diets: Some research suggests that certain dietary patterns rich in fruits, vegetables, and omega-3 fatty acids might help reduce inflammation in the body.
The “Money” aspect comes into play here, as healthy eating can be a long-term investment in your well-being, potentially reducing future healthcare costs associated with OA complications.

Navigating Your OA Journey: A Blend of Medical Expertise, Technological Empowerment, and Financial Wisdom
The treatment of osteoarthritis is not a one-size-fits-all approach. It requires a collaborative effort between you and a team of healthcare professionals. Understanding who to consult – from your PCP as your initial guide to orthopedic surgeons for structural interventions and rheumatologists for inflammatory components – is the first step.
Furthermore, embracing the technological advancements in diagnostics, treatment delivery, and patient education empowers you to take a more active role in your care. Building a strong “Brand” of self-advocacy and adherence to your treatment plan, coupled with the financial wisdom to invest in your health and well-being, are equally critical. By integrating these pillars – expert medical care, technological innovation, strong personal branding of proactive health management, and sound financial planning – you can navigate the challenges of osteoarthritis and strive for a more comfortable and functional life.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.