In the landscape of modern medicine, the question of “what blood can AB- receive” is no longer just a biological query found in a textbook; it is a complex data management challenge. AB-negative is one of the rarest blood types globally, found in approximately 1% or less of the population. From a technical perspective, managing this scarcity requires a sophisticated intersection of predictive analytics, secure supply chain logistics, and advanced biotechnological engineering.
As we move deeper into the decade, the integration of Technology (Tech) into hematology has transformed how we approach blood compatibility. The “receiving” of blood for an AB- patient is now a process governed by algorithms, tracked by decentralized ledgers, and optimized by artificial intelligence. This article explores the technological frameworks that ensure the right blood reaches the right patient at the right time.
Precision Diagnostics: The Software Behind Blood Matching
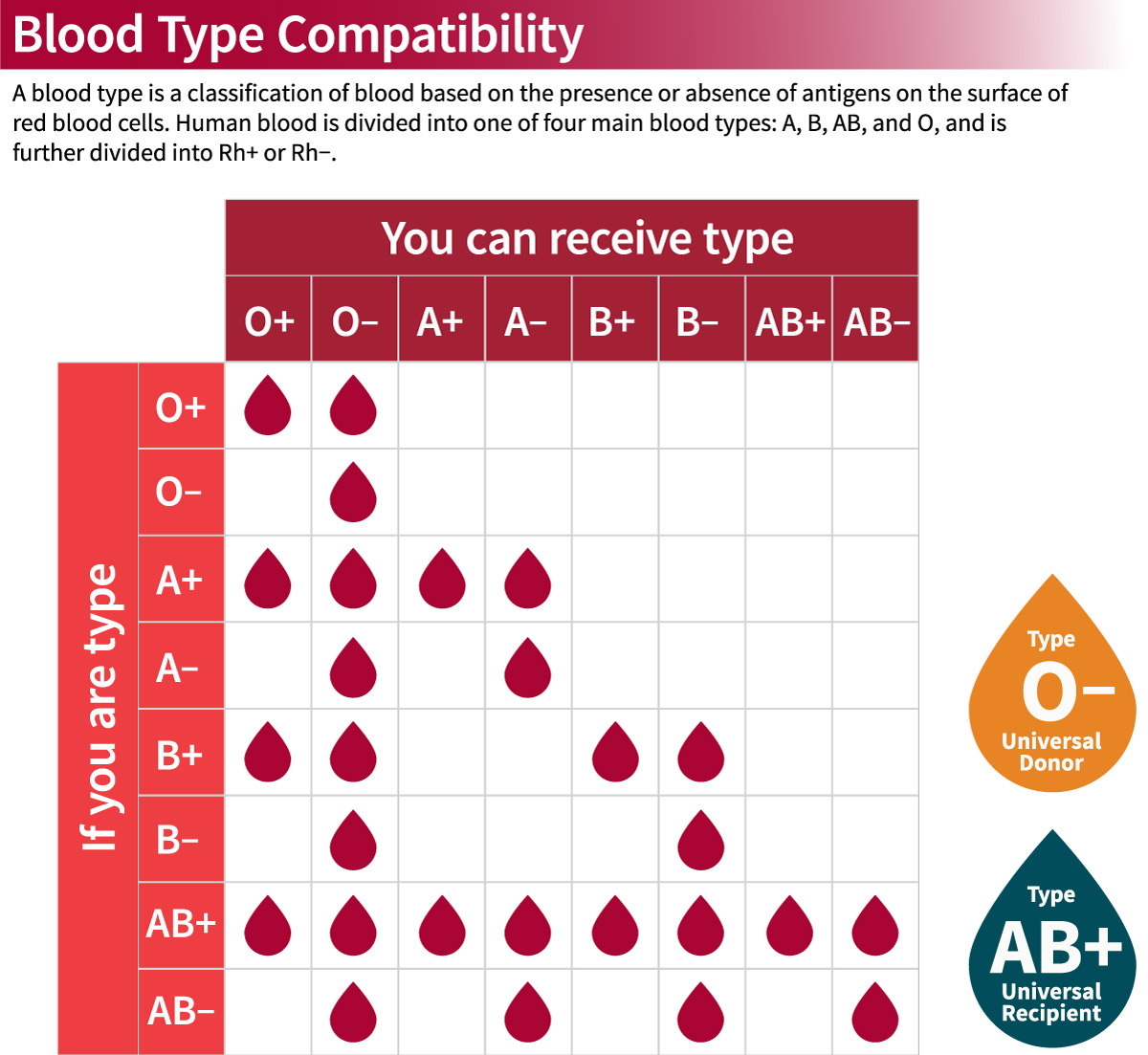
The biological reality of AB-negative blood is that it is the “universal plasma donor” but a highly restricted recipient. A person with AB- blood can receive O-, A-, B-, and AB- blood. However, they cannot receive any Rh-positive blood. In a high-pressure clinical environment, the margin for error is zero. This is where HealthTech software ecosystems take the lead.
AI-Driven Cross-Matching Algorithms
Traditional blood typing involved manual laboratory testing that, while accurate, was subject to human error and time delays. Modern hospitals now utilize automated immunohematology analyzers integrated with AI-driven cross-matching software. These systems use machine learning to predict potential transfusion reactions by analyzing not just the ABO/Rh groups, but also minor antigens that could complicate an AB- transfusion. By processing thousands of data points from a patient’s electronic health record (EHR), these algorithms ensure that the “input” (the donor blood) is perfectly compatible with the “host system” (the patient).
Cloud-Based Donor Registries and Real-Time Availability
Because AB- blood is so rare, local supplies are often insufficient. Tech platforms have evolved to create national and international cloud-based registries. These platforms function similarly to high-frequency trading systems, monitoring the “inventory” of AB- units across multiple jurisdictions. When an AB- patient is admitted, the software can instantly ping the nearest available unit, calculate the logistics of drone-based or high-speed transport, and reserve the unit in real-time. This digital oversight minimizes the “latency” between the need for blood and the delivery of the life-saving resource.
Blockchain and the Integrity of the Rare Blood Supply Chain
When dealing with a resource as scarce as AB-negative blood, the integrity of the supply chain is paramount. The industry is increasingly turning to blockchain technology—the same decentralized architecture that powers digital currencies—to manage the lifecycle of a blood bag from the donor’s arm to the recipient’s vein.
Real-Time Traceability and Cold Chain Monitoring
Blood is a perishable biological asset. AB- blood units must be stored at precise temperatures to remain viable. Through the Internet of Things (IoT), “smart” blood bags equipped with RFID tags and temperature sensors transmit data to a blockchain ledger. This creates an immutable record of the blood’s journey. If an AB- unit intended for a patient experiences a temperature excursion (getting too warm or too cold), the system automatically flags the unit as “corrupted” in the digital ledger, preventing it from being used. This level of technical oversight ensures that what the patient “receives” is not just compatible, but also of the highest quality.
Decentralized Donor Networks
Privacy is a significant concern for donors with rare blood types. Blockchain allows for the creation of decentralized donor networks where an individual’s AB- status is stored securely. Smart contracts can be used to notify donors when their specific blood type is in critically low supply without exposing their personal identity to third-party data brokers. This “privacy-by-design” approach encourages participation in the donor pool, ensuring that the technical infrastructure for AB- receiving remains robust and populated with active data.

The Future of Synthetic Blood and Lab-Grown Solutions
Perhaps the most exciting frontier in the tech sector is the attempt to bypass the scarcity of AB- blood altogether through bio-engineering and synthetic biology. If tech can simulate or create blood, the constraints of “what AB- can receive” become obsolete.
Bioprinting and Artificial Oxygen Carriers
Advanced 3D bioprinting technology is currently being researched to create synthetic red blood cells. Using specialized bio-inks, researchers are working on “printing” cells that mimic the oxygen-carrying capacity of natural blood without the antigens that cause rejection. For an AB- patient, a “universal” synthetic blood would eliminate the need to hunt for rare negative-type donors. These artificial oxygen carriers (AOCs) are being developed using sophisticated molecular modeling software that simulates how synthetic molecules will interact with human hemoglobin.
CRISPR and Universal Donor Conversion
Gene-editing technology, specifically CRISPR-Cas9, is being utilized in a “tech-first” approach to blood management. Scientists are developing enzymatic “molecular scissors” that can strip the A and B antigens off red blood cells. In theory, this would allow tech-driven labs to convert A-, B-, or AB- blood into O- blood (the universal donor). From a technical standpoint, this is a data-processing task at the molecular level—identifying the precise carbohydrate chains to “delete” to reformat the blood into a version the AB- body can receive without an immune response.
Digital Security and Ethical Considerations in Genomic Data
As blood typing becomes more integrated with genomic sequencing and digital tracking, the “Tech” of AB- blood management enters the realm of cybersecurity. A person’s blood type, especially a rare one like AB-, is a piece of sensitive biological metadata.
Protecting Rare Blood Type Databases
Hospitals and blood banks are increasingly targets for ransomware attacks. If a database containing the locations and identities of AB- donors is compromised, it poses a risk to both the healthcare infrastructure and the individual donors. Cybersecurity protocols, including multi-factor authentication and end-to-end encryption for EHRs, are now as vital to blood transfusions as the needles themselves. Ensuring that the “receiving” process is secure means protecting the digital handshake between the donor database and the surgical suite.
Wearable Tech and Emergency Transfusion Protocols
In the future, the “what can AB- receive” question will be answered instantly by wearable devices. Smartwatches and subdermal NFC chips can now store a patient’s critical blood data. In an emergency where a patient is unconscious, a paramedic’s handheld scanner can interface with the wearable tech to identify the AB- requirement immediately. This integration of hardware and biological data reduces the “time-to-treatment” metric, which is the most critical KPI (Key Performance Indicator) in emergency medicine.

Conclusion: The Convergence of Biology and Bitrate
The question of what blood an AB- individual can receive is fundamentally a problem of compatibility and resource management—two areas where technology excels. Through the application of AI in diagnostics, blockchain in logistics, and CRISPR in molecular engineering, the medical community is moving toward a future where “rarity” is no longer a life-threatening variable.
For the AB- patient, the “system” they are a part of is becoming increasingly digital. Their safety is ensured by high-speed data networks, their blood is tracked by immutable ledgers, and their future may very well be secured by lab-grown cells designed in a virtual environment. In the modern era, the management of rare blood types is a testament to the power of Tech to solve the most delicate challenges of human biology. By treating blood compatibility as a sophisticated data-matching problem, we ensure that the 1% of the population with AB- blood receives the same standard of care—and the same hope for a healthy outcome—as everyone else.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.